Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (20): 3235-3241.doi: 10.3969/j.issn.2095-4344.1191
Previous Articles Next Articles
Diagnosis and treatment of deltoid ligament injury of ankle joint
Wang Guixin, He Jinquan
- First Department of Foot and Ankle Surgery, Tianjin Hospital, Tianjin 300211, China
-
Online:2019-07-18Published:2019-07-18 -
Contact:He Jinquan, Chief physician, First Department of Foot and Ankle Surgery, Tianjin Hospital, Tianjin 300211, China -
About author:Wang Guixin, Master, Attending physician, First Department of Foot and Ankle Surgery, Tianjin Hospital, Tianjin 300211, China -
Supported by:the Science and Technology Foundation of Tianjin Hospital in 2017, No. TJYY1605 (to WGX)
CLC Number:
Cite this article
Wang Guixin, He Jinquan. Diagnosis and treatment of deltoid ligament injury of ankle joint[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(20): 3235-3241.
share this article

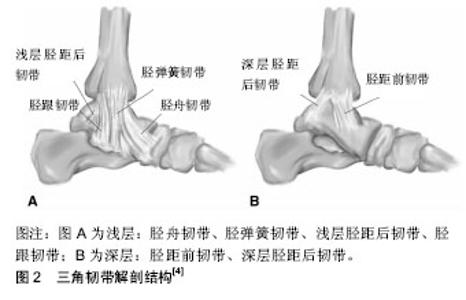
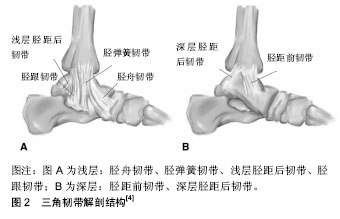
三角韧带浅层由4个部分组成,其中胫弹簧韧带和胫舟韧带是通常都存在的,而胫距浅韧带和胫跟韧带则存在着变异。其中,胫舟韧带由于其近端非常贴近关节囊,所以在实际解剖中很难将胫舟韧带独立的分离出 来[6]。Cromeens等[3]认为胫舟韧带和胫跟韧带是一个独立的解剖结构,只是远端存在2个不同的止点,称之为胫跟舟韧带。三角韧带浅层韧带可以维持距骨和内踝的力线,对抗距骨相对于胫骨的外旋和外翻应力[6]。三角韧带深层是由深层的胫距前韧带与胫距后韧带组成,其中,深层的胫距后韧带是恒定存在,深层的胫距前韧带则存在着变异。三角韧带深层有防止距骨外移和外旋的作用,同时可以起到稳定踝关节,防止踝关节过度跖屈和外旋的作用[7]。多数学者认为与浅层相比三角韧带深层稳定踝关节作用更明显,原因在于三角韧带浅层断裂时距骨轻度移位或无移位时踝关节仍处于稳定状态,而浅深两层断裂完全时距骨倾斜度增加至14°,此时踝关节严重失稳。总之,三角韧带具有维持胫距跟复合关节稳定的重要作用[8],见表1。"
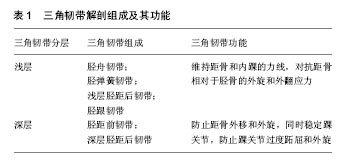

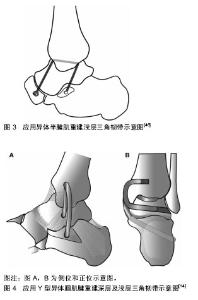
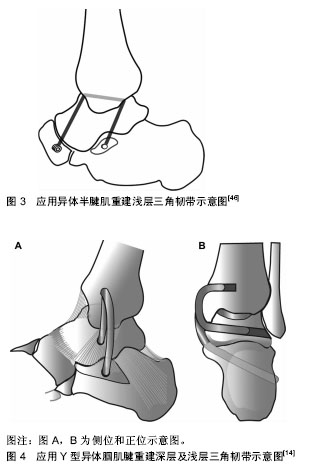
2.2 踝关节三角韧带的损伤及其诊断 2.2.1 踝关节三角韧带的损伤机制 三角韧带的急性损伤:三角韧带急性损伤占所有踝关节损伤的10%-15%,损伤主要是由于踝关节外翻或者外旋导致的[9]。典型的损伤是失去平衡时,足在旋前位着地引起。此时,旋前或外翻的暴力导致踝关节的外旋或外展。这种损伤经常发生在不平坦的地面上行走或跑步,或在不平坦的地面上跳跃和着陆时。单纯急性三角韧带损伤非常罕见,多伴有下胫腓联合损伤、距骨骨软骨损伤或踝关节骨折[10]。在踝关节急性损伤Lauge-Hansen分类中,旋后外旋(SER)、旋前外旋(PER)及旋前外展这3种损伤类型,均有可能发生三角韧带损伤,其中以旋后外旋型最为常见[11]。 三角韧带的慢性损伤:严重的踝关节扭伤可以导致踝关节内侧三角韧带的损伤,当这种损伤被忽视并且没有得到有效诊治时,就会出现三角韧带的慢性损伤,其表现为踝关节内侧的慢性不稳定[12]。俞光荣等[13]研究发现三角韧带的慢性损伤,会引起距骨的跖屈和过度旋前,最终会导致内侧足弓的塌陷,后足外翻以及踝关节内侧不稳定的发生。在平足畸形中,胫后肌腱功能不全使内侧足弓的塌陷,踝关节内侧结构,三角肌韧带,以及弹簧韧带受到持续性的张力刺激,会产生对于三角韧带的慢性损伤,最终致使三角韧带功能的丧失,导致跟骨外翻,踝穴内距骨外翻,形成Ⅳ期成人获得性扁平足畸形[14]。 2.2.2 踝关节三角韧带损伤的临床表现及体征 三角韧带损伤主要表现为内踝局部有淤血肿胀、内踝部压痛及踝关节不稳定[4]。