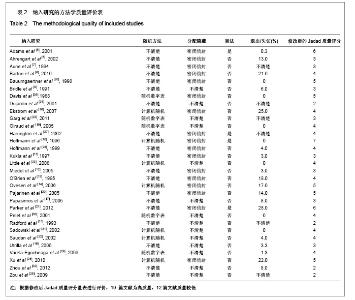
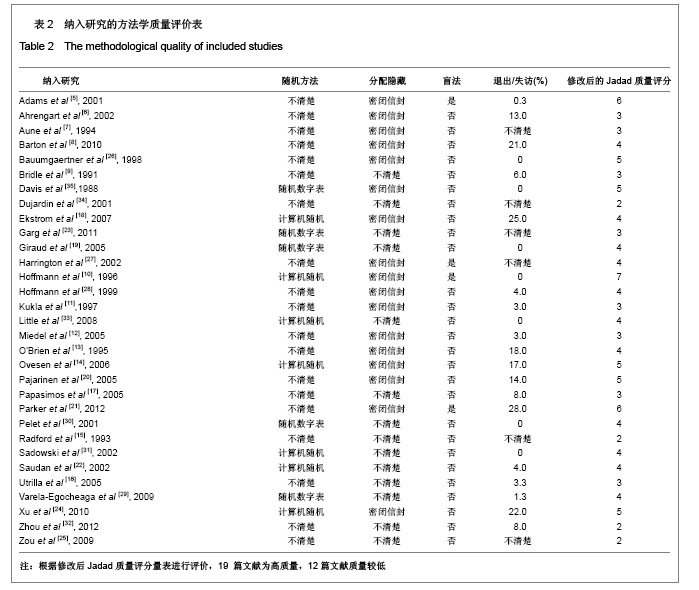
Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (4): 736-743.doi: 10.3969/j.issn.2095-4344.2013.04.026
Previous Articles Next Articles
Intramedullary nails versus extramedullary fixation in the repair of intertrochanteric fractures: A Meta-analysis
Wang Ben1, Ge Zhen-xin1, Yang Guo-yue2, Zhang Dong-zheng1, Zhang Yin-guang3, Tian Wei3, Liu Zhao-jie3, Jia Jian3
- 1 Graduate School of Tianjin Medical University, Tianjin 300200, China
2 Department of Orthopedics, Tianjin Third Central Hospital, Tianjin 300170, China
3 Department of Orthopedics and Traumatology, Tianjin Hospital, Tianjin 300211, China
-
Received:2012-10-13Revised:2012-10-27Online:2013-01-22Published:2013-03-05 -
Contact:Wang Ben★, Studying for master’s degree, Physician, Graduate School of Tianjin Medical University, Tianjin 300200, China 5421120@qq.com -
About author:Wang Ben★, Studying for master’s degree, Physician, Graduate School of Tianjin Medical University, Tianjin 300200, China 5421120@qq.com
CLC Number:
Cite this article
Wang Ben, Ge Zhen-xin, Yang Guo-yue, Zhang Dong-zheng, Zhang Yin-guang, Tian Wei, Liu Zhao-jie, Jia Jian. Intramedullary nails versus extramedullary fixation in the repair of intertrochanteric fractures: A Meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(4): 736-743.
