Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (8): 1280-1286.doi: 10.3969/j.issn.2095-4344.2216
Previous Articles Next Articles
Finite element analysis on the biomechanical changes of patellar tendinitis
Zhou Yu, Long Xiaoan, Li Ning, Wang Chun
- Chengdu Sport University, Chengdu 610041, Sichuan Province, China
-
Received:2019-05-30Revised:2019-06-04Accepted:2019-07-10Online:2020-03-18Published:2020-01-23 -
Contact:Wang Chun, Professor, Doctoral supervisor, Chengdu Sport University, Chengdu 610041, Sichuan Province, China -
About author:Zhou Yu, Master candidate, Chengdu Sport University, Chengdu 610041, Sichuan Province, China -
Supported by:the Key Research & Development Project of Sichuan Provincial Department of Science and Technology, No. 2017SZ0018; the Sports Science and Health Innovation Project of Chengdu Sport University, No. CX17B05
CLC Number:
Cite this article
Zhou Yu, Long Xiaoan, Li Ning, Wang Chun. Finite element analysis on the biomechanical changes of patellar tendinitis[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(8): 1280-1286.
share this article
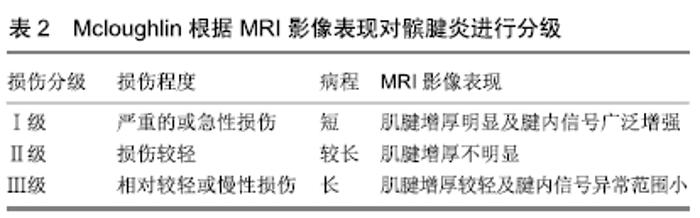
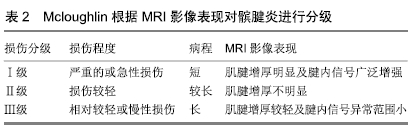
2.1 有限元法在髌腱炎损伤机制研究中的应用 利用有限元法能够实现对髌腱生物力学功能特点和损伤机制等的分析及评估。起先,RICHARDS等[11]在1996年为确定跳台动作和髌骨肌腱炎之间是否存在预测关系,定量分析排球扣球和跳台动作中下肢的动力学变化,通过有限元模型的逻辑回归分析发现,扣球和跳台起跳阶段的垂直地面反作用力是预测肌腱炎的重要指标,即胫骨外扭转力矩变化使髌腱发生变形和位移,为髌腱炎等损伤的出现提供了力学依据。BORK等[12]通过研究跑鞋几何形状和材料的关系对下肢过度使用的疾病综合征进行有限元动态模拟,了解到胫骨疲劳性骨折和髌骨肌腱病可能是重复强迫后足内旋在地面接触运动阶段产生过度使用损伤的结果,研究发现髌腱周围压力分布不均易产生疼痛。SLOTKIN等[13]对青少年膝关节发育状况进行了有限元模拟,通过三维重建发现膝关节周围的生长变化、生物力学和解剖结构增加了前膝关节疼痛诊断和治疗的复杂性,该模型旨在非手术治疗中通过改善神经-肌肉控制和恢复下肢动力链功能来缓解前膝关节疼痛。综合以上研究结果表明,利用有限元法对髌腱等膝关节疾病进行生物力学特征分析,可以模拟髌腱疼痛产生的风险因素,进一步验证与膝关节伸肌结构的高张力和高负荷显著相关,同时髌腱炎的产生与增加胫骨外侧扭转力矩和膝关节加深屈曲角度有相关性。运用有限元法对髌腱承受较高张力的危险因素有以下2方面。 膝部解剖学特点及相关组织病变是导致髌腱张力增加的内在因素。已有相关实验证明导致髌腱炎疼痛产生的原因,与股四头肌腱高张力和髌骨位移改变相关[14-15]。SCATTONE等[16]对股骨进行有限元模型分析,验证跳跃着陆时髌骨矢状面位置改变对伴有和不伴有髌骨肌腱病变运动员下肢生物力学、髌腱力学特性和疼痛的直接影响,结果表明患髌骨肌腱炎运动员比未患髌骨肌腱炎运动员表现出更高的髌骨初始位置,所以在着陆过程中增加躯干屈曲使髌骨下移,可能是减少跳跃运动员肌腱过载的一个重要策略。SLANE等[17]通过有限元分析对股骨进行模拟,指出股内收肌紧张痉挛是导致髌腱张力增加的一个重要原因。BODEN等[18]利用MRI影像学及三维重建探讨了下肢骨骼排列是否影响,指出如果膝关节不稳定经常左右摇摆,肌腱受到不必要的压力,不加以纠正会延长髌腱损伤病程,见表2。 "

