Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (3): 428-437.doi: 10.3969/j.issn.2095-4344.2417
Previous Articles Next Articles
Outcomes and metal ion levels of Birmingham hip resurfacing versus total hip arthroplasty: a systematic review and meta-analysis
Fan Zhirong1, Huang Yongquan2, Peng Jiajie1, Hong Weiwu1, Zhong Degui1, Su Haitao2, Liu Zitao2, Jiang Tao2
- 1Second Clinical Medical College, Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China; 2Department of Orthopedics, Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China
-
Received:2019-03-21Revised:2019-04-09Accepted:2019-04-23Online:2020-01-28Published:2019-12-26 -
Contact:Jiang Tao, Master, Associate chief physician, Department of Orthopedics, Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China -
About author:Fan Zhirong, Master candidate, Second Clinical Medical College, Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China -
Supported by:the Scientific Research Project of Guangdong Traditional Chinese Medicine Bureau in 2018, No. 20182043; the Basic and Applied Research in Guangdong Province (Provincial Natural Science Foundation), No. 2018A030313694
CLC Number:
Cite this article
Fan Zhirong, Huang Yongquan, Peng Jiajie, Hong Weiwu, Zhong Degui, Su Haitao, Liu Zitao, Jiang Tao. Outcomes and metal ion levels of Birmingham hip resurfacing versus total hip arthroplasty: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 428-437.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
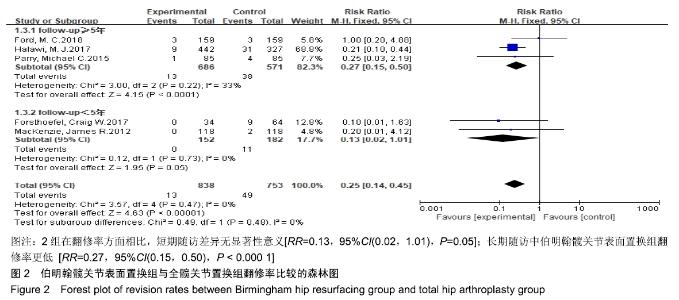
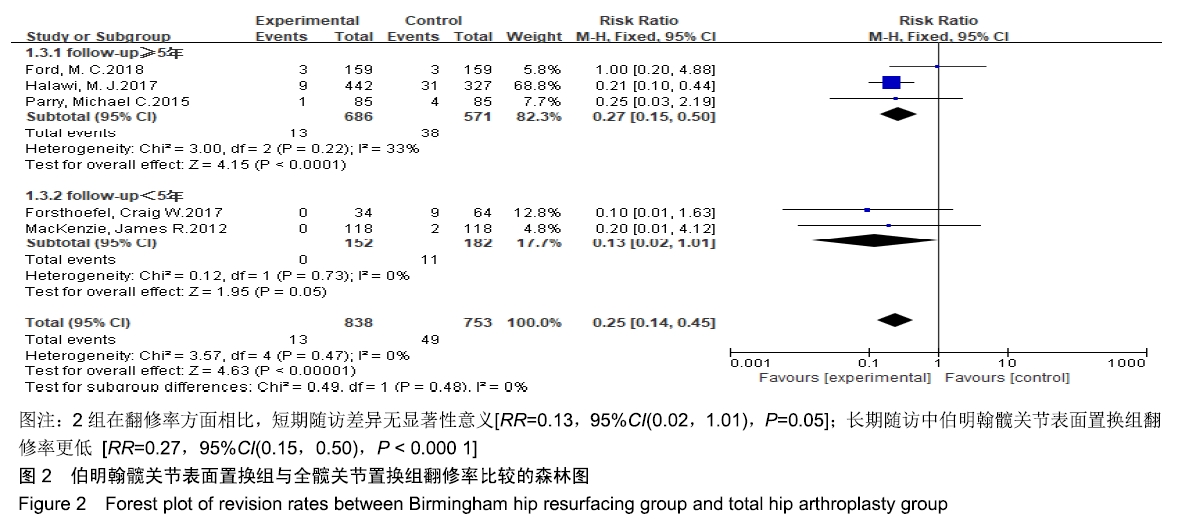
2.3 Meta分析结果 2.3.1 翻修率 共有5篇文献报道了翻修数量[18,20-22,24],其中3篇文献随访时间超过5年[20-21,24],2篇文献则不足5年[18,22],故按照随访时间长短分为2个亚组,分别为短期随访组(随访时间不足5年)和长期随访组(随访时间超过5年)。亚组异质性检验结果显示,短期随访组(I2=0%,P=0.73)与长期随访组(I2=33%,P=0.22)组间具有同质性,故采用固定效应模型合并效应量。Meta分析结果显示,无论是短期随访还是长期随访,伯明翰髋关节表面置换组和全髋关节置换组比较均具有更少的翻修率,但是短期随访组组间差异无显著性意义(RR=0.13,95%CI(0.02,1.01),P=0.05),长期随访组组间差异有显著性意义(RR=0.27,95%CI(0.15,0.50),P < 0.000 1),见图2。"
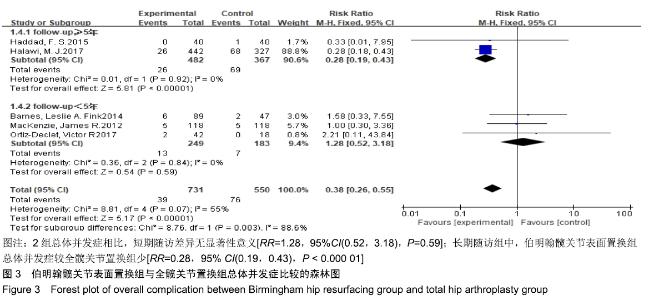
