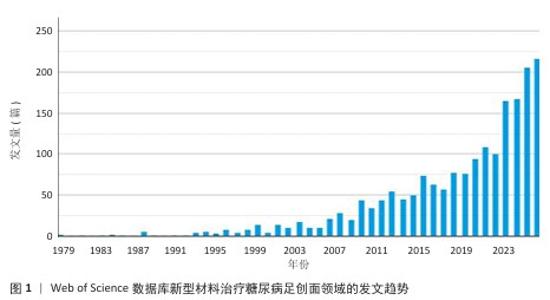
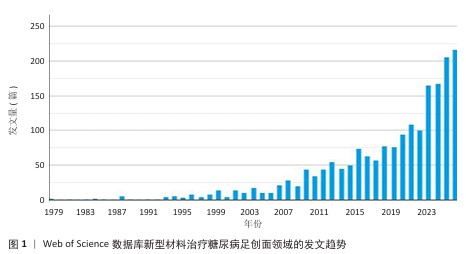
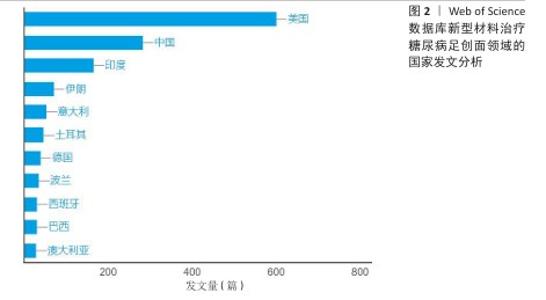
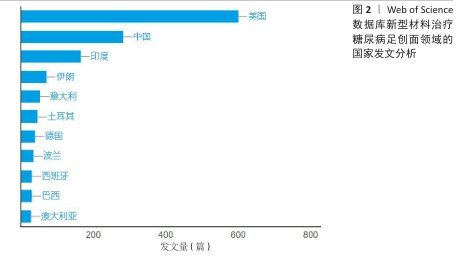
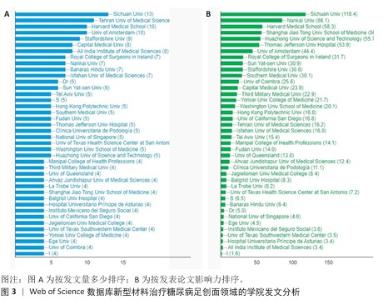
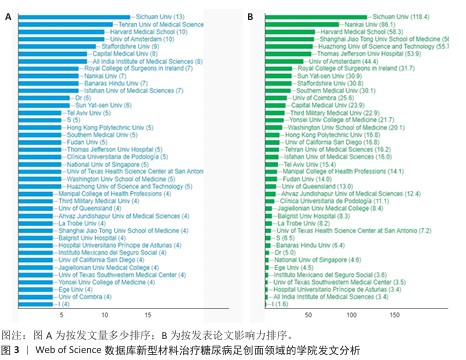
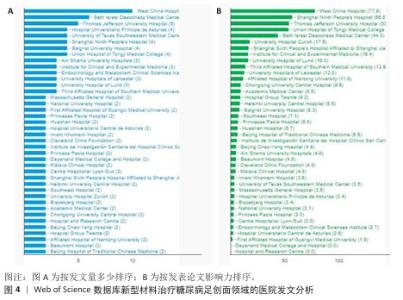
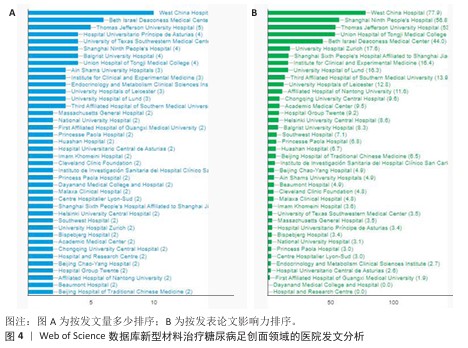
[1] MOURA LI, DIAS AM, CARVALHO E, et al.Recent advances on the development of wound dressings for diabetic foot ulcer treatment--a review. Acta Biomater. 2013;9(7):7093-114.