患者在运动或者正常生活中,经常会出现,由于踝关节内侧不稳定而感到的踝关节“无力感”[15]。踝关节对于内侧不稳定的适应能力很差。Femino等[16]描述了踝关节内侧三角韧带功能不全时在行走末期摆动期间距骨会产生微小旋转半脱位,此时后足处于内翻位置,当跟骨受到一个外翻应力,将影响距骨内旋恢复到正常的位置。这种额外旋转应变随时间的累积将损伤胫距关节的软骨细胞,这可能是导致创伤后关节炎的危险因素[17]。 大量的慢性踝关节外侧不稳定的患者均伴有踝关节内侧的不稳定,可出现踝关节内侧疼痛,行走无力,以及后足的旋前畸形,同时核磁研究发现72%的慢性踝关节不稳定患者存在有三角韧带损伤,踝关节外侧腓骨下端的撞击疼痛也可能是由慢性踝关节三角韧带损伤导致的跟骨外翻引起的[18]。 绝大多数的学者认为成人获得性平足症是由于胫后肌腱功能不全引起的,但Alshalawi等[12]发现有的非对称性平足症患者在进行提踵试验时,跟骨的外翻是可以纠正的,这说明这部分患者胫后肌腱功能正常,因此Alshalawi等[12]认为这样的平足畸形是由于慢性三角韧带损伤引起的踝关节内侧不稳定而导致的。 2.2.3 踝关节三角韧带损伤的诊断方法 应力位X射线片:非应力状态下,通过踝穴位X射线片上,踝穴内侧间隙的大小来判断三角韧带损伤程度,仍然存在很大的争论,但通常认为,内侧间隙大于4 mm且大于胫距关节间隙1 mm,则提示三角韧带断裂[4]。应力位的X射线检查,是判断踝关节内侧结构完整性以及踝关节稳定性客观且非常重要的检查手段[19]。应力位X射线检查最好是在麻醉下进行,通过重力或者手法外力进行外翻或外旋的检查。Leba等[20]比较了手动施加外力与通过自身重力进行应力下的影像学检查,发现两者的检查结果相当,而重力下的应力位拍片患者疼痛较轻,同时减少了医生在射线中的暴露,因此更具有优势。对于应力位X射线检查也存在不同的观点。Schottle等[21]认为不能单独应用应力位X射线检查来确诊三角韧带的损伤,他们推荐当应力下X射线检查内侧间隙达到5 mm时,还应结合其他影像学检查来提高诊断的准确性。Alshalawi等[12]则认为应力位的X射线检查对于诊断踝关节内侧不稳定或者踝关节旋转不稳定是无效的,而且会造成局部的疼痛,甚至加重损伤。 磁共振成像(MRI)检查:MRI被广泛认为是评估软组织病变的金标准。王旭等[22]对30例术前MRI诊断为三角韧带损伤的旋后外旋型踝关节骨折的病例,进行术中麻醉下外旋应力试验,并通过手术探查,发现术前MRI检查的三角韧带损伤与应力试验和术中探查结果一致,因此,MRI对于判断三角韧带是否损伤有一定价值,可以指导旋后-外旋型踝关节骨折不同程度损伤的鉴别与治疗方法的选择。国外学者Salat等[23]认为,冠状面MRI检查可以很清楚显示三角韧带的解剖结构。Alshalawi等[12]在踝关节MRI研究中发现,三角韧带浅层的撕裂通常位于韧带的远端,深层撕裂常见于韧带的近端,应用冠状面的MRI检查可以确诊深层三角韧带损伤,而三角韧带的远端撕裂或弹簧韧带损伤则需要进行MRI的矢状位检查才能发现。 也有学者认为MRI检查也存在一定的局限性。Yu 等[24]研究发现在急性三角韧带损伤合并踝关节骨折的病例中,应用MRI检查对于三角韧带损伤进行诊断会有20%的假阴性表现。Park等[25]也发现,在踝关节内侧不稳定的病例中,通常表现为损伤的三角韧带变长,而这种损伤很难通过MRI检查进行确诊,因此MRI检查诊断三角韧带损伤,特别是在慢性损伤中,敏感性为84%,而特异性为75%。 超声检查:对于评价三角韧带损伤和踝关节内侧不稳定,超声检查可以作为MRI检查的一种替代方法,特别是在急性损伤的病例中[26]。Henari等[27]研究发现,应用超声检查来辨别踝关节旋后外旋型Ⅱ度损伤与旋后外旋型Ⅳ度损伤中三角韧带的损伤情况时,准确性和完整性均为100%。在踝关节超声检查时,通过手法外翻,可以清晰的显示三角韧带的完整性。随着超声检查技术的不断发展,诊断经验的积累,超声检查在三角韧带损伤诊断的应用会越来越广泛,也会更加的精准。 关节镜检查:踝关节镜是诊断踝关节不稳定时三角韧带损伤和解剖结构异常的非常有效的诊断工具[12,28]。踝关节镜不仅可以减轻踝关节内的出血,还可以直接观察三角韧带的损伤情况[29]。在148例患者的研究中,关节镜检查发现踝关节内侧不稳定的患病率(36.5%)高于临床上推测的(25.7%)。Hintermann等[30]在对110例患者的单独研究中,通过临床查体只有5例可以确诊为踝关节内侧不稳定,而通过关节镜检查则发现23例存在踝关节内侧不稳定。这2项研究都表明,踝关节内侧不稳定性的发生率比想象的要高,在临床上可能被漏诊。Hintermann等[30]建议在进行踝关节韧带修补或重建手术前,应常规应用踝关节镜进行探查,明确MRI检查的准确性,判断三角韧带的完整性,以及除外是否存在合并损伤,如踝关节软骨损伤等。 2.3 踝关节三角韧带损伤的治疗 2.3.1 急性三角韧带损伤的治疗 保守治疗与手术治疗的争论:由于三角韧带解剖上的特殊性,手术修复难度较大,在临床上对急性三角韧带损伤的手术指征或治疗方案仍然没有统一的意见,存在很大的争论[31]。很多早期的研究结果指出,是否手术修复三角韧带损伤,对于功能预后没有差异。