Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (53): 8547-8552.doi: 10.3969/j.issn.2095-4344.2014.53.004
Previous Articles Next Articles
Patients with necrosis of the femoral head and taking hormone for a long time after fibular graft: eight hips receiving total hip replacement
Wang Yan-mao, Zhang Chang-qing, Ding Hao, Chen Sheng-bao
- Department of Orthopedics, The Sixth People’s Hospital, Shanghai Jiao Tong University, Shanghai 200233, China
-
Revised:2014-11-03Online:2014-12-24Published:2014-12-24 -
Contact:Zhang Chang-qing, M.D., Doctoral supervisor, Chief physician, Department of Orthopedics, The Sixth People’s Hospital, Shanghai Jiao Tong University, Shanghai 200233, China -
About author:Wang Yan-mao, Studying for master’s degree, Department of Orthopedics, The Sixth People’s Hospital, Shanghai Jiao Tong University, Shanghai 200233, China -
Supported by:the Key Project of Shanghai Science and Technology Committee, No. 11411950400
CLC Number:
Cite this article
Wang Yan-mao, Zhang Chang-qing, Ding Hao, Chen Sheng-bao. Patients with necrosis of the femoral head and taking hormone for a long time after fibular graft: eight hips receiving total hip replacement[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(53): 8547-8552.
share this article
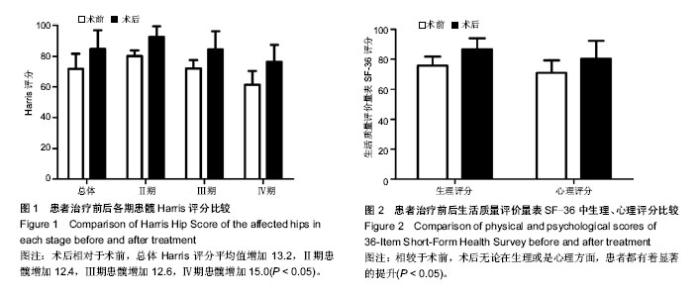
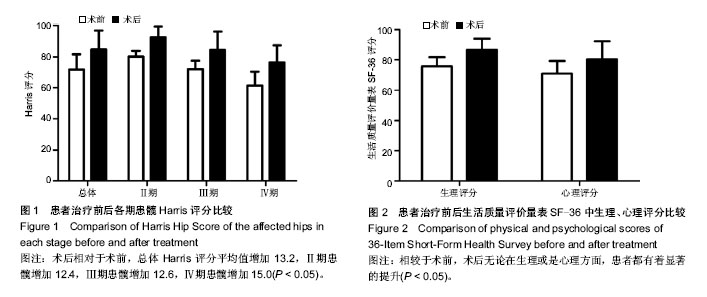
2.3 并发症及转归 所有患者均从术后第1天开始进行功能锻炼,直至患肢完全负重,术后无患者出现急性并发症,10侧患髋出现了创伤性血肿(10%),4侧(4%)患肢出现了下肢深静脉血栓,但均通过口服抗凝药物得到有效控制,8侧(8%)患肢出现了术后拇趾背伸困难及感觉异常,保守治疗后病情逐渐好转。 在随访的过程中,共有8侧(8%)患髋最终进行了全髋关节置换,其中包括2髋Steinberg分期Ⅲ期(4.5%),以及6髋Ⅳ期(25%)。另外有一部分患者影像学检查显示病情进一步地恶化,但未进行全髋关节置换,而是选择服用镇痛药物或减免患肢负重来降低疼痛感,主要原因是由于患者年龄较轻,综合人工关节的使用寿命及个人经济条件所作出的决定。 2.4 Harris评分 使用Harris评分量表对比了患髋治疗前后髋关节的功能情况。术前96侧患髋总体Harris评分平均值为71.7±9.8,其中Ⅱ期患髋平均值为80.2±3.6,Ⅲ期患髋平均值为72.0±5.4,Ⅳ期患髋平均值为61.4±9.0。在最近一次的随访中,总体Harris评分平均值为84.9±12.0(P < 0.05),Ⅱ期患髋平均值为92.6±6.8(P < 0.05),Ⅲ期患髋平均值为84.6±11.6(P < 0.05),Ⅳ期患髋平均值为76.4±11.0 (P < 0.05)(图1)。术后相对于术前总体Harris评分平均值增加13.2,Ⅱ期患髋增加12.4,Ⅲ期患髋增加12.6,Ⅳ期患髋增加15.0。 2.5 生活质量评价量表(SF-36)评分 SF-36评价量表分为生理评分及心理评分两方面。术前54例患者生理评分平均值为75.8±6.0,心理评分平均值为71.0±8.4。在最近一次的随访中,患者术后总体生理评分平均值为86.8±7.2 (P < 0.05),平均提升11.0;心理评分平均值为80.4±12.0 (P < 0.05),平均提升9.4。相较于术前,无论在生理或是心理方面,患者都有着显著的提升,见图2。"
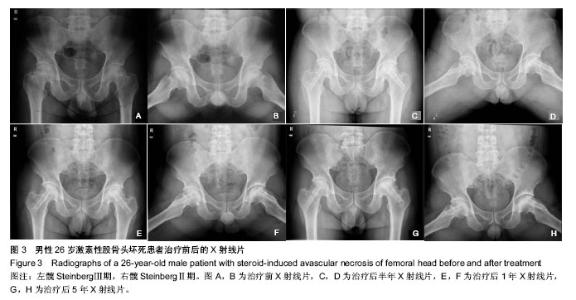
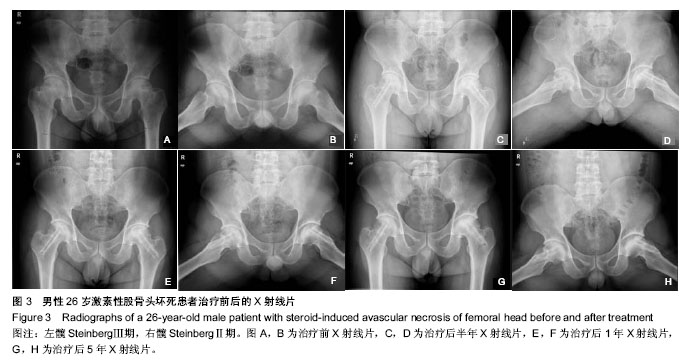
2.6 影像学评估 影响学的评估方式如前文所述。最近一次随访结果显示,61侧(63%)患髋影像学检查表现为改善,14侧(15%)患髋表现为稳定,21侧(22%)患髋表现为恶化。依照Steinberg分期,①改善:Ⅱ期21例(75%),Ⅲ期28例(64%),Ⅳ期12例(50%)。②稳定:Ⅱ期2例(7%),Ⅲ期8例(18%),Ⅳ期4例(17%)。③恶化:Ⅱ期5例(18%),Ⅲ期8例(18%),Ⅳ期8例(33%)。 2.7 典型病例 男性患者,26岁,特发性血小板减少性紫癜病史2年,术前服用激素剂量为8.0 mg/d,双侧股骨头坏死(左髋Steinberg Ⅲ期,右髋SteinbergⅡ期),确诊6个月。于2008年5月入院,术前Harris评分:左侧70,右侧78;SF-36评分:生理评分74,心理评分70。 入院后完善术前检查后行双侧带血管的游离腓骨移植,术后无特殊并发症发生。患者术后继续服用激素,调整剂量为6.0 mg/d,原发病得到有效控制。 术后1年,Harris评分:左侧82,右侧90;SF-36评分:生理评分84,心理评分80;X射线片示:左侧稳定,右侧改善。术后5年,Harris评分:左侧80,右侧86;SF-36评分:生理评分82,心理评分82;X射线片显示:左侧稳定,右侧改善,见图3。"