根据髌腱所处的解剖位置,其如同弓弦般紧张于髌尖及胫骨转子之间,长期跳跃或膝部屈曲落地模式不当(内翻或外翻动作)反复牵拉引起髌腱过高张力,从而导致髌腱炎。EDAMA等[19]为探讨影响髌腱炎发生机制的解剖学因素,调查了50具尸体上的100条腿,对髌下缘的形态、髌腱附着部位、髌腱长度和病程进行了详细研究,并利用有限元模拟膝跳跃运动力学过程,在对髌下缘呈尖型和前型2种类型进行模拟跳跃运动中,髌骨后倾导致膝关节屈曲时,髌下缘和髌腱近后表面受到撞击,提示这可能导致损伤;另一方面,对于后型和钝型,提示髌下缘后突肌腱纤维可能存在较强的拉应力,有限元分析验证后与标本结果一致。SCATTONE SILVA等[20]验证跳跃着陆时改变矢状面躯干位置对伴有和不伴有髌骨肌腱病变运动员下肢生物力学、髌腱拉应力和疼痛的直接影响,有限元分析结果显示:躯干屈曲越大髌腱拉应力越低;但将膝关节内、外翻应力加载作为研究变量得出:矢状面峰值运动学、动力学的数值变化曲线及着陆时髌骨肌腱拉应力峰值增加、膝关节伸肌力矩增加,运动员疼痛明显加重,说明内、外翻动作使髌腱的应力增加。MCCLAY等[21]探讨了篮球运动员患髌骨肌腱炎和踝关节扭伤的病因及力学关系,采用有限元分析软件进行下肢关节运动学和结构参数的典型运动动作模拟,如在膝内翻上篮落地和侧向运动中发现,胫骨及髌韧带周围应力在内翻落地时显著增大,即应力峰值出现在内翻落地状态,验证力学状态的真实性。JOHNSTON等[22]探讨了自行车运动对膝关节力学的影响,发现由于膝关节在蹬踏时多处于内、外翻模式并在踏板处产生扭矩,导致肌腱等软组织易受伤。综上研究结果显示,跳跃时内、外翻会使髌腱承受较大的应力分布,在张力的幅值和时间方面都有增加,推测长期表现为膝内、外翻模式易诱发髌腱炎。 2.2 有限元法在髌腱炎治疗方法研究中的应用 髌腱炎(跳跃者膝)最主要的表现为训练中跑、跳或蹲时出现膝关节髌腱-腱骨结合部的疼痛[23]。临床应用保守治疗和手术治疗2种手段来缓解髌腱炎的疼痛。随着数字化技术的发展,计算机建模功能的提升帮助有限元分析软件更强大和完善。有限元分析法在髌腱炎缓解疼痛和康复方面起到了重要指治疗导策略。 2.2.1 保守治疗 对髌腱痛处进行适当的按摩,可松解已产生粘连的髌腱前面与深筋膜之间的结缔组织(腱围),改善血循,促进组织液和静脉血回流,有助于降低肌腱内部组织的压力[24]。按摩手法是治疗髌腱炎的方法之一,分髌底前缘推压和胫骨转子刮拨。华英汇[25]在研究股内斜肌/股外侧肌髌腱末端受力的有限元分析中提出,随着髌底前缘粘连层的增加,髌腱屈曲度减小,髌腱应力也随之增加;同时,将胫骨结节打磨光滑,髌腱下端活动度增加,应力曲线呈下降趋势。因此,在对髌腱治疗的同时采用使患者有胀感的力度对股内斜肌和股外侧肌进行按摩,可缓解髌腱应力分布。DAN等[26]利用有限元法分析髌骨肌腱病变内在生物力学危险因素的评价中指出,通过增加髌腱牵引力线与股四头肌力矩的夹角可以直接减小对髌腱的应力,同时增加髌腱中心点角和降低髌骨高度测得的髌腱应力。TYLER等[27]利用有限元法成功证明了髌骨矢状位倾斜对髌韧带压力的影响,运用计算机描述一种新的测量髌骨股骨关系的方法,称为前后髌骨倾斜,即膝关节X射线侧位片上髌骨关节面与股骨前骨干轴之间形成的角度,研究结果显示与对照组相比,髌腱病变患者的前后倾斜平均减少了4.5°,这种差异的存在为生物力学提供了解释。刘波[28]通过动物实验对髌腱进行归一化滞后环面积、循环蠕变和剩余蠕变、应力松弛、生理应力范围的弹性测试,发现电针治疗可以增加试件的部分塑性变形,加快应力松弛,提升生理应力范围的弹性,这些变化对末端病治疗有积极意义。 目前临床上治疗髌腱炎使用针灸、超声波等治疗3个月无效时,建议采用体外冲击波治疗。LEITGEB等[29]对髌腱炎进行冲击波模拟的有限元分析,当髌腱的负压达到3.0 Pa、频率为10 Hz时对膝部应变能量的统计,模拟分析缩小冲击波作用在膝部的范围,显示多脉冲击波产生的累积效应对髌腱的治疗效果更佳。 2.2.2 手术治疗 髌腱腱围剥离及髌腱变性部分切除是治疗髌腱炎的主要有创治疗手段,此治疗手段的生物力学依据多由有限元法提供。临床上的髌腱腱围剥离是为了缓解髌腱承受的过高张力。BALDWIN等[30]在膝关节置换力学评估的动态有限元仿真中提出,髌腱柔韧性的恢复是膝关节损伤康复的难题,即使外科采用膝关节假体的内固定器对髌腱有一定解压作用,但术后步态姿势的异常仍会导致髌腱炎的产生。仝路等[31]在膝关节三维数字化模型的研究中,列举了国内南方医科大学钟世镇教授率先开展“虚拟中国人”人体切片建模的研究工作,并利用中国男性1号的膝关节断层切片图像建立了可供力学分析和假体设计的膝关节三维模型。有限元分析主要针对膝关节解剖参数的研究,临床上应用三维重建技术分析研究膝关节解剖结构及软组织和内部髓腔的大小和运动轨迹等数据,对国内膝关节假体的设计和选择具有重要意义。吴阳等[32]利用关节镜下射频治疗顽固性髌腱腱病,结果显示射频治疗能有效改善患者的膝前痛症状,极大提高患者膝关节功能。有限元研究发现,肌腱炎症不仅与反复劳损有关,还与体质量指数、足弓高度、错误动作模式有一定的联系[33]。同时剥离后的髌腱-腱围能降低粘连在髌腱上的应力,缓解集中在髌骨下缘的张力所导致的牵拉疼痛[34]。因此临床上对髌腱炎的治疗首先考虑保守方式,如果髌腱粘连严重或变性则行切除(剥离),还应考虑结构的完整性。