Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (6): 917-923.doi: 10.3969/j.issn.2095-4344.2453
Previous Articles Next Articles
Internal fixation strategies for different lateral wall types of intertrochanteric fractures of the femur
Guo Tianqing, Xue Fei, Feng Wei
- Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010000, Inner Mongolia Autonomous Region, China
-
Received:2019-05-14Revised:2019-05-25Accepted:2019-07-06Online:2020-02-28Published:2020-01-18 -
Contact:Feng Wei, Chief physician, Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010000, Inner Mongolia Autonomous Region, China -
About author:Guo Tianqing, Master candidate, Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010000, Inner Mongolia Autonomous Region, China -
Supported by:the Scientific Research Project of Institutions of Higher Learning in Inner Mongolia Autonomous Region, No. NJZZ14143
CLC Number:
Cite this article
Guo Tianqing, Xue Fei, Feng Wei. Internal fixation strategies for different lateral wall types of intertrochanteric fractures of the femur[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(6): 917-923.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
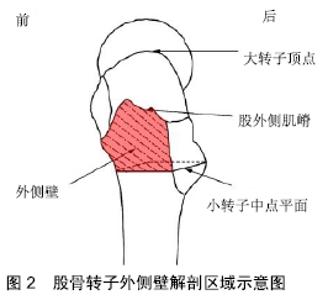
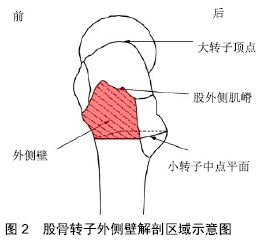
2.1 外侧壁概念提出及完善 手术能够达到骨折的满意复位,并且提供牢固的固定,能使患者摆脱卧床,早期下地进行日常生活。长久以来,人们认为想要达到股骨转子间骨折内固定的稳定,关键因素在于复位后内侧的骨折块,认为包含了股骨距、小转子的后内侧骨折块是决定复位稳定性并能提供牢固固定的关键所在,很久以前EVANS[3]就提出了这一观点。1980年,JENSEN[4]提出了前内侧骨皮质能够维持骨折复位的稳定,从而使骨折端继发移位降低。进入20世纪90年代,1995年BAUMGAERTNER等[5]提出了顶尖距的概念,报道了头颈钉在股骨头内的距离对骨折稳定的重要性。1996年,PAKER[6]研究并发现了股骨大转子外侧骨皮质的完整有利于提高股骨转子间骨折内固定的稳定性,因其连接股骨干并能对股骨干的内移起到阻止作用。新的概念不断提出,也丰富了人们对影响股骨转子间骨折内固定稳定性因素的认识。直到2004年,GOTFRIED[7]首次提出了股骨转子外侧壁对于骨折内固定稳定性的重要性,并认为外侧壁的影响要远大于顶尖距对于术后疗效的影响,但是Gotfried并没有具体的给出外侧壁的概念和范围。2005年IM等[8]通过回归分析发现,股骨转子间骨折复位丢失的显著与否与股骨外侧壁是否完整息息相关。紧接着2007年PALM等[9]提出,在二次手术翻修中是否发现继发外侧壁骨折是最重要的预测因素。IM等[8]和PALM等[9]相继通过实验证实了股骨转子外侧壁的作用所在,并且提出了外侧壁在解剖学上的范围:上至股外侧肌嵴,与大转子相接,下至小转子中点平面的股骨近端外侧皮质,见图2[10]。2013年,ABRAM等[11]对大转子入针点、顶尖距和外侧壁3点固定稳妥的病例进行生物力学研究,提出了相对于入针点和顶尖距,外侧壁的完整性作为术后疗效的预测指标更有意义也更重要。同年,HSU等[12]通过回顾性研究预测骨折内固定稳定的可靠因素,在考虑患者的年龄、骨折类型、性别、外侧壁厚度、顶尖距等诸多因素中,外侧壁厚度成为最关键的因素。股骨外侧壁这一概念在提出后,经过IM等[8]、PALM等[9]、ABRAM等[11]、HSU等[12]的不断完善,改变了长久以来人们对于前内侧骨皮质、后内侧骨块在骨折内固定稳定性起决定性作用的大局,对外侧壁影响股骨转子间骨折内固定稳定性因素进行了补充,使认识更全面、更利于手术治疗。2018年,通过CT三维重建技术,GAO等[13]重新定义了外侧壁的范围:上至股骨外侧嵴,下至股骨外侧皮质与股骨颈下缘骨皮质切线的焦点。 "

2.2 股骨转子间骨折的手术治疗方式 手术治疗股骨转子间骨折时,主要采用动力髋螺钉、经皮加压接骨板、股骨近端解剖锁定钢板、股骨近端锁定加压钢板、倒置微创内固定系统钢板等髓外固定系统,以及Gamma钉、股骨近端髓内钉、股骨近端防旋髓内钉、亚洲型股骨近端防旋髓内钉、股骨近端联合加压交锁髓内钉系统、股骨近端可膨胀髓内钉等髓内固定系统。理想的内置物要求:能够提供更坚强的内固定,以利于患者早期的负重功能锻炼;更容易的植入技术,使年轻医生的学习曲线减短,使手术操作更顺畅;更低的股骨头切割率、内置物的术后松动及其他器械相关并发症的发生率;更有力的加压技术,能够促进骨折更快的愈合;更微创的操作,减少手术操作期间并发症的发生率;更低廉的费用,减轻患者及家属的负担。 2.3 外侧壁的重要意义 患者进入手术室麻醉后以仰卧位平躺于牵引床上,双下肢置于足部支架被牢牢固定,临床医生通过外展位沿着患侧下肢的长轴方向牵引试行手法复位,在透视照射下观察正位片应见内侧皮质骨接触良好,侧位片亦应见后侧皮质骨接触良好。若内侧后侧等有重叠或者裂纹,可适当的内外旋患肢并调整牵引,以达到标准复位的目的。无论是在髓内固定还是在髓外固定中,头颈钉入针点都是在股骨外侧肌嵴的下方2 cm左右区域的外侧骨皮质,打入股骨头的位置。所以外侧壁的完整性对于内置物在该区域进针至关重要。GAO等[13]回顾性分析了2004年5月至2015年4月间99例接受股骨近端骨折(股骨外侧壁骨折)手术治疗成年患者的医疗记录,以确定植入失败的相关因素。