| [1] Babis GC, Sakellariou V, Parvizi J, et al. Osteonecrosis of the femoral head. Orthopedics. 2011;34(1): 39. [2] Wei BF, Ge XH. Treatment of osteonecrosis of the femoral head with core decompression and bone grafting. Hip Int. 2011;21(2): 206-210. [3] Wang XS, Zhuang QY, Weng XS, et al. Etiological and clinical analysis of osteonecrosis of the femoral head in Chinese patients. Chin Med J (Engl). 2013;126(2):290-295. [4] Weinstein RS. Glucocorticoids, osteocytes, and skeletal fragility: the role of bone vascularity. Bone. 2010;46(3): 564-570. [5] Griffith JF, Antonio GE, Kumta SM, et al. Osteonecrosis of hip and knee in patients with severe acute respiratory syndrome treated with steroids. Radiology. 2005;235(1):168-175. [6] Marston SB, Gillingham K, Bailey RF, et al. Osteonecrosis of the femoral head after solid organ transplantation: a prospective study. J Bone Joint Surg Am. 2002;84-A(12): 2145-2151. [7] 郑志辉,王少伟,李伟居,等.保髋治疗股骨头坏死的特异性量表[J]. 中国组织工程研究, 2012,16 (35):6570-6575. [8] Mont MA, Jones LC, Hungerford DS. Nontraumatic osteonecrosis of the femoral head: ten years later. J Bone Joint Surg Am. 2006; 88(5):1117-1132. [9] Korompilias AV, Lykissas MG, Beris AE, et al. Vascularised fibular graft in the management of femoral head osteonecrosis: twenty years later. J Bone Joint Surg Br. 2009;91(3):287-293. [10] Steinberg ME, Hayken GD, Steinberg DR. A quantitative system for staging avascular necrosis. J Bone Joint Surg Br. 1995;77(1): 34-41. [11] Zhang C, Zeng B, Xu Z, et al. Treatment of femoral head necrosis with free vascularized fibula grafting: a preliminary report. Microsurgery. 2005;25(4):305-309. [12] Gao YS, Liu XL, Sheng JG, et al. Unilateral free vascularized fibula shared for the treatment of bilateral osteonecrosis of the femoral head. J Arthroplasty. 2013;28(3):531-536. [13] Ware JE JR, Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care. 1992;30(6):473-483. [14] Yu J, Coons SJ, Draugalis JR, et al. Equivalence of Chinese and US-English versions of the SF-36 health survey. Qual Life Res. 2003;12(4): 449-457. [15] Ohzono K, Saito M, Sugano N, et al. The fate of nontraumatic avascular necrosis of the femoral head. A radiologic classification to formulate prognosis. Clin Orthop Relat Res. 1992;277:73-78. [16] 毕鑫,李多玉,杨毅,等.不同人工骨材料复合骨髓间充质干细胞治疗早期股骨头坏死:争议与进展[J].中国组织工程研究,2014, 18(12): 1957-1962. [17] 章乐成,尹宗生.骨髓间充质干细胞及其载体在股骨头坏死治疗中的研究与进展[J].中国组织工程研究,2014,18(3):440-445. [18] Scully SP, Aaron RK, Urbaniak JR. Survival analysis of hips treated with core decompression or vascularized fibular grafting because of avascular necrosis. J Bone Joint Surg Am. 1998; 80(9):1270-1275. [19] Dailiana ZH, Toth AP, Gunneson E, et al. Free vascularized fibular grafting following failed core decompression for femoral head osteonecrosis. J Arthroplasty. 