share this article
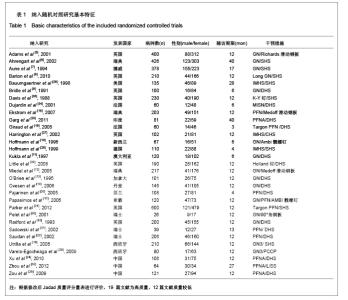
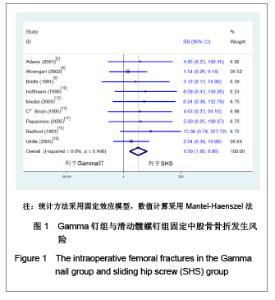
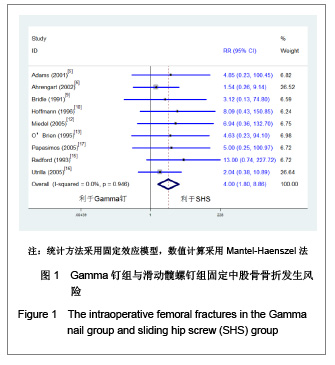
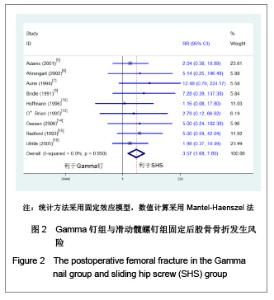
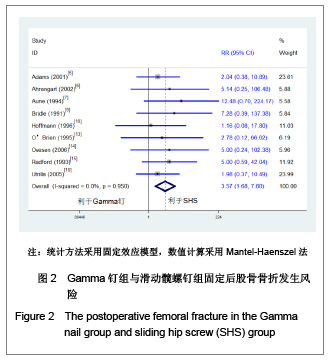
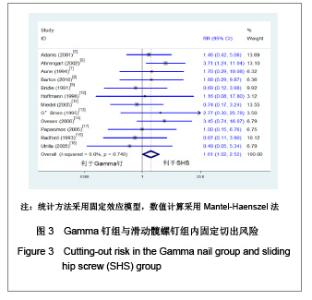
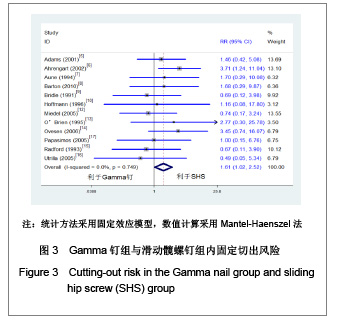
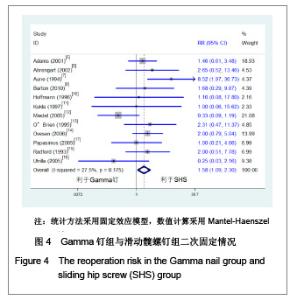
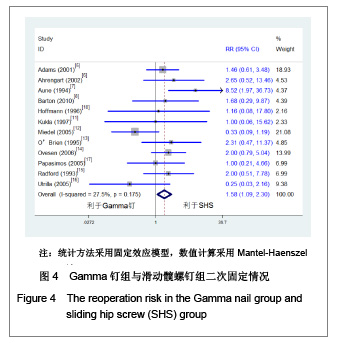
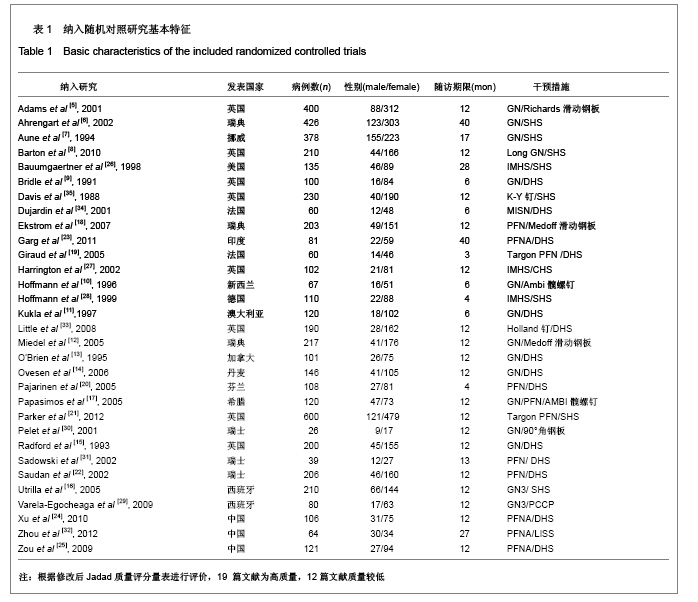
2.1 检索结果分析 初检文献1 856篇,通过阅读标题、摘要后排除明显不符合要求文献1681篇,阅读全文排除文献44篇,最终纳入分析文献31篇[5-35],计5 217例患者,详细资料见表1。 2.2 纳入研究的方法学质量评估 所有纳入文献均为随机对照试验,其中12篇文献通过采用计算机或者随机数字表的方法来随机分配,17篇文献通过密闭信封来确保分配隐藏,仅4篇文献提到盲法,25篇文献对失访进行了描述。根据修改后Jadad质量评分量表进行评价,19 篇文献为高质量,12篇文献质量较低。见表2。 2.3 Meta分析结果 本文纳入的所有研究均为随机对照试验,文献间异质性检验用卡方检验分析各研究结果间的统计学异质性,以I2值判断异质性大小,若I2 < 50%认为各研究间不存在异明显的异质性,采用固定效应模型;I2 > 50%则认为各研究间存在明显的异质性,采用随机效应模型;各结局指标如为二分变量则效应值采用RR,如为连续变量,效应值则采用MD。 Gamma钉与滑动髋螺钉各项结局指标比较:共13项随机对照研究 (n=2 656)对Gamma钉和滑动髋螺钉进行了比较[5-17]。12项研究(n=2 278)显示Gamma钉组术中股骨骨折风险明显高于滑动髋螺钉组(RR=4.00, 95%CI:1.80-8.86,P < 0.01),见图1。13项研究结果显示Gamma钉组术后股骨骨折(RR=3.57,95%CI:1.68-7.60,P < 0.01),内固定切出风险(RR =1.61, 95%CI:1.02-2.52,P =0.04)高于滑动髋螺钉组,见图2,3。12项研究报道了再固定情况,Gamma钉组(n =1 195)共67例患者进行了二次固定,明显多于滑动髋螺钉组(n=1 234)的43例(RR=1.58,95%CI:1.09-2.30,P=0.02),见图4,Gamma钉组随访期内髋部或大腿部残留疼痛(RR=1.31,95%CI:1.09-1.57,P < 0.01)明显高于滑动髋螺钉组。两组在手术时间(MD=2.42,95%CI:-3.71-8.55,P=0.44)、术中失血(MD=83.25,95%CI:-171.21-337.70,P=0.52)、骨折不愈合率(RR=0.49,95%CI:0.22-1.12;P=0.09)、伤口感染(RR=0.92,95%CI:0.48-1.77,P=0.80)、死亡率(RR=1.03,95%CI:0.87-1.22,P=0.71)、平均住院时间(MD=1.50, 95%CI:-0.53-3.53,P=0.15)无明显差异。 股骨近端髓内钉与滑动髋螺钉各项结局指标比较:有6项研究(n=1面礼257)对股骨近端髓内钉与滑动髋螺钉进行了比较[17-22],两组患者在手术时间(MD=-1.45,95%CI:-8.48-5.59,P=0.69)、术中失血量(MD=-172.32, 95%CI:-426.91-82.26,P=0.18)、术中暴露于放射线时间(MD=0.90,95%CI:-0.03-1.83,P=0.06)、固定中及术后股骨骨折、内固定切出(RR=1.27, 95%CI:0.57-2.85,P=0.56)、骨折不愈合(RR=0.50,95%CI:0.09-2.68,P=0.42)、伤口感染(RR=1.43,95%CI:0.78-2.62,P=0.24)、二次固定(RR=1.43,95%CI:0.81-2.53,P=0.22)、死亡率(RR=1.11,95%CI:0.65-1.87,P=0.70)、平均住院时间(MD=0.27, 95%CI:-0.76-1.30,P=0.60)方面无明显差异。 股骨近端抗旋髓内钉与滑动髋螺钉各项结局指标比较: 共3项随机对照研究(n=307)比较了股骨近端抗旋髓内钉与滑动髋螺钉[23-25]。股骨近端抗旋髓内钉组平均失血量为185.9 mL,少于滑动髋螺钉组的438.9 mL[23]。髋关节功能Harris评分股骨近端抗旋髓内钉组(81分)优于滑动髋螺钉组(76分),但固定中放射时间股骨近端抗旋髓内钉组(5.1 min)明显长于滑动髋螺钉组(MD=2.11, 95%CI:1.78-2.43,P < 0.01)。两组患者手术时间(MD=-14.50,95%CI:-66.44-37.44,P=0.58)、固定中及术后股骨骨折[24-25]、内固定切出[23-25]、骨折不愈合[23-25]、二次固定风险[25]、伤口感染[23-24]、死亡率(RR=1.00,95%CI:0.39-2.58,P=1.00)、平均住院时间无明显差异[24]。"

髓内髋螺钉与滑动髋螺钉各项结局指标比较:共3项随机对照研究(n=347)比较了髓内髋螺钉与滑动髋螺钉[26-28]。髓内髋螺钉组平均术中失血245 mL,少于滑动髋螺钉组的340 mL[26]。术中暴露于放射线时间髓内髋螺钉组为3.3 min,明显长于滑动髋螺钉组的2.1 min (MD=1.20,95%CI: 0.88-1.52,P < 0.01)。两组患者在手术时间(MD=6.10,95%CI:-21.34-33.53,P=0.66)、固定中(RR=3.69,95%CI: 0.61-22.16,P=0.15)及术后股骨骨折(RR=5.12,95%CI: 0.61-43.33,P=0.13)、内固定切出(RR=1.01,95%CI: 0.21-4.90,P=0.99)、二次固定风险[28]、骨折不愈合(RR=1.71,95%CI: 0.23-12.72,P=0.60)、伤口感染[28]、死亡率(RR=0.90,95%CI: 0.62-1.30,P=0.58)、髋部或大腿残留疼痛(RR=1.02,95%CI: 0.66-1.58,P=0.92)等方面无明显差异。 7项随机对照研究(n=689)对一些其他常见髓内固定器与髓外固定器各项指标进行比较[29-35]。Gamma钉与PCCP、Gamma钉与90°度角钢板疗效与安全性相似[29-30]。股骨近端髓内钉组手术时间短于动力髁螺钉(DCP)组[31]。股骨近端抗旋髓内钉组平均手术时间为 65.4 min,明显缩短[32]。滑动髋螺钉组手术时间、术中暴露于放射线时间少于Holland钉,但术中失血也更多,且最终髋关节功能评分Holland钉组也更好一些[33]。髓内髋螺钉组患者不仅手术时间、术中失血少于滑动髋螺钉组患者,且固定后开始有效负重时间也更早[34]。K-Y髓内钉与滑动髋螺钉在各主要方面无明显差异[35]。"