关于髌骨肌腱病变的病因是一种应力屏蔽/压缩现象还是一种重复的微超载发病机制的争论仍在继续。然而,有足够的临床证据排除压迫性病因,有足够的生物力学尸体证据和有限元模型支持重复性微过载,符合临床研究中已知的过载外在危险因素支持重复性微过载的病因。利用有限元分析探讨髌骨肌腱病变和伸肌机制的生物力学中,假设识别潜在危险因素即将髌骨的外侧面视为一个杠杆,两侧的力矩必须保持平衡,通过外侧平面X射线片对试验组(髌骨肌腱病变患者)和对照组(非髌骨肌腱病变患者)分析了髌骨相关杠杆测量值的差异,发现试验组髌腱-胫骨结节结合部力矩明显大于对照组[26]。HAYES等[35]指出,有限元法在肌腱尺寸的精准测量已被证明有助于肌腱部分切除和肌腱移植的开展,数字化模拟出肌腱的应力和应变,对于判断正常肌腱和退化肌腱之间的差异具有重要意义。王大忠 等[36]通过建立含有模拟韧带、肌肉等部分软组织结构的膝关节有限元模型,采用三维步态分析仪采集试验对象运动中关节运动轨迹及其同步的肌电图信号,计算出同步肌力大小,配准到三维有限元模型,进行仿真步态分析髌韧带等软组织响应特点,研究表明肌肉张力是关节主要稳定因素,韧带张力与肌肉张力呈负相关,对临床髌腱腱纵行切开提供了力学依据。 2.3 有限元法在可穿戴设备及肌内效贴设计中的应用 在研究髌腱炎常规治疗和缓解策略的同时,越来越多的研究将焦点放在膝关节可穿戴设备及肌内效贴的设计上,有限元也是此类研究的常用方法。 2.3.1 可穿戴设备设计方面 最初,利用有限元法进行膝关节护具的研究中,李翼等建立一个膝关节三维模型,模拟了在膝关节佩戴一种动态生物功能腿部护具(依据不同种类的保护带)后的髌骨压力分布,来确定保护带佩戴位置对髌腱附着部压力大小的影响[37]。LAVAGNINO等[38]基于放射学测量研究了髌骨加压带对于减小跳高者膝关节损伤部位髌腱张力的影响,结果显示不同幅度的屈膝运动对髌腱响应特点都有直接影响,佩戴护具可以自动调节膝部材料的弹性模量,在膝角度数极小或高运动量下依然可以提供弹力保护,加固髌骨、防止位移。秦鹍等[39]应用剪切波弹性成像测量髌腱和股四头肌的硬度,并进行重复性测试信度研究,得出结论剪切波弹性成像是一种可靠、可重复的方法。也有研究表明佩戴后托稳定型髌骨带对治疗轻度髌腱炎有效[40-42]。有研究利用有限元模型预测处于不同状态时髌腱局部张力的相应变化,发现髌下带可以通过增加髌腱角来减少髌腱区域的平均局部应变[43-44]。WILLY等[45]认为髌骨应该被看作是一个杠杆,髌腱-股四头肌力矩随着膝关节佩戴双侧强力束带限制屈曲程度的变化而变化,利用有限元分析等一系列数学方程来描述髌骨在矢状面上位置和力的关系,简单理解为髌腱在第一次屈曲时处于相对较高的应力水平,然后将这种关系逆转为相对于髌腱股四头肌有较高的应力水平。 多年来运动专家提倡使用下肢加压带作为一种治疗方法,以减少各种原因引起的膝关节前疼痛,包括髌腱病、髌半脱位、髌股综合征、奥斯古-舒尔特病和髌骨软化症。尽管经常使用这些矫形器,而且佩戴这些矫形器运动员的主观膝关节前疼痛减轻,但对髌骨带发挥作用的潜在机制尚未阐明。然而,还没有研究评估髌骨带对髌腱本身张力的影响。最近的一项尸体研究表明,髌骨带降低了髌下脂肪垫压力和髌股关节面接触应力,平均降低了10%[45]。DUNKMAN等[46]探讨了利用髌骨带改变髌腱角,即通过减少局部髌腱张力变化起到缓解疼痛的作用。有限元模型计算表明,髌骨肌腱病变可能是较小髌骨-髌骨肌腱角高定位肌腱张力的结果,使用特殊托型髌腱加压束带时模型张力会减小[47-49]。跳跃着陆时,在经典位置的髌腱张力与髌腱角呈负相关。 2.3.2 肌内效贴设计方面 根据髌腱炎及髌股关节疼痛综合征不同的伤病情况,设计科学有效的肌内效贴治疗方案,将其作为保守治疗中缓解疼痛的治疗手段[50-51],例如考虑到髌腱在整个下肢动力链中与髋关节和足/踝复合体的联动配合,针对股四头肌过紧[52]、髌骨位置过高[53]、胫骨前肌薄弱等原因造成的髌腱炎进行肌贴干预[54],结合运动康复训练改善髌腱应力分布,以帮助运动员恢复运动水平,重返赛场。目前,关于髌骨加压带的研究设计主要针对髌骨带形状和材料方面,根据人体肌肉发力顺序设计符合动力学的髌骨带,使其作用于髌腱的牵拉应力最小化。采用肌贴干预旨在肌肉起止点处加压来改变髌腱局部应变模式,再通过运动训练激活原动肌,减小对髌腱的牵拉,利用肌贴加压处来调整髌腱的弹性模量,从而提高肌肉等软组织的牵拉耐受能力[55-56]。此外,BENJAMIN等[57-58]通过有限元分析探讨了不同紧度肌内效贴作为支撑条件在肌腱和韧带等软组织结构内部的应力和应变情况,发现随着肌内效贴弹性紧度的增加,肌腱的压力峰值逐渐减小。肌内效贴的使用不仅可以提高纤维软骨对压缩负荷的适应能力,还可以实现膝关节的阻抗控制策略,在跳跃运动时调节股四头肌的力矩,减小对髌腱的牵应力[59-60]。自定义形状贴扎技术满足膝关节发力的具体要求。有研究对髌腱进行有限元分析,探讨3种肌内效贴形状(A型、X型、Y型)及3种弹性紧度(120%,150%,180%)对髌腱压力的影响,结果表明肌贴形状对峰值压强影响较小,对弹性紧度影响较大[61]。 "

