Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (13): 2358-2367.doi: 10.3969/j.issn.2095-4344.2013.13.012
Previous Articles Next Articles
Repairing ankle lateral collateral ligament chronic injury using different methods: A stability assessment
Jiao Chen, Hu Yue-lin, Guo Qin-wei, Wang Cheng, Mei Yu, Xie Xing, Yang Yu-ping, Chen Lin-xin, Jiang Dong
- Institute of Sports Medicine, Peking University Third Hospital, Beijing 100191, China
-
Received:2012-10-24Revised:2012-12-22Online:2013-03-26Published:2013-03-26 -
Contact:Hu Yue-lin, Chief physician, Institute of Sports Medicine, Peking University Third Hospital, Beijing 100191, China sportshyl@sina.com -
About author:Jiao Chen☆, Doctor, Associate chief physician, Institute of Sports Medicine, Peking University Third Hospital, Beijing 100191, China jiaoshuj@mail.tsinghua.edu.cn
CLC Number:
Cite this article
Jiao Chen, Hu Yue-lin, Guo Qin-wei, Wang Cheng, Mei Yu, Xie Xing, Yang Yu-ping, Chen Lin-xin, Jiang Dong. Repairing ankle lateral collateral ligament chronic injury using different methods: A stability assessment[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(13): 2358-2367.
share this article
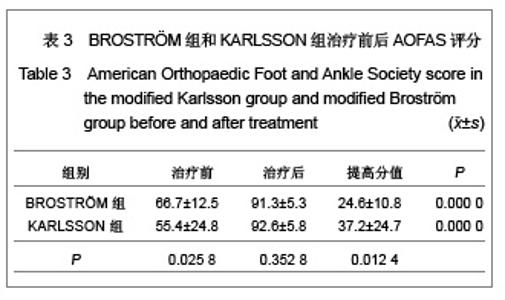
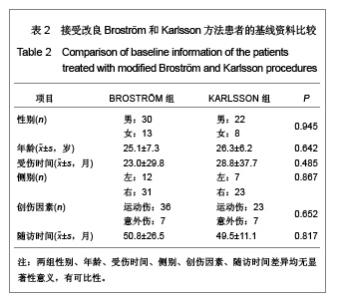
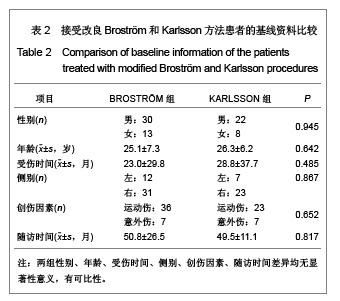
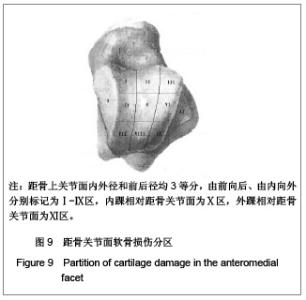
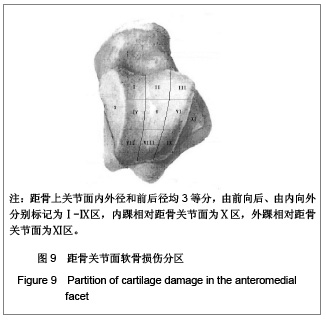
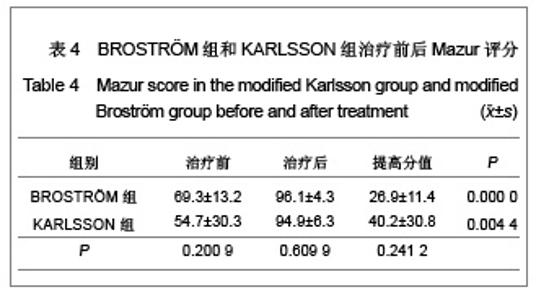
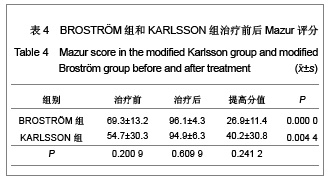
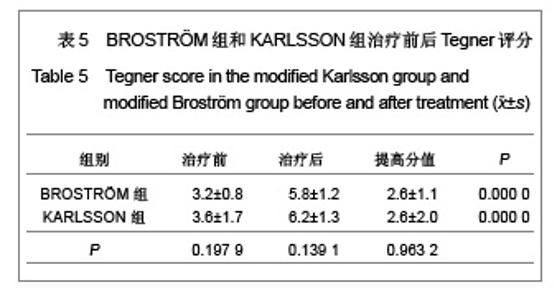
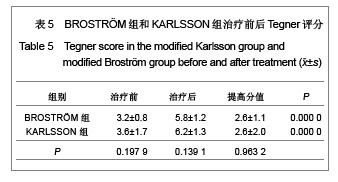
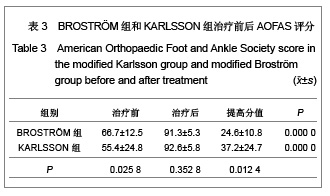
距骨上关节面内外径和前后径均3等分,由前向后、由内向外分别标记为Ⅰ-Ⅸ区,内踝相对距骨关节面为Ⅹ区,外踝相对距骨关节面为Ⅺ区。胫骨关节面与之相对同样分为11个区。发生软骨损伤的部位42处,其中距骨Ⅰ区为11例,距骨Ⅲ区6例,距骨Ⅳ区1例,距骨Ⅴ区1例,距骨Ⅵ区2例,距骨Ⅸ区1例,距骨Ⅹ区3例,距骨Ⅺ区4例;胫骨Ⅰ区6例,胫骨Ⅱ区2例,胫骨Ⅲ区2例,胫骨Ⅹ区2例,胫骨Ⅺ区1例。踝关节内侧部分(Ⅰ、Ⅳ、Ⅶ和Ⅹ区)软骨损伤共23处,占54.8%,而距胫关节前内侧关节面(距骨Ⅰ区和胫骨Ⅰ区)软骨损伤共17处,占所有软骨损伤的40.5%。 2.4 患者治疗后AOFAS评分、Mazur评分和Tegner评分 BROSTRÖM组和KARLSSON组患者治疗后AOFAS评分、Mazur评分和Tegner评分较术前均有明显的提高。KARLSSON组患者治疗前AOFAS评分明显低于BROSTRÖM组,但治疗后AOFAS评分两组无明显差异,AOFAS提高的分值KARLSSON组明显高于BROSTRÖM组,见表3。两组治疗前和治疗后的Mazur评分、Tegner评分及其提高的分值差异均无显著性意义,见表4,5。"

两组患者术后随访时均进行抽屉试验和内翻应力试验检查。BROSTRÖM组有2例患者均在术后1年再次内翻扭伤,伤后1例患者前抽屉试验阳性,内翻试验阴性,另1例患者两试验均阳性。经过中立位石膏固定3周后,前者两试验均阴性,后者两试验仍均为阳性。其他患者随访时两试验均为阴性。KARLSSON组1例患者术后1年再次扭伤(内翻伤),伤后前抽屉试验阳性,内翻应力试验阴性,诊断为“距腓前韧带再断裂”,予以中立位石膏固定3周,复查抽屉试验和内翻应力试验均为阴性,此后未再伤。其余患者两试验均为阴性。 2.5 患者预后结果 BROSTRÖM组1例再伤患者(上述前者)经石膏固定后痊愈,未再扭伤,另1例此后再次扭伤2次,有不稳感,该2例均可参加娱乐性体育运动。KARLSSON组再伤患者经石膏固定后痊愈,未再发生损伤,无不稳症状,可参加竞技性体育运动(足球)。 2.6 患者满意度测评结果 BROSTRÖM组患者的满意度平均为7.3(3-9),Karlsson组患者的满意度平均为7.6(6-8),两组比较差异无显著性意义(P=0.684 9)。 2.7 患者手术时间 BROSTRÖM组患者的平均手术时间为(91.5±24.5) min,KARLSSON组患者的平均手术时间为(73.3±14.5) min,两组比较差异无显著性意义(P=0.000 2)。 2.8 患者治疗后不良反应 所有73例患者治疗后未发生感染、神经损伤、骨折、固定锚钉脱出或断裂和关节粘连等并发症。2例合并距下关节损伤的患者,治疗后相应部位仍遗留慢性疼痛,其中1例经理疗后缓解。"