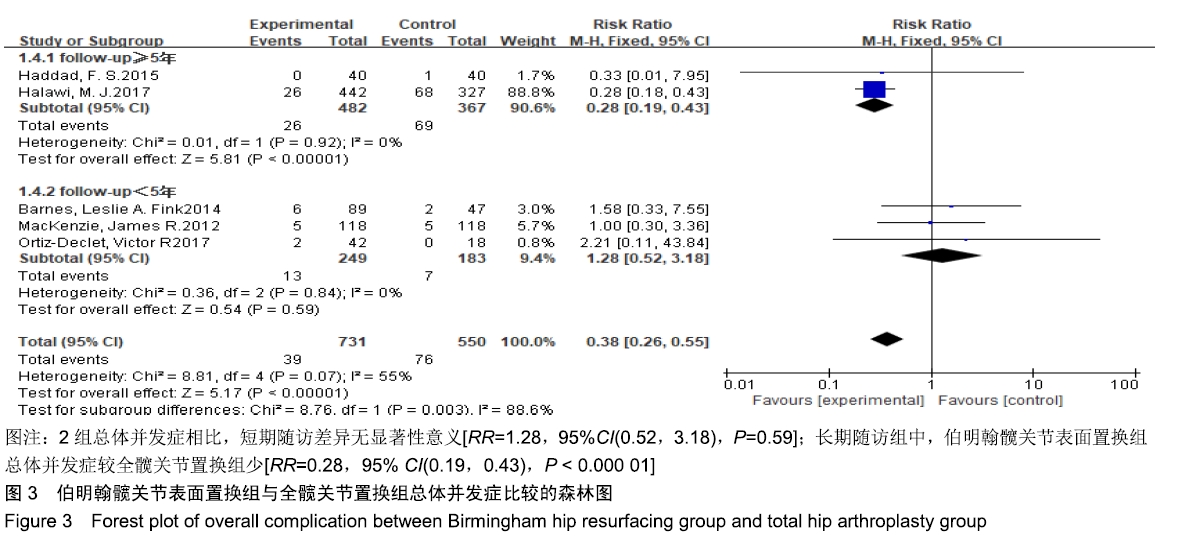
2.3.2 总体并发症 共有5篇文献报道了总体并发 症[3,16-18,21],其中2篇文献随访时间超过5年[16,20-21,24],3篇文献随访时间不足5年[3,17-18,22],故按照随访时间长短分为短期随访组和长期随访组2个亚组。亚组异质性检验结果显示,短期随访组(I2=0%,P=0.84)与长期随访组(I2=0%,P=0.92)组间具有同质性,故采用固定效应模型合并效应量。Meta分析结果显示,短期随访组中,伯明翰髋关节表面置换组并发症发生率较全髋关节置换组稍高,但2组间差异无显著性意义(RR=1.28,95%CI(0.52,3.18),P=0.59);长期随访组中,伯明翰髋关节表面置换组总体并发症较全髋关节置换少,2组间差异有显著性意义(RR=0.28,95%CI(0.19,0.43), P < 0.000 01),见图3。"
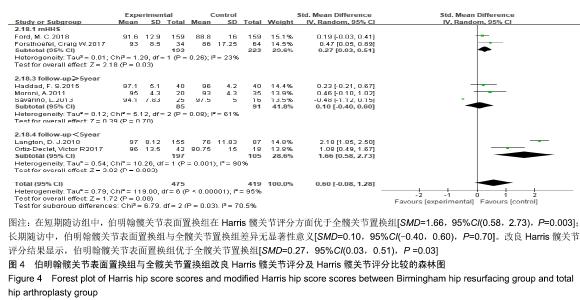
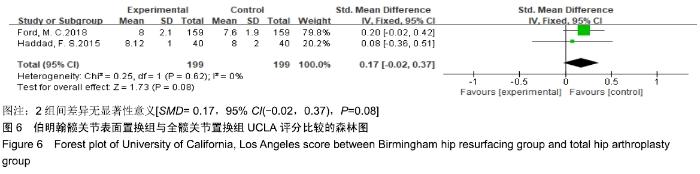
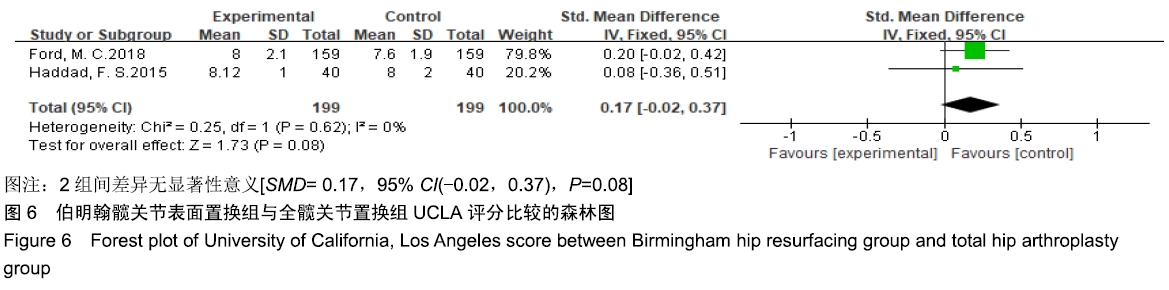
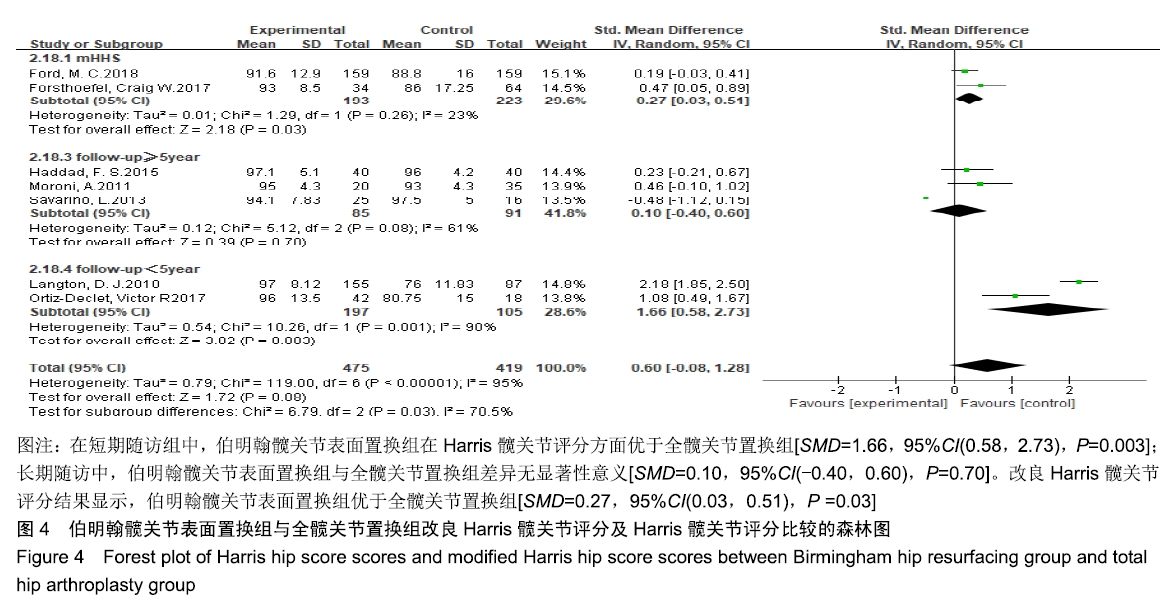
2.3.3 改良Harris髋关节评分及Harris髋关节评分 共有2篇文献报道了改良Harris髋关节评分[20,22],5篇文献报道了Harris髋关节评分[3,16,19,25-26],根据评分类型及随访时间分为3个亚组,分别为改良Harris髋关节评分组、短期随访组和长期随访组,由于各组异质性检验提示组间异质性较大,亚组分析后采用随机效应模型合并效应量。Meta分析结果显示,在短期随访组中,伯明翰髋关节表面置换组在Harris髋关节评分方面优于全髋关节置换组,组间差异有显著性意义[SMD=1.66,95%CI(0.58,2.73),P=0.003];长期随访中,伯明翰髋关节表面置换组与全髋关节置换组差异无显著性意义[SMD=0.10,95%CI(-0.40,0.60), P= 0.70]。改良Harris髋关节评分结果显示,伯明翰髋关节表面置换组优于全髋关节置换组,2组差异有显著性意义[SMD=0.27,95%CI(0.03,0.51),P=0.03],见图4。"
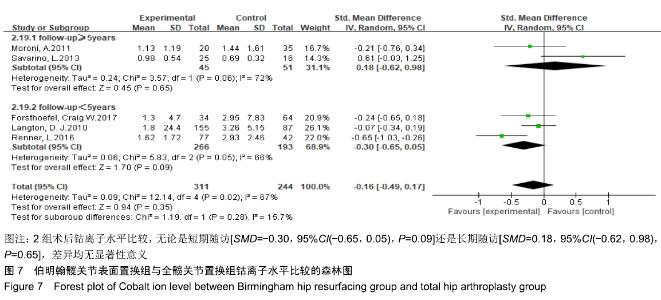
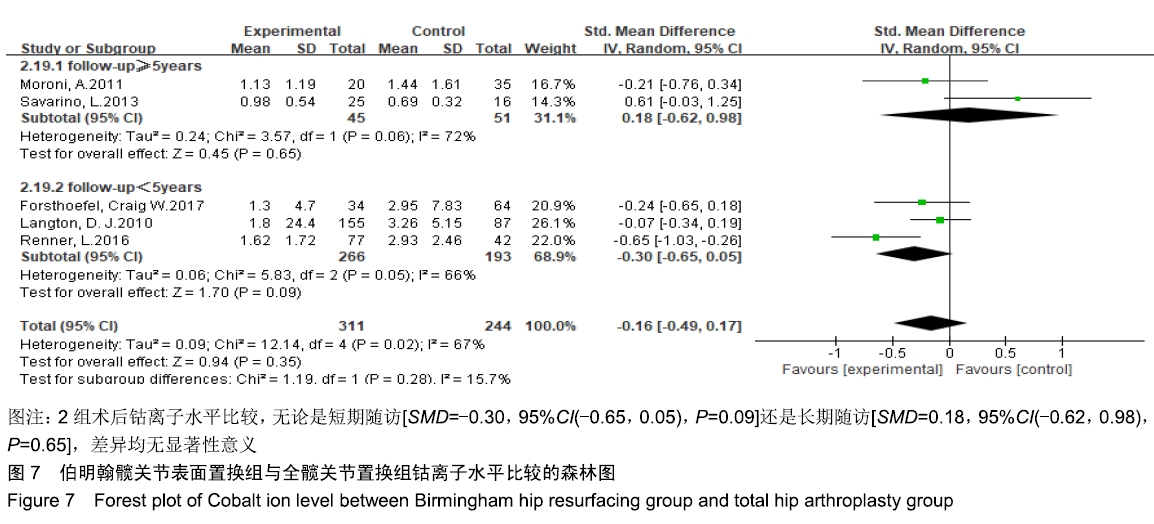
2.3.6 钴离子水平 共有5篇文献报道了钴离子水平[19,22-23,25-26],其中3篇为短期随访结果[19,22-23],2篇为长期随访结果[25-26],分为2个亚组,分别为短期随访组和长期随访组,由于2组异质性检验均提示有较高的异质性(短期随访组:I2=66%,P=0.05;长期随访组:I2=72%,P=0.06),故采用随机效应模型合并效应量。Meta分析结果显示,伯明翰髋关节表面置换组与全髋关节置换组在术后钴离子水平比较,无论是短期随访[SMD=-0.30,95%CI(-0.65,0.05), P=0.09]还是长期随访[SMD=0.18,95%CI(-0.62,0.98), P=0.65] ,见图7,2组差异均无显著性意义。"
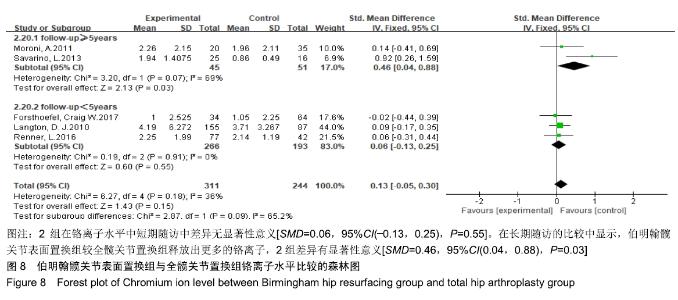
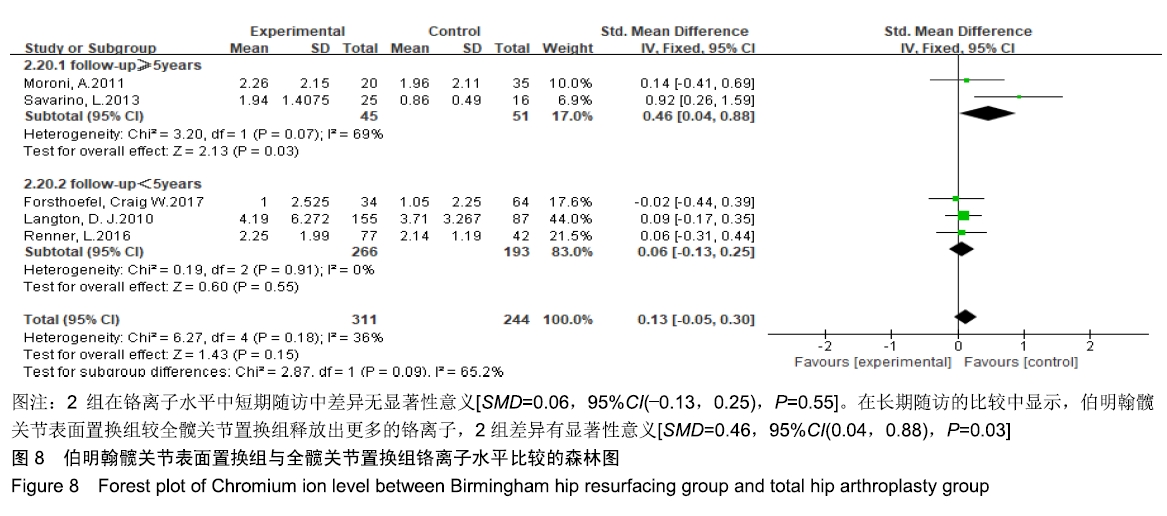
2.3.7 铬离子水平 共有5篇文献报道了铬离子水平[19,22-23,25-26],其中3篇为短期随访结果[19,22-23],2篇为长期随访结果[25-26],异质性检验结果显示在短期随访组间具有同质性(I2=0%,P=0.91),但是在长期随访组中提示异质性较高(I2=69%,P=0.07),采用固定效应模型合并效应量。Meta分析结果显示,伯明翰髋关节表面置换组与全髋关节置换组在术后铬离子水平比较,2组在短期随访中差异无显著性意义[SMD=0.06,95%CI(-0.13,0.25), P=0.55]。但是2组在长期随访的比较中发现,伯明翰髋关节表面置换组较全髋关节置换组释放出更多的铬离子,2组差异有显著性意义[SMD=0.46,95%CI(0.04,0.88),P=0.03],见图8。"

