Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (44): 7066-7070.doi: 10.3969/j.issn.2095-4344.2014.44.003
Previous Articles Next Articles
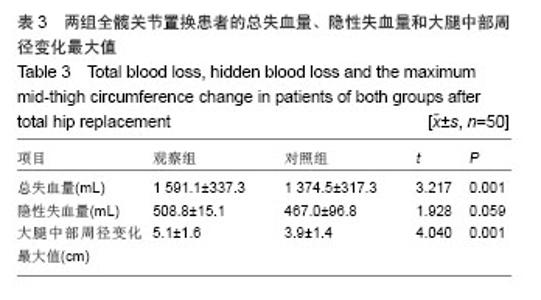
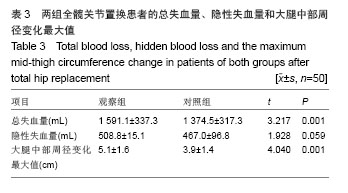
Reinfusion of autologous drainage blood after total hip replacement under the application of anticoagulant
Li Wei
- Department of Bone and Joint Surgery, Weifang People’s Hospital, Weifang 261041, Shandong Province, China
-
Online:2014-10-22Published:2014-10-22 -
About author:Li Wei, M.D., Attending physician, Department of Bone and Joint Surgery, Weifang People’s Hospital, Weifang 261041, Shandong Province, China
CLC Number:
Cite this article
Li Wei. Reinfusion of autologous drainage blood after total hip replacement under the application of anticoagulant[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(44): 7066-7070.
share this article
| [1]李军,王健,史占军,等.全髋关节置换后应用利伐沙班安全性的Meta分析[J].中国组织工程研究,2012,16(9):1618-1621. [2]Geerts WH, Pineo GF, Heit JA, et al. Prevention of venous thromboembolism: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126(3 Suppl):338S-400S. [3]Geerts WH, Bergqvist D, Pineo GF, et al. Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133(6 Suppl):381S-453S. [4]Turpie AG. Oral, direct factor Xa inhibitors in development for the prevention and treatment of thromboembolic diseases. Arterioscler Thromb Vasc Biol. 2007;27(6):1238-1247. [5]Jadad AR, Moore RA, Carroll D, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17(1):1-12. [6]Eriksson BI, Borris L, Dahl OE, et al. Oral, direct Factor Xa inhibition with BAY 59-7939 for the prevention of venous thromboembolism after total hip replacement. J Thromb Haemost. 2006;4(1):121-128. [7]Eriksson BI, Borris LC, Dahl OE, et al. Dose-escalation study of rivaroxaban (BAY 59-7939)--an oral, direct Factor Xa inhibitor--for the prevention of venous thromboembolism in patients undergoing total hip replacement. Thromb Res. 2007; 120(5):685-693. [8]Eriksson BI, Borris LC, Friedman RJ, et al. Rivaroxaban versus enoxaparin for thromboprophylaxis after hip arthroplasty. N Engl J Med. 2008;358(26): 2765-2775. [9]Eriksson BI, Borris LC, Dahl OE, et al. A once-daily, oral, direct Factor Xa inhibitor, rivaroxaban (BAY 59-7939), for thromboprophylaxis after total hip replacement. Circulation. 2006;114(22):2374-2381. [10]Kakkar AK, Brenner B, Dahl OE, et al. Extended duration rivaroxaban versus short-term enoxaparin for the prevention of venous thromboembolism after total hip arthroplasty: a double-blind, randomised controlled trial. Lancet. 2008;372 (9632):31-39. [11]颜世海,颜鹏.全膝关节置换术后自体引流血回输有效性及安全性的Meta分析[J].实用医学杂志,2014,(10):1644-1647. [12]刘宏鸣,朱吉桂,叶峥,等.植骨加盖行生物学固定型全髋关节置换治疗严重成人髋关节发育不良[J].中国组织工程研究,2014, 18(26):4120-4124. [13]Ogino D, Kawaji H, Konttinen L, et al. Total hip replacement in patients eighty years of age and older. J Bone Joint Surg Am. 2008;90(9):1884-1890. [14]Keisu KS, Mathiesen EB, Lindgren JU. The uncemented fully textured Lord hip prosthesis: a 10- to 15-year followup study. Clin Orthop Relat Res. 2001;(382):133-142. [15]Mulliken BD, Bourne RB, Rorabeck CH, et al. A tapered titanium femoral stem inserted without cement in a total hip arthroplasty. Radiographic evaluation and stability. J Bone Joint Surg Am. 1996;78(8):1214-1225. [16]Glassman AH, Bobyn JD, Tanzer M. New femoral designs: do they influence stress shielding? Clin