得出结论为大转子与股骨外侧壁交界处的游离骨碎片和穿过股骨外侧壁的横向骨折线,是股骨近端骨折合并股骨外侧壁骨折时植入失败的预测因子,股骨外侧壁的完整性与股骨近端骨折的预后相关,对于股骨近端骨折伴股骨外侧壁骨折的有效治疗可能需要股骨外侧壁重建。CIUFO等[14]研究发现,完整的外侧壁可有效地支撑头颈处的碎骨块,为近端骨碎片提供强有力的外侧支撑作用,使骨块之间相互接触并相互嵌入,不仅可促进骨折的愈合,而且进一步加强了稳定。如果外侧壁的完整性遭到了破坏,无法从外侧对近端骨碎片进行支撑就会造成骨质的塌陷。完整的外侧壁同样是股骨干近端的延续,能很好的对抗股骨干的内移,若外侧壁破裂,就相当于在生物力学上形成了转子下骨折,远端的骨块相比于近端的骨块更容易向内侧移动,当移位量大于1/3时就会导致髋部力学的改变,骨折复位产生丢失,髋关节变得外展无力,力矩变得短缩,从而引发肢体短缩,患者术后基本步态发生改变,骨盆平衡能力丧失,甚至丧失行走能力。外侧壁的完整防止了头颈骨块之间的旋转与内翻,为内固定的植入提供了支持,并且在生物力学上分散了应力,减少了螺钉所承受的应力,有效防止头颈螺钉的后退切出,并且在一定程度上减轻了主钉与头颈钉连接接口处的杠杆产生的应力,不仅防止了主钉的弯曲断裂,而且对头颈钉的过度滑移起到防止作用,为头颈钉提供了3点受力外侧作用力,从而降低使内固定的失败率[14]。术前要充分对外侧壁的完整性进行评估分析,根据不同外侧壁的状态来决定不同的骨折分型[15],在术前明确并选择合适的内固定方式,术中可根据具体情况及时更改术前设计的方案,避免造成医源性的二次骨折。 2.4 外侧壁分型 依据外侧壁的结构是否完整,GOTFRIED[7]、PALM[9]、SUN等[16]提出了关于外侧壁的3种分型:①外侧壁稳定型骨折:顺向的稳定骨折,包含了A1的3个亚型和A2.1亚型,其中A1的3个亚型是简单的2部分骨折,单条的骨折线延伸至内侧的骨皮质,其复位较简单,复位后能够承担大部分的负荷,A2.1亚型为小转子无移位大转子完整的骨折;②外侧壁危险型:顺向的不稳定骨折,包含了A2.2和A2.3亚型,是累及了小转子和部分大转子的骨折;③外侧壁破裂型:同样也是不稳定骨折,为原发性外侧壁破裂,包含了A3的3个亚型,后内侧与外侧的支撑结构遭到破坏(累及外侧壁),骨折线从股外侧肌嵴以远穿出。该分型是在AO分型的基础上整理得出,体现了骨折的稳定与否。 "

| [1] CELIK T, MUTLU I, OZKAN A, et al.Comparison of the Lag Screw Placements for the Treatment of Stable and Unstable Intertrochanteric Femoral Fractures regarding Trabecular Bone Failure.J Med Eng. 2016;2016:5470798. [2] ALEXIOU KI, ROUSHIAS A, VARITIMIDIS SE, et al. Quality of life and psychological consequences in elderly patients after a hip fracture: a review. Clin Interv Aging.2018;13:143-150. [3] EVANS EM.The treatment of trochanteric fractures of the femur.J Bone Joint Surg Br.1949;31B(2):190-203. [4] JENSEN JS.Classification of trochanteric fractures.Acta Orthop Scand. 1980;51:803-810. [5] BAUMGAERTNER MR, CURTIN SL, LINDSKOG DM, et al.The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip.J Bone Joint Surg Am.1995;77: 1058-1064. [6] PARKER MJ.Trochanteric hip fractures. Fixation failure commoner with femoral medialization, a comparison of 101 cases.Acta Orthop Scand.1996;67:329-332. [7] GOTFRIED Y.The lateral trochanteric wall: a key element in the reconstruction of unstable pertrochanteric hip fractures.Clin Orthop Relat Res.2004;(425):82-86. [8] IM GI, SHIN YW, SONG YJ.Potentially unstable intertrochanteric fractures.J Orthop Trauma.2005;19:5-9. [9] PALM H, JACOBSEN S, SONNE-HOLM S, et al.Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation.J Bone Joint Surg Am. 2007;89: 470-475. [10] 马卓,张世民.股骨粗隆外侧壁研究进展[J].国际骨科学杂志, 2012,33(4): 221-224. [11] ABRAM SG, POLLARD TC, ANDRADE AJ.Inadequate 'three-point' proximal fixation predicts failure of the Gamma nail.Bone Joint J. 2013; 95-B(6):825-830. [12] HSU CE, SHIH CM, WANG CC, et al.Lateral femoral wall thickness. A reliable predictor of post-operative lateral wall fracture in intertrochanteric fractures.Bone Joint J.2013;95-B(8):1134-1138. [13] GAO Z, LV Y, ZHOU F, et al.Risk factors for implant failure after fixation of proximal femoral fractures with fracture of the lateral femoral wall. Injury.2018;49:315-322. [14] CIUFO DJ, ZARUTA DA, LIPOF JS, et al.Risk Factors Associated With Cephalomedullary Nail Cutout in the Treatment of Trochanteric Hip Fractures.J Orthop Trauma.2017;31(11):583-588. [15] FUTAMURA K, BABA T, HOMMA Y, et al. New classification focusing on the relationship between the attachment of the iliofemoral ligament and the course of the fracture line for intertrochanteric fractures.Injury. 