| [1] DOS SANTOS WM, CAURIN GAP, SIQUEIRA AAG.Design and control of an active knee orthosis driven by a rotary Series Elastic Actuator. Control Eng Pract.2017;58:307-318. [2] OSTI L, PAPALIA R, BUONO AD, et al.Simultaneous surgi-cal management of chronic grade-2 valgus instability of the knee andan terior cruciate ligament deficiency in athletes.Knee Surg Sports Traumatol Arthrosc.2010;l8(3):312-316. [3] DERKSEN T, KEPPLER J, MILLER S.Chain Reactions: The Biomechanics of Biking.(Cover story).Biomechanics.2004;11(4):22-31. [4] ESKILDSEN SM, BERKOFF DJ, KALLIANOS SA, et al.The use of an IL1-receptor antagonist to reverse the changes associated with established tendinopathy in a rat model.Scand J Med Sci Sports. 2019; 29(1):82-88. [5] JUNG HJ, FISHER MB, WOO SL.Role of biomechanics in the understanding of normal, injured, and healing ligaments and tendons.Sports Med Arthrosc Rehabil Ther Technol.2009;1(1):9. [6] MAGANARIS CN, CHATZISTERGOS P, REEVES ND, et al. Quantification of Internal Stress-Strain Fields in Human Tendon: Unraveling the Mechanisms that Underlie Regional Tendon Adaptations and Mal-Adaptations to Mechanical Loading and the Effectiveness of Therapeutic Eccentric Exercise.Front Physiol. 2017;8:91. [7] AHMADZADEH H, FREEDMAN BR, CONNIZZO BK, et al. Micromechanical poroelastic finite element and shear-lag models of tendon predict large strain dependent Poisson's ratios and fluid expulsion under tensile loading.Acta Biomater.2015;22:83-91. [8] XIONG Y, ZHAO X, XIANG H, et al.Biomechanical Responses and Injury Characteristics of Knee Joints under Longitudinal Impacts of Different Velocities.Appl Bionics Biomech.2018;2018:1407345. [9] MERSMANN F, BOHM S, ARAMPATZIS A.Imbalances in the Development of Muscle and Tendon as Risk Factor for Tendinopathies in Youth Athletes: A Review of Current Evidence and Concepts of Prevention. Front Physiol.2017;8:987. [10] KAEDING C, BEST TM.Tendinosis: pathophysiology and nonoperative treatment.Sports Health. 