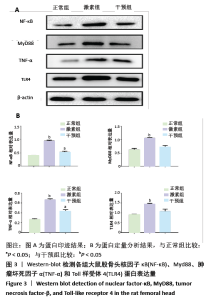
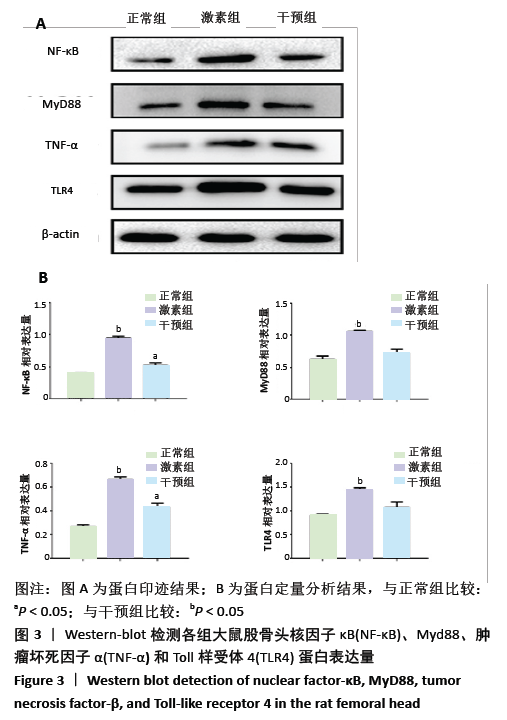
[1] FANG S, LI Y, CHEN P. Osteogenic effect of bone marrow mesenchymal stem cell-derived exosomes on steroid-induced osteonecrosis of the femoral head. Drug design, development and therapy. 2019;13: 45-55.
[2] OKAZAKI S, NAGOYA S, MATSUMOTO H, et al. TLR4 stimulation and corticosteroid interactively induce osteonecrosis of the femoral head in rat. J Orthop Res. 2016;34(2):342-325.
[3] TIAN L, WEN Q, DANG X, et al. Immune response associated with Toll-like receptor 4 signaling pathway leads to steroid-induced femoral head osteonecrosis. BMC Musculoskelet Disord. 2014;15:18.
[4] PEI J, FAN L, NAN K, et al. Excessive Activation of TLR4/NF-κB Interactively Suppresses the Canonical Wnt/β-catenin Pathway and Induces SANFH in SD Rats. Scientific Reports. 2017;7(1):11928.
[5] 范思奇,曾平,周怡,等. ITRAQ技术筛选系统性红斑狼疮合并股骨头坏死的血清差异蛋白质组学变化[J].中国组织工程研究,2019, 23(3):476-481.
[6] 袁捷,张军,林吉,等.通络生骨胶囊治疗股骨头坏死的临床研究[J].中药新药与临床药理,2004,15(6):429-431.
[7] 海阔,李可大.通络生骨胶囊(复方生脉成骨胶囊)治疗股骨头坏死142例临床研究[J].实用中医内科杂志,2014,28(10):28-30.
[8] 袁捷,林吉,徐传毅,等.通络生骨胶囊预防激素性股骨头缺血性坏死的药效学实验[J].中药新药与临床药理,2005,16(3): 185-188.
[9] 章建华, 张成龙, 尹华. 激素类型对大鼠股骨头坏死模型的影响[J].中华中医药杂志,2014,29(12):3969-73.
[10] 蒋玮,曹林忠,邬明峻,等. 激素性股骨头坏死动物模型的建立及评价[J].中国实验动物学报,2019,27(6):799-804.
[11] 汪小敏,曹林忠,张晓刚,等. 激素性股骨头坏死中医“证”的三大组学研究进展[J].中国骨质疏松杂志,2018,24(7):966-970.
[12] 陈卫衡, 何伟, 童培建,等. 股骨头坏死中医辨证标准(2019年版) [J].中医正骨,2019,31(6):1-2.
[13] 孙琳, 张涛, 柴智. 木豆叶提取物对心肌缺血再灌注损伤大鼠的保护作用[J].中草药,2015,46(22):3382-3385.
[14] 李译,林惠湦,陈妮,等.通络生骨胶囊对骨关节炎的治疗作用及其分子机制研究[J].中医药信息,2020,37(1):6-11.
[15] 张金超,王立伟, 孙静,等.木豆叶水提物对兔破骨细胞样细胞的形成及其骨吸收功能的影响[J].河北大学学报(自然科学版),2009, 29(1):45-50.
[16] 郑元元,杨京,陈迪华,等.木豆叶提取物对人的类成骨细胞TE85成骨功能和体外破骨细胞分化的影响[J].药学学报,2007,42(4): 386-391.
[17] 赵飞, 姚忠军, 胡炳炎, 等. 木豆叶提取物对股骨头坏死大鼠血液流变学及骨髓间充质干细胞分化的影响[J].疑难病杂志,2020, 19(7):730-734.
[18] 陈达,陈晓波,白昱旸,等.通络生骨胶囊促进兔激素性股骨头坏死修复的机制研究[J].中药新药与临床药理,2016,27(3):351-356.
[19] 杨俊兴, 方斌, 徐传毅,等. 通络生骨胶囊对激素性股骨头坏死大鼠骨钙素、降钙素与骨密度的影响[J].广州中医药大学学报,2007, 24(1):41-43.
