Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (27): 6978-6984.doi: 10.12307/2026.836
Previous Articles Next Articles
Force analysis of three-dimensional finite element models for single radius and multi radius prostheses during flexion and extension in total knee arthroplasty
Chen Dongxu1, Huang Dachao2, Hu Yang1, Li Zhaoxu1
- 1Nanxishan Hospital of Guangxi Zhuang Autonomous Region, Guilin 541000, Guangxi Zhuang Autonomous Region, China; 2School of Graduates, Guilin Medical University, Guilin 541000, Guangxi Zhuang Autonomous Region, China
-
Received:2025-10-17Accepted:2026-01-06Online:2026-09-28Published:2026-04-16 -
Contact:Li Zhaoxu, Chief physician, Nanxishan Hospital of Guangxi Zhuang Autonomous Region, Guilin 541000, Guangxi Zhuang Autonomous Region, China -
About author:Chen Dongxu, MS, Associate chief physician, Nanxishan Hospital of Guangxi Zhuang Autonomous Region, Guilin 541000, Guangxi Zhuang Autonomous Region, China -
Supported by:Guangxi Medical and Health Appropriate Technology Development and Promotion Project, No. S2023033 (to CDX); Guangxi Medical and Health Appropriate Technology Development and Promotion Project, No. S2024069 (to LZX); Guangxi Key Medical and Health Discipline Cultivation Project (to CDX)
CLC Number:
Cite this article
Chen Dongxu, Huang Dachao, Hu Yang, Li Zhaoxu. Force analysis of three-dimensional finite element models for single radius and multi radius prostheses during flexion and extension in total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(27): 6978-6984.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
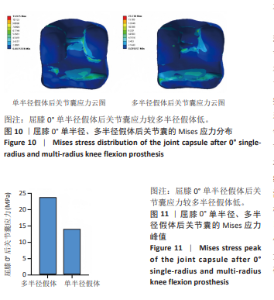
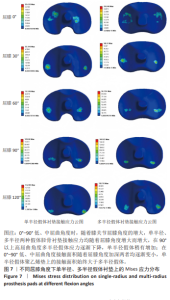
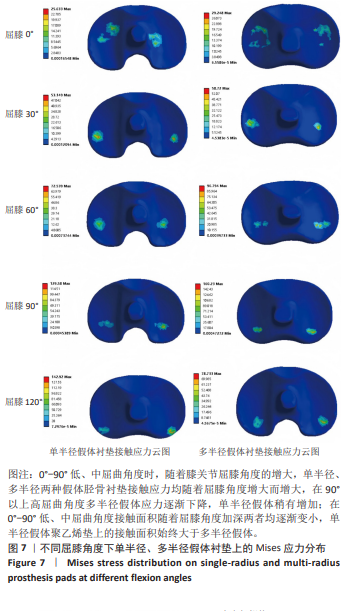
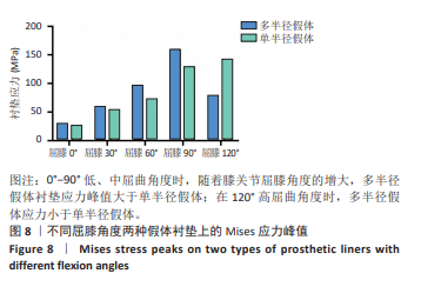
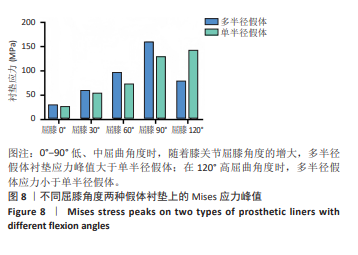
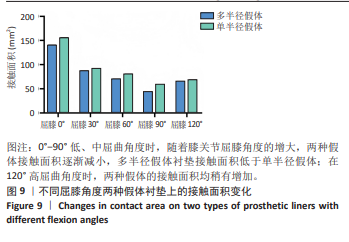
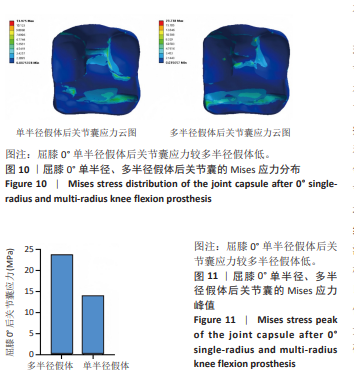
在0°-90°不同屈膝角度,全膝关节置换术后多半径假体应力变化趋势与单半径假体类似,当膝关节处于0°站立位时,垫片的应力峰值为29.25 MPa,至屈膝90°垫片应力峰值增加至160.23 MPa,增加幅度为447.80%;在90°-120°不同屈膝角度,垫片的应力峰值由最高160.23 MPa降至78.33 MPa,降低幅度为51.11%。 研究发现屈膝0°,单半径假体接触面积为156.83 mm2,多半径假体接触面积为141.36 mm2,在0°-90°不同屈膝角度,两种假体接触面积都有逐渐减少的趋势,在屈膝90°接触面积均降至最低,分别为59.78 mm2和44.05 mm2;在120°屈膝角度又有逐渐增大的趋势,分别增大至69.23 mm2和86.39 mm2。 2.3 两种假体后关节囊应力分布及应力峰值 为了解两种假体伸直位后关节囊的受力情况,测量了屈膝0°两种假体后关节囊的应力,结果显示在膝关节完全伸直状态,单半径假体后关节囊应力为14.00 MPa,多半径假体后关节囊应力为23.74 MPa,单半径假体后关节囊承受应力低于多半径假体(图10,11)。"
| [1] 杨彬,王上增,杨顺,等.生地黄提取物对膝骨关节炎兔软骨细胞凋亡的影响[J].中国医学科学院学报,2025,47(2):198-206. [2] SOMAIYA KJ, SAMAL S, BOOB MA. Physiotherapeutic intervention techniques for knee osteoarthritis: A systematic review. Cureus. 