Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (3): 356-361.doi: 10.3969/j.issn.2095-4344.0030
Previous Articles Next Articles
Efficacy of intravenous versus topical administration of tranexanmic acid in primary total knee arthroplasty
Hu Wen-hao
- Department of Orthopedics, the Affiliated Huai’an First People’s Hospital, Nanjing Medical University, Huai’an 223300, Jiangsu Province, China
-
Online:2018-01-28Published:2018-01-28 -
About author:Hu Wen-hao, Master, Department of Orthopedics, the Affiliated Huai’an First People’s Hospital, Nanjing Medical University, Huai’an 223300, Jiangsu Province, China -
Supported by:the Project of Nanjing Medical University, No. 2016NJMU142
CLC Number:
Cite this article
Hu Wen-hao. Efficacy of intravenous versus topical administration of tranexanmic acid in primary total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(3): 356-361.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
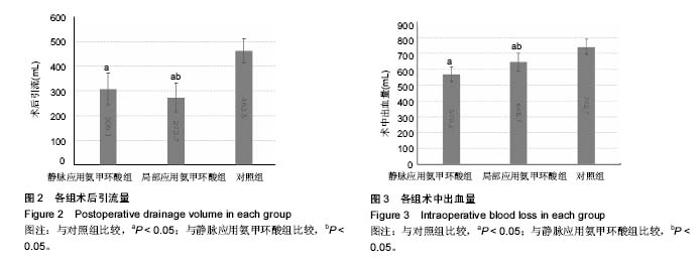
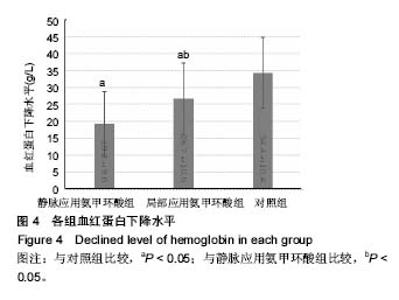
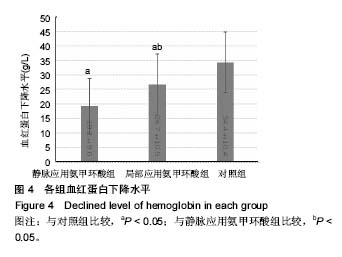
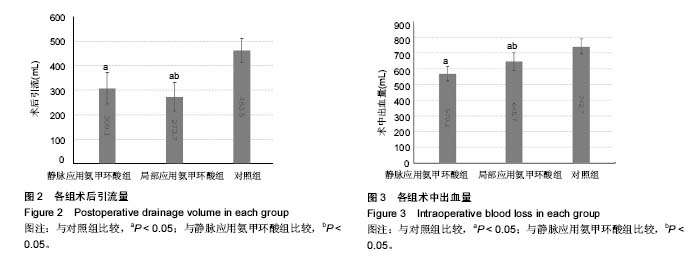
2.2 失血量对比 通过对比发现,静脉应用氨甲环酸组、局部应用氨甲环酸组与对照组相比,应用氨甲环酸2组的术中失血量及术后引流量有明显降低,通过引流管在关节腔内局部应用氨甲环酸,术后引流量减少了约189.8 mL;静脉应用氨甲环酸组的术后引流量减少了约154.4 mL,差异有显著性意义(P < 0.05)。在2个应用氨甲环酸组中,局部应用氨甲环酸相对于静脉应用,术后引流量可以减少 35.4 mL,差异有显著性意义(P < 0.05);而静脉应用氨甲环酸组的总失血量(术中失血量+术后引流量)低于局部应用氨甲环酸组,差异有显著性意义(P < 0.05),见图2,3。 2.3 血红蛋白水平对比 与术前血红蛋白水平相比,静脉应用氨甲环酸组、局部应用氨甲环酸组与对照组的术后血红蛋白分别下降(19.2±9.6)g/L,(26.7±10.5)g/L,(34.4± 10.4)g/L。在2个应用氨甲环酸组中,血红蛋白的下降水平均明显低于对照组(P < 0.05);静脉应用氨甲环酸组血红蛋白的下降水平明显低于局部应用氨甲环酸组(P < 0.05),见图4。 2.4 术后并发症 各组患者术后伤口及关节无明显红肿,14 d拆线时手术切口愈合良好。术后所有患者出院前膝关节功能达到伸直0°,屈曲≥90°。术后第14天行双下肢动静脉血管B超检查,均未发现静脉血栓形成。所有患者均未出现肺栓塞表现,未行胸部CT扫描。 "
| [1] Panteli M, Papakostidis C, Dahabreh Z, et al. Topical tranexamic acid in total knee replacement: a systematic review and meta-analysis. Knee. 2013;20(5):300.[2] Spahn DR, Casutt M. Eliminating blood transfusions: new aspects and perspectives. Anesthesiology. 2000;93(1): 242-255.[3] Dunn CJ, Goa KL. Tranexamic acid: a review of its use in surgery and other indications. Drugs. 1999,57(6): 1005-1032. [4] Soliman R, Yousef H, Alghadam F, et al. Prospective, Randomized, comparative study between aprotinin and tranexamic acid in cardiac surgery. J Anesthes Clin Res. 2013;2(1):201-205.[5] Calamari D, Zuccato E, Castiglioni S, et al. Strategic survey of therapeutic drugs in the Rivers Po And Lambro in northern Italy. Env Scie Technol. 2015;37(7):1241-1248.[6] Sanz-Reig J, Parra RB, Ferrández MJ, et al. Single intravenous tranexamic acid dose to reduce blood loss in primary total knee replacement. Rev Esp Cir Ortop Traumatol. 2016;60(2):106-112. [7] Chen JY, Chin PL, Moo IH, et al. Intravenous versus intra-articular tranexamic acid in total knee arthroplasty: A double-blinded randomised controlled noninferiority trial. Knee. 2016;23(1):152-156. [8] Gillette BP, Desimone LJ, Trousdale RT, et al. Low risk of thromboembolic complications with tranexamic acid after primary total hip and knee arthroplasty. Clin Orthop Relat Res. 2013;471(1):150-154.[9] Hynes M, Calder P, Scott G. The use of tranexamic acid to reduce blood loss during total knee arthroplasty. Knee. 2003; 10(4):375-377.[10] Kagoma YK, Crowther MA, Douketis J, et al. Use of antifibrinolytic therapy to reduce transfusion in patients undergoing orthopedic surgery: a systematic review of randomized trials. Thromb Res. 2009;123(5):687.[11] Madsen RV, Nielsen CS, Kallemose T, et al. Low risk of thromboembolic events after routine administration of tranexamic acid in hip and knee arthroplasty. J Arthroplasty. 