2.4 敏感度分析 此次研究对亚组分析后仍然无法消除异质性的观察指标,如Harris髋关节评分和钴离子水平。进行逐一排除单个研究后观察效应量是否发生明显改变的敏感度分析,以明确异质性来源。在长期随访的Harris髋关节评分组,剔除SAVARINO等[25]的研究后组间异质性消失,但是重新阅读全文后未见明显错漏,故异质性的来源可能来自于随访时间,因为HADDAD等[16]的随访时间为10年以上,而MORONI等[26]的观察时间在5年左右,但是SAVARINO等[25]的随访时间介于两者之间。在钴离子水平方面,在短期随访组中删除RENNER等[23]的研究后异质性消失,阅读全文后亦未发现明显错漏,异质性可能与不同研究中术者的手术操作技术水平高低有关。"

| [1] LEARMONTH ID, YOUNG C, RORABECK C. The operation of the century: total hip replacement. Lancet. 2007;370(9597): 1508-1519. [2] MCMINN D, TREACY R, LIN K, et al. Metal on metal surface replacement of the hip. Experience of the McMinn prothesis. Clin Orthop Relat Res. 1996;329 Suppl:S89-98. [3] ORTIZ-DECLET VR, IACOBELLI DA, YUEN LC, et al. Birmingham hip resurfacing vs total hip arthroplasty: a matched-pair comparison of clinical outcomes. J Arthroplasty. 2017;32:3647-3651. [4] UEMURA K, TAKAO M, HAMADA H, et al. Long-term results of birmingham hip resurfacing arthroplasty in asian patients. J Artif Organs. 2018;21:117-123. [5] HUNTER TJA, MOORES TS, MORLEY D, et al. 10-year results of the Birmingham Hip Resurfacing: a non-designer case series. Hip Int 2018;28:50-52. [6] OAK SR, STRNAD GJ, O'ROURKE C, et al. Mid-Term Results and Predictors of Patient-Reported Outcomes of Birmingham Hip Resurfacing. J Arthroplasty. 2017;32:110-118. [7] MURRAY DW, GRAMMATOPOULOS G, PANDIT H, et al. The ten-year survival of the Birmingham hip resurfacing: an independent series. J Bone Joint Surg Br. 2012;94:1180-1186. [8] TREACY RBC, MCBRYDE CW, SHEARS E, et al. Birmingham hip resurfacing: A minimum follow-up of ten years. J Bone Joint Surg. 2011;93 B:27-33. [9] DANIEL J, PRADHAN C, ZIAEE H, et al. Results of Birmingham hip resurfacing at 12 to 15 years: a single-surgeon series. Bone Joint J. 2014;96-B(10):1298. [10] SMITH TO, NICHOLS R, DONELL ST, et al. The clinical and radiological outcomes of hip resurfacing versus total hip arthroplasty: a meta-analysis and systematic review. Acta Orthopaedica. 2010;81:684-695. [11] VISHWANATHAN K, AKBARI K, PATEL AJ. Is the modified Harris hip score valid and responsive instrument for outcome assessment in the Indian population with pertrochanteric fractures? J Orthop. 