Warner等[32]认为踝关节内侧间隙恢复后,断裂的三角韧带可瘢痕愈合,通过保守治疗即可得到满意疗效,仅当三角韧带断端进入关节造成踝穴内软组织嵌顿,影响术中距骨复位时,才需要探查。Mak 等[33]认为外踝骨折及下胫腓联合得到解剖复位并有效固定,恢复了踝穴的正常关系,则无需手术修复三角韧带,可采用石膏固定。Sun等[34]对41例合并三角韧带损伤的B型踝关节骨折的手术治疗进行了前瞻性对照研究,三角韧带手术修复组与非手术组,在踝穴间隙、临床功能预后方面没有统计学差异,因此作者对于B型踝关节骨折不支持常规手术探查修复三角韧带。 由于踝关节三角韧带直接修复难度较大,有作者通过固定下胫腓恢复踝关节的稳定性。Jones等[35]比较了外踝骨折内固定结合下胫腓固定与外踝骨折内固定结合三角韧带修复的预后结果,两组没有统计学差异。但下胫腓螺钉不能恢复距骨在踝穴内的稳定性,在维持踝关节稳定性方面,三角韧带起着首要的作用[34]。Yu等[24]的一项多中心研究,对106例外踝骨折合并三角韧带损伤的患者,进行骨折复位内固定的同时一期修复三角韧带,平均随访27个月,临床评分满意,术后应力位片未见异常,也未出现创伤性关节炎,作者建议对于骨折内固定后仍存在踝关节内侧不稳时,应给予三角韧带的手术修复,防止出现踝关节不稳定出现的并发症。Zhao等[36]的研究发现,C型踝关节骨折中,三角韧带的手术修复可以明显减低术后踝关节内侧间隙,并降低踝关节复位不良和失败率,因此对于C型踝关节骨折建议进行三角韧带的手术修复。Woo等[37]总结了78例踝关节骨折合并三角韧带损伤手术的病例,指出三角韧带手术后可以明显的减小踝关节内侧间隙,同时强调,当合并下胫腓联合损伤时,三角韧带的手术修复是至关重要的。俞光荣等[38]提出,以下情况时应修复三角韧带:患者年青活动量大,尤其是运动员;踝关节内侧间隙大于5 mm以上;踝关节内侧肿胀和淤血较严重;CT可见踝关节内侧间隙有小骨折块;MRI示三角韧带深浅层完全断裂;踝骨折骨折固定后内侧间隙过大或不稳定。以下情况时可以考虑不处理三角韧带:老年及全身情况不好的患者;踝关节内侧肿胀和血肿不严重;术前X射线片内侧间隙较对侧仅大于1 mm;骨折复位后内侧稳定、间隙正常。 三角韧带是维持距骨在踝穴内正常位置,维持踝关节稳定性的重要结构,因此急性三角韧带损伤是否给予手术修复,取决于三角韧带的损伤是否影响到了踝关节的稳定性,如果骨折有效复位和固定后,踝关节仍不稳定,就应当给予三角韧带的一期手术修复,当然还要结合患者年龄,对运动和功能的要求,以及全身情况等综合考虑。 急性三角韧带损伤的修复:近年来,带线锚钉技术已经成为修复三角韧带应用最广泛的技术,并取得了理想的临床效果[39-40]。而且有学者研究指出,对于同时合并三角韧带损伤和下胫腓联合分离的踝关节骨折,应用带线锚钉修复三角韧带可替代下胫腓螺钉[41]。 三角韧带损伤断裂的部位通常在韧带的近端,即三角韧带内踝止点处,急性损伤通常应用缝合锚钉将三角韧带缝合固定于内踝止点。而对于三角韧带深层从距骨止点断裂的病例,同样可以应用锚钉固定于距骨的内侧面,缝合固定三角韧带。但需要注意的是,韧带缝线最终的打结固定,需要在骨折复位固定后进行,这样可以避免复位骨折时对于已缝合的三角韧带产生张力影响而导致韧带修复失败[42]。 随着踝关节关节镜技术的不断进步,应用关节镜对三角韧带损伤进行诊断和治疗越来越广泛,特别是在不合并踝关节骨折,通过影像学检查不能确定是否存在三角韧带损伤的病例中,应用关节镜可以直视下判断三角韧带的损伤程度,同时给予监视下修复,并且可以通过关节镜来判断损伤修复后踝关节的稳定性[29,43]。 2.3.2 慢性三角韧带损伤的修复与重建 对于慢性三角韧带损伤导致的慢性踝关节内侧不稳定,可以通过物理康复治疗、佩戴恢复内侧足弓的鞋垫、佩戴纠正下肢力线及维持踝关节稳定的支具和矫正器、穿戴维持后足内侧稳定性的矫形鞋等方法进行3-6个月的保守治疗,若保守治疗失败,患者仍感踝关节内侧不稳定,持续性疼痛,足踝部畸形加重,严重影响生活和工作时,应该给予手术治疗。手术的目的是重建踝关节稳定性,纠正畸形,防止踝关节反复扭伤,及降低软骨损伤的发生[12]。Stufkens等[44]及Alshalawi等[12]均建议在进行三角韧带修复或重建手术前,应进行诊断性的关节镜检查,进一步明确慢性三角韧带的诊断及损伤的程度。 带线锚钉技术不仅可以应用于急性三角韧带损伤,对于慢性三角韧带损伤,同样有效。Wang等[39]对17例应用踝关节镜确诊为慢性三角韧带损伤的病例,应用带线锚定技术对三角韧带进行了修复,取得了很满意的效果。Pellegrini等[45]首次报道了对13例慢性三角韧带功能不全的患者,应用Internal Brace加强修复三角韧带,短期随访,取得了良好的功能结果。 慢性三角韧带损伤的病例中,残留的三角韧带通常是很薄弱的,甚至是缺如的,因此此时进行三角韧带的修复手术,往往是很困难的,通常需要更加精密的重建手术,来重建踝关节的稳定,纠正足踝部的畸形[14]。很多学者应用自体肌腱(如踇长屈肌腱、腓骨长肌腱、腘肌腱等)进行三角韧带的重建,均取得了较好的重建效果[18],然而自体肌腱移植对患者手术创伤相对较大,而且取腱部位肌力会受到影响,可能会影响远期的临床效果。 近年来,很多国外学者尝试应用异体肌腱进行三角韧带的重建。Jung等[46]介绍了应用异体半腱肌重建浅层三角韧带(胫舟韧带及胫跟韧带)的新方法,并认为此方法有效而且简便易行、损伤小,见图3。Oburu与Myerson[14]应用Y型的异体腘肌腱重建深层及浅层三角韧带,同时在异体肌腱表面应用纤维束带或不可吸收纤维线编织缝合,防止异体肌腱远期的张力减退,增加踝关节长期的稳定性,降低了踝关节炎的发生,见图4。 比较三角肌韧带修复手术与重建手术的优劣,还需要大量临床病历资料的积累和总结。当慢性三角韧带损伤通过保守治疗失败,并且不可能直接修复三角韧带时,使用自体肌腱移植或同种异体肌腱移植重建通常可作为最后的保留手段。 "