2009;1(4):284-292. [11] RICHARDS DP, AJEMIAN SV, WILEY JP, et al.Knee joint dynamics predict patellar tendinitis in elite volleyball players.Am J Sports Med. 1996;24(5):676-683. [12] BORK H, THORWESTERN L, GREIF H, et al.Kinematische Untersuchung der Rueckfusspronation bei verschiedenen Laufschuhen/ Kinematic examination rearfoot pronation in different running shoes. Deutsche Zeitschrift fuer Sportmedizin.1998;49(11 Suppl):207-211. [13] SLOTKIN S, THOME A, RICKETTS C, et al.Anterior Knee Pain in Children and Adolescents:Overview and Management.J Knee Surg. 2018;31(5):392-398. [14] BOHM S, MERSMANN F, ARAMPATZIS A.Human tendon adaptation in response to mechanical loading: a systematic review and meta-analysis of exercise intervention studies on healthy adults.Sports Med Open.2015;1(1):7. [15] MERSMANN F, CHARCHARIS G, BOHM S, et al.Muscle and Tendon Adaptation in Adolescence: Elite Volleyball Athletes Compared to Untrained Boys and Girls.Front Physiol.2017;8:417. [16] SCATTONE SILVER R, Purdam CR, Fearon AM, et al.Effects of Altering Trunk Position during Landings on Patellar Tendon Force and Pain. Med Sci Sports Exerc.2017;49(12):2517-2527. [17] SLANE LC, DANDOIS F, BOGAERTS S, et al.Non-uniformity in the healthy patellar tendon is greater in males and similar in different age groups.J Biomech 2018;80:16-22. [18] BODEN RA, RAZAK A, HUSSAIN SM, et al.Loose body following cross-pin fixation for anterior cruciate ligament reconstruction.J Orthop Traumatol.2012;14(2):155-157. [19] EDAMA M, KAGEYAMA I, NAKAMURA M, et al.Anatomical study of the inferior patellar pole and patellar tendon.Scand J Med Sci Sports. 2017;27(12):1681-1687. [20] SCATTONE SILVA R, PURDAM CR, FEARON AM, et al.Effects of Altering Trunk Position during Landings on Patellar Tendon Force and Pain.Med Sci Sports Exerc.2017;49(12):2517-2527. [21] MCCLAY IS, ROBINSON JR, ANDRIACCHI TP, et al.A Kinematic Profile of Skills in Professional Basketball Players.J Appl Biomech. 1994;10(3):205-221. [22] JOHNSTON TE, BASKINS TA, KOPPEL RV, et al.The Influence of extrinsic factors on Knee Biomechanics during cycling: A Systematic review of the Literature.Int J Sports Phys Ther. 2017;12(7):1023-1033. [23] 许定国,刘述芝,陈源吨.有限元分析法在人体下肢关节损伤生物力学中的研究进展[J].重庆医学,2013,42(20):2423-2424,2431. [24] FREEDMAN BR, ZUSKOV A, SARVER JJ, et al.Evaluating changes in tendon crimp with fatigue loading as an ex vivo structural assessment of tendon damage.J Orthop Res.2015;33(6):904-910. [25] 华英汇.