2018;15:40-46. [12] NILSDOTTER A, BREMANDER A. Measures of hip function and symptoms: Harris Hip Score (hhs), Hip Disability and Osteoarthritis Outcome Score (HOOS), Oxford Hip Score (OHS), Lequesne Index of Severity for Osteoarthritis of the Hip (LISOH), and American Academy of Orthopedic Surgeons (AAOS) Hip and Knee Questionnaire. Arthritis Care Res (Hoboken). 2011;63 Suppl 11:S200-207. [13] COLLINS NJ, MISRA D, FELSON DT, et al. Measures of knee function: International Knee Documentation Committee (IKDC) Subjective Knee Evaluation Form, Knee Injury and Osteoarthritis Outcome Score (KOOS), Knee Injury and Osteoarthritis Outcome Score Physical Function Short Form (KOOS-PS), Knee Outcome Survey Activities of Daily Living Scale (KOS-ADL), Lysholm Knee Scoring Scale, Oxford Knee Score (OKS), Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Activity Rating Scale (ARS), and Tegner Activity Score (TAS). Arthritis Care Res (Hoboken). 2011;63 Suppl 11:S208-228. [14] HARRIS WH. Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am. 1969;51:737-755. [15] MOHER D, LIBERATI A, TETZLAFF J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7): e1000097. [16] HADDAD FS, KONAN S, TAHMASSEBI J. A prospective comparative study of cementless total hip arthroplasty and hip resurfacing in patients under the age of 55 years a ten-year follow-up. Bone Joint J. 2015;97B:617-622. [17] BARNES LAF, JOHNSON SH, PATRICK DA JR, et al. Metal-on-metal hip resurfacing compared with total hip arthroplasty: two to five year outcomes in men younger than sixty five years. Int Orthop. 2014;38:2435-2440. [18] MACKENZIE JR, O'CONNOR GJ, MARSHALL DA, et al. Functional outcomes for 2 years comparing hip resurfacing and total hip arthroplasty. J Arthroplasty. 