2007;22(5): 679-688. [20] Yoo MC, Chung DW, Hahn CS. Free vascularized fibula grafting for the treatment of osteonecrosis of the femoral head. Clin Orthop Relat Res. 1992;277:128-138. [21] Judet H, Gilbert A. Long-term results of free vascularized fibular grafting for femoral head necrosis. Clin Orthop Relat Res. 2001;386:114-119. [22] Berend KR, Gunneson EE, Urbaniak JR. Free vascularized fibular grafting for the treatment of postcollapse osteonecrosis of the femoral head. J Bone Joint Surg Am. 2003; 85-A(6): 987-993. [23] Gao YS, Chen SB, Jin DX, et al. Modified surgical techniques of free vascularized fibular grafting for treatment of the osteonecrosis of femoral head: Results from a series of 407 cases. Microsurgery. 2013. [24] Takano-murakami R, Tokunaga K, Kondo N, et al. Glucocorticoid inhibits bone regeneration after osteonecrosis of the femoral head in aged female rats. Tohoku J Exp Med. 2009; 217(1):51-58. [25] Zhao FC, Li ZR, Guo KJ. Clinical analysis of osteonecrosis of the femoral head induced by steroids. Orthop Surg.2012;4(1): 28-34. [26] Li X, Jin L, Cui Q, et al. Steroid effects on osteogenesis through mesenchymal cell gene expression. Osteop Int. 2005; 16(1):101-108. [27] Miyanishi K, Yamamoto T, Irisa T, et al. Bone marrow fat cell enlargement and a rise in intraosseous pressure in steroid-treated rabbits with osteonecrosis. Bone. 2002;30(1): 185-90. [28] Tan G, Kang PD, Pei FX. Glucocorticoids affect the metabolism of bone marrow stromal cells and lead to osteonecrosis of the femoral head: a review. Chin Med J (Engl). 2012;125(1):134-139. [29] Drescher W, Bunger MH, Weigert K, et al. Methylprednisolone enhances contraction of porcine femoral head epiphyseal arteries. Clin Orthop Relat Res. 2004;423:112-117. [30] Xu J, Zhang CQ, Zhang KG, et al. Modified Free Vascularized Fibular Grafting for the Treatment of Femoral Neck Nonunion. J Orthop Trauma. 2010;24(4):230-235. [31] Li M, Shen Y, Halloran BP, et al. Skeletal response to corticosteroid deficiency and excess in growing male rats. Bone. 1996;19(2):81-88. [32] Wang Y, Ohtsuka-isoya M, Shao P, et al. Effects of methylprednisolone on bone formation and resorption in rats. Japan J Pharmacol. 2002;90(3):236-246. [33] Cui Q, Wang GJ, Balian G. Steroid-induced adipogenesis in a pluripotential cell line from bone marrow. J Bone Joint Surg Am. 1997;79(7):1054-1063. [34] Kerachian MA, Seguin C, Harvey EJ. Glucocorticoids in osteonecrosis of the femoral head: a new understanding of the mechanisms of action. J Ster Biochem Mol Biol. 2009; 114(3-5):121-128. |
| [1] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [2] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [3] | Li Xiangze, Bu Xianmin, Li Dongmei, Chi Yulei, Su Qiang, Jin Xintong, Zhao Jian, Zhang Gaotian, Wu Bin, Meng Chunyang . Stem cells, cytokines, hormones, neuropeptides and genes in traumatic brain trauma to promote fracture healing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3057-3063. |
| [4] | Huang Zeling, Shi Shanni, He Junjun, Gao Hongjian, Ge Haiya, Hong Zhenqiang. Meta-analysis of safety and effectiveness of proximal fibular osteotomy and high tibial osteotomy in the treatment of knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2945-2952. |
