Chinese Journal of Tissue Engineering Research
Previous Articles Next Articles
Concentrated red bone marrow/platelet-rich fibrin compound with an autologous periosteum debris scaffold for repair of mandibular defects
Guo Ling-yu, Liu Kai, Liu Shu-fa
- Department of Oral and Maxillofacial Surgery, Hospital of Stomatology, Jiamusi University, Jiamusi 154000, Heilongjiang Province, China
-
Received:2012-09-14Revised:2012-10-09Online:2013-05-21Published:2013-05-21 -
Contact:Liu Kai, Master, Attending physician, Department of Oral and Maxillofacial Surgery, Hospital of Stomatology, Jiamusi University, Jiamusi 154000, Heilongjiang Province, China lkdx1980@163.com -
About author:Guo Ling-yu★, Studying for master’s degree, Department of Oral and Maxillofacial Surgery, Hospital of Stomatology, Jiamusi University, Jiamusi 154000, Heilongjiang Province, China yuling861012@sina.com
CLC Number:
Cite this article
Guo Ling-yu, Liu Kai, Liu Shu-fa. Concentrated red bone marrow/platelet-rich fibrin compound with an autologous periosteum debris scaffold for repair of mandibular defects[J]. Chinese Journal of Tissue Engineering Research, doi: 10.3969/j.issn.2095-4344.2013.21.006.
share this article
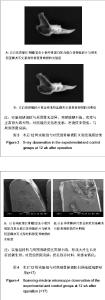
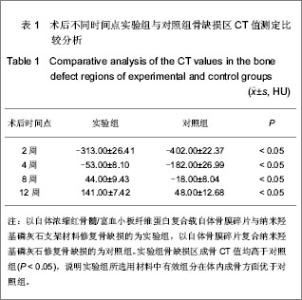
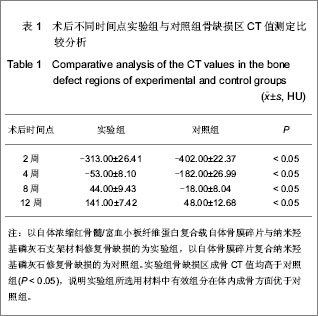
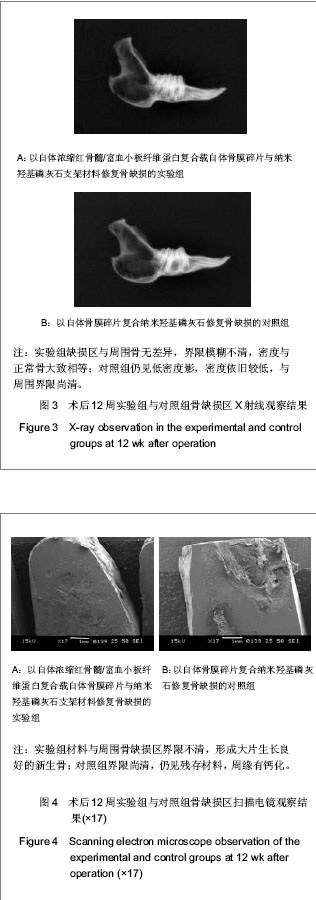
2.1 实验动物数量分析 36只兔均进入结果分析。 2.2 实验组与对照组术后不同时间点骨缺损处大体观察结果 术后2周时,实验组与对照组骨缺损区均有纤维状组织包裹,对照组多见炎性渗出,两组材料均有小部分吸收,与周围骨界限清,探针检测质地较软。术后4周时,实验组材料吸收明显,缺损边缘与周边骨结合较牢固,探测质地较硬;对照组纤维组织充填较多,质地软。术后8周时,实验组材料大部吸收,缺损区与周围骨无明显差异,硬度明显增加;对照组残存材料较多,硬度不及实验组。术后12周时,实验组缺损区骨膜包被,硬度与周围骨相当;对照组表面仍有纤维组织,硬度不明显。 2.3 实验组与对照组术后不同时间点骨缺损处X射线检测结果 术后2周时,实验组与对照组低密度影明显,有材料阻射影,与周围骨组织界清。术后4周时,实验组可见絮状高密度影,材料可见吸收,硬度增加,与周围正常骨边界尚清;对照组缺损区材料阻射影依旧清楚,低密度影多,与周围界限清。术后8周时,实验组区域可见均匀骨痂影像,有骨性连接,骨密度增加,与周围界限不清;对照组缺损区可见絮状高密度影,骨密度较低,与周围界限尚清。术后12周时,实验组缺损区与周围骨无差异,界限模糊不清,密度与正常骨大致相等;对照组仍见低密度影,密度依旧较低,与周围界限尚清,见图3。 2.4 实验组与对照组术后不同时间点骨缺损处扫描电镜检测结果 术后2周时,两组缺损区材料均与周围骨界限有裂隙。术后4周时,实验组材料与周围骨结合较紧,界限不清,有纤维组织长入,骨痂形成;对照组界限清楚,少量胶原纤维长入。术后8周时实验组材料与周围骨界限模糊,大量骨痂形成;对照组缺损区材料与周围骨界限不明显,少量骨痂形成。术后12周时,实验组材料与周围骨缺损区界限不清,形成大片生长良好的新生骨;对照组界限尚清,仍见残存材料,周缘有钙化,见图4。"

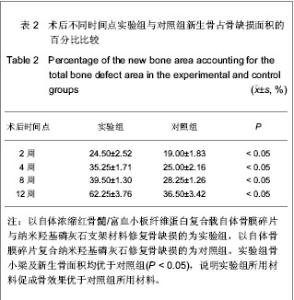
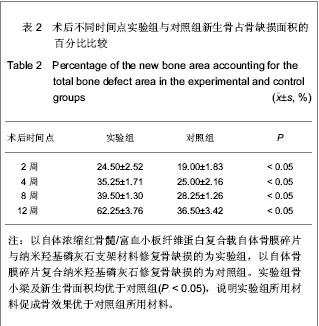
2.5 实验组与对照组术后不同时间点骨缺损处组织学检测结果 术后2周时,实验组缺损区内可见大量成骨细胞长入,细胞呈多角形,少量成纤维细胞和炎细胞浸润,红染骨基质明显;对照组可见大量成纤维细胞,炎细胞,少量成骨细胞,材料未见溶解吸收。术后4周时,实验组可见材料部分吸收,骨小梁致密成熟,可见丰富骨髓组织及骨陷窝;对照组材料吸收不明显,成骨细胞生成数量少,材料与周围界限清。术后8周时,实验组可见大量新生骨,骨小梁生成,材料吸收明显;对照组缺损区多见纤维组织和散在新生骨。术后12周时,实验组材料基本吸收,骨小梁形成规则,密度增大,皮质骨样结构增多,可见成熟骨外板和哈佛氏系统,生成骨髓组织内可见多样细胞;对照组材料残存,边界不清,材料内部多见纤维组织板状骨少见,多见纤维骨痂,骨小梁形成不规则,新生骨面积小,见图5。"