[20] 陈雷雷,陈晓波,洪郭驹,等.活血祛瘀法干预激素性股骨头坏死骨组织的修复[J].中国组织工程研究,2016,20(15):2148-2155.
[21] 高彦淳,冯勇, 张长青. 激素性股骨头坏死发生机制的研究进展[J].国际骨科学杂志,2018,39(4):231-234.
[22] 张华峰, 徐倩. 细胞凋亡在激素性股骨头坏死中作用机制的研究进展[J].中华老年骨科与康复电子杂志,2016,2(2):119-124.
[23] WANG A, REN M, WANG J. The pathogenesis of steroid-induced osteonecrosis of the femoral head: A systematic review of the literature. Gene. 2018;671:103-109.
[24] GAIKWAD S, NAVEEN C, AGRAWAL-RAJPUT R. Toll-like receptor-4 antagonism mediates benefits during neuroinflammation. Neural Regen Res. 2016;11(4):552-553.
[25] ZHENG L, SHEN X, YE J, et al. Metformin alleviates hyperglycemia-induced apoptosis and differentiation suppression in osteoblasts through inhibiting the TLR4 signaling pathway. Life sciences. 2019; 216:29-38.
[26] PANARO MA, CORRADO A, BENAMEUR T, et al. The Emerging Role of Curcumin in the Modulation of TLR-4 Signaling Pathway: Focus on Neuroprotective and Anti-Rheumatic Properties. Int J Mol Sci. 2020; 21(7):2299.
[27] WIDERA D, AGUILAR RM, COTTRELL GS. Toll-like receptor 4 and protease-activated receptor 2 in physiology and pathophysiology of the nervous system: more than just receptor cooperation? Neural Regen Res. 2019;14(7):1196-1201.
[28] SI Y, CHEN YB, CHEN SJ, et al. TLR4 drives the pathogenesis of acquired cholesteatoma by promoting local inflammation and bone destruction. Sci Rep. 2015;5:16683.
[29] LIU YH, HUANG D, LI ZJ,et al. Toll-like receptor-4-dependence of the lipopolysaccharide-mediated inhibition of osteoblast differentiation.Genet Mol Res. 2016;15(2). doi: 10.4238/gmr.15027191.
[30] LITAK J, GROCHOWSKI C, LITAK J, et al. TLR-4 Signaling vs. Immune Checkpoints, miRNAs Molecules, Cancer Stem Cells, and Wingless-Signaling Interplay in Glioblastoma Multiforme-Future Perspectives. Int J Mol Sci. 2020;21(9):3114.
[31] 田雷, 周东生, 孙水, 等. Toll样受体4信号通路过度激活在大鼠激素性股骨头坏死中的作用[J].西安交通大学学报(医学版),2014, 35(5):622-629.
[32] SOUZA PPC, LERNER UH. Finding a Toll on the Route: The Fate of Osteoclast Progenitors After Toll-Like Receptor Activation. Front Immunol. 2019;10:1663.
[33] HUXFORD T, HOFFMANN A, GHOSH G. Understanding the logic of IκB:NF-κB regulation in structural terms. Current topics in microbiology and immunology. 2011;349:1-24.
[34] SAKOWICZ A. The role of NFκB in the three stages of pregnancy - implantation, maintenance, and labour: a review article. BJOG. 2018; 125(11):1379-1387.
[35] KIM K, KIM JH, KIM I, et al. TRIM38 regulates NF-κB activation through TAB2 degradation in osteoclast and osteoblast differentiation. Bone. 2018;113:17-28.
[36] LIN TH, PAJARINEN J, LU L, et al. NF-κB as a Therapeutic Target in Inflammatory-Associated Bone Diseases. Adv Protein Chem Struct Biol. 2017;107:117-154.
[37] JIMI E, TAKAKURA N, HIURA F, et al. The Role of NF-κB in Physiological Bone Development and Inflammatory Bone Diseases: Is NF-κB Inhibition “Killing Two Birds with One Stone”? Cells. 2019;8(12):1636.
[38] BOYCE BF, XIU Y, LI J, et al. NF-κB-Mediated Regulation of Osteoclastogenesis. Endocrinol Metab (Seoul). 2015;30(1):35-44.
[39] NDAYISABA A, JELLINGER K, BERGER T, et al. TNFα inhibitors as targets for protective therapies in MSA: a viewpoint. J Neuroinflammation. 2019;16(1):80.
[40] ZHENG L, WANG W, NI J, et al. Role of autophagy in tumor necrosis factor-α-induced apoptosis of osteoblast cells. J Investig Med. 2017; 65(6):1014-1020.
[41] ZHU S, HE H, GAO C, et al. Ovariectomy-induced bone loss in TNFα and IL6 gene knockout mice is regulated by different mechanisms. J Mol Endocrinol. 2018;60(3):185-198.
[42] BAI F, CHEN X, YANG H, et al. Acetyl-11-Keto-β-Boswellic Acid Promotes Osteoblast Differentiation by Inhibiting Tumor Necrosis Factor-α and Nuclear Factor-κB Activity. J Craniofac Surg. 2018;29(7):1996-2002.
[43] TAKAYANAGI H. The unexpected link between osteoclasts and the immune system. Adv Exp Med Biol. 2010;658:61-68.
[44] RAGGATT LJ, PARTRIDGE NC. Cellular and molecular mechanisms of bone remodeling. J Biol Chem. 2010;285(33):25103-25108.
|