Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (23): 3619-3624.doi: 10.12307/2021.029
Previous Articles Next Articles
Changes of osteogenic growth factors in the broken end of bone nonunion under stress
Liu Jinwei1, Chen Yunzhen2, Wan Chunyou1
- 1Department of Orthopedics, Tianjin Hospital, Tianjin 300211, China; 2Department of Orthopedics, Qilu Hospital of Shandong University, Jinan 250012, Shandong Province, China
-
Received:2020-06-06Revised:2020-06-12Accepted:2020-07-14Online:2021-08-18Published:2021-01-26 -
Contact:Wan Chunyou, Master, Chief physician, Department of Orthopedics, Tianjin Hospital, Tianjin 300211, China -
About author:Liu Jinwei, Master, Physician, Department of Orthopedics, Tianjin Hospital, Tianjin 300211, China -
Supported by:2019 Research Project of Tianjin Municipal Health Commission for Integrated Chinese and Western Medicine, No. 2019114 (to WCY)
CLC Number:
Cite this article
Liu Jinwei, Chen Yunzhen, Wan Chunyou. Changes of osteogenic growth factors in the broken end of bone nonunion under stress[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3619-3624.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
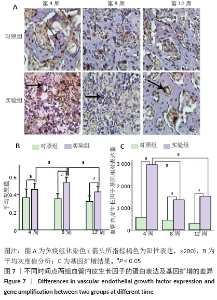
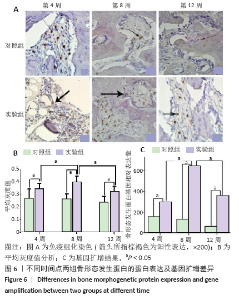
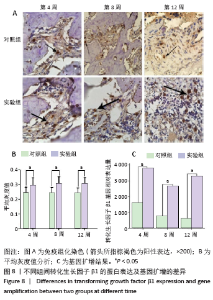
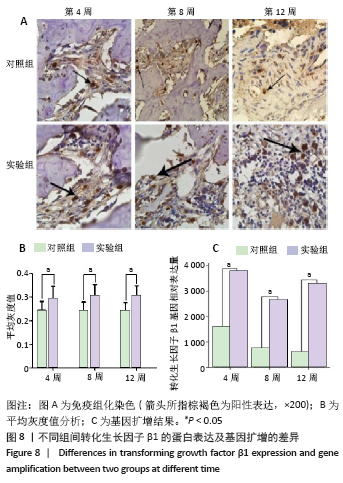
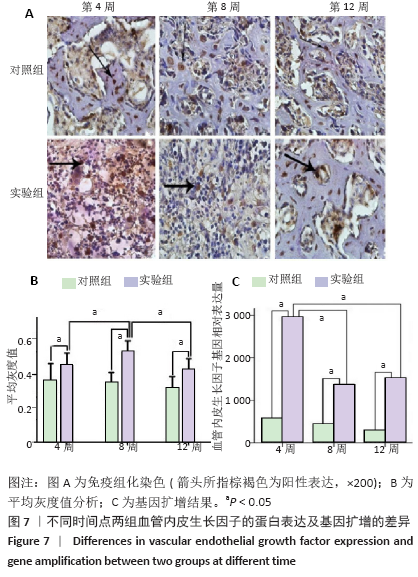
实验组在第8周血管内皮生长因子出现高峰,与同组第4,12周比较差异有显著性意义(P < 0.05);第4周与第12周间表达无明显差异,但均高于同期对照组(P < 0.05,图7)。实验组转化生长因子β1在第4,8,12周与同期对照组比较差异有显著性意义(P < 0.05),实验组内比较差异无显著性意义(图8)。 对照组骨不连断端骨形态发生蛋白2、血管内皮生长因子、转化生长因子β1均有表达,但整体呈低表达,无峰值变化,组间的表达差异无显著性意义(P < 0.05)。 2.5 RT-PCR分析结果 实验组中骨形态发生蛋白基因表达在第8周出现峰值,与第4,12周比较差异有显著性意义(P < 0.05;图6),血管内皮生长因子基因扩增在第4周出现峰值,与第8,12周比较差异有显著性意义(P < 0.05;图7);转化生长因子β1在各期表达平稳,无高峰期,但表达量高于对照组,差异有显著性意义(P < 0.05;图8)。相对于对照组,实验组骨形态发生蛋白、血管内皮生长因子、转化生长因子β1基因扩增差异有显著性意义(P < 0.05)。"
| [1] NELSON FR, BRIGHTON CT, RYABY J, et al. Use of physical forces in bone healing. J Am Acad Orthop Surg. 2003;11(5):344-354. [2] 韩昕光, 毕郑钢, 王东奎, 等. 骨不连接区成骨活性的实验研究[J]. 中华创伤骨科杂志,2009,11(1):45-50. [3] REED AA, JOYNER CJ, BROWNLOW HC, et al. Human atrophic fracture non-unions are not avascular. J Orthop Res. 2002;20(3):593-599. [4] SIGURDSEN U, REIKERAS O, UTVAG SE. The influence of compression on the healing of experimental tibial fractures. Injury.2011;42(10):1152-1156. [5] SANTOS A, BAKKER AD, WILLEMS HM, et al. Mechanical loading stimulates BMP7, but not BMP2, production by osteocytes. Calcif Tissue Int. 2011; 89(4):318-326. [6] PALOMARES KT, GLEASON RE, MASON ZD, et al. Mechanical stimulation alters tissue differentiation and molecular expression during bone healing. J Orthop Res. 2009;27(9):1123-1132. [7] SCHWARZ C, WULSTEN D, ELLINGHAUS A, et al. Mechanical load modulates the stimulatory effect of BMP2 in a rat nonunion model. Tissue Eng Part A. 2013;19(1-2):247-254. [8] BOERCKEL JD, UHRIG BA, WILLETT NJ, et al. Mechanical regulation of vascular growth and tissue regeneration in vivo. Proc Natl Acad Sci U S A. 2011;108(37):E674-680. [9] 赵震宇, 邵林, 刘建宇, 等. 