Orthop Relat Res. 2006; 453:64-74. [17]Fousek J, Indráková P. Total hip arthroplasty in post-dysplastic hip arthritis. Can type and position of the acetabular component influence longevity of the prosthesis? Acta Chir Orthop Traumatol Cech. 2007;74(1):47-54. [18]Gill TJ, Sledge JB, Müller ME. Total hip arthroplasty with use of an acetabular reinforcement ring in patients who have congenital dysplasia of the hip. Results at five to fifteen years. J Bone Joint Surg Am. 1998;80(7):969-979. [19]廖万东,胡柳生,石双平.自体血联合不同胶体急性高容量血液稀释用于老年髋关节置换术的安全性[J].实用医学杂志,2012,28(9) 1476-1478. [20]程文俊,王俊文,任义军,等.利伐沙班与低分子量肝素在初次全髋关节置换术后深静脉血栓形成防治中的比较研究[J].中华创伤骨科杂志,2012,14(6):480-483. [21]Elias A, Cadène A, Elias M, et al. Extended lower limb venous ultrasound for the diagnosis of proximal and distal vein thrombosis in asymptomatic patients after total hip replacement. Eur J Vasc Endovasc Surg. 2004;27(4):438-444. [22]Kakkar AK, Brenner B, Dahl OE, et al. Extended duration rivaroxaban versus short-term enoxaparin for the prevention of venous thromboembolism after total hip arthroplasty: a double-blind, randomised controlled trial. Lancet. 2008;372 (9632):31-39. [23]Pitto RP, Hamer H, Heiss-Dunlop W, et al. Mechanical prophylaxis of deep-vein thrombosis after total hip replacement a randomised clinical trial. J Bone Joint Surg Br. 2004;86(5):639-642. [24]Colwell CW Jr, Froimson MI, Mont MA, et al. Thrombosis prevention after total hip arthroplasty: a prospective, randomized trial comparing a mobile compression device with low-molecular-weight heparin. J Bone Joint Surg Am. 2010; 92(3):527-535. [25]程文俊,徐海军,肖志宏,等.利伐沙班抗凝状态下术后自体引流血回输对初次全髋关节置换术后隐性失血和肢体肿胀的影响[J].南方医科大学学报,2014,(3):438-440. [26]Sarkanovi? ML, Gvozdenovi? L, Savi? D, et al. Autologous blood transfusion in total knee replacement surgery. Vojnosanit Pregl. 2013;70(3):274-278. [27]Santana M, Martínez E, Herrera E, et al. Effectiveness of postoperative autologous blood transfusion after knee replacement surgery and influence of preoperative hemoglobin level. Rev Esp Anestesiol Reanim. 2005; 52(6): 315-320. [28]Hatzidakis AM, Mendlick RM, McKillip T, et al. Preoperative autologous donation for total joint arthroplasty. An analysis of risk factors for allogenic transfusion. J Bone Joint Surg Am. 2000;82(1):89-100. [29]Jones HW, Savage L, White C, et al. Postoperative autologous blood salvage drains--are they useful in primary uncemented hip and knee arthroplasty? A prospective study of 186 cases. Acta Orthop Belg. 2004;70(5):466-473. [30]Borghi B, Casati A. Incidence and risk factors for allogenic blood transfusion during major joint replacement using an integrated autotransfusion regimen. The Rizzoli Study Group on Orthopaedic Anaesthesia. Eur J Anaesthesiol. 2000;17(7): 411-417. [31]Ku?era B, Náhlík D, Hart R, et al. Post-operative retransfusion and intra-operative autotransfusion systems in total knee arthroplasty. A comparison of their efficacy. Acta Chir Orthop Traumatol Cech. 2012;79(4):361-366. [32]Moonen AF, Knoors NT, van Os JJ, et al. Retransfusion of filtered shed blood in primary total hip and knee arthroplasty: a prospective randomized clinical trial. Transfusion. 2007; 47(3):379-384. [33]Oberhofer D, Saki? K, Jankovi? S, et al. How to improve perioperative blood management in patients undergoing total hip or knee replacement surgery? Lijec Vjesn. 