2012;27:750-757. [19] LANGTON DJ, JAMESON SS, JOYCE TJ, et al. Early failure of metal-on-metal bearings in hip resurfacing and large-diameter total hip replacement: A consequence of excess wear. J Bone Joint Surg Br. 2010;92:38-46. [20] FORD MC, HELLMAN MD, KAZARIAN GS, et al. Five to ten-year results of the birmingham hip resurfacing implant in the u.s.: a single institution's experience. J Bone Joint Surg Am. 2018;100: 1879-1887. [21] HALAWI MJ, OAK SR, BRIGATI D, et al. Birmingham hip resurfacing versus cementless total hip arthroplasty in patients 55 years or younger: a minimum five-year follow-up. J Clin Orthop Trauma. 2017;9(4):285-288. [22] FORSTHOEFEL CW, BROWN NM, BARBA ML. Comparison of metal ion levels in patients with hip resurfacing versus total hip arthroplasty. J Orthop. 2017;14:561-564. [23] RENNER L, FASCHINGBAUER M, SCHMIDT-BRAEKLING T, et al. Cobalt serum levels differ in well functioning Birmingham resurfacing and Birmingham modular THA. Arch Orthop Trauma Surg. 2016;136:715-721. [24] PARRY MC, POVEY J, BLOM AW, et al. Comparison of acetabular bone resection, offset, leg length and post operative function between hip resurfacing arthroplasty and total hip arthroplasty. J Arthroplasty. 2015;30:1799-1803. [25] SAVARINO L, CADOSSI M, CHIARELLO E, et al. Do ion levels in metal-on-metal hip resurfacing differ from those in metal-on-metal THA at long-term followup? Clin Orthop Relat Res. 2013;471: 2964-2971. [26] MORONI A, SAVARINO L, HOQUE M, et al. Do ion levels in hip resurfacing differ from metal-on-metal THA at midterm? Clin Orthop Relat Res. 2011;469:180-187. [27] DANIEL J, PRADHAN C, ZIAEE H, et al. Results of Birmingham hip resurfacing at 12 to 15 years: a single-surgeon series. Bone Joint J. 2014;96-b:1298-1306. [28] CARR AM, DESTEIGER R. Osteolysis in patients with a metal-on-metal hip arthroplasty. ANZ J Surg. 2008;78:144-147. [29] HUK OL, CATELAS I, MWALE F, et al. Induction of apoptosis and necrosis by metal ions in vitro. J Arthroplasty. 2004;19:84-87. [30] LADON D, DOHERTY A, NEWSON R, et al. Changes in metal levels and chromosome aberrations in the peripheral blood of patients after metal-on-metal hip arthroplasty. J Arthroplasty. 