新型外固定器制作大鼠负重骨节段性骨缺损模型的实验研究[J]. 中华创伤骨科杂志,2010,12(12):1160-1163. [10] HUANG G, LIU G, ZHANG F, et al. Combination of heel-strike like mechanical loading with deproteinized cancellous bone scaffold implantation to repair segmental bone defects in rabbits. Int J Med Sci. 2017;14(9):871-879. [11] Yang H, Embry RE, Main RP. Effects of loading duration and short rest insertion on cancellous and cortical bone adaptation in the mouse tibia. PLoS One.2017;12(1):e0169519 [12] BEDFORD TG, TIPTON CM, WILSON NC, et al. Maximum oxygen consumption of rats and its changes with various experimental procedures. J Appl Physiol Respir Environ Exerc Physiol. 1979;47(6):1278-1283 [13] 梁军,钱洁,王惠芳,等.不同强度的主动运动对大鼠膝关节软骨的影响[J].中国康复医学杂志,2012,27(1):8-11. [14] JOHNSON KD, FRIERSON KE, KELLER TS, et al. Porous ceramics as bone graft substitutes in long bone defects: a biomechanical, histological, and radiographic analysis. J Orthop Res. 1996;14(3):351-369. [15] CHAROENPANICH A, WALL ME, TUCKER CJ, et al. Cyclic tensile strain enhances osteogenesis and angiogenesis in mesenchymal stem cells from osteoporotic donors. Tissue Eng Part A. 2014;20(1-2):67-78. [16] HU M, QIN YX. Dynamic fluid flow stimulation on cortical bone and alterations of the gene expressions of osteogenic growth factors and transcription factors in a rat functional disuse model.Arch Biochem Biophys. 2014;545:154-161. [17] JIANG Y, WANG Y, TANG G. Cyclic tensile strain promotes the osteogenic differentiation of a bone marrow stromal cell and vascular endothelial cell co-culture system. Arch Biochem Biophys. 2016;607:37-43. [18] CLAES L, BLAKYTNY R, BESSE J, et al. Late dynamization by reduced fixation stiffness enhances fracture healing in a rat femoral osteotomy model. J Orthop Trauma. 2011;25(3):169-174. [19] GARDNER MJ, VAN DER MEULEN MC, DEMETRAKOPOULOS D, et al. In vivo cyclic axial compression affects bone healing in the mouse tibia. J Orthop Res. 2006;24(8):1679-1686. [20] ZHAO F, VAUGHAN TJ, MCNAMARA LM. Quantification of fluid shear stress in bone tissue engineering scaffolds with spherical and cubical pore architectures. Biomech Model Mechanobiol. 2016;15(3):561-577. [21] MCDERMOTT AM, HERBERG S, MASON DE, et al. Recapitulating bone development through engineered mesenchymal condensations and mechanical cues for tissue regeneration. Sci Transl Med. 2019;11(495). [22] LEE S, SUZUKI T, IZAWA H, et al. The Influence of the Type of Continuous Exercise Stress Applied during Growth Periods on Bone Metabolism and Osteogenesis. J Bone Metab. 2016;23(3):157-164. [23] WANG L, HSU HY, LI X, et al. Effects of Frequency and Acceleration Amplitude on Osteoblast Mechanical Vibration Responses: A Finite Element Study. Biomed Res Int. 2016;2016:2735091. [24] 查丁制. 低强度高频率振动对成骨细胞生物学特性的影响及机制[D]. 广州:南方医科大学, 2011. [25] EINHORN TA,GERSTENFELD LC.Fracture healing: mechanisms and interventions. Nat Rev Rheumatol. 