股内斜肌/股外侧肌肌力不平衡在髌腱腱病发病机制中的作用[D].上海:复旦大学,2007:23-25. [26] DAN MJ, MCMAHON J, PARR WCH, et al.Evaluation of Intrinsic Biomechanical Risk Factors in Patellar Tendinopathy: A Retrospective Radiographic Case-Control Series.Orthop J Sports Med. 2018;6(12): 2325967118816038. [27] TYLER TF,HERSHMAN EB,NICHOLAS SJ,et al.Evidence of abnormal anteroposterior patellar tilt in patients with patellar tendinitis with use of a new radiographic measurement.Am J Sports Med. 2002;30(3):396-401. [28] 刘波.电针治疗腱末端病的生物力学研究-Ⅱ电针对末端结构粘弹性的影响[J].中国中医骨伤科,1995,3(6):4-8. [29] LEITGEB J, KOETTSDORFER J, SCHUSTER R, et al.Primary anterior cruciate ligament reconstruction in athletes: a 5- year follow up comparing patellar tendon versus hamstring tendon autograft. Wien Klin Wochenschr.2014;126(13-14):397-402. [30] BALDWIN MA, CLARY CW, FITZPATRICK CK, et al.Dynamic finite element knee simulation for evaluation of knee replacement mechanics.J Biomech.2012;45(3):474-483. [31] 仝路,李彦林,胡猛.三维数字化模型在膝关节修复重建中的应用进展[J].中国修复重建外科杂志,2013,27(1):50-53. [32] 吴阳,陈世益,董宇.关节镜下射频治疗顽固性髌腱腱病的回顾性研究[J].中国运动医学杂志,2017,36(3):248-250. [33] 王建平,韩雪莲,季文婷,等.人体膝胫股关节相对运动的三维图像配准分析[J].生物医学工程学杂志,2009,26(6):1340-1344. [34] 许宋锋,于秀淳,徐明,等.内侧腓肠肌瓣前移在重建胫骨上段骨肿瘤保肢术伸膝装置中的应用与临床疗效[J].中国矫形外科杂志, 2011,19(14): 1162-1166. [35] HAYES A,EASTON K,DEVANABOYINA PT,et al.A review of methods to measure tendon dimensions. J Orthop Surg Res.2019;14(1):18. [36] 王大忠,余正红,周民强,等.3D膝关节模型的构建[J].中国组织工程研究与临床康复,2010,14(48):8945-8949. [37] 香港纺织及成衣研发中心有限公司.动态生物功能腿部护具:中国, CN201510307042.4[P].2017.01.04. [38] LAVAGNINO M, ARNOCZKY SP, DODDS J, et al.Infrapatellar Straps Decrease Patellar Tendon Strain at the Site of the Jumper's Knee Lesion: A Computational Analysis Based on Radiographic Measurements.Sports Health.2011;3(3):296-302. [39] 秦鹍,冯亚男,李亚鹏,等.剪切波弹性成像技术量化评估肌腱肌肉弹性模量的信度[J].中国康复理论与实践,2018,24(10):1201-1205. [40] HUBERTI HH, HAYES WC, STONE JL, et al.Force ratios in the quadriceps tendon and ligamentum patellae.J Orthop Res.1984;2(1):49-54. [41] BOROTIKAR BS, SHEEHAN FT.In vivo patellofemoral contact mechanics during active extension using a novel dynamic MRI-based methodology.Osteoarthritis Cartilage.2013;21(12):1886-1894. [42] LAVAGNINO