| [1] Waterman BR, Belmont PJ Jr, Cameron KL, et al. Risk factors for syndesmotic and medial ankle sprain: role of sex, sport, and level of competition. Am J Sports Med. 2011;39(5): 992-998.[2] Yammine K.The morphology and prevalence of the deltoid complex ligament of the Ankle. Foot Ankle Spec. 2017;10(1): 55-62.[3] Cromeens BP, Kirchhoff CA, Patterson RM, et al. An attachment-based description of the medial collateral and spring ligament complexes. Foot Ankle Int. 2015;36: 710-721. [4] Lee S, Lin J, Hamid KS, et al. Deltoid ligament rupture in ankle fracture: diagnosis and management. J Am Acad Orthop Surg. 2018. doi: 10.5435/JAAOS-D-18-00198.[5] Boss AP, Hintermann B. Anatomical study of the medial ankle ligament complex. Foot Ankle Int. 2002;23(6): 547-553. [6] Panchani P, Chappell T, Moore G, et al. Anatomic study of the deltoid ligament of the ankle. Foot Ankle Int. 2014; 35(9):916-921.[7] Campbell K, Michalski M, Wilson K, et al. The ligament anatomy of the deltoid complex of the ankle: a qualitative and quantitative anatomical study. J Bone Joint Surg Am. 2014;96(8):e62. [8] Lee T, Jang K, Choi G, et al. The contribution of anterior deltoid ligament to ankle stability in isolated lateral malleolar fractures. Injury 2016;47(7):1581-1585.[9] 高武长,王英振.切开复位内固定踝关节骨折:联合带线锚钉修复三角韧带损伤的意义[J].中国组织工程研究, 2016,20(9): 1255-1260. [10] 张明珠,俞光荣,赵有光,等.踝关节骨折合并三角韧带完全断裂的手术治疗-1项多中心研究报告[J].足踝外科电子杂志,2014, 1(1):26-29. [11] Fernandez I, Gerzina C, Thabet AM, et al. Adding deltoid ligament repair in ankle fracture treatment: is it necessary? A systematic review. Foot Ankle Surg. 2018. doi: 10.1016/j.fas.2018.11.001. [12] Alshalawi S, Galhoum AE, Alrashidi Y, et al. Medial ankle instability: the deltoid dilemma. Foot Ankle Clin. 2018;23(4): 639-657. [13] 俞光荣,杨云峰,张凯,等.距下关节、踝关节对后足运动影响的实验研究[J].中华骨科杂志,2005,25(4):236-239.