Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (33): 5397-5404.doi: 10.3969/j.issn.2095-4344.2346
Previous Articles Next Articles
Efficacy and safety of percutaneous kyphoplasty versus posterior short-segment fixation with vertebra augmentation for Kummell’s disease: a meta-analysis
Zhan Fangbiao1, Xie Lizhong1, Zou Xinsen2, Long Jie1, Cheng Jun1, Zhang Xianwei3
1Department of Orthopedics, 2Intensive Care Unit, 3Department of Sleep Medicine, Three Gorges Hospital (Chongqing Three Gorges Central Hospital), Chongqing University, Chongqing 404000, China
-
Received:2020-02-10Revised:2020-02-18Accepted:2020-03-18Online:2020-11-28Published:2020-10-15 -
Contact:Cheng Jun, Associate chief physician, Department of Orthopedics, Three Gorges Hospital (Chongqing Three Gorges Central Hospital), Chongqing University, Chongqing 404000, China Zhang Xianwei, Attending physician, Department of Sleep Medicine, Three Gorges Hospital (Chongqing Three Gorges Central Hospital), Chongqing University, Chongqing 404000, China -
About author:Zhan Fangbiao, Doctoral candidate, Associate chief physician, Department of Orthopedics, Three Gorges Hospital (Chongqing Three Gorges Central Hospital), Chongqing University, Chongqing 404000, China
CLC Number:
Cite this article
Zhan Fangbiao, Xie Lizhong, Zou Xinsen, Long Jie, Cheng Jun, Zhang Xianwei. Efficacy and safety of percutaneous kyphoplasty versus posterior short-segment fixation with vertebra augmentation for Kummell’s disease: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5397-5404.
share this article

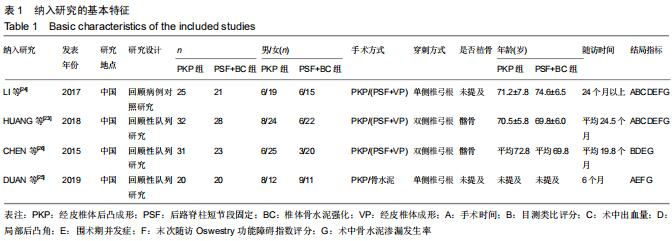