2016;47(8):1685-1691. [16] SUN LL, LI Q, CHANG SM.The thickness of proximal lateral femoral wall.Injury.2016;47: 784-785. [17] YANG X, WU Q, WANG X.Investigation of perioperative hidden blood loss of unstable intertrochanteric fracture in the elderly treated with different intramedullary fixations.Injury.2017;48:1848-1852. [18] KRIGBAUM H, TAKEMOTO S, KIM HT, et al.Costs and Complications of Short Versus Long Cephalomedullary Nailing of OTA 31-A2 Proximal Femur Fractures in U.S. Veterans.J Orthop Trauma.2016;30(3):125-129. [19] LI B, LI J, WANG S, et al.Clinical analysis of peri-operative hidden blood loss of elderly patients with intertrochanteric fractures treated by unreamed proximal femoral nail anti-rotation.Sci Rep.2018;8:3225. [20] SUN FG, WANG DX, HU YT, et al.Clinical observation of proximal femoral anti-rotation nail for the treatment of femoral intertrochanteric fracture.Zhongguo Gu Shang.2017;30:915-919. [21] FOSS NB, KEHLET H. Hidden blood loss after surgery for hip fracture. J Bone Joint Surg Br.2006; 88:1053-1059. [22] JACOB J, DESAI A, TROMPETER A.Decision Making in the Management of Extracapsular Fractures of the Proximal Femur - is the Dynamic Hip Screw the Prevailing Gold Standard?Open Orthop J. 2017;11:1213-1217. [23] SHARMA A, SETHI A, SHARMA S.Treatment of stable intertrochanteric fractures of the femur with proximal femoral nail versus dynamic hip screw: a comparative study.Rev Bras Ortop.2018;53: 477-481. [24] SETIOBUDI T, NG YH, LIM CT, et al.Clinical outcome following treatment of stable and unstable intertrochanteric fractures with dynamic hip screw.Ann Acad Med Singap.2011;40:482-487. [25] YEGANEH A, TAGHAVI R, MOGHTADAEI M.Comparing the Intramedullary Nailing Method Versus Dynamic Hip Screw in Treatment of Unstable Intertrochanteric Fractures.Med Arch.2016; 70:53-56. [26] JOSHI D, DHAMANGAONKAR AC, RAMAWAT S, et al.Predictors of iatrogenic lateral wall fractures while treating intertrochanteric fracture femur with the dynamic hip screw system in Indian patients.Eur J Orthop Surg Traumatol.2015;25:677-682. [27] YU W, ZHANG X, ZHU X, et al.Proximal femoral nails anti-rotation versus dynamic hip screws for treatment of stable intertrochanteric femur fractures: an outcome analyses with a minimum 4 years of follow-up.BMC Musculoskelet Disord.2016;17:222. [28] PRADEEP AR, KIRANKUMAR A, DHEENADHAYALAN J, et al. Intraoperative lateral wall fractures during Dynamic Hip Screw fixation for intertrochanteric fractures-Incidence, causative factors and clinical outcome.Injury. 2018;49:334-338. [29] SHARMA G, SINGH R, GN KIRAN K, et al.Which AO/OTA 31-A2 pertrochanteric fractures can be treated with a dynamic hip screw without developing a lateral wall fracture? A CT-based study.Int Orthop. 