[14] Oburu E, Myerson MS. Deltoid ligament repair in flatfoot deformity. Foot Ankle Clin. 2017;22(3):503-514. [15] Lotscher P, Lang T, Zwicky L, et al. Osteoligamentous injuries of the medial ankle joint. Eur J Trauma Emerg Surg 2015;41(6):615-621.[16] Femino JE, Vaseenon T, Phisitkul P, et al. Varus external rotation stress test for radiographic detection of deep deltoid ligament disruption with and without syndesmotic disruption: a cadaveric study. Foot Ankle Int. 2013;34(2):251-260.[17] Hastie G, Akhtar S, Butt U, et al. Weightbearing radiograph facilitate functional treatment of ankle fractures of uncertain stability. J Foot Ankle Surg 2015;54(6):1042-1066.[18] Knupp M, Lang TH, Zwicky L, et al. Chronic ankle instability (medial and lateral). Clin Sports Med. 2015;34:679-688.[19] Ashraf A, Murphree J, Wait E, et al. Gravity stress radiographs and the effect of ankle position on deltoid ligament integrity and medial clear space measurements. J Orthop Trauma. 2017;31(5):270-274. [20] LeBa T, Gugala Z, Morris R, et al. Gravity versus manual external rotation stress view in evaluating ankle stability: a prospective study. Foot Ankle Spec. 2015;8(3):175-179.[21] Schottel PC, Fabricant PD, Berkes MB, et al. Manual stress ankle radiography has poor ability to predict deep deltoid ligament integrity in a supination external rotation fracture cohort. J Foot Ankle Surg. 2015; 54:531-535. [22] 王旭,张超,尹建文,等.MRI与术中外旋应力试验在旋后-外旋踝关节骨折中的应用价值比较[J].中国骨与关节外科,2014, 7(4):276-279. [23] Salat P, Le V, Veljkovic A, et al. Imaging in foot and ankle instability. Foot Ankle Clin. 2018;23(4):499-522. [24] Yu GR, Zhang MZ, Aiyer A, et al. Repair of the acute deltoid ligament complex rupture associated with ankle fractures: a multicenter clinical study. J Foot Ankle Surg. 2015;54(2): 198-202.[25] Park HJ, Cha SD, Kim S, et al. Accuracy of MRI findings in chronic lateral ankle ligament injury: comparison with surgical findings. Clin Radiol 2012;67(4):313-318. [26] Morvan G, Busson J, Wybier M, et al. Ultrasound of the ankle. Eur J Ultrasound 2001;14(1):73-82. [27] Henari S, Banks LN, Radovanovic I, et al.Ultrasonography as a diagnostic tool in assessing deltoid ligament injury in supination external rotation fractures of the ankle. Orthopedics. 2011;34(10):639-643.