Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (15): 2310-2316.doi: 10.3969/j.issn.2095-4344.2585
Previous Articles Next Articles
Change of related functions and double lower limb length after total knee arthroplasty
Tang Jinlong1, Yang Guanjie1, Liu Lei1, Xu Shizhuang2, Zhao Fengchao1
- 1Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221002, Jiangsu Province, China; 2Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China
-
Received:2019-03-26Revised:2019-04-03Accepted:2019-05-23Online:2020-05-28Published:2020-03-20 -
Contact:Zhao Fengchao, MD, Chief physician, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221002, Jiangsu Province, China -
About author:Tang Jinlong, Master, Physician, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221002, Jiangsu Province, China -
Supported by:the Key Social Development Project of Science and Technology Department of Jiangsu Province, No. BE2016642
CLC Number:
Cite this article
Tang Jinlong, Yang Guanjie, Liu Lei, Xu Shizhuang, Zhao Fengchao. Change of related functions and double lower limb length after total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(15): 2310-2316.
share this article
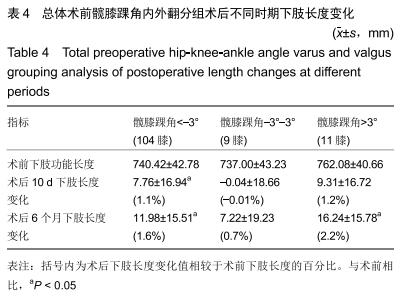
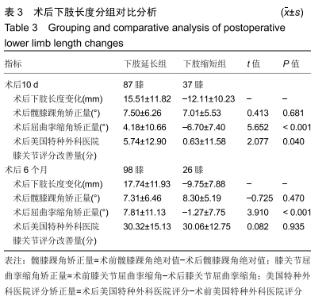
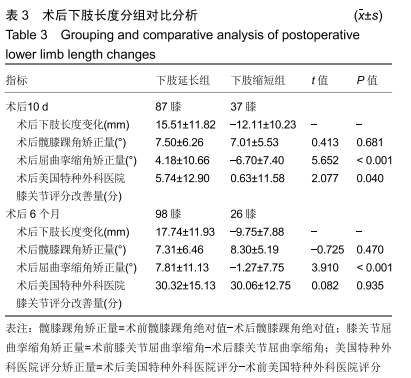
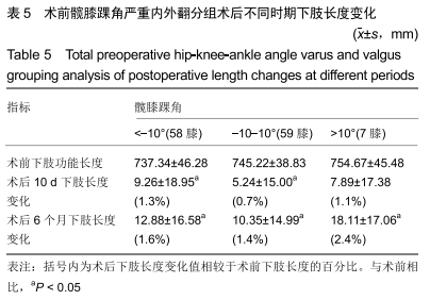
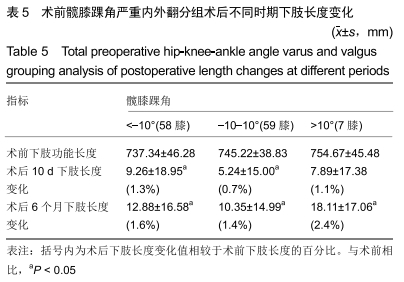
术后6个月:总体下肢长度变化为延长(11.97± 15.85) mm。98膝(79.0%)下肢长度延长,平均增长(17.74± 11.93) mm,其中术后屈曲挛缩角矫正量在2组间差异有显著性意义(P < 0.05),见表3。说明与下肢缩短组相比,术后6个月时下肢延长组术后屈曲挛缩角矫正量较大。 相关性分析:术后10 d屈曲挛缩角矫正量以及美国特种外科医院膝关节评分改善量与术后10 d下肢长度变化间存在相关性(r=0.615,P < 0.001;r=0.232,P=0.010);术后6个月屈曲挛缩角矫正量与术后6个月下肢长度变化间存在相关性(r=0.502,P < 0.001)。 2.4.2 髋膝踝角分组对术后下肢长度及功能的影响 根据髋膝踝角分为3组,内翻组髋膝踝角<-3°,外翻组髋膝踝角>3°,中立位组髋膝踝角-3°-3°。内翻组在术后10 d及6个月时,术后下肢长度与术前比差异均有显著性意义(P < 0.001);外翻组术后10 d时术后下肢长度与术前比差异无显著性意义,术后6个月时术后下肢长度与术前比差异有显著性意义(P=0.007);中立位组术后10 d及6个月术后长度与术前比差异均无显著性意义。术后10 d时,只有内翻组患者术后下肢长度与术前比差异有显著性意义;术后6个月内翻组及外翻组术后下肢长度与术前比差异有显著性意义。术后10 d及6个月时,下肢长度延长量及延长百分比均为:外翻组>内翻组>中立位组,见表4。 "
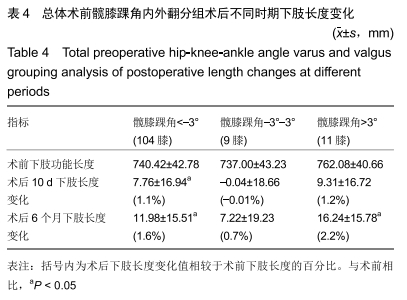
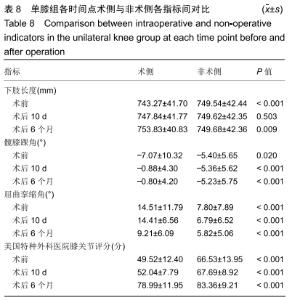
2.4.4 单膝组术前及术后各指标变化 单膝组术侧下肢长度术前短于非术侧(P < 0.001),术后10 d术侧及非术侧长度差异无显著性意义(P=0.503),术后6个月术侧长度长于非术侧(P=0.009)。术侧髋膝踝角在术前大于非术侧(P=0.020),在术后10 d及术后6个月均小于非术侧(P < 0.001)。术侧屈曲挛缩角在术前、术后10 d及术后6个月均大于非术侧(P < 0.001)。术侧美国特种外科医院膝关节评分在各时间点均小于非术侧(P < 0.001)。 总体看,单膝组术侧下肢长度在术后10 d及术后6个月均延长,髋膝踝角角度在术后10 d较前矫正最多,屈曲挛缩角在术后6个月较前矫正最多,美国特种外科医院膝关节评分在术后6个月较前增加最多。非术侧下肢长度及髋膝踝角术后变化很小,屈曲挛缩角轻度矫正,美国特种外科医院膝关节评分在术后6个月较之前增加最多,见表8。 "
| [1] TANG X, WANG S, ZHAN S, et al. The prevalence of symptomatic knee osteoarthritis in china: results from the china health and retirement longitudinal study. Arthritis Rheumatol. 2016;68(3): 648-653. [2] 张晓盈,彭嘉婧,刘传慧,等.骨关节炎患者用药治疗现状的全国多中心大样本现场调查[J]. 北京大学学报(医学版), 2018, 50(6): 1044-1048. [3] 雷光华,王坤正.骨关节炎诊疗指南(2018年版)解读[J].中华骨科杂志, 2018,38(12): 716-717. [4] HOOPER G, ROTHWELL A, FRAMPTON C. The low contact stress mobile-bearing total knee replacement: a prospective study with a minimum follow-up of ten years. J Bone Joint Surg Br. 2009;91(1): 58-63. [5] CHANG MJ, SO S, PARK CD, et al. Long-term follow-up and survivorship of single-radius, posterior-stabilized total knee arthroplasty. J Orthop Sci. 2018;23(1): 92-96. [6] HEESTERBEEK PJC, VAN HOUTEN AH, KLENK JS, et al. Superior long-term survival for fixed bearing compared with mobile bearing in ligament-balanced total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2018;26(5):1524-1531. [7] RITTER MA, KEATING EM, SUEYOSHI T, et al. Twenty-five-years and greater, results after nonmodular cemented total knee arthroplasty. J Arthroplasty. 