M, ARNOCZKY S, ELVIN N, et al.Patellar tendon strain is increased at the site of the jumper’s knee lesion during knee flexion and tendon loading.Am J Sports Med.2008;36:2110-2118. [43] PIZZOLATO C, LLOYD DG, BARRETT RS, et al.Bioinspired Technologies to Connect Musculoskeletal Mechanobiology to the Person for Training and Rehabilitation.Front Comput Neurosci. 2017;11:96. [44] BOHNSACK M, HALCOUR A, KLAGES P, et al.The influence of patellar bracing on patellar and knee load-distribution and kinematics: an experimental cadaver study.Knee Surg Sports Traumatol Arthrosc. 2008;16:135-141. [45] WILLY RW, MEIRA EP.Current concepts in biomechanic intervation for patellofemoral pain.Int J Sports Phys Ther.2016;11(6):877-890. [46] DUNKMAN AA, BUCKLEY MR, MIENALTOWSKI MJ, et al.Decorin expression is important for age-related changes in tendon structure and mechanical properties.Matrix Biol.2012;32(1):3-13. [47] LAVAGNINO M, WALL ME,LITTLE D, et al.Tendon mechanobiology: Current knowledge and future research opportunities.J Orthop Res. 2015;33(6):813-822. [48] REES JD, MAFFULI N, COOK J.Management of tendinopathy.Am J Sports Med.2009;37:1855-1867. [49] KHAN KM, MAFFULLI N, COLEMAN BD, et al. Patellar tendinopathy: some aspects of basic science and clinical management.Br J Sports Med.1998;32(4):346-355. [50] KHAYYERI H, GUSTAFSSON A, HEUIJERJANS A, et al.A fibre-reinforced poroviscoelastic model accurately describes the biomechanical behaviour of the rat Achilles tendon.PLoS One. 2015; 10(6):e0126869. [51] FANG F, LAKE SP.Modelling approaches for evaluating multiscale tendon mechanics.Interface Focus.2016;6(1):20150044. [52] CHEN K, HU X, BLEMKER SS, et al.Multiscale computational model of Achilles tendon wound healing: Untangling the effects of repair and loading.PLoS Comput Biol.2018;14(12):e1006652. [53] TISCHER T, PAUL J, PAPE D, et al.The Impact of Osseous Malalignment and Realignment Procedures in Knee Ligament Surgery: A Systematic Review of the Clinical Evidence.Orthop J Sports Med. 2017;5(3):2325967117697287. [54] GORDON JA, FREEDMAN BR, ZUSKOV A, et al.Achilles tendons from decorin- and biglycan-null mouse models have inferior mechanical and structural properties predicted