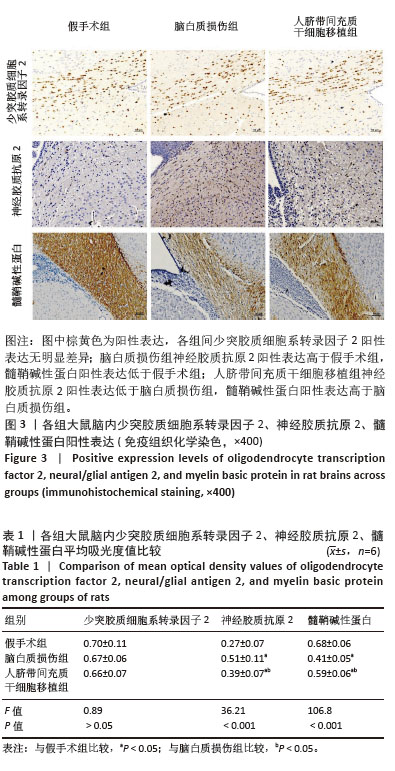
[1] SCHNEIDER J, MILLER SP. Preterm brain Injury: White matter injury. Handb Clin Neurol. 2019;162:155-172.
[2] SERNEELS PJ, DE SCHUTTER JD, DE GROEF L, et al. Oligodendroglial heterogeneity in health, disease, and recovery: deeper insights into myelin dynamics. Neural Regen Res. 2025;20(11):3179-3192.
[3] BACK SA. White matter injury in the preterm infant: pathology and mechanisms. Acta Neuropathol. 2017;134(3):331-349.
[4] WADDELL J, LIN S, CARTER K, et al. Early Postnatal Neuroinflammation Produces Key Features of Diffuse Brain White Matter Injury in Rats. Brain Sci. 2024;14(10):976.
[5] QI L, HU L, QIAN R, et al. Advances in mesenchymal stem cell-centered stem cell therapy in the treatment of hypoxic-ischemic injury. Int Immunopharmacol. 2024;143(Pt 2):113430.
[6] 巴依尔才次克,王彦梅,朱艳萍.间充质干细胞移植改善脑室周围白质软化损伤作用的研究[J].实验动物科学,2021,38(2):22-29.
[7] GHANBARI A, RAD F, SHAHRAKI MH, et al. Human mesenchymal stem cells-derived microvesicles increase oligodendrogenesis and neurogenesis of cultured adult neural stem cells. Neurosci Lett. 2024;841:137951.
[8] MUKAI T, TOJO A, NAGAMURA-INOUE T. Umbilical Cord-Derived Mesenchymal Stromal Cells Contribute to Neuroprotection in Neonatal Cortical Neurons Damaged by Oxygen-Glucose Deprivation. Front Neurol. 2018;9:466.
[9] QIN D, WANG C, LI D, et al. Exosomal miR-23a-3p derived from human umbilical cord mesenchymal stem cells promotes remyelination in central nervous system demyelinating diseases by targeting Tbr1/Wnt pathway. J Biol Chem. 2024;300(1):105487.
[10] RICE JE 3RD, VANNUCCI RC, BRIERLEY JB. The influence of immaturity on hypoxic-ischemic brain damage in the rat. Ann Neurol. 1981;9(2):131-141.
[11] 张军,李明霞,王超,等.不同剂量人脐带间充质干细胞移植对新生大鼠脑白质损伤的修复作用[J].中国当代儿科杂志,2024,26(4):394-402.
[12] 张书绢,王超,徐倩倩,等.NF-κB信号通路在人脐带间充质干细胞移植对新生大鼠脑白质损伤修复中的作用[J].中国当代儿科杂志,2024,26(12):1352-1361.
[13] GEORGE P, CHARLES W.大鼠脑立体定位图谱[M].葛启钏,译.北京:人民卫生出版社,2005:1-63.
[14] RUSS JB, OSTREM BEL. Acquired Brain Injuries Across the Perinatal Spectrum: Pathophysiology and Emerging Therapies. Pediatr Neurol. 2023;148:206-214.
[15] YATES N, GUNN AJ, BENNET L, et al. Preventing Brain Injury in the Preterm Infant-Current Controversies and Potential Therapies. Int J Mol Sci. 2021;22(4):1671.