2016; 31(10):2199-2202. [8] 裴福兴.中国髋、膝关节置换的现状及展望[J].中国骨与关节杂志, 2012, 1(1) 4-8. [9] BHAVE A, MONT M, TENNIS S, et al. Functional problems and treatment solutions after total hip and knee joint arthroplasty. J Bone Joint Surg Am. 2005; 87(1): 9-21. [10] ULRICH SD, BHAVE A, MARKER DR, et al. Focused rehabilitation treatment of poorly functioning total knee arthroplasties. Clin Orthop Relat Res. 2007;464(464): 138-145. [11] AUSTIN MS, HOZACK WJ, SHARKEY PF, et al. Stability and leg length equality in total hip arthroplasty. J Arthroplasty. 2003;18(3): 88-90. [12] GURNEY B, MERMIER CR, GIBSON A, et al. Effects of limb-length discrepancy on gait economy and lower-extremity muscle activity in older adults. J Bone Joint Surg. 2001;83-A(6):907-915. [13] LANG JE, SCOTT RD, LONNER JH, et al. Magnitude of limb lengthening after primary total knee arthroplasty. J Arthroplasty. 2012;27(3): 341-346. [14] KIM SH, RHEE SM, LIM JW, et al. The effect of leg length discrepancy on clinical outcome after TKA and identification of possible risk factors. Knee Surg Sports Traumatol Arthrosc. 2016;24(8): 2678-2685. [15] VAIDYA S, PATEL M, PANGHATE A, et al. Total knee arthroplasty: Limb length discrepancy and functional outcome. Indian J Orthop. 2010;44(3):300-307. [16] TIPTON S, SUTHERLAND J, SCHWARZKOPF R. Change in limb length after total knee arthroplasty. Geriatr Orthop Surg Rehabil. 2015;6(3): 197-201. [17] 陈进良,袁华,冯剑楠,等. 影响DR双下肢全长拼接技术成功率的因素分析及控制策略[J].中国医疗设备, 2018,33(12):87-90. [18] GAO F, MA J, SUN W, et al. Radiographic assessment of knee–ankle alignment after total knee arthroplasty for varus and valgus knee osteoarthritis. Knee. 2017; 24(1): 107-115. [19] BORGBJERG J, MADSEN F, ODGAARD A. Patient self-assessed passive range of motion of the knee cannot replace health professional measurements. J Knee Surg. 2017;30:829-834. [20] INSALL JN, RANAWAT CS, AGLIETTI P, et al. A comparison of four models of total knee-replacement prostheses. J Bone Joint Surg Am. 1976;58(6): 754-765. [21] KIM YH, YOON SH, KIM JS. The long-term results of simultaneous fixed-bearing and mobile-bearing total knee replacements performed in the same patient. J Bone Joint Surg. 2007;89-B(10): 1317-1323. [22] KANE RL, SALEH KJ, WILT TJ, et al. The Functional outcomes of total knee arthroplasty. J Bone Joint Surg Am. 2005; 87(8): 1719-1724. [23] LANG JE, SCOTT RD, LONNER JH, et al. Magnitude of limb lengthening after primary total knee arthroplasty. J Arthroplasty. 2012;27(3): 341-346. [24] AARON A, WEINSTEIN D, THICKMAN D, et al. Comparison of orthoroentgenography and computed tomography in the measurement of limb-length discrepancy. J Bone Joint Surg Am. 1992;74(6): 897-902. [25] TANZER M, MILLER J. The natural history of flexion contracture in total knee arthroplasty. A prospective study. Clin Orthop Relat Res. 1989;248(248): 129-134. [26] CHINNAPPA J, CHEN DB, HARRIS IA, et al. Predictors and functional implications of change in leg length following total knee arthroplasty. J Arthroplasty. 2017;32(9): 2725-2729. [27] MUFTY S, VANDENNEUCKER H, BELLEMANS J. The influence of leg length difference on clinical outcome after revision TKA. Knee. 2014;21(2): 424-427. [28] OHMORI T, KABATA T, KAJINO Y, et al. Three-dimensional limb lengthening after total knee arthroplasty in a simulation study. Mod Rheumatol. 2018;28(6):1029-1034. [29] SHETTY GM, MULLAJI A, KHALIFA AA, et al. The effect of sagittal knee deformity on preoperative measurement of coronal mechanical alignment during total knee arthroplasty. Knee Surg Relat Res. 2017; 29(2):110-114. |