2016;40:1009-1017. [30] 张世民,祝晓忠,黄轶刚,等.外侧壁危险型股骨粗隆间骨折DHS与PFNA治疗的回顾性对比研究[J].中国矫形外科杂志, 2010,18(22):1868-1872. [31] HSU CE, CHIU YC, TSAI SH, et al.Trochanter stabilising plate improves treatment outcomes in AO/OTA 31-A2 intertrochanteric fractures with critical thin femoral lateral walls.Injury.2015; 46: 1047-1053. [32] ARIRACHAKARAN A, AMPHANSAP T, THANINDRATARN P, et al. Comparative outcome of PFNA, Gamma nails, PCCP, Medoff plate, LISS and dynamic hip screws for fixation in elderly trochanteric fractures: a systematic review and network meta-analysis of randomized controlled trials.Eur J Orthop Surg Traumatol.2017; 27:937-952. [33] LANGFORD J, PILLAI G, UGLIAILORO AD, et al.Perioperative lateral trochanteric wall fractures: sliding hip screw versus percutaneous compression plate for intertrochanteric hip fractures.J Orthop Trauma. 2011;25:191-195. [34] HU Y, HAN L, FANG W, et al.Comparison of anatomical locking plate and Gamma nail for the treatment of intertrochanteric fracture with external wall fractures.Zhongguo Gu Shang.2016;29: 496-501. [35] SHAH MD, KAPOOR CS, SONI RJ, et al. Evaluation of outcome of proximal femur locking compression plate (PFLCP) in unstable proximal femur fractures.J Clin Orthop Trauma.2017;8(4): 308-312. [36] 唐天华,谭文成,唐三元,等.经皮加压钢板与动力髋螺钉治疗股骨转子间骨折的Meta分析[J].中国矫形外科杂志, 2015,23(16):1454-1460. [37] COLLINGE CA, HYMES R, ARCHDEACON M, et al.Unstable Proximal Femur Fractures Treated With Proximal Femoral Locking Plates: A Retrospective, Multicenter Study of 111 Cases.J Orthop Trauma. 2016;30:489-495. [38] GADEGONE WM, SHIVASHANKAR BH, LOKHANDE V, et al. Augmentation of proximal femoral nail in unstable trochanteric fractures..SICOT J.2017;3:12. [39] SHODA E, KITADA S, SASAKI Y, et al.Proposal of new classification of femoral trochanteric fracture by three-dimensional computed tomography and relationship to usual plain X-ray classification.J Orthop Surg(Hong Kong).2017;25:2309499017692700. [40] CHO JW, KENT WT, YOON YC, et al.Fracture morphology of AO/OTA 31-A trochanteric fractures: A 3D CT study with an emphasis on coronal fragments.Injury.2017;48:277-284. [41] HORWITZ DS, TAWARI A, SUK M.Nail Length in the Management of Intertrochanteric Fracture of the Femur.J Am Acad Orthop Surg.2016; 24:e50-58. [42] HWANG JH, OH JK, HAN SH, et al.Mismatch between PFNa and medullary canal causing difficulty in nailing of the pertrochanteric fractures.Arch Orthop Trauma Surg.2008;128:1443-1446. [43] DÍAZ VJ, CAÑIZARES AC, MARTÍN IA, et al.Predictive variables of open reduction in intertrochanteric fracture nailing: a report of 210 cases.Injury.2016;47 Suppl 3:S51-S55. [44] KULKARNI SGO, BABHULKAR SS, KULKARNI SM, et al. Augmentation of intramedullary nailing in unstable intertrochanteric fractures using cerclage wire and lag screws: a comparative study. Injury.2017;48 Suppl 2:S18-S22. [45] BABHULKAR S.Unstable trochanteric fractures: Issues and avoiding pitfalls.Injury.2017;48: 803-818. [46] XU JW, HAN L, HU YG, et al.[A medium term therapeutic effects of anatomic locking plate for femoral intertrochanteric with lateral femoral wall fractures].Zhongguo Gu Shang.2017;30: 256-260. [47] WU YIS, XU B, YU ZQ, et al.Biomechanical study of the lateral wall of the femur in the treatment of femoral intertrochanteric fracture with intramedullary or extramedullary fixation.Zhongguo Gu Shang. 2017; 30: 247-251. |