| [1] He QX, Xie GZ. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2011;15(13):2371-2375. 何启新,谢广中.人工股骨头置换与动力髋螺钉置入内固定修复老年股骨转子间骨折的Meta分析[J].中国组织工程研究与临床康复,2011,15(13):2371-2375. [2] Canale ST, BeatyJH. Beijing: People's Military Medical Press. 2011. Canale ST, BeatyJH.坎贝尔骨科固定学[M]. 11版.北京:人民军医出版社,2011.[3] Lin PC, Chang SY. Functional recovery among elderly people one year after hip fracture surgery. J Nurs Res. 2004;12(1):72-82. [4] Collaboration TC. Cochrane handbook for systematic reviews of interventions 4.2.2. The Cochrane Collaboration. 2004.[5] Adams CI, Robinson CM, Court-Brown CM, et al. Prospective randomized controlled trial of an intramedullary nail versus dynamic screw and plate for intertrochanteric fractures of the femur. J Orthop Trauma. 2001;15(6):394-400.[6] Ahrengart L, Törnkvist H, Fornander P, et al. A randomized study of the compression hip screw and gamma nail in 426 fractures. Clin Orthop Relat Res. 2002;(401):209-222.[7] Aune AK, Ekeland A, Odegaard B, et al. Gamma nail vs compression screw for trochanteric femoral fractures 15 reoperations in a prospective, randomized study of 378 patients. Acfa Orthop Scand. 1994;65(2):127-130. [8] Barton TM, Gleeson R, Topliss C, et al. A comparison of the long gamma nail with the sliding hip screw for the treatment of AO/OTA 31-A2 fractures of the proximal part of the femur: a prospective randomized trial. J Bone Joint Surg Am. 2010; 92(4):792-798. [9] Bridle SH, Patel AD, Bircher M, et al. Fixation of intertrochanteric fractures of the femur. A randomised prospective comparison of the gamma nail and the dynamic hip screw. J Bone Joint Surg Br. 1991;73(2):330-334. [10] Hoffman CW, Lynskey TG. Intertrochanteric fractures of the femur: a randomized prospective comparison of the gamma nail and the ambl hip screw. Aust N Z J Surg. 1996;66(3):151-155.[11] Kukla C, Heinz T, Berger G, et al. Gamma nail vs. dynamic hip screw in 120 patients over 60 years-A randomized trial. Acta Chir Austriaca. 1997;29(5):290-293. [12] Miedel R, Ponzer S, Törnkvist H, et al. The standard Gamma nail or the Medoff sliding plate for unstable trochanteric and subtrochanteric fractures. J Bone Joint Surg Br. 2005;87-B: 68-75. [13] O'Brien PJ, Meek RN, Blachut PA, et al. Fixation of intertrochanteric hip fractures: gamma nail versus dynamic hip screw. a randomized, prospective study. Can J Surg. 1995;(38):516-520. [14] Ovesen O, Andersen M, Poulsen T, et al. The trochanteric gamma nail versus the dynamic hip screw: a prospective randomised study. One-year follow-up of 146 intertrochanteric fractures. Hip Int. 2006;16(4):293-298.