| [1] Brand RL, Collins MD. Operative management of ligamentous injuries to the ankle. Clin Sports Med.1982; 1:117-130.[2] Maehlum S, Daljord OA.Acute sports injuries in Oslo: a one year study. Br J Sports Med.1984;18:181-185.[3] Garrick JG. The frequency of injury, mechanism of injury and epidemiology of ankle sprains. Am J Sports Med.1977; 5: 241-242.[4] Takao M, Oae K, Uchio Y,et al. Anatomical Reconstruction of the Lateral Ligaments of the Ankle With a Gracilis Autograft: A New Technique Using an Interference Fit Anchoring System. Am J Sport Med.2005;33:814-823.[5] Colville MR, Marder RA, Boyle JJ, et al.Strain measurement in lateral ankle ligament. Am J Sports Med. 1990;18:196-200.[6] Komenda GA, Ferkel RD. Arthroscopic findings associated with the unstable ankle. Foot Ankle Int.1999;20:708-713.[7] Okuda R, Kinoshita M, Morikawa J, et al. Arthroscopic Findings in Chronic Lateral Ankle Instability: Do Focal Chondral Lesions Influence the Results of Ligament Reconstruction? Am J Sports Med.2005; 33:35-42.[8] Karlsson J, Lansinger O. Lateral instability of the ankle joint. Clin Orthop. 1992;276:253-261.[9] Gould N, Seligson D, Gassman J.Early and late repair of lateral ligaments of the ankle. Foot Ankle.1980;1:84-89.[10] Shino K, Nakagawa S, Inoue M,et al.Deterioration of patellofemoral articular surfaces after anterior cruciate ligament reconstruction. Am J Sports Med.1993;21:201-211.[11] Mazur JM, Schwartz E, Simon SR. Ankle arthrodesis. Long-term follow-up with gait analysis.J Bone Joint Surg Am. 1979;61(7):964-975.[12] Tegner Y, Lysholm J.Rating system in the evaIuation of knee liga-ment injury.Clin Orthop Relat Res.1984;198:43-49.[13] Hintermann B, Boss A, Schafer D. Arthroscopic findings in patients with chronic ankle instability. Am J Sports Med.2002; 30:402-409.[14] Van Dijk CN, Bossuyt PM, Marti RK. Medial ankle pain after lateral ligament rupture. J Bone Joint Surg Br. 1996; 78: 562-567.[15] Noguchi K.Biomechanical analysis for osteoarthritis of the ankle. Nippon Seikeigeka Gakkai Zasshi.1985;59:215-222.[16] Krips R, Van Dijk CN, Halasi T, et al. Anatomical reconstruction versus tenodesis for the treatment of chronic anterolateral instability of the ankle joint: a 2- to 10-year follow-up, multicenter study. Knee Surg, Sports Traumatol, Arthrosc. 2000;8:173-179.[17] Snook GA, Chrisman OD, Wilson TC. Long-term results of the Chrisman- Snook operation for reconstruction of the lateral ligaments of the ankle. J Bone Joint Surg Am.1985; 67: 1-7.[18] Becker HP, Ebner S, Ebner D, et al. 12-year outcome after modified Watson-Jones tenodesis for ankle instability. Clin Orthop.1999;358:194-204.[19] Solakoglu C, Kiral A, Pehlivan O, et al. Late-term reconstruction of lateral ankle ligaments using a split peroneus brevis tendon graft (Colville’s technique) in patients with chronic lateral instability of the ankle. International Orthopaedics.2003;27:223-227.[20] Krips R,Van Dijk CN, Halasi T,et al.Long-term outcome of anatomical reconstruction versus tenodesis for the treatment of chronic anterolateral instability of the ankle joint: a multicenter study.Foot Ankle Int. 2001;22:415-421.