2024;16(3):e56817. [3] CROSS M, SMITH E, HOY D, et al. The global burden of hip and knee osteoarthritis: estimates from the global burden of disease 2010 study. Ann Rheum Dis. 2014; 73(7):1323-1330. [4] DE GRAE MNM, NASEHI A, DALURY DF, et al. Improved performance of cementless total knee arthroplasty (TKA)across international registries: a comparative review. Ir J Med Sci. 2025;194(2):675-681. [5] SKOU ST, ROOS EM, LAURSEN MB, et al. A Randomized, Controlled Trial of Total Knee Replacement. N Engl J Med. 2015;373(17):1597-1606. [6] EVANS JT, WALKER RW, EVANS JP, et al. How long does a knee replacement last? A systematic review and meta-analysis of case series and national registry reports with more than 15 years of follow-up. Lancet. 2019;393:655-663. [7] 乔凯, 田康, 陈琦, 等. 不同股骨假体屈曲角下人工膝关节生物力学特征的有限元分析[J]. 中华老年骨科与康复电子杂志,2025,11(2):65-76. [8] KHAN M, OSMAN K, GREEN G, et al. The epidemiology of failure in total knee arthroplasty: avoiding your next revision. Bone Joint J. 2016;98-B(1 Suppl A): 105-112. [9] PINSKEROVA V, IWAKI H, FREEMAN MAR. The shapes and relative movements of the femur and tibia at the knee. Orthopade. 2000;29 Suppl 1:S3-S5. [10] KESSLER O, DÜRSELEN L, BANKS S, et al. Sagittal curvature of total knee replacements predicts in vivo kinematics. Clin Biomech (Bristol). 2007;22(1): 52-58. [11] HAMILTON DF, BURNETT R, PATTON JT, et al. Implant design influences patient outcome after total knee arthroplasty: a prospective double-blind randomised controlled trial. Bone Joint J. 2015;97-b:64-70. [12] LARSEN B, JACOFSKY MC, JACOFSKY DJ. Quantitative, Comparative Assessment of Gait Between Single-Radius and Multi-Radius Total Knee Arthroplasty Designs. J Arthroplasty. 2015;30:1062-1067. [13] HINAREJOS P, PUIG-VERDIE L, LEAL J, et al. No differences in functional results and quality of life after single-radius or multiradius TKA. Knee Surg Sports Traumatol Arthrosc. 2016;24:2634-2640. [14] ŞENTÜRK F, DEMIREL M, YENIGÜN MY, et al. Functional outcome comparison of single-radius and multi-radius femur in total knee arthroplasty. Acta Orthop Traumatol Turc. 2025;59(3):156-163. [15] LEI T, JIANG Z, QIAN H, et al. Comparison of Single-Radius with Multiple-Radius Femur in Total Knee Arthroplasty: A Meta-Analysis of Prospective Randomized Controlled Trials. Orthop Surg. 2022;14(9):2085-2095. [16] LIU S, LONG H, ZHANG Y, et al. Meta-Analysis of Outcomes of a Single-Radius Versus Multi-Radius Femoral Design in Total Knee Arthroplasty. J Arthroplasty. 2016;31(3):646-654. [17] OLIVIU RC, ZAZGYVA A, SEPTIMIU S, et al. Mid-term results of total knee replacement with single-radius versus multi-radius posterior-stabilized implants. Acta Orthop Traumatol Turc. 2016;50(2):125-131. [18] MUGNAI R, DIGENNARO V, ENSINI A, et al. Can TKA design affect the clinical outcome? Comparison between two guided-motion systems. Knee Surg Sports Traumatol Arthrosc. 2014;22(3):581-589. [19] LUO Z, ZHOU K, WANG H, et al. Comparison between Mid-Term Results of Total Knee Arthroplasty with Single-Radius versus Multiple-Radii Posterior-Stabilized Prostheses. J Knee Surg. 2022;35(2):204-214. [20] 苏德君, 董万鹏, 董跃福, 等. 