[28] Hintermann B, Boss A, Shafer D.Arthroscopic findings in patients with chronic ankle instability. Am J Sports Med. 2002;30(3):402-409.[29] Schairer W, Nwachukwu B, Dare DM, et al. Arthroscopically assisted open reduction-internal fixation of ankle fractures: significance of the arthroscopic ankle drive-through sign. Arthrosc Tech 2016;5(2):e407-e412.[30] Hintermann B, Scha ?fer D. Arthroscopic assessment of the chronic unstable ankle joint. Knee Surg Sports Traumatol Arthrosc 1996;4(1):48-52.[31] Dabash S, Elabd A, Potter E, et al. Adding deltoid ligament repair in ankle fracture treatment: is it necessary? A systematic review. Foot Ankle Surg. 2018. doi: 10.1016/j.fas.2018.11.001.[32] Warner SJ, Garner MR, Hinds RM, et al. Correlation between the Lauge-Hansen classification and ligament injuries in ankle fractures. J Orthop Trauma. 2015;29(12): 547-548. [33] Mak MF, Gartner L, Pearce CJ. Management of syndesmosis injuries in the elite athlete. Foot Ankle Clin. 2013;18(2):195-214.[34] Sun X, Li T, Sun Z, et al. Does routinely repairing deltoid ligament injuries in type B ankle joint fractures influence long term outcomes? Injury. 2018;49(12):2312-2317. [35] Jones CR, Nunley JN. Deltoid ligament repair versus syndesmotic ?xation in bimalleolar equivalent ankle fractures. J Orthop Trauma 2015;29(5):245-249. [36] Zhao HM, Lu J, Zhang F, et al. Surgical treatment of ankle fracture with or without deltoid ligament repair: a comparative study. BMC Musculoskelet Disord. 2017; 18(1):543. [37] Woo SH, Bae SY, Chung HJ. Short-term results of a ruptured deltoid ligament repair during an acute ankle fracture fixation. Foot Ankle Int 2018;39:35-45. [38] 俞光荣,洪浩.踝关节损伤的治疗进展与思考[J].中国骨伤,2016, 29(12):1071-1073. [39] Wang X, Ma X, Zhang C, et al. Treatment of chronic deltoid ligament injury using suture anchors. Orthop Surg. 2014;6: 223-228.[40] Hsu AR, Lareau CR, Anderson RB. Repair of acute super?cial deltoid complex avulsion during ankle fracture ?xation in national football league players. Foot Ankle Int. 2015;36:1272-1278.[41] 高怡加,黄枫,劳永生,等.锚钉修复三角韧带后踝关节的稳定性[J].中国组织工程研究,2017,21(19):3011-3016.