| [1] | Xu Xiaopei, Lü Xin. Classification of intertrochanteric fractures with medial wall destruction in elderly patients and recovery of bony support and continuity of the cortical bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2259-2265. |
| [2] | Liang Jie, Xiang Feifan, Yang Kun, Sun Yuanlin, Zhou Wei, Xiang Yong, Yang Yunkang. Intramedullary fixation versus plate fixation in the treatment of displaced mid-shift clavicle fractures: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(6): 947-955. |
| [3] | Tao Jin, Xiong Guirun, Liu Pengran, Jiao Rui, Li Xiaolei, Yan Lianqi. Clinical significance of external wall of femoral intertrochanteric fracture and the treatment of internal fixation [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(30): 4854-4859. |
| [4] |
Zhang Qingzhu, Fan Qi, Yin Xuelian, Wang Pengcheng, Hou Jing, Feng Zhen, Shi Litao, Zhang Zhongyan, Li Aihua, Wan Qian .
Comparison of three implants for treating intertrochanteric fractures of cerebral infarction hemiplegia side in older adults
[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(24): 3805-3811.
|
| [5] | Chen Jun-ming, Li Wen-cheng, Cai Yu, Ding Er-qin. Appropriate metal implants for internal fixation of proximal femoral fractures [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(9): 1679-1686. |
| [6] | Wang Ben, Ge Zhen-xin, Yang Guo-yue, Zhang Dong-zheng, Zhang Yin-guang, Tian Wei, Liu Zhao-jie, Jia Jian. Intramedullary nails versus extramedullary fixation in the repair of intertrochanteric fractures: A Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(4): 736-743. |
| [7] | Li Yan, Wang Dong, Sun Hai-yu, Liu Liang, Li Shu-wei. Comprehensive evaluation of intramedullary fixation and extramedullary fixation in the treatment of unstable femoral intertrochanteric fractures [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(35): 6254-6260. |
| [8] | Long Qiu-ping, Liao Qian-de, Yin Ke, Zhong Da, Niu Bing, Ding Deng-feng. Comparison of hidden blood loss in two kinds of internal fixation for femoral intertrochanteric fractures [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(30): 5460-5465. |
| [9] | Guo Xiao-liang1, Wei Xiao-chun2, Wang Xiao-hu2. Intramedullary fixation for the treatment of femoral intertrochanteric fracture: Pros and cons evaluation [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(26): 4904-4911. |
| [10] | Gao Yan-ming, Zhang Lu. Anti-rotation intramedullary nail and dynamic hip screw internal fixation for treatment of femoral intertrochanteric fractures [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(13): 2455-2462. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||