| [1] Dohan DM,Choukroun J,Diss A,et al.Platelet-rich fibrin (PRF):A second-generation platelet concentrate.Part II:Platelet-related biologic features.Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):E45-50.[2] Simonpieri A,Del Corso M,Sammartino G,et al. The relevance of Choukroun's platelet-rich fibrin and metronidazole during complex maxillary rehabilitations using bone allograft. Part I: a new grafting protocol.Implant Dent.2009;18(2):102-111.[3] Lundquist R,Dziegiel MH,Agren MS. Bioactivity and stability of endogenous fibrogenic factors in platelet-rich fibrin..Wound Repair Regen.2008;16 (3):356-363.[4] Simonpieri A,Choukroun J,Del Corso M,et al. Simultaneous sinus-lift and implantation using microthreaded implants and leukocyte-and platelet-rich fibrin as sole grafting material: a six-year experience.Implant Dent.2011;20(1):2-12.[5] Xie MM,Zhao BD,Wang WY,et al. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2010;14(16): 2911-2915.谢苗苗,赵保东,王维英,等.口腔修复膜材料在牙种植中引导骨再生的效应[J]. 中国组织工程研究与临床康复,2010,14(16): 2911-2915.[6] Soltan M,Smiler DG,Gailani F.A newplatinumstandard for bone grafting:autogenous stem cells.Implant Dent.2005;14 (4):322-325.[7] Hernigou P, Poignard A, Manicom O, et al. The use of percutaneousautologous bone marrow transplantation in nonunion and avascularnecrosis of bone.J Bone Joint Surg Br.2005;87(7):896-902.[8] Yeo C,Saunders N,Locca D,et al.Ficoll-Paque versus Lymphoprep:a comparative study of two density gradient media for therapeutic bone marrow mononuclear cell preparations.Regen Med.2009;4(5):689-696.[9] Zhang YC,Wu LM,Liu GH,et al.Linchuang Yiyao Shijian. 2010; 19(16):1044-1046.张远成,吴立明,刘国辉,等.自体骨髓干细胞移植在治疗骨不连中的疗效观察[J]. 临床医药实践,2010,19(16):1044-1046.[10] Sun QZ,Yan HY,Wang P,et al.Zhongguo Xiandai Yixue Zazhi. 2002;12(12): 25-27.孙庆仲,闫红艳,王鹏,等.自体骨膜细胞及红骨髓经皮注射修复骨缺损的实验研究[J].中国现代医学杂志,2002,12(12): 25-27.[11] Zou GY,Jiang F.Guangxi Yike Daxue Xuebao. 2003;20(1): 64-66.邹国耀,江峰.自体游离骨膜骨髓自固化磷酸钙复合移植治疗节段性骨缺损的实验研究[J].广西医科大学学报,2003,20(1): 64-66.[12] Ouyang L,Wang J.Hangkong Hangtian Yiyao. 2009;19(8): 59-60.欧阳林,王健.自体骨髓移植治疗骨折延迟愈合与不愈合的疗效观察[J].航空航天医药,2009,19(8):59-60. [13] Betz OB,Betz VM,Abdulazim A,et al.Healing of large segmental bone defects induced by expedited bone morphogenetic protein-2 gene-activated, syngeneic muscle grafts. Hum Gene Ther.2009;20(12):1589-1596.[14] Lacerda SA,Lanzoni JF,Bombonato-Prado KF,et al. Osteogenic potential of autogenous bone associated with bone marrow osteoblastic cells in bony defects: a histomorphometric study. Implant Dent.2009;18(6):521-529.[15] Yin SC,Jiao ZH,Wang GG,et al.Zhongguo Zhongyi Gushangke Zazhi. 2011;19(6):23-24.尹世昌,焦振华,王功国,等.浓缩自体骨髓移植配合中药治疗骨不连临床研究[J].中国中医骨伤科杂志,2011,19(6):23-24.[16] Yao WX,Ma A,Zhu LL,et al.Zhongguo Yixue Kexueyuan Xuebao. 2011;33(4):387-392.姚旺祥,马安,朱六龙,等.浓缩自体骨髓复合纤维蛋白胶修复兔桡骨陈旧性骨缺损[J].中国医学科学院学报,2011,33(4):387-392. [17] Lee K,Goodman SB. Cell therapy for secondary osteonecrosis of the femoral condyles using the Cellect DBM System: a preliminary report.J Arthroplasty.2009;24(1):43-48.[18] Pei M,He F,Boyce BM,et al.Repair of full-thickness femoral condyle cartilage defects using allogeneic synovial cell-engineered tissue constructs.Osteoarthritis Cartilage. 2009; 17(6):714-722.[19] Fu ZC.Yatai Chuantong Yiyao. 2011;7(4):4-5.付振才.复合PRP联合bBMP组织工程骨修复兔桡骨缺损的实验研究[J].亚太传统医药,2011,7(4):4-5.[20] Choukroun J,Adda F,Schoeffler C,et al.Une opportunité en paro-implantologie: le PRF.Implantodontie.2000;42:55-62 .