2017;32(4):1298-1303. [12] Zhu M, Chen JY, Yew AK, et al. Intra-articular tranexamic acid wash during bilateral total knee arthroplasty. J Orthop Surg (Hong Kong). 2015;23(3):290-293. [13] May JH, Rieser GR, Williams CG, et al. The assessment of blood loss during total knee arthroplasty when comparing intravenous vs intracapsular administration of tranexamic acid. J Arthroplasty. 2016;31(11):2452-2457.[14] Sun Q, Yu X, Nie X, et al. The efficacy comparison of tranexamic acid for reducing blood loss in total knee arthroplasty at different dosage time. J Arthroplasty. 2017; 32(1):33-36. [15] Shin YS, Yoon JR, Lee HN, et al. Intravenous versus topical tranexamic acid administration in primary total knee arthroplasty: a meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2016;23(105):1-11.[16] Sadigursky D, Andion D, Boureau P, et al. Effect of tranexamic acid on bleeding control in total knee arthroplasty. Acta Ortop Bras. 2016;24(3):131-136. [17] Digas G, Koutsogiannis I, Meletiadis G, et al. Intra-articular injection of tranexamic acid reduce blood loss in cemented total knee arthroplasty. Eur J Orthop Surg Traumatol. 2015; 25(7):1181-1188.[18] Vijay BS, Vikram B, Subhro M, et al. Role of tranexamic acid in reducing postoperative blood loss and transfusion requirement in patients undergoing hip and femoral surgeries. Saudi J Anaesth. 2013;7(1):29-32.[19] Rasouli MR, Parvizi J. Tranexamic Acid in total joint arthroplasty: efficacy and safety. Arch Bone Joint Surg. 2015; 3(1):1.[20] Aglietti P, Baldini A, Vena LM, et al. Effect of tourniquet use on activation of coagulation in total knee replacement. Clin Orthop Relat Res. 2000;371(371):169.[21] Darina DCL, Pablo MH, Flores YN, et al. Influence of mealtime habits on the risk of weight gain and obesity in Mexican adults. Public Health Nutr. 2016;20(2):220-232.[22] Wong J, Abrishami A, El BH, et al. Topical application of tranexamic acid reduces postoperative blood loss in total knee arthroplasty: a randomized, controlled trial. J Bone Joint Surg Am. 2010;92(15):2503.[23] Hirotaka M, Kotaro I. Intra-articular injection of tranexamic acid via a drain plus drain-clamping to reduce blood loss in cementless total knee arthroplasty. J Orthop Surg Res. 2012; 7(1):1-6.[24] Irwin A, Khan SK, Jameson SS, et al. Oral versus intravenous tranexamic acid in enhanced-recovery primary total hip and knee replacement: results of 3000 procedures. Bone Joint J. 2013;95-B(11):1556.[25] Pongcharoen B, Ruetiwarangkoon C. Does tranexamic acid reduce blood loss and transfusion rates in unicompartmental knee arthroplasty. J Orthop Sci. 2016;21(2):211-215. [26] Valentine SL, Randolph AG. Weaning children from mechanical ventilator support// Pediatric and neonatal mechanical ventilation. Springer Berlin Heidelberg, 2015.[27] Alipour M, Tabari M, Keramati M, et al. Effectiveness of oral Tranexamic acid administration on blood loss after knee artroplasty: a randomized clinical trial. Transfus Apher Sci. 2013;49(3):574-577.[28] Zohar E, Ellis M, Ifrach N, et al. The postoperative blood-sparing efficacy of oral versus intravenous tranexamic acid after total knee replacement. Anesthesia Analgesia. 2004;99(6):1679-1683.[29] Rosenstein AD, Michelov YA, Thompson S, et al. Benefits of limited use of a tourniquet combined with intravenous tranexamic acid during total knee arthroplasty. Ochsner J. 2016;16(4):443-449. [30] Lin PC, Hsu CH, Chen WS, et al. Does tranexamic acid save blood in minimally invasive total knee arthroplasty? Clini Orthop Relat Res. 2011;469(7):1995-2002.