非对称型假体设计及全膝关节置换后的力学分析[J]. 中国组织工程研究,2025,29(3):510-516. [21] MONONEN ME, JURVELIN JS, KORHONEN RK. Implementation of a gait cycle loading into healthy and meniscectomised knee joint models with fibril-reinforced articular cartilage. Comput Methods Biomech Biomed Engin. 2015;18(2): 141-152. [22] WANG XH, LI H, DONG X, et al. Comparison of ISO 14243-1 to ASTM F3141 in terms of wearing of knee prostheses. Clin Biomech (Bristol). 2019;63:34-40. [23] WANG ZW, WEN L, LUAN YC, et al. Restoration of Joint Inclination in Total Knee Arthroplasty Offers Little Improvement in Joint Kinematics in Neutrally Aligned Extremities. Front Bioeng Biotechnol. 2021;9:673275. [24] FANG C, LUAN Y, WANG Z, et al. Moderate External Rotation of Tibial Component Generates More Natural Kinematics Than Internal Rotation After Total Knee Arthroplasty. Front Bioeng Biotechnol. 2022;10:910311. [25] 苏德君,曹雪坤,马洪浩,等.全膝关节置换假体的生物力学分析[J].中国运动医学杂志,2024,43(2):94-102. [26] 高辉,王晨艳,李志,等.不同屈曲状态下固定轴和移动轴膝关节胫-股关节的生物力学变化[J].太原理工大学学报,2021,52(1):144-150. [27] 李钟鑫,刘璐,高丽兰,等.人体全膝关节精细有限元模型建立及有效性验证[J].生物医学工程与临床,2020,24(5):501-507. [28] 章安琪,化昊天,蔡恬媛,等.全膝关节置换后疼痛:研究现状及趋势分析[J].中国组织工程研究,2026,30(3):795-804. [29] LIU S, LONG H, ZHANG Y, et al. Meta-Analysis of Outcomes of a Single-Radius Versus Multi-Radius Femoral Design in Total Knee Arthroplasty. J Arthroplasty. 2016;31(3):646-654. [30] FIRESTONE TP, EBERLE RW. Surgical management of symptomatic instability following failed primary total knee replacement. J Bone Jt Surg. 2006;88:80-84. [31] 任敬,巩航辉,郑世成,等.单半径假体全膝关节置换术对重度膝关节骨性关节炎患者膝关节活动度和术后并发症的影响[J].陕西医学杂志,2022, 51(10):1249-1252. [32] NOBLE PC, CONDITT MA, COOK KF, et al. The John Insall Award: Patient expectations affect satisfaction with total knee arthroplasty. Clin Orthop Relat Res. 2006;452:35-43. [33] 路凡,耿彬,滕飞,等.多半径与单半径全膝关节假体的研究进展[J].中国矫形外科杂志,2020,28(23):2162-2165. [34] BROWNE C, HERMIDA JC, BERGULA A, et al. Patellofemoral forces after total knee arthroplasty: effect of extensor moment arm. Knee. 2005;12(2):81-88. [35] OSTERMEIER S, STUKENBORG-COLSMAN C. Quadriceps force after TKA with femoral single radius. Acta Orthop. 2011;82(3):339-343. [36] EZECHIELI M, DIETZEK J, BECHER C, et al. The influence of a single-radius-design on the knee stability. Technol Health Care. 2012;20(6):527-534. [37] 彭正午,王波,黄添隆,等.单半径和多半径后稳定型膝关节假体疗效的Meta分析[J].中华关节外科杂志(电子版),2020,14(4):461-468. [38] ZHANG ZH, QI YS, WEI BG, et al. Application strategy of finite element analysis in artificial knee arthroplasty. Front Bioeng Biotechnol. 2023;11:1127289. [39] RYBICKI EF, SIMONEN FA, WEIS JR EB. On the mathematical analysis of stress in the human femur. J Biomech. 1972;5(2):203-215. [40] BREKELMANS WAM, POORT HW, SLOOFF T. A new method to analyse the mechanical behaviour of skeletal parts. Acta Orthop Scand. 1972;43(5):301-317. [41] PRICE AJ, ALVAND A, TROELSEN A, et al. Knee replacement. Lancet. 