2004;19:78-83. [31] SAVARINO L, GRANCHI D, CIAPETTI G, et al. Ion release in patients with metal-on-metal hip bearings in total joint replacement: a comparison with metal-on-polyethylene bearings. J Biomed Mater Res. 2002;63(5):467-474. [32] HUBER M, REINISCH G, TRETTENHAHN G, et al. Presence of corrosion products and hypersensitivity-associated reactions in periprosthetic tissue after aseptic loosening of total hip replacements with metal bearing surfaces. Acta Biomater. 2009; 5(1):172-180. [33] DAVIES AP, WILLERT HG, CAMPBELL PA, et al. An unusual lymphocytic perivascular infiltration in tissues around contemporary metal-on-metal joint replacements. J Bone Joint Surg Am. 2005;87(1):18-27. [34] BOSKER BH, ETTEMA HB, BOOMSMA MF, et al. High incidence of pseudotumour formation after large-diameter metal-on-metal total hip replacement: a prospective cohort study. J Bone Joint Surg Br. 2012;94(6):755-761. [35] ZHANG L, CHEN Z, LI L, et al. Metal ions levels between metal-on-metal total hip arthroplasty and metal-on-metal hip resurfacing arthroplasty: a meta-analysis. Int J Clin Exp Med. 2018;11:453-462. [36] GARBUZ DS, TANZER M, GREIDANUS NV, et al. The John Charnley Award: Metal-on-metal hip resurfacing versus large-diameter head metal-on-metal total hip arthroplasty: a randomized clinical trial. Clin Orthop Relat Res. 2010;468: 318-325. [37] HART AJ, SABAH SA, SAMPSON B, et al. Surveillance of patients with metal-on-metal hip resurfacing and total hip prostheses: a prospective cohort study to investigate the relationship between blood metal ion levels and implant failure. J Bone Joint Surg Am. 2014;96:1091-1099. [38] GILBERT JL, BUCKLEY CA, JACOBS JJ. In vivo corrosion of modular hip prosthesis components in mixed and similar metal combinations. The effect of crevice, stress, motion, and alloy coupling. J Biomed Mater Res. 1993;27(12):1533-1544. [39] HALLAB NJ, MESSINA C, SKIPOR A, et al. Differences in the fretting