2.1 文献检索结果分析 初步检索共得到1 256篇文献,EndNote、NoteExpress软件查重删除重复文献(n=436),依据纳入排除标准阅读标题、摘要后排除113篇,初步纳入文献23篇。经阅读全文后最终纳入4篇文献进行Meta分 析[23-26],均为已公开发表的临床对照研究,其中1篇为回顾性病例对照研究,3篇为回顾性队列研究,共200例患者,其中PKP组108例,PSF+BC组92例。文献筛选流程见图1,纳入文献基本情况见表1。由2位作者根据NOS量表分别对纳入的4篇文献进行质量评价,从病例选择、对照、结局指标3个方面进行评价,6星及以上为高质量文献,回顾性临床对照研究文献评分分别为6星1篇,7星2篇,8星1篇。 "
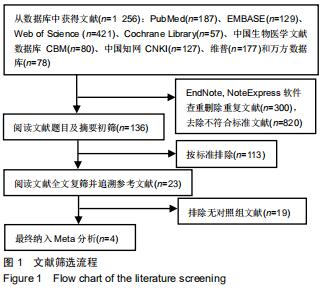
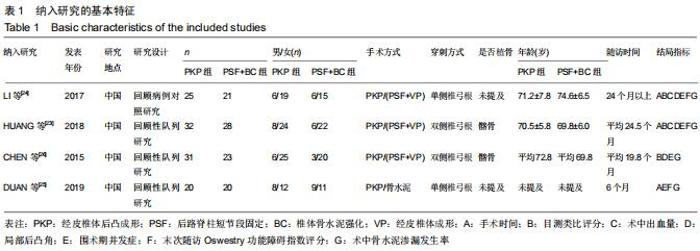
2.1 文献检索结果分析 初步检索共得到1 256篇文献,EndNote、NoteExpress软件查重删除重复文献(n=436),依据纳入排除标准阅读标题、摘要后排除113篇,初步纳入文献23篇。经阅读全文后最终纳入4篇文献进行Meta分 析[23-26],均为已公开发表的临床对照研究,其中1篇为回顾性病例对照研究,3篇为回顾性队列研究,共200例患者,其中PKP组108例,PSF+BC组92例。文献筛选流程见图1,纳入文献基本情况见表1。由2位作者根据NOS量表分别对纳入的4篇文献进行质量评价,从病例选择、对照、结局指标3个方面进行评价,6星及以上为高质量文献,回顾性临床对照研究文献评分分别为6星1篇,7星2篇,8星1篇。 "
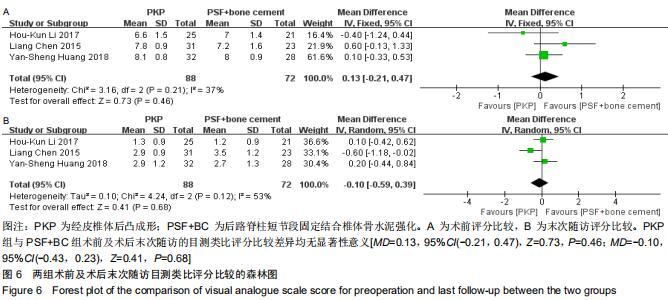
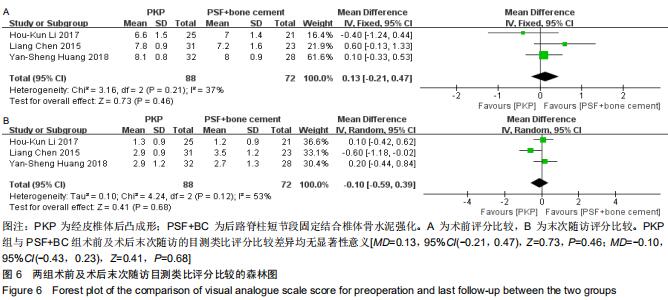
2.2.5 目测类比评分 纳入的4篇文献中3篇详细比较了术前及末次随访目测类比评分[23-24,26]。文献间术前目测类比评分无异质性(Chi2=3.16,df=2,I2=37%,P=0.21),选择固定效应模型进行Meta分析;文献间术后末次随访目测类比评分有异质性(Chi2=4.24,df=2,I2=53%,P=0.12),选择随机效应模型进行Meta分析。两组术前与术后末次随访的目测类比评分比较差异均无显著性意义[MD=0.13,95%CI(-0.21,0.47),Z=0.73,P=0.46;MD=-0.10,95%CI(-0.43,0.23),Z=0.41,P=0.68],见图6。 "
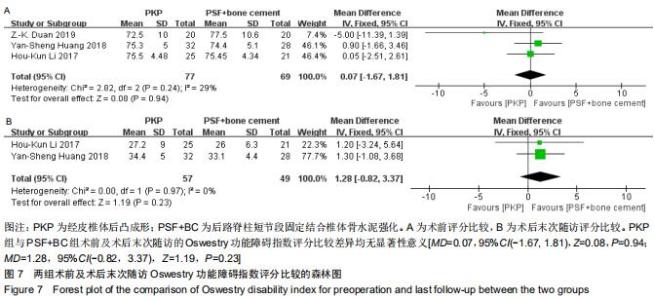
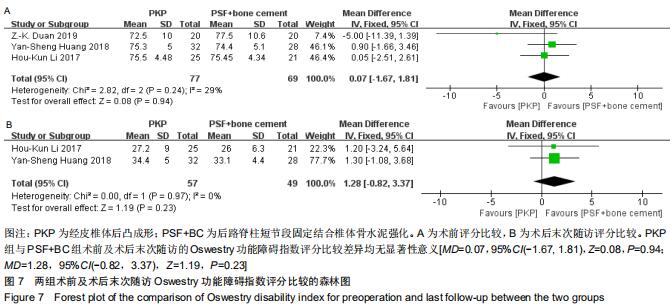
2.2.6 Oswestry功能障碍指数评分 纳入的4篇文献中3篇详细比较了术前及术后末次随访Oswestry功能障碍指数评分[23-25]。文献间术前Oswestry功能障碍指数评分无异质性(Chi2=2.82,df=2,I2=29%,P=0.24),选择固定效应模型进行Meta分析。两组术前Oswestry功能障碍指数评分比较差异无显著性意义[MD=0.07,95%CI(-1.67, 1.81),Z=0.08,P=0.94],见图7A。因考虑到DUAN等[25]报道的Oswestry功能障碍指数末次随访时间为6个月,而HUANG等[23]和LI等[24]报道的Oswestry功能障碍指数术后末次随访时间为24个月左右,若纳入DUAN等报道的Oswestry功能障碍指数进行Meta分析可能结果不可靠,故纳入2篇文献进行亚组分析[23-24]。文献间术后末次随访Oswestry功能障碍指数评分无异质性(Chi2=0.00,df=1,I2=0%,P=0.97),选择随机固定模型进行Meta分析。两组末次随访的Oswestry功能障碍指数评分比较差异无显著性意义[MD=1.28,95%CI(-0.82,3.37),Z=1.19,P=0.23],见图7B。 "