[42] Wang X, Zhang C, Yin J, et al. Treatment of medial malleolus or pure deltoid lig- ament injury in patients with supination-external rotation type IV ankle fractures. Orthop Surg. 2017;9(1):42-48. [43] Kusnezov N, Eisenstein E, Diab N, et al. Medial malleolar fractures and associated deltoid ligament disruptions: current management controversies. Orthopedics. 2017; 40(2):e216-e222. [44] Stufkens SA, van den Bekerom MP, Knupp M, et al. The diagnosis and treatment of deltoid ligament lesions in supination-external rotation ankle fractures: a review. Strategies Trauma Lim Reconstr. 2012;7:73-85. [45] Pellegrini MJ, Torres N, Cuchacovich NR, et al. Chronic deltoid ligament insufficiency repair with Internal Brace augmentation. Foot Ankle Surg. 2018. doi: 10.1016/j.fas.2018.10.004.[46] Jung HG, Park JT, Eom JS, et al. Reconstruction of superficial deltoid ligaments with allograft tendons in medial ankle instability: a technical report. Injury. 2016;47(3): 780-783. |
| [1] | Yi Meizhi, Luo Guanghua, Xiao Yawen, Hu Rong, Chen Xiaolong, Zhao Heng. MRI findings of anatomical variations of the talus [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3888-3893. |
| [2] | Wang Lei, Qi Rong, Li Jia, Qiu Zhixue, Wang Kai, Suo Nanangxiu. Minimally invasive percutaneous plate osteosynthesis and elastic nail system in the treatment of distal tibiofibular fracture in adults [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1864-1868. |
| [3] | Bao Chunyu, Yan Mingming. Biomechanical characteristics of ankle joint in volleyball players during stop-jump [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 662-666. |
| [4] | Weng Shiyang, Wu Kai, Lin Jian, Huang Yinjun, Wang Qiugen, Huang Jianhua. Double-strand suture anchor in the treatment of tibiofibular syndesmosis injury [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5332-5337. |
| [5] | Fan Zhirong, Peng Jiajie, Zhong Degui, Zhou Lin, Su Haitao, Huang Yongquan, Wu Jianglin, Liang Yihao. Suture anchor combined with open reduction and internal fixation versus open reduction and internal fixation for ankle fracture combined with deltoid ligament injury: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1307-1312. |
| [6] | Luo Jian, Wang Lihua, Wang Tao, Wen Hui. Changes of stress and displacement of three-dimensional finite element model of ankle joint using different material assignment methods [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(18): 2822-2826. |