[21] Sugimoto K, Takakura Y, Kumai T, et al. Reconstruction of the Lateral Ankle Ligaments with Bone-Patellar Tendon Graft in Patients with Chronic Ankle Instability: A Preliminary Report. Am J Sports Med.2002;30:340-346.[22] Pagenstert GI,Valderrabano V,Hintermann B.Lateral Ankle Ligament Reconstruction With Free Plantaris Tendon Graft. Techniques in Foot and Ankle Surgery.2005;4:104-112.[23] Gould N.Repair of lateral ligament of ankle. Foot Ankle. 1987;8:55-58.[24] Nakata K, Shino K, Horibe S, et al. Reconstruction of the lateral ligaments of the ankle using solvent-dried and gamma-irradiated allogeneic fascia lata. J Bone Joint Surg Br. 2000;82:579-582.[25] Wainright WB, Spritzer CE, Lee JY, et al. The effect of modified Broström-Gould repair for lateral ankle instability on in vivo tibiotalar kinematics.Am J Sports Med 2012;40: 2099-2104.[26] Brostrom L.Sprained ankle. VI: Surgical treatment of “chronic” ligament ruptures. Acta Chir Scan. 1996;243:551-565[27] Colville MR.Surgical treatment of the unstable ankle. J Am Acad Orthop Surg. 1998;6:368-377.[28] Su EP, Healey JH. Salvage reconstruction for lateral ankle instability using a tendon allograft. Clin Orthop 2003;415: 232-238.[29] Ellis SJ, Williams BR, Pavlov H, et al. Results of anatomic lateral ankle ligament reconstruction with tendon allograft HSS J. 2011;7:134-140.[30] Kakarala G,Rajan DT.Anterior Talo-fibular ligament reconstruction using synthetic ligament and the extensor digitorum brevis. Clin J Sport Med. 2006;16:366-368.[31] Cook JJ, Cook EA. Bioscaffolds and the reconstruction of ligaments and tendons in the foot and ankle. Clin Podiatr Med Surg 2009;26:535-543.[32] Usami N, Inokuchi S, Hiraishi E, et al.Clinical application of artificial ligament for ankle instability--long-term follow-up. J Long Term Eff Med Implants. 2000;10(4):239-250.[33] Schroven IT, Geens S, Beckers L, et al: Experience with the Leeds-Keio artificial ligament for anterior cruciate ligament reconstruction, Knee Surg Sports Traumatol Arthrosc, 1994; 2:4:214-218.[34] Lukianov AV, Gillquist J, Grana WA, et al. An anterior cruciate ligament (ACL) evaluation format for assessment of artificial or autologous anterior cruciate reconstruction results. Clin Orthop 1987;218:167-180.[35] Larson RL. Synthetic materials for the replacement of knee ligaments, Ann Chir Gynaecol 1991;80:149-154.[36] Guidoin M, Marois Y, Bejui J, et al. Analysis of retrieved polymer fiber based replacements for the ACL. Biomaterials 2000;21:2461-2474.[37] Laurencin CT, Freeman JW. Ligament tissue engineering: An evolutionary materials science approach. Biomaterial 2005; 26:7530-7536.[38] Pederson B, Tesoro D, Wertheimer SJ, et al. Mitek anchor system: a new technique for tenodesis and ligamentous repair of the foot and ankle.J Foot Surg. 1991;30:48-51.[39] Messer TM, Cummins CA, Ahn J, et al. Outcome of the modified Broström procedure for chronic lateral ankle instability using suture anchors. Foot Ankle Int. 2000;21: 996-1003.