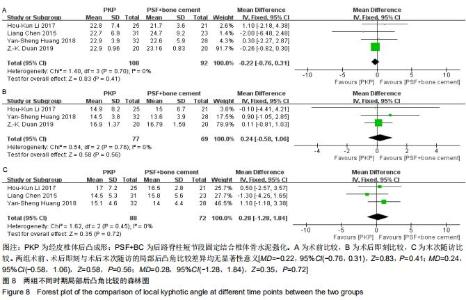
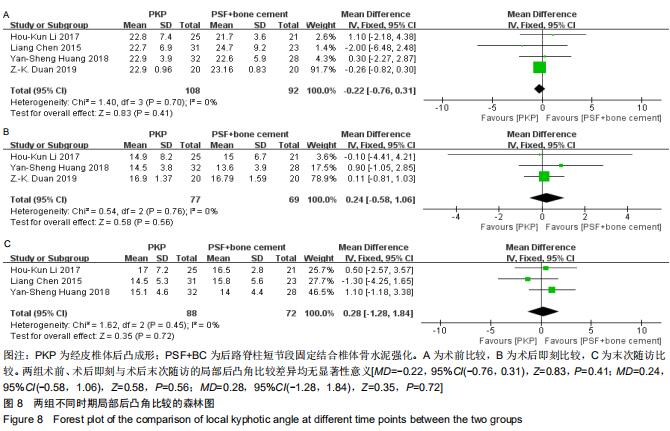
2.2.7 局部后凸角 纳入的4篇文献均详细比较了术前局部后凸角[23-26],文献间无异质性(Chi2=1.40,df=3,I2=0%,P=0.70),选择固定效应模型进行Meta分析。两组术前的局部后凸角比较差异无显著性意义[MD=-0.22,95%CI(-0.76, 0.31),Z=0.83,P=0.41],见图8A。纳入的4篇文献中本3篇比较了术后即刻局部后凸角[23-25],文献间无异质性(Chi2=0.54,df=2,I2=0%,P=0.76),选择固定效应模型进行Meta分析。两组术后即刻的局部后凸角比较差异无显著性意义[MD=0.24,95%CI(-0.58,1.06),Z=0.58,P=0.56],见图8B。纳入的4篇文献中3篇比较了术后末次随访局部后凸角[23-24,26],文献间无异质性(Chi2=1.62,df=2,I2=0%,P=0.45),选择固定效应模型进行Meta分析。两组术后末次随访的局部后凸角比较差异无显著性意义[MD=0.28,95%CI(-1.28,1.84),Z=0.35,P=0.72],见图8C。 "
|
[1] KIM YC, KIM YH, HA KY. Pathomechanism of intravertebral clefts in osteoporotic compression fractures of the spine.Spine J. 2014;14:659-666.
[2] WANG G, YANG H, CHEN K. Osteoporotic vertebral compression fractures with an intravertebral cleft treated by percutaneous balloon kyphoplasty.J Bone Joint Surg Br.2010;92:1553-1557.
[3] FORMICA M, BASSO M, CAVAGNARO L,et al. Kümmell disease: illustrative case for definition criteria.Spine J. 2016;16(10):e707-e708.
[4] CHOU LH, KNIGH RQ. Idiopathic avascular necrosis of a vertebral body.Case report and literature review.Spine (Phila Pa 1976). 1997; 22(16):1928-1932.
[5] FREEDMAN BA, HELLER JG. Kummel disease:a not-so-rare complication of osteoporotic vertebral compression fractures.J Am Board Fam Med.2009;22(1):75-78.
[6] JANG JS, KIM DY, LEE SH. Efficacy of percutaneous vertebroplasty in the treatment of intravertebral pseudarthrosis associated with noninfected avascular necrosis of the vertebral body.Spine (Phila Pa 1976).2003;28(14):1588-1592.