2015;11(1):45-54. [26] NAUTH A, GIANNOUDIS PV, EINHORN TA, et al. Growth factors: beyond bone morphogenetic proteins. J Orthop Trauma.2010;24(9):543-546. [27] STEINBRECH DS, MEHRARA BJ, SAADEH PB, et al. Hypoxia regulates VEGF expression and cellular proliferation by osteoblasts in vitro. Plast Reconstr Surg. 1999;104(3):738-747. [28] KERAMARIS NC, CALORI GM, NIKOLAOU VS, et al. Fracture vascularity and bone healing: a systematic review of the role of VEGF. Injury. 2008;39 Suppl 2:S45-557. [29] SENEL K, BAYKAL T, SEFEROGLU B, et al. Circulating vascular endothelial growth factor concentrations in patients with postmenopausal osteoporosis. Arch Med Sci. 2013;9(4):709-712. [30] BALTZER AW, LATTERMANN C, WHALEN JD, et al. Genetic enhancement of fracture repair: healing of an experimental segmental defect by adenoviral transfer of the BMP-2 gene. Gene Ther. 2000;7(9):734-739. [31] MIYAZAKI M, MORISHITA Y, HE W, et al. A porcine collagen-derived matrix as a carrier for recombinant human bone morphogenetic protein-2 enhances spinal fusion in rats. Spine J. 2009;9(1):22-30. [32] KHAN SN, BOSTROM MP, LANE JM. Bone growth factors. Orthop Clin North Am. 2000;31(3):375-388. [33] ECKARDT H, CHRISTENSEN KS, LIND M, et al. Recombinant human bone morphogenetic protein 2 enhances bone healing in an experimental model of fractures at risk of non-union. Injury. 2005;36(4):489-994. [34] MCBRIDE-GAGYI SH, MCKENZIE JA, BUETTMANN EG, et al. Bmp2 conditional knockout in osteoblasts and endothelial cells does not impair bone formation after injury or mechanical loading in adult mice. Bone. 2015;81:533-543. [35] PATIL AS, SABLE RB, KOTHARI RM. An update on transforming growth factor-β (TGF-β): sources, types, functions and clinical applicability for cartilage/bone healing. J Cell Physiol. 2011;226(12):3094-3103. [36] CARTER DR, BLENMAN PR, BEAUPRÉ GS. Correlations between mechanical stress history and tissue differentiation in initial fracture healing. J Orthop Res. 1988;6(5):736-748. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [5] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [6] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [7] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [8] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [9] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [10] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [11] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [12] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [13] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [14] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [15] | Liang Yan, Zhao Yongfei, Xu Shuai, Zhu Zhenqi, Wang Kaifeng, Liu Haiying, Mao Keya. Imaging evaluation of short-segment fixation and fusion for degenerative lumbar scoliosis assisted by highly selective nerve root block [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1423-1427. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||