corrosion of metal-metal and ceramic-metal modular junctions of total hip replacements. J Orthop Res. 2004;22: 250-259. [40] TRAINA F, DE CLERICO M, BIONDI F, et al. Sex differences in hip morphology: is stem modularity effective for total hip replacement? J Bone Joint Surg. 2009;91 Suppl 6(S6):121-128. [41] GRAMMATOPOULOS G, PANDIT H, Oxford Hip and Knee Group, et al. The relationship between head-neck ratio and pseudotumour formation in metal-on-metal resurfacing arthroplasty of the hip. J Bone Joint Surg. 2010;92-B(11): 1527-1534. |
| [1] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [2] | Liu Jianyou, Jia Zhongwei, Niu Jiawei, Cao Xinjie, Zhang Dong, Wei Jie. A new method for measuring the anteversion angle of the femoral neck by constructing the three-dimensional digital model of the femur [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3779-3783. |
| [3] | Zou Shouping, Lu Daoyun, Ye Li. Minimally invasive percutaneous pedicle screw technique for thoracolumbar fractures: biomechanical changes of the spine during 6-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3865-3869. |
| [4] | Jiang Shengyuan, Li Dan, Jiang Jianhao, Shang-you Yang, Yang Shuye. Biological response of Co2+ to preosteoblasts during aseptic loosening of the prosthesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3292-3299. |
| [5] | Liu Pengran, Jiao Rui, Tao Jin, Chen Hui, Dai Jihang, Yan Lianqi. Comparison of the effects of total hip arthroplasty with different interface prostheses in the treatment of elderly hip diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2347-2351. |
| [6] | Li Yonghe, Wang Xiankang, Meng Yu, Liu Lu, Zhang Chunqiu, Ye Jinduo . Mechanical analysis on the position difference of short-stemmed prosthesis in hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2394-2399. |
| [7] | Ma Long, Tan Xiaoxin, Sun Guoshao. A 5-year follow-up on sagittal alignment and radiological outcomes of consecutive three-level anterior cervical discectomy and fusion and hybrid surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1879-1885. |