[7] PARK JW, PARK JH, JEON HJ, et al. Kümmell's Disease Treated with Percutaneous Vertebroplasty: Minimum 1 Year Follow-Up.Korean J Neurotrauma.2017;13(2):119-123.
[8] LI H, LIANG CZ, CHEN QX. Kümmell’s disease,an uncommon and complicated spinal disorder:a review.J Int Med Res. 2012;40(2):406-414.
[9] LU W, WANG L, XIE C, et al. Analysis of percutaneous kyphoplasty or short-segmental fixation combined with vertebroplasty in the treatment of Kummell disease.J Orthop Surg Res.2019;14(1):311.
[10] ZHANG X, HU W, YU J, et al. An effective treatment option for kümmell disease with neurological deficits:Modified transpedicular subtraction and disc osteotomy combined with long‑segment fixation.Spine (Phila Pa 1976).2016;41(15):E923-930.
[11] RUAN J, GONG X, KONG J, et al. Effect of B vitamin (folate, B6, and B12) supplementation on osteoporotic fracture and bone turnover markers:A meta-analysis.Med Sci Monit.2015;21:875-881.
[12] CHEN GD, LU Q, WANG GL, et al. Percutaneous kyphoplasty for kümmell disease with severe spinal canal stenosis. Pain Physician. 2015;18(6):E1021-1028.
[13] MATZAROGLOU C, GEORGIOU CS, PANAGOPOULOS A, et al. Kümmell's disease:Clarifying the mechanisms and patients' inclusion criteria.Open Orthop J.2014;8:288-297.
[14] CHEN F, XIA YH, CAO WZ, et al. Percutaneous kyphoplasty for the treatment of spinal metastases.Oncol Lett.2016;11(3):1799-1806.
[15] LIU H, ZHANG J, LIANG X, et al. Distribution Pattern Making Sense:Patients Achieve Rapider Pain Relief with Confluent Rather Than Separated Bilateral Cement in Percutaneous Kyphoplasty for Osteoporotic Vertebral Compression Fractures.World Neurosurg. 2019;126:e1190-e1196.
[16] ZHANG Y, LIU H, HE F, et al. Safety and efficacy of percutaneous kyphoplasty assisted with O-arm navigation for the treatment of osteoporotic vertebral compression fractures at T6 to T9 vertebrae.Int Orthop.2020;44(2):349-355.
[17] NIU J, SONG D, ZHOU H, et al. Percutaneous Kyphoplasty for the Treatment of Osteoporotic Vertebral Fractures With Intravertebral Fluid or Air.Clin Spine Surg.2017;30(8):367-373.
[18] KAWAGUCHI S,HORIGOME K,YAJIMA H,et al.Symptomatic relevance of intravertebral cleft in patients with osteoporotic vertebral fracture.J Neurosurg Spine.2010;13(2):267-275.
[19] WEI P, YAO Q, XU Y, et al. Percutaneous kyphoplasty assisted with/without mixed reality technology in treatment of OVCF with IVC:a prospective study.J Orthop Surg Res.2019;14(1):255.
[20] SUDO H, ITO M, KANEDA K, et al. Anterior decompression and strut graft versus posterior decompression and pedicle screw fixation with vertebroplasty for osteoporotic thoracolumbar vertebral collapse with neurologic deficits.Spine J.2013;13(12):1726-1732.
[21] UCHIDA K, NAKAJIMA H, YAYAMA T, et al. Vertebroplasty-augmented short-segment posterior fixation of osteoporotic vertebral collapse with neurological deficit in the thoracolumbar spine: comparisons with posterior surgery without vertebroplasty and anterior surgery.J Neurosurg Spine.2010;13(5):612-621.
[22] WAGNER AL, BASKURT E. Refracture with cement extrusion following percutaneous vertebroplasty of large interbody cleft.AJNR Am J Neuroradiol.2006;27(1):230-231.
[23] HUANG YS, HAO DJ, FENG H, et al. Comparison of Percutaneous Kyphoplasty and Bone Cement-Augmented Short-Segment Pedicle Screw Fixation for Management of Kümmell Disease.Med Sci Monit. 2018;24:1072-1079.
[24] LI HK, HAO DJ, YANG JS, et al. Percutaneous kyphoplasty versus posterior spinal fixation with vertebroplasty for treatment of Kümmell disease.Medicine (Baltimore). 2017;96(51):e9287.