2018; 392(10158):1672-1682. [42] WANG JY, QI YS, BAO HRC, et al. The effects of different repair methods for a posterior root tear of the lateral meniscus on the biomechanics of the knee: a finite element analysis. J Orthop Surg Res. 2021;16(1):296. [43] CASTELLARIN G, BORI E, RAPALLO L, et al. Biomechanical analysis of different levels of constraint in TKA during daily activities. Arthroplasty. 2023;5(1):3. [44] INNOCENTI B, BORI E, PIANIGIANI S. Biomechanical Analysis of the Use of Stems in Revision Total Knee Arthroplasty. Bioengineering (Basel). 2022;9(6):259. [45] PARK HJ, BAE TS, KANG SB, et al. A three-dimensional finite element analysis on the effects of implant materials and designs on periprosthetic tibial bone resorption. PLoS One. 2021;16(2):e0246866. [46] HARWIN SF, ISSA K, GIVEN K, et al. Clinical and patient-reported outcomes of primary TKA with a single-radius design. Orthopedics. 2013;36:e877-e882. [47] HUNT NC, GHOSH KM, BLAIN AP, et al. How does laxity after single radius total knee arthroplasty compare with the native knee? J Orthop Res. 2014;32: 1208-1213. [48] JO AR, SONG EK, LEE KB, et al. A comparison of stability and clinical outcomes in single-radius versus multi-radius femoral design for total knee arthroplasty. J Arthroplasty. 2014;29: 2402-2406. [49] 姬林松.不同型号膝关节PS型假体匹配的三维动态有限元分析[D].昆明:昆明医科大学,2016. [50] BAEK JH, LEE SC, CHOI K, et al. Long-term survivorship of total knee arthroplasty with a single-radius, high-flexion posterior stabilized prosthesis. Knee. 2021; 30:275-282. |
| [1] | Liu Wenlong, Dong Lei, Xiao Zhengzheng, Nie Yu. Finite element analysis of tibial prosthesis loosening after fixed-bearing unicompartmental knee arthroplasty for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2191-2198. |
| [2] | Zheng Wangyang, Fei Ji, Yang Di, Zhao Lang, Wang Lingli, Liu Peng, Li Haiyang. Finite element analysis of the force changes of the supraspinatus tendon and glenohumeral joint during the abduction and flexion of the humerus [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2199-2207. |
| [3] | Cai Qirui, Dai Xiaowei, Zheng Xiaobin, Jian Sili, Lu Shaoping, Liu Texi, Liu Guoke, Lin Yuanfang. Mechanical effects of Long’s traction orthopedic method on cervical functional units: quantitative analysis of biomechanical model of head and neck [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2208-2216. |
| [4] | Rao Jingcheng, Li Yuwan, Zheng Hongbing, Xu Zhi, Zhu Aixiang, Shi Ce, Wang Bing, Yang Chun, Kong Xiangru, Zhu Dawei. Biomechanical differences between the new proximal femoral stable intramedullary nail and traditional intramedullary nail#br# [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2217-2225. |