| [8] | Jing Yucheng, Wang Le, Wang Xianyun, Wei Mei, Li Min, Ji Lishuang, Ma Fangfang, Liu Gang , Zheng Mingqi. Umbilical cord mesenchymal stem cell transplantation in the treatment of ischemic heart disease: a 3-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(1): 6-12. |
| [9] | Milalimmu•Multiza, Zhao Wei, Varesjiang•Nyyaz, Yuan Hong, Wang Li. Direct anterior approach versus anterolateral approach in total hip arthroplasty: comparison of early postoperative patient’s perception [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1318-1323. |
| [10] | Huang Hetao, Pan Jianke, Yang Weiyi, Zeng Lingfeng, Liang Guihong, Liu Jun. Systematic evaluation of the efficacy and safety of collum femoris preserving prosthesis in total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(6): 962-967. |
| [11] | Zhang Yuda, Wang Changyao, Wang Xiangyu. Imaging evaluation after minimally invasive total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5379-5384. |
| [12] | Liu Changlu, Ma Libo, Liu Xiaomin, Huang Jian. Meta-analysis of efficacy and safety of short-stem versus long-stem hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 416-421. |
| [13] | Liu Tiansheng, Su Bin. Advantages and learning curve of direct anterior approach in total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(27): 4364-4369. |
| [14] | Hu Zhengxia, Lan Hai, Yuan Jin, Li Kainan. Total hip arthroplasty for senile femoral neck fractures: SuperPATH approach versus traditional posterolateral approach [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(24): 3834-3839. |
| [15] | Lin Jiebin, Shi Yuling, Gao Fenghe, Liang Zujian. Meta-analysis of efficacy of oral versus intravenous tranexamic acid in reducing blood loss after total knee and hip arthroplasties [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(24): 3925-3930. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||