2012;134 (11-12): 322-327. [34]Innerhofer P, Klingler A, Klimmer C, et al. Risk for postoperative infection after transfusion of white blood cell-filtered allogeneic or autologous blood components in orthopedic patients undergoing primary arthroplasty. Transfusion. 2005;45(1):103-110. [35]Rees JE, Jeavons R, Dixon JH. An economic justification for autologous blood re-infusion in primary total knee replacement surgery. Ann R Coll Surg Engl. 2005;87(2): 102-105. [36]Zhang Y, Li ZJ, Zheng YF, et al. Delayed drainage versus autotransfusion drainage and routine drainage after total knee arthroplasty: a comparative study. J Orthop Surg Res. 2013;8: 39. [37]Kang DG, Khurana S, Baek JH, et al. Efficacy and safety using autotransfusion system with postoperative shed blood following total knee arthroplasty in haemophilia. Haemophilia. 2014;20(1):129-132. [38]Aksoy Y, Altinel L, Köse KÇ. The comparison of the effects of intraoperative bleeding control and postoperative drain clamping methods on the postoperative blood loss and the need for transfusion following total knee arthroplasty. Acta Orthop Traumatol Turc. 2011;45(3):190-194. [39]Matsuda K, Nozawa M, Katsube S, et al. Reinfusion of unwashed salvaged blood after total knee arthroplasty in patients with rheumatoid arthritis. Int Orthop. 2009;33(6): 1615-1618. [40]Hourlier H, Fennema P. Chemoprophylaxis without intra-articular wound drainage can replace autotransfusion in primary TKA. Orthopedics. 2011;34(6):154. [41]So-Osman C, Nelissen RG, Koopman-van Gemert AW, et al. Patient blood management in elective total hip- and knee-replacement surgery (part 2): a randomized controlled trial on blood salvage as transfusion alternative using a restrictive transfusion policy in patients with a preoperative hemoglobin above 13 g/dl. Anesthesiology. 2014;120(4): 852-860. [42]Mutsuzaki H, Ikeda K. Intra-articular injection of tranexamic acid via a drain plus drain-clamping to reduce blood loss in cementless total knee arthroplasty. J Orthop Surg Res. 2012; 7:32. [43]Jones HW, Savage L, White C, et al. Postoperative autologous blood salvage drains--are they useful in primary uncemented hip and knee arthroplasty? A prospective study of 186 cases. Acta Orthop Belg. 2004;70(5):466-473. [44]Strümper D, Weber EW, Gielen-Wijffels S, et al. Clinical efficacy of postoperative autologous transfusion of filtered shed blood in hip and knee arthroplasty. Transfusion. 2004; 44(11):1567-1571. [45]Kim HJ, Fraser MR, Kahn B, et al. The efficacy of a thrombin-based hemostatic agent in unilateral total knee arthroplasty: a randomized controlled trial. J Bone Joint Surg Am. 2012;94(13):1160-1165. [46]高福强,李子剑,张克,等.初次全膝关节置换术后隐性失血的影响因素研究[J].中华外科杂志,2011,49(5):419-423. |
| [1] | Chen Ziyang, Pu Rui, Deng Shuang, Yuan Lingyan. Regulatory effect of exosomes on exercise-mediated insulin resistance diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 4089-4094. |
| [2] | Chen Yang, Huang Denggao, Gao Yuanhui, Wang Shunlan, Cao Hui, Zheng Linlin, He Haowei, Luo Siqin, Xiao Jingchuan, Zhang Yingai, Zhang Shufang. Low-intensity pulsed ultrasound promotes the proliferation and adhesion of human adipose-derived mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3949-3955. |
| [3] | Yang Junhui, Luo Jinli, Yuan Xiaoping. Effects of human growth hormone on proliferation and osteogenic differentiation of human periodontal ligament stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3956-3961. |