[31] Good L, Peterson E, Lisander B. Tranexamic acid decreases external blood loss but not hidden blood loss in total knee replacement. Br J Anaesthesia. 2003;90(5):596.[32] Mahdi M, Ali TM, Mehdi S, et al. Low dose perioperative intravenous tranexamic acid in patients undergoing total knee arthroplasty: a double-blind randomized placebo controlled clinical trial. J Blood Transfus. 2015;2015(1):1-5.[33] Ishida K, Tsumura N, Kitagawa A, et al. Intra-articular injection of tranexamic acid reduces not only blood loss but also knee joint swelling after total knee arthroplasty. Int Orthop. 2011; 35(11):1639-1645.[34] Loš?ák J, Gallo J, Špi?ka J, et al. Intra-articular application of tranexamic acid significantly reduces blood loss and transfusion requirement in primary total knee arthroplasty. Acta Chir Orthop Traumatol Cech. 2016;83(4):254-262.[35] Pinsornsak P, Rojanavijitkul S, Chumchuen S. Peri-articular tranexamic acid injection in total knee arthroplasty: a randomized controlled trial. BMC Musculoskelet Disord.2016; 17(32):313. [36] Danninger T, Rasul R, Poeran J, et al. Blood transfusions in total hip and knee arthroplasty: an analysis of outcomes. Thescient World J. 2014; 2014(2):623460.[37] Wong J, Abrishami A, El BH, et al. Topical application of tranexamic acid reduces postoperative blood loss in total knee arthroplasty: a randomized, controlled trial. J Bone Joint Surg Am. 2010;92(15):2503-2513. [38] DiBlasi JF, Smith RP, Garavaglia J, et al. Comparing cost, efficacy, and safety of intravenous and topical tranexamic acid in total hip and knee arthroplasty. Am J Orthop (Belle Mead NJ). 2016;45(7):E439-439E443. [39] Shang J, Wang H, Zheng B, et al. Combined intravenous and topical tranexamic acid versus intravenous use alone in primary total knee and hip arthroplasty: A meta-analysis of randomized controlled trials. Int J Surg. 2016;36(Pt A): 324-329.[40] Delanois RE, Gwam C, Mistry JB, et al. Intraarticular administration of tranexamic acid is safe and effective in total knee arthroplasty patients at high-risk for thromboembolism. Surg Technol Int. 2016;30(205):279-283. [41] Fu Y, Shi Z, Han B, et al. Comparing efficacy and safety of 2 methods of tranexamic acid administration in reducing blood loss following total knee arthroplasty: A meta-analysis. Medicine (Baltimore). 2016;95(50):e5583.[42] He P, Zhang Z, Li Y, et al. Efficacy and safety of tranexamic acid in bilateral total knee replacement: a meta-analysis and systematic review. Med Sci Monit. 2015;21(30):3634-3642. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [3] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [4] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [5] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [6] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [7] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [8] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [9] | Yuan Jiawei, Zhang Haitao, Jie Ke, Cao Houran, Zeng Yirong. Underlying targets and mechanism of Taohong Siwu Decoction in prosthetic joint infection on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1428-1433. |
| [10] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [11] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [12] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [13] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [14] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [15] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||