| [1] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [2] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [3] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [4] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [5] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [6] | Peng Chao, Liu Yunpeng, Hua Guojun, Yang Jiaji, Wang Xingliang, Wang Xiaolong. Imaging evaluation of the hip-knee-ankle angle and osteoarthritis progression before and after partial meniscectomy for degenerative medial meniscus posterior root tear [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3368-3373. |
| [7] | Deng Zhibo, Li Zhi, Wu Yahong, Mu Yuan, Mu Yuexi, Yin Liangjun. Local infiltration anesthesia versus femoral nerve block for pain control and safety after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3401-3408. |
| [8] | Mieralimu•Muertizha, Ainiwaerjiang•Damaola, Lin Haishan, Wang Li . Relationship between tibio-femoral mechanical axis deviation on coronal plane and early joint function recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3300-3304. |
| [9] | Huang Chenyu, Tang Cheng, Wei Bo, Li Jiayi, Li Xuxiang, Zhang Huikang, Xu Yan, Yao Qingqiang, Wang Liming. Application of three-dimensional printing guide plate in total knee arthroplasty for patients with varus and valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2789-2793. |
| [10] | Li Shangzhi, Zheng Dezhi, Liu Jun. Early analgesia of cocktail therapy after total knee arthroplasty with enhanced recovery after surgery program [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2794-2798. |
| [11] | Liu Jinlei, Yin Li, Zhang Yi, Wang Haitao, Li Zhuangyan, Xia Peige, Qiao Renqiu. Effects of intravenous tranexamic acid combined with periarticular multipoint injection of tranexamic acid cocktail on blood loss and pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2833-2839. |
| [12] | Xu Hui, Kang Bingxin, Gao Chenxin, Zhao Chi, Xu Xirui, Sun Songtao, Xie Jun, Xiao Lianbo, Shi Qi. Effectiveness of Tuina in the treatment of pain after total knee arthroplasty in patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2840-2845. |
| [13] | Deng Bo, Hong Hainan, Fan Yongyong, Cai Guoping, Feng Xingbing, Hong Zhenghua. Efficacy and safety of tourniquet application in total knee arthroplasty and only at the time of cementing: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2908-2914. |
| [14] | Li Yang, Jiang Shuyun, Li Yiying, Yu Yan, Lu Xiaoying, Wang Danci . Spatiotemporal, kinematic and kinetic characteristics of gait in children with genu valgus [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2303-2308. |
| [15] | Liu Kun, Xu Hao, Wang Yingzhen, Zhang Haining, Fang Yuan, Xiang Shuai, Lü Chengyu. Direct repair of medial collateral ligament injury combined with brace in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2352-2357. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||