| [5] | Chen Long, Wang Xiaozhen, Xi Jintao, Lu Qilin. Biomechanical performance of short-segment screw fixation combined with expandable polyetheretherketone vertebral body replacement in osteoporotic vertebrae [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2226-2235. |
| [6] | Yan Xiangning, Chen Lei, Chen Yonghuan, Wang Chao, Li Xiaosheng. Influence of different depths and loads on knee joint mechanics and peripheral muscle force characteristics during squatting [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2236-2247. |
| [7] | Zhang Nan, Meng Qinghua, Bao Chunyu. Characteristics and clinical application of ankle joint finite element models [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2343-2349. |
| [8] | He Yixiang, Qiao Wanjia, Wang Wenji. Effectiveness and safety of tranexamic acid versus epsilon-aminocaproic acid in total hip and knee arthroplasties: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2361-2369. |
| [9] | Zhang Zizheng, Luo Wang, Liu Changlu. Application value of finite element analysis on unicompartmental knee arthroplasty for medial knee compartmental osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2313-2322. |
| [10] | Zhang Xianxu, Ma Zhong, Liu Xin, Huang Lei, Shen Wenxiang, Luo Zhiqiang . Lumbar fusion combined with unilateral fixation for lumbar degenerative diseases: biomechanics, technical evolution, and clinical applications [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2334-2342. |
| [11] | Chen Huiting, Zeng Weiquan, Zhou Jianhong, Wang Jie, Zhuang Congying, Chen Peiyou, Liang Zeqian, Deng Weiming. Tail anchoring technique of vertebroplasty in treatment of osteoporotic vertebral compression fractures with intravertebral cleft: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2145-2152. |
| [12] | Zeng Xuan, Weng Rui, Ye Shicheng, Tang Jiadong, Mo Ling, Li Wenchao. Two lumbar rotary manipulation techniques in treating lumbar disc herniation: a finite element analysis of biomechanical differences [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2153-2161. |
| [13] | Cheng Qisheng, Julaiti·Maitirouzi, Xiao Yang, Zhang Chenwei, Paerhati·Rexiti. Finite element analysis of novel variable-diameter screws in modified cortical bone trajectory of lumbar vertebrae [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2162-2171. |
| [14] | Wu Hongxu, Liu Xuanyu, Wang Taoyu, Wang Shiyao, Cheng Jingyi, Zhang Mingwen, Zhang Yinxia, Liu Zhihua, Wang Xiaojie. Finite element simulation of scoliosis with muscle unit introduction: verification of correction effect under bidirectional load [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2172-2181. |
| [15] | Liu Jiafu, Ren Ruxia, Liao Zhouwei, Zhou Xiali, Wu Yihong, Zhang Shaoqun. Three-dimensional finite element analysis of cervical spine biomechanical characteristics in a rat model of cervical vertigo [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2182-2190. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||