[15] Radford PJ, Needoff M, Webb JK. A prospective randomised comparison of the dynamic hip screw and the gamma locking nail. J Bone Joint Surg Br. 1993;75-B:789-793. [16] Utrilla AL, Sanz Reig J, Miralles MF, et al. Trochanteric gamma nail and compression hip screw for trochanteric fractures a randomized, prospective, comparative study in 210 elderly patients with a new design of the gamma nail. J Orthop Trauma. 2005;19(4):229-233. [17] Papasimos S, Koutsojannis CM, Panagopoulos A, et al. A randomised comparison of AMBI, TGN and PFN for treatment of unstable trochanteric fractures. Arch Orthop Trauma Surg. 2005;125(7):462-468. [18] Ekström W, Karlsson-Thur C, Larsson S, et al. Functional outcome in treatment of unstable trochanteric and subtrochanteric fractures with the proximal femoral nail and the medoff sliding plate. J Orthop Trauma. 2007;21(1):18-25. [19] Giraud B, Dehoux E, Jovenin N, et al. Pertrochanteric fractures: a randomized prospective study comparying dynamic screw plate and intramedullary fixation. Rev Chir Orthop Reparatrice Appar Mot. 2005;91(8):732-736. [20] Pajarinen J, Lindahl J, Michelsson O, et al. Pertrochanteric femoral fractures treated with a dynamic hip screw or a proximal femoral nail. J Bone Joint Surg Br. 2005;87-B:76-81.[21] Parker MJ, Bowers TR, Pryor GA. Sliding hip screw versus the Targon PF nail in the treatment of trochanteric fractures of the hip. J Bone Joint Surg Br. 2012;94-B:391-397. [22] Saudan M, Lübbeke A, Sadowski C, et al. Pertrochanteric fractures: is there an advantage to an intramedullary nail? a randomized, prospective study of 206 patients comparing the dynamic hip screw and proximal femoral nail. J Orthop Trauma. 2002;16(6):386-393.[23] Garg B, Marimuthu K, Kumar V, et al. Outcome of short proximal femoral nail antirotation and dynamic hip screw for fixation of unstable trochanteric fractures. A randomised prospective comparative trial. Hip Int. 2011;21(05):531-536. [24] Xu YZ, Geng DC, Mao HQ, et al. A comparison of the proximal femoral nail antirotation device and dynamic hip screw in the treatment of unstable pertrochanteric fracture. J Int Med Res. 2010;38(4):1266-1275. [25] Zou J, Xu Y, Yang H. A comparison of proximal femoral nail antirotation and dynamic hip screw devices in trochanteric fractures. J Int Med Res. 2009;37(4):1057-1064. [26] Baumgaertner MR, Curtin SL, Lindskog DM. Intramedullary versus extramedullary fixation for the treatment of intertrochanteric hip fractures. Clin Orthop Relat Res. 1998; (348):87-94. [27] Harrington P, Nihal A, Singhania AK. Intramedullary hip screw versus sliding hip screw for unstable intertrochanteric femoral fractures in the elderly. Injury. 