[25] DUAN ZK, ZOU JF, HE XL, et al. Bone-filling mesh container versus percutaneous kyphoplasty in treating Kümmell’s disease.Arch Osteoporos.2019;14(1):109.
[26] CHEN L, DONG R, GU Y, et al. Comparison between Balloon Kyphoplasty and Short Segmental Fixation Combined with Vertebroplasty in the Treatment of Kümmell’s Disease.Pain Physician. 2015;18(4):373-381.
[27] WANG G, YANG H, MENG B, et al. Post-traumatic osteoporotic vertebral osteonecrosis treated using balloon kyphoplasty.Clin Neurosci. 2011;18(5):664-668.
[28] WU AM, CHI YL, NI WF. Vertebral compression fracture with intravertebral vacuum cleft sign: Pathogenesis,image,and surgical intervention.Asian Spine J.2013;7(2):148-155.
[29] PFLUGMACHER R, SCHROEDER RJ, KLOSTERMANN CK. Incidence of adjacent vertebral fractures in patients treated with balloon kyphoplasty:Two years' prospective follow-up.Acta Radiol. 2006;47(8):830-840.
[30] XIA YH, CHEN F, ZHANG L, et al. Percutaneous kyphoplasty treatment evaluation for patients with Kümmell disease based on a two‑year follow‑up.Exp Ther Med.2018;16(4):3617-3622.
[31] PIAO M, DARWONO AB, ZHU K, et al. Extrapendicular Approach of Unilateral Percutaneous Vesselplasty for the Treatment of Kummell Disease.Int J Spine Surg.2019;13(2):199-204.
[32] 王小刚,杨 彬,王亚寒,等.单侧穿刺椎体成形术治疗Kummell病的疗效观察[J].中国矫形外科杂志,2019,27(1):86-88.
[33] 蒋杰,张勇.单侧穿刺经皮椎体后凸成形与椎体成形骨水泥注射治疗Kummell病的对比[J].中国组织工程研究,2019,23(22):3481-3487.
[34] WANG H, DING W. Posterior Vertebral Column Resection Through Unilateral Osteotomy Approach for Old Lumbar Fracture Combined with Kummell Disease.World Neurosurg.2018;109:147-151.
[35] LEE SH, CHO DC, SUNG JK. Catastrophic intramedullary hematoma following Kümmell’s disease with large intravertebral cleft.Spine J. 2008;8(6):1007-1010.
[36] LEE SH, KIM ES, EOH W. Cement augmented anterior reconstruction with short posterior instrumentation:A less invasive surgical option for Kümmell’s disease with cord compression.J Clin Neurosci. 2011;18(4): 509-514.
[37] HUANG YS, GE CY, FENG H, et al. Bone Cement-Augmented Short-Segment Pedicle Screw Fixation for Kümmell Disease with Spinal Canal Stenosis.Med Sci Monit.2018;24:928-935.
[38] HUANG Y, PENG M, HE S, et al. Clinical efficacy of percutaneous kyphoplasty at the hyperextension position for the treatment of osteoporotic Kümmell disease.Clin Spine Surg.2016;29(4):161-166.
[39] WANG W, LIU Q, LIU WJ, et al. Different Performance of Intravertebral Vacuum Clefts in Kümmell's Disease and Relevant Treatment Strategies. Orthop Surg.2020;12(1):199-209.
[40] ZHANG GQ, GAO YZ, ZHENG J, et al. Posterior decompression and short segmental pedicle screw fixation combined with vertebroplasty for Kümmell’s disease with neurological deficits. Exp Ther Med. 2013; 5(2):517-522.
[41] YANG DL, YANG SD, CHEN Q, et al. The treatment evaluation for osteoporotic Kümmell disease by modified posterior vertebral column resection:Minimum of one-year follow-up.Med Sci Monit. 2017;23: 606-612.
[42] WANG F, WANG D, TAN B, et al. Comparative study of modified posterior operation to treat Kümmell’s disease.Medicine (Baltimore). 2015;94(39):e1595. [43] LIM J, CHOI SW, YOUM JY, et al. Posttraumatic Delayed Vertebral Collapse:Kummell’s Disease.J Korean Neurosurg Soc.2018;61(1):1-9. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [8] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [9] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [10] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [11] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [12] | Yao Rubin, Wang Shiyong, Yang Kaishun. Minimally invasive transforaminal lumbar interbody fusion for treatment of single-segment lumbar spinal stenosis improves lumbar-pelvic balance [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1387-1392. |
| [13] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [14] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [15] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||