| [5] | Wang Lei, Qi Rong, Li Jia, Qiu Zhixue, Wang Kai, Suo Nanangxiu. Minimally invasive percutaneous plate osteosynthesis and elastic nail system in the treatment of distal tibiofibular fracture in adults [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1864-1868. |
| [6] | Xiang Feifan, Tan Xiaoqi, Xiang Yong, Liang Jie, Zhou Wei, Luo Liang, Gu Hao, Yang Yunkang. Effect of anatomic locking plate combined with allograft fibula on proximal humerus fracture: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5897-5904. |
| [7] | Mo Fan, Hua Qikai, Zhao Jinmin, Sha Ke, Xie Qi, Zhang Jin, Yang Yuan, Huang Weifeng, Wang Hao, Huang Hao, Chen Yinghua. Efficacy of free fibula transplantation combined with platelet rich plasma in the treatment of early necrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(35): 5675-5681. |
| [8] | Weng Shiyang, Wu Kai, Lin Jian, Huang Yinjun, Wang Qiugen, Huang Jianhua. Double-strand suture anchor in the treatment of tibiofibular syndesmosis injury [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5332-5337. |
| [9] | Wang Dong, Zeng Debin, Lin Qiao, Liu Kehui. Tibiofibular syndesmosis reduction after screw fixation of ankle fracture evaluated by CT imaging [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5349-5353. |
| [10] | Tian Chenyang, Chen Bin, Sun Zhengtao, Wang Xinjun, Sun Haiyu. Suture-Button fixation and screw fixation for the treatment of distal tibiofibular syndesmosis injury: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 485-492. |
| [11] | Hou Haisheng, Yang Li, Yan Xiaowei. Efficacy of 3D Max mesh versus common mesh for laparoscopic inguinal hernia repair [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(28): 4588-4592. |
| [12] | Tu Dongpeng, Yu Yikang, Liu Zheng, Fan Xin, Zhang Wenkai, Xu Chao. Meta-analysis of locking plate combined with fibular allograft and locking plate alone in the treatment of proximal humeral fractures [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(27): 4389-4397. |
| [13] | Ji Haihong, Dong Qiang. Finite element analysis of different fixation methods for mandibular defects reconstructing with fibula flaps [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(24): 3821-3827. |
| [14] | Zhao Yongjie, Sun Guangchao, Guan Guofeng, Du Rui, Zhu Xiaodong. Effect of preserving the integrity of peroneal tendon sheath on hindfoot function after calcaneus fracture surgery [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(23): 3662-3666. |
| [15] | Ling Guanhan, Li Yongbin, Pan Xuewen, Lin Hengfeng, He Ke, Li Yuanchun, Lu Baiyu, Chen Changlin. Three-dimensional finite element analysis of fibula implantation for China-Japan Friendship Hospital type osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(18): 2817-2822. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