[2] MARIADOSS AVA, SIVAKUMAR AS, LEE CH, et al. Diabetes mellitus and diabetic foot ulcer: Etiology, biochemical and molecular based treatment strategies via gene and nanotherapy. Biomed Pharmacother. 2022;151:113134.
[3] YANG J, CHEN Z, PAN D, et al. Umbilical Cord-Derived Mesenchymal Stem Cell-Derived Exosomes Combined Pluronic F127 Hydrogel Promote Chronic Diabetic Wound Healing and Complete Skin Regeneration. Int J Nanomedicine. 2020;15:5911-5926.
[4] LIU Z, BIAN X, LUO L, et al. Spatiotemporal single-cell roadmap of human skin wound healing.Cell Stem Cell. 2025;32(3):479-498.e8.
[5] CULLEN B, SMITH R, MCCULLOCH E, et al. Mechanism of action of PROMOGRAN, a protease modulating matrix, for the treatment of diabetic foot ulcers. Wound Repair Regen. 2002;10(1): 16-25.
[6] RÖMLING U, KJELLEBERG S, NORMARK S, et al. Microbial biofilm formation: a need to act. J Intern Med. 2014;276(2):98-110.
[7] SINGHAL L, SINGH KA, PANDA RK, et al. VG111: A novel formulation demonstrating clinical evidence of anti-pathogenic activity and accelerated wound healing in humans and companion animals. J Lab Physicians. 2024;16:347-357.
[8] HUANG F, LU X, YANG Y, et al. Microenvironment-Based Diabetic Foot Ulcer Nanomedicine. Adv Sci (Weinh). 2023;10(2):e2203308.
[9] FENG H, HUANG W, ZHOU Q, et al. Efficacy and safety of Resina Draconis for wound repair in the treatment of diabetic foot ulcer: A systematic review and meta-analysis of randomized controlled trials. Complement Ther Clin Pract. 2023;50:101707.
[10] LIU E, HU X, ZHANG W, et al. Efficacy and safety of ultrasound-assisted wound debridement in the treatment of diabetic foot ulcers: a systematic review and meta-analysis of 11 randomized controlled trials. Front Endocrinol (Lausanne). 2024;15:1393251.
[11] CHEN Y, WANG X, TAO S, et al. Research advances in smart responsive-hydrogel dressings with potential clinical diabetic wound healing properties. Mil Med Res. 2023;10(1):37.
[12] ZHOU Z, DENG T, TAO M, et al. Snail-inspired AFG/GelMA hydrogel accelerates diabetic wound healing via inflammatory cytokines suppression and macrophage polarization. Biomaterials. 2023;299:122141.
[13] TOLEUTAYEV T, DYUSSUPOV A, IMANBAEV M, et al.
Modern methods of surgical treatment of diabetic foot syndrome. Georgian Med News. 2024;(357):6-10.
[14] LEI FR, SHEN XF, ZHANG C, et al. Clinical efficacy of endovascular revascularization combined with vacuum-assisted closure for the treatment of diabetic foot. World J Diabetes. 2024;15(7): 1499-1508.
[15] ZHOU X, KANG C, HU Y, et al. Study on insulin resistance and ischemic cerebrovascular disease: A bibliometric analysis via CiteSpace. Front Public Health. 2023;11:1021378.
[16] ALBERTS A, BRATU AG, NICULESCU AG, et al. New Perspectives of Hydrogels in Chronic Wound Management.Molecules. 2025;30(3):686.
[17] ARABPOUR Z, ABEDI F, SALEHI M, et al. Hydrogel-Based Skin Regeneration. Int J Mol Sci. 2024;25(4):1982.
[18] TANG L, XIE S, WANG D, et al. Astragalus polysaccharide/carboxymethyl chitosan/sodium alginate based electroconductive hydrogels for diabetic wound healing and muscle function assessment.Carbohydr Polym. 2025;350:123058.
[19] CHHILLAR A, JAISWAL A. Hyaluronic Acid-Based Self-Healing Hydrogels for Diabetic Wound Healing. Adv Healthc Mater. 2025;14(4):e2404255.
[20] BAIER LEACH J, BIVENS KA, PATRICK CW JR, et al.
Photocrosslinked hyaluronic acid hydrogels: natural, biodegradable tissue engineering scaffolds. Biotechnol Bioeng. 2003;82(5):578-589.