| [4] | Sun Jianwei, Yang Xinming, Zhang Ying. Effect of montelukast combined with bone marrow mesenchymal stem cell transplantation on spinal cord injury in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3962-3969. |
| [5] | Gao Shan, Huang Dongjing, Hong Haiman, Jia Jingqiao, Meng Fei. Comparison on the curative effect of human placenta-derived mesenchymal stem cells and induced islet-like cells in gestational diabetes mellitus rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3981-3987. |
| [6] | Hao Xiaona, Zhang Yingjie, Li Yuyun, Xu Tao. Bone marrow mesenchymal stem cells overexpressing prolyl oligopeptidase on the repair of liver fibrosis in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3988-3993. |
| [7] | Liu Jianyou, Jia Zhongwei, Niu Jiawei, Cao Xinjie, Zhang Dong, Wei Jie. A new method for measuring the anteversion angle of the femoral neck by constructing the three-dimensional digital model of the femur [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3779-3783. |
| [8] | Meng Lingjie, Qian Hui, Sheng Xiaolei, Lu Jianfeng, Huang Jianping, Qi Liangang, Liu Zongbao. Application of three-dimensional printing technology combined with bone cement in minimally invasive treatment of the collapsed Sanders III type of calcaneal fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3784-3789. |
| [9] | Qian Xuankun, Huang Hefei, Wu Chengcong, Liu Keting, Ou Hua, Zhang Jinpeng, Ren Jing, Wan Jianshan. Computer-assisted navigation combined with minimally invasive transforaminal lumbar interbody fusion for lumbar spondylolisthesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3790-3795. |
| [10] | Hu Jing, Xiang Yang, Ye Chuan, Han Ziji. Three-dimensional printing assisted screw placement and freehand pedicle screw fixation in the treatment of thoracolumbar fractures: 1-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3804-3809. |
| [11] | Shu Qihang, Liao Yijia, Xue Jingbo, Yan Yiguo, Wang Cheng. Three-dimensional finite element analysis of a new three-dimensional printed porous fusion cage for cervical vertebra [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3810-3815. |
| [12] | Wang Yihan, Li Yang, Zhang Ling, Zhang Rui, Xu Ruida, Han Xiaofeng, Cheng Guangqi, Wang Weil. Application of three-dimensional visualization technology for digital orthopedics in the reduction and fixation of intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3816-3820. |
| [13] | Sun Maji, Wang Qiuan, Zhang Xingchen, Guo Chong, Yuan Feng, Guo Kaijin. Development and biomechanical analysis of a new anterior cervical pedicle screw fixation system [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3821-3825. |
| [14] | Lin Wang, Wang Yingying, Guo Weizhong, Yuan Cuihua, Xu Shenggui, Zhang Shenshen, Lin Chengshou. Adopting expanded lateral approach to enhance the mechanical stability and knee function for treating posterolateral column fracture of tibial plateau [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3826-3827. |
| [15] | Zhu Yun, Chen Yu, Qiu Hao, Liu Dun, Jin Guorong, Chen Shimou, Weng Zheng. Finite element analysis for treatment of osteoporotic femoral fracture with far cortical locking screw [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3832-3837. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||