2002;33(1):23-28. [28] Hoffmann R, Schmidmaier G, Schulz R, et al. Classic nail versus DHS. A prospective randomised study on operative fixation of trochanteric femur fractures. Unfallchirurg. 1999; 102(3):182-190.[29] Varela-Egocheaga JR, Iglesias-Colao R, Suárez-Suárez MA, et al. Minimally invasive osteosynthesis in stable trochanteric fractures: a comparative study between Gotfried percutaneous compression plate and Gamma 3 intramedullary nail. Arch Orthop Trauma Surg. 2009;129(10): 1401-1407.[30] Pelet S, Arlettaz Y, Chevalley F. Per-and subtrochanteric femoral fractures management with blade plate versus gamma nail fixation: a prospective randomized study. Swiss Surg. 2001;7(3):126-133. [31] Sadowski C, Lübbeke A, Saudan M, et al. Treatment of reverse oblique and transverse intertrochanteric fractures with use of an intramedullary nail or a 95° screw-plate. J Bone Joint Surg Am. 2002;84-A(3):372-381.[32] Zhou F, Zhang ZS, Yang H, et al. Less invasive stabilization system (LISS) versus proximal femoral nail anti-rotation (PFNA) in treating proximal femoral fractures: a prospective randomized study. J Orthop Trauma. 2012;26(3):155-162. [33] Little NJ, Verma V, Fernando C, et al. A prospective trial comparing the Holland nail with the dynamic hip screw in the treatment of intertrochanteric fractures of the hip. J Bone Joint Surg Br. 2008:90(8):1073-1078. [34] Dujardin FH, Benez C, Polle G, et al. Prospective randomized comparison between a dynamic hip screw and a mini-invasive static nail in fractures of the trochanteric area: preliminary results. J Orthop Trauma. 2001;15(6):401-406. [35] Davis TR, Sher JL, Checketts RG, et al. lntertrochanteric fractures of the femur: a prospective study comparing the use of the Kiintscher-Y nail and a sliding hip screw. Injury. 1988; 19(6):421-426. |
| [1] | Wang Qisa, Lu Yuzheng, Han Xiufeng, Zhao Wenling, Shi Haitao, Xu Zhe. Cytocompatibility of 3D printed methyl acrylated hyaluronic acid/decellularized skin hydrogel scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1912-1920. |
| [2] | Wang Songpeng, Liu Yusan, Yu Huanying, Gao Xiaoli, Xu Yingjiang, Zhang Xiaoming, Liu Min. Bidirectional regulation of reactive oxygen species based on zeolitic imidazolate framework-8 nanomaterials: from tumor therapy and antibacterial activity to cytoprotection [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2033-2013. |
| [3] | Liu Yang, Liu Donghui , Xu Lei, Zhan Xu, Sun Haobo, Kang Kai. Role and trend of stimuli-responsive injectable hydrogels in precise myocardial infarction therapy [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2072-2080. |