[21] Cieslik-Bielecka A,Bielecki T,Gazdzik TS,et al. Improved treatment of mandibular odontogenic cysts with platelet-rich gel .Oral Surg Oral Med Oral Pathol Oral Radiol Endod.2008; 105(4):423-429.[22] Wildemann B,Schmidmaier G,Brenner N,et al. Quantification, localization, and expression of IGF-I and TGF-β1 during growth factor-stimulated fracture healing.Calcif Tissue Int. 2004;74(4):388-397.[23] Nakajima F,Nakajima A,Ogasawara A,et al.Effects of a single percutaneous injection of basic fibroblast growth factor on the healing of a closed femoral shaft fracture in the rat.Calcif Tissue Int.2007;81(2):132-138.[24] Chang Y,Hsieh PH,Chao CC.The efficiency of Percoll and Ficoll density gradient media in the isolation of marrow derived human mesenchymal stem cells with osteogenic potential.Chang Gung Med J.2009;32(3):264-275.[25] Sharma S,Garg NK,Veliath AJ,et al.Percutaneous bone-marrow grafting of osteotomies and bony defects in rabbits.Acta Orthopaedica Scandinavica. 1992;63(2): 166-169. [26] Wang BL,Sun W,Shi ZC,et al.Treatment of nontraumatic osteonecrosis of the femoral head with the implantation of core decompression and concentrated autologous bone marrow containing mononuclear cells. Arch Orthop Trauma Surg.2010;130(7):859-865.[27] Ma JT,Yu M,Zhang MC,et al.Clinical observation on percutaneous autologous bone marrow grafting for treatment of fracture nonunion.Zhongguo Gu Shang.2009;22(11): 862-864.[28] Zhang M,Yang ZX,Shi ZY,et al.Zhongguo Linchuang Kangfu. 2005;9(30):75-77.张明,杨智贤,石展英,等.自体骨泥混入骨膜碎片植骨与单纯自体骨泥植骨修复骨缺损的效果对比实验[J].中国临床康复,2005, 9(30):75-77.[29] Yang XM,Shi W,Du YK,et al.Zhongguo Xiufu Chongjian Waike Zazhi. 2009;23(10):1254-1259.杨新明,石蔚,杜雅坤,等.带蒂筋膜瓣包裹自体红骨髓接种的组织工程骨修复骨缺损的实验研究[J].中国修复重建外科杂志,2009, 23(10):1254-1259.[30] Ueno T,Kagawa T,Fukunaga J,et al. Evaluation of osteogenic/chondrogenic cellular proliferation and differentiation in the xenogeneic periosteal graft.Ann Plast Surg.2002;48(5):539.[31] Wang DX,Mou SL,Wang JR,et al.Zhongguo Jiaoxing Waike Zazhi. 2009;17(22):1735-1738.王代宪,牟淑玲,王建然,等.负载骨形态发生蛋白与血管内皮生长因子的超聚消旋乳酸修复兔桡骨缺损的实验研究[J].中国矫形外科杂志,2009,17(22):1735-1738. |
| [1] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [2] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [3] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [4] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [5] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [6] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [7] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [8] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [9] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [10] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [11] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [12] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [13] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [14] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [15] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||