[16] DEAN JM, MORAVEC MD, GRAFE M, et al. Strain-specific differences in perinatal rodent oligodendrocyte lineage progression and its correlation with human. Dev Neurosci. 2011;33(3-4):251-260.
[17] SEMPLE BD, BLOMGREN K, GIMLIN K, et al. Brain development in rodents and humans: Identifying benchmarks of maturation and vulnerability to injury across species. Prog Neurobiol. 2013;106-107:1-16.
[18] ZENG Y, WANG H, ZHANG L, et al. The optimal choices of animal models of white matter injury. Rev Neurosci. 2019;30(3):245-259.
[19] LIN Q, LIN L, LI L, et al. Dynamic changes of oligodendrogenesis in neonatal rats with hypoxic-ischemic white matter injury. Brain Res. 2023;1817:148495.
[20] MOTAVAF M, PIAO X. Oligodendrocyte Development and Implication in Perinatal White Matter Injury. Front Cell Neurosci. 2021;15:764486.
[21] LI S, ZHANG J, LIU X, et al. Proteomic characterization of hUC-MSC extracellular vesicles and evaluation of its therapeutic potential to treat Alzheimer’s disease. Sci Rep. 2024;14(1):5959.
[22] CHAUBEY S, THUESON S, PONNALAGU D, et al. Early gestational mesenchymal stem cell secretome attenuates experimental bronchopulmonary dysplasia in part via exosome-associated factor TSG-6. Stem Cell Res Ther. 2018;9(1):173.
[23] XIAO Y, CZOPKA T. Myelination-independent functions of oligodendrocyte precursor cells in health and disease. Nat Neurosci. 2023;26(10):1663-1669.
[24] DUFOUR A, HEYDARI OLYA A, FOULON S, et al. Neonatal inflammation impairs developmentally-associated microglia and promotes a highly reactive microglial subset. Brain Behav Immun. 2025;123:466-482.
[25] FABRES RB, CARDOSO DS, ARAGÓN BA, et al. Consequences of oxygen deprivation on myelination and sex-dependent alterations. Mol Cell Neurosci. 2023;126:103864.
[26] DUERDEN EG, HALANI S, NG K, et al. White matter injury predicts disrupted functional connectivity and microstructure in very preterm born neonates. Neuroimage Clin. 2019;21:101596.
[27] HOANG DM, PHAM PT, BACH TQ, et al. Stem cell-based therapy for human diseases. Signal Transduct Target Ther. 2022;7(1):272.
[28] ZHU LH, BAI X, ZHANG N, et al. Improvement of human umbilical cord mesenchymal stem cell transplantation on glial cell and behavioral function in a neonatal model of periventricular white matter damage. Brain Res. 2014;1563: 13-21.
[29] BONORA M, DE MARCHI E, PATERGNANI S, et al. Tumor necrosis factor-α impairs oligodendroglial differentiation through a mitochondria-dependent process. Cell Death Differ. 2014;21(8):1198-1208.
[30] THEOPHANOUS S, SARGIANNIDOU I, KLEOPA KA. Glial Cells as Key Regulators in Neuroinflammatory Mechanisms Associated with Multiple Sclerosis. Int J Mol Sci. 2024;25(17):9588.
[31] DEY D, TYAGI S, SHRIVASTAVA V, et al. Using Human Fetal Neural Stem Cells to Elucidate the Role of the JAK-STAT Cell Signaling Pathway in Oligodendrocyte Differentiation In Vitro. Mol Neurobiol. 2024;61(8):5738-5753.
[32] DROMMELSCHMIDT K, SERDAR M, BENDIX I, et al. Mesenchymal stem cell-derived extracellular vesicles ameliorate inflammation-induced preterm brain injury. Brain Behav Immun. 2017;60:220-232.
[33] TAPIA-BUSTOS A, LESPAY-REBOLLEDO C, VÍO V, et al. Neonatal Mesenchymal Stem Cell Treatment Improves Myelination Impaired by Global Perinatal Asphyxia in Rats. Int J Mol Sci. 2021;22(6):3275.
[34] JIAO Y, SUN YT, CHEN NF, et al. Human umbilical cord-derived mesenchymal stem cells promote repair of neonatal brain injury caused by hypoxia/ischemia in rats. Neural Regen Res. 2022;17(11):2518-2525. |