| [7] | Sun Chenguang1, Wang Chun2. Muscle activation characteristics during two balance tests in patients with functional ankle instability [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(15): 2320-2326. |
| [8] | Qiu Peng1, Cheng Yongzhong1, Liu Guangwei2, He Da1, Zhu Jianfei1, Cheng Hao1, Wen Jianmin1, Wu Liyan1 . Establishment of the model of pronation-external rotation trimalleolar fracture after closed osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(36): 5828-5832. |
| [9] | Huang Dawu1, Liu Lu2, Zhu Xing1, Wang Xinbao1, Chen Yueliang3 . Characteristics of isokinetic muscle strength of lower limb joints in elite female short track speed skaters [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(36): 5803-5810. |
| [10] | Xie Qiang, Wang Zhi-hui, Liu Wen-yi, Gao Yun-feng, Xue Xin-xin. Mechanical stability after plating ankle arthrodesis based on three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(3): 392-397. |
| [11] | Chai Hao, Wu Ting, Shu Li, Zhang Lei. Screw fixation versus plate fixation for posterior malleolus fracture: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(27): 4423-4428. |
| [12] | Song Fa-ming, Wang Chun. Biomechanical characteristics of the patients with functional ankle instability when landing on the slope [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(27): 4380-4386. |
| [13] | Guo Yong-liang, Feng Chong-rui, Zhang Xin-fei . Reliability of BTS three-dimensional motion capture system in gait analysis [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(23): 3665-3669. |
| [14] | Huang Dan, He Xiu-zhen, Yang Xu-huan, Peng Si-min, Wu Ying-xian. Stratification of injuries to the lateral collateral ligament of the ankle using ultrasound: protocol of a prospective, single-center, diagnostic trial and preliminary results [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(23): 3681-3686. |
| [15] | Shi Yu, Liao Yong-hua, Luo Jiong. Biomechanical analysis of human balance and buffer capacity of ankle joint when dropping from height after taping [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(19): 3014-3020. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||