| [4] | Gao Feng, Zhang Jun, Yu Wenjun, Chanyu Yujing, Zhao Le, Hu Yuting, Wang Junhua, Liu Yongfu. Effects of wrist-hand orthosis on hand dysfunction in stroke patients: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2124-2131. |
| [5] | Lai Yu, Chen Yueping, Zhang Xiaoyun. Research hotspots and frontier trends of bioactive materials in treating bone infections [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2132-2144. |
| [6] | Zheng Yin, Wu Zhenhua, Zhang Cheng, Ruan Kexin, Gang Xiaolin, Ji Hong. Safety and efficacy of immunoadsorption therapy for rheumatoid arthritis: a network meta-analysis and systematic review [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1260-1268. |
| [7] | Chen Qiang, Wu Wenjuan, Jiang Shuhua, Huang Da. Physical exercise improves physical function in burn patients: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1269-1281. |
| [8] | Leng Xiaoxuan, Zhao Yuxin, Liu Xihua. Effects of different neuromodulatory stimulation modalities on non-motor symptoms in Parkinson’s patients: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1282-1293. |
| [9] | Wen Xiaolong, Weng Xiquan, Feng Yao, Cao Wenyan, Liu Yuqian, Wang Haitao. Effects of inflammation on serum hepcidin and iron metabolism related parameters in patients with type 2 diabetes mellitus: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1294-1301. |
| [10] | Wang Mingqi, Feng Shiya, Han Yinhe, Yu Pengxin, Guo Lina, Jia Zixuan, Wang Xiuli. Construction and evaluation of a neuralized intestinal mucosal tissue engineering model in vitro [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 892-900. |
| [11] | Yu Shiyu, Yu Sutong, Xu Yang, Zhen Xiangyan, Han Fengxuan. Advances in research and application of tissue engineering therapeutic strategies in oral submucous fibrosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 936-948. |
| [12] | Jiang Yang, Peng Hao, Song Yanping, Yao Na, Song Yueyu, Yin Xingxiao, Li Yanqi, Chen Qigang. Isometric exercise reduces resting blood pressure: a meta-analysis of moderating factors and dose effects [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 975-986. |
| [13] | Li Hanyue, Li Yini, Xiang Linmei, Li Sen. Effects of resistance exercise therapy on pain and function in patients with cervical spondylotic radiculopathy: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 987-996. |
| [14] | Sun Jiahe, Shi Jipeng, Zhu Tianrui, Quan Helong, Xu Hongqi. Effect of exercise intervention in elderly individuals with sarcopenia and its comorbidities: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 997-1007. |
| [15] | Yang Yuanyuan, Zhou Shanshan, Cheng Xiaofei, Feng Luye, Tang Jiqin. Network meta-analysis of non-invasive brain stimulation in the treatment of lower limb motor dysfunction after stroke [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 1008-1018. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||