by an image-based empirical damage model.J Biomech.2015;48(10):2110-2115. [55] MARIESWARAN M, SIKIDAR A, GOEL A, et al. An extended OpenSim knee model for analysis of strains of connective tissues.Biomed Eng Online.2018;17(1):42. [56] VISNES H, BAHR R.Training volume and body composition as risk factors for developing jumper’s knee among young elite volleyball players.Scand J Med Sci Sports.2013;23(5):607-613. [57] BENJAMIN M, RALPHS JR.Fibrocartilage in tendons and ligaments--an adaptation to compressive load.J Anat.1998;193 (Pt 4):481-494. [58] GRAU S, MAIWALD C, KRAUSS I, et al.What are the causes and treatment strategies for patellar-tendinopathy in female runners?J Biomech.2008;41:2042-2046. [59] CORTES DH, SUYDAM SM, SILBERNAGEL KG, et al.Continuous Shear Wave Elastography: A New Method to Measure Viscoelastic Properties of Tendons in Vivo.Ultrasound Med Biol. 2015;41(6): 1518-1529. [60] DAN M, PARR W, BROE D, et al.Biomechanics of the knee extensor mechanism and its relationship to patella tendinopathy: a review.J Orthop Res.2018;36(12):3105-3112. [61] ENSEKI K, HARRIS-HAYES M, WHITE DM, et al.Nonarthritic hip joint pain.J Orthop Sports Phys Ther.2014;44(6):A1-A32. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [3] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [4] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [5] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [6] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [7] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [8] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [9] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [10] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [11] | Yuan Xinping, Shao Yanbo, Wu Chao, Wang Jianling, Tong Liangcheng, Li Ying. Accuracy of target bone segments in personalized differential modeling and simulation of CT scanning parameters at fracture end [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 912-916. |
| [12] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [13] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [14] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [15] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||