[21] XIAO S, ZHAO T, WANG J, et al. Gelatin Methacrylate (GelMA)-Based Hydrogels for Cell Transplantation: an Effective Strategy for Tissue Engineering. Stem Cell Rev Rep. 2019;15(5): 664-679.
[22] PAN G, LI M, MU L, et al. Photothermal/Photodynamic Synergistic Antibacterial Hydrogel Dressing with pH/Glucose Dual Responsive Pirfenidone Release for Diabetic Foot Ulcers. Adv Funct Mater. 2025;35(9):2416205.
[23] QU J, ZHAO X, LIANG Y, et al. Degradable conductive injectable hydrogels as novel antibacterial, anti-oxidant wound dressings for wound healing. Chem Eng J. 2019;362:548-560.
[24] QI XL, SHI YZ, ZHANG CF, et al. A Hybrid Hydrogel with Intrinsic Immunomodulatory Functionality for Treating Multidrug-Resistant Pseudomonas aeruginosa Infected Diabetic Foot Ulcers. ACS Mater Lett. 2024;6(7):2533-2547.
[25] SÁNCHEZ ML, VALDEZ H, CONDE M, et al. Polymers and Bioactive Compounds with a Macrophage Modulation Effect for the Rational Design of Hydrogels for Skin Regeneration. Pharmaceutics. 2023;15(6):1655.
[26] WANG S, ZHANG J, ZHOU W, et al. Injectable carrier hydrogel for diabetic foot ulcer wound repair. J Mater Sci. 2023;58:11441-11468.
[27] METCALFE AD, FERGUSON MW. Tissue engineering of replacement skin: the crossroads of biomaterials, wound healing, embryonic development, stem cells and regeneration. J R Soc Interface. 2007;4(14):413-437.
[28] CHENG F, SONG DY, LI HB, et al. Recent Progress in Biomedical Scaffold Fabricated via Electrospinning: Design, Fabrication and Tissue Engineering Application. Adv Funct Mater. 2025; 35(1):2406950.
[29] YUE Y, LIU X, PANG L, et al. Astragalus Polysaccharides/PVA Nanofiber Membranes Containing Astragaloside IV-Loaded Liposomes and Their Potential Use for Wound Healing. Evid Based Complement Alternat Med. 2022;2022:9716271.
[30] ZHANG L, YANG G, JOHNSON BN, et al. Three-dimensional (3D) printed scaffold and material selection for bone repair. Acta Biomater. 2019; 84:16-33.
[31] BAI Y, WANG Z, HE X, et al. Application of Bioactive Materials for Osteogenic Function in Bone Tissue Engineering. Small Methods. 2024;8(8):e2301283.
[32] HAIJIE C, LEI W, KAI W, et al. Fish collagen sponge with human umbilical cord mesenchymal stem cells for diabetic wound repair in rats. J Cell Physiol. 2025;240(1):e31471.
[33] TSAI HW, WANG PH, TSUI KH. Mesenchymal stem cell in wound healing and regeneration. J Chin Med Assoc. 2018;81(3):223-224.
[34] MARTINA M, HUTMACHER DW. Biodegradable polymers applied in tissue engineering research: a review. Polymer International. 2007;56(2): 145-157.
[35] VIJAYAKUMAR V, SAMAL SK, MOHANTY S, et al. Recent advancements in biopolymer and metal nanoparticle-based materials in diabetic wound healing management. Int J Biol Macromol. 2019; 122:137-148.
[36] AMINZAI MT, PATAN A. Recent Applications and Evaluation of Metal Nanoparticle–Polymer Hybrids as Chronic Wound Dressings. J Nanomater. 2024. doi: 10.1155/2024/3280349.
[37] WANG L, YANG Y, HAN W, et al. Novel design and development of Centella Asiatica extract - loaded poloxamer/ZnO nanocomposite wound closure material to improve anti-bacterial action and enhanced wound healing efficacy in diabetic foot ulcer. Regen Ther. 2024;27:92-103.
[38] WEI T, PAN T, PENG X, et al. Janus liposozyme for the modulation of redox and immune homeostasis in infected diabetic wounds. Nat Nanotechnol. 2024;19(8):1178-1189.
[