[40] Rupp S, Georg T, Gauss C, Kohn D, et al. Fatigue testing of suture anchors. Am J Sports Med. 2002;30:239-247.[41] Waldrop NE 3rd, Wijdicks CA, Jansson KS, et al. Anatomic suture anchor versus the Broström technique for anterior talofibular ligament repair: a biomechanical comparison. Am J Sports Med 2012;40:2590-2596[42] Giza E, Nathe R, Nathe T, et al. Strength of bone tunnel versus suture anchor and push-lock construct in Broström repair. Am J Sports Med. 2012;40:1419-1423[43] Ilahi OA, Younas SA, Ho DM, et al. Security of knots tied with ethibond, fiberwire, orthocord, or ultrabraid. Am J Sports Med. 2008;36:2407-2414.[44] Karlsson J,Eriksson BI,Bergsten T,et al.Comparison of two anatomic reconstructions for chronic lateral instability of the ankle joint. Am J Sports Med.1997;25:48-53.[45] Bell SJ, Mologne TS, Sitler DF, et al. Twenty-six-year results after Broström procedure for chronic lateral ankle instability. Am J Sports Med.2006;34:975-978.[46] Takebayashi T, Yamashita T, Minaki Y, et al. Mechanosensitive afferent units in the lateral ligament of the ankle. J Bone Joint Surg Br.1997;79:490-493.[47] Kynsburg A, Halasi T, Tállay A, et al. Changes in joint position sense after conservatively treated chronic lateral ankle instability. Knee Surg Sports Traumatol Arthrosc.2006;14: 1299-1306.[48] Halasi T, Kynsburg A, Tállay A, et al. Changes in joint position sense after surgically treated chronic lateral ankle instability. Br J Sports Med 2005;39;818-824.[49] O’Connor D. Sinus tarsi syndrome: A clinical entity. J Bone Joint Surg Am.1958;66:720.[50] Beltran J, Munchow AM, Khabiri H, et al. Ligaments of the lateral aspect of the ankle and sinus tarsi: An MR imaging study. Radiology.1990;177:455-458.[51] Klein MA, Spreitzer AM. MR imaging of the tarsal sinus and canal: Normal anatomy, pathologic findings, and features of the sinus tarsi syndrome. Radiology.1993;186:233-240.[52] Lektrakul N, Chung CB, Lai YM, et al. Tarsal sinus: Arthrographic, MR imaging, MR arthrographic, and pathologic findings in cadavers and retrospective study data in patients with sinus tarsi syndrome. Radiology.2001;219:802-810.[53] Parisien JS, Vangsness T. Arthroscopy of the subtalar joint: An experimental approach. Arthroscopy.1985;1:53-57.[54] Williams MM,Ferkel RD.Subtalar arthroscopy: Indications, technique, and results. Arthroscopy 1998;14:373-381.[55] Goldberger MI, Conti SF.Clinical outcome after subtalar arthroscopy.Foot Ankle Int 1998;19:462-465.[56] Lowy A, Schilero J, Kanat IO. Sinus tarsi syndrome: A postoperative analysis. J Foot Surg 1985;24:108-112.[57] Frey C,Feder KS,DiGiovanni CW.Arthroscopy deconstructs sinus tarsi diagnosis. Biomechanics 1999;6:57-62.[58] Lee KB, Bai LB, Song EK, et al. Subtalar arthroscopy for sinus Tarsi syndrome: arthroscopic findings and clinical outcomes of 33 consecutive cases. Arthroscopy.2008;24: 1130-1134. |
| [1] | Chen Zehua, Ye Xiangling, Chen Weijian, Du Jianping, Liu Wengang, Xu Xuemeng. Effect of pronated foot posture on proprioception and postural stability based on foot posture index [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1324-1328. |
| [2] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [3] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [4] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [5] | Wang Jiangna, Zheng Huifen, Sun Wei. Changes in dynamic stability, motor coordination and joint mechanics of the lower extremity during stair descent and performing phone task [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 837-843. |
| [6] | Kong Lingbao, Lü Xin. Effect of implant selection and approach on support in the operation of posterolateral tibial plateau fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 942-947. |
| [7] | Zheng Li, Li Dadi, Hu Weifan, Tang Jinlong, Zhao Fengchao. Risk assessment of contralateral knee arthroplasty after unilateral total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 374-379. |
| [8] | Huang Youyi, Yuan Wei. Application of 3D printing technology in fracture and deformity of foot and ankle [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 438-442. |
| [9] | Xie Chengxin, Wang Wei, Wang Chenglong, Li Qinglong, Yin Dong. Systematic review and meta-analysis of bone morphogenetic protein for the treatment of acute tibial fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 486-492. |
| [10] | Liu Fang, Shan Zhengming, Tang Yulei, Wu Xiaomin, Tian Weiqun. Effects of hemostasis and promoting wound healing of ozone sustained-release hydrogel [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3445-3449. |
| [11] | Zhao Hongshun, A Jiancuo, Wang Deyuan, Xu Zhihua, Gao Shunhong. Factors affecting the height of early intervertebral space after lumbar interbody fusion via lateral approach [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3332-3336. |
| [12] | Li Yuefei, Li Rui, Ren Jiabin, Liu Xin, Sun Ning, Liu Weike, Bi Jingwei, Sun Zhaozhong. Three-dimensional CT analysis of the treatment of thoracic disc herniation by percutaneous endoscopic posterolateral approach: establishment of a good osseous channel [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3354-3359. |
| [13] | Peng Chao, Liu Yunpeng, Hua Guojun, Yang Jiaji, Wang Xingliang, Wang Xiaolong. Imaging evaluation of the hip-knee-ankle angle and osteoarthritis progression before and after partial meniscectomy for degenerative medial meniscus posterior root tear [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3368-3373. |
| [14] | Zheng Kai, Li Rongqun, Sun Houyi, Zhang Weicheng, Li Ning, Zhou Jun, Zhu Feng, Wang Yijun, Xu Yaozeng. Computer-navigated versus conventional one-stage bilateral total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3305-3312. |
| [15] | Dong Liping, Luo Huaiqing, Yuan Heng, Long Juan, Xu Shaohui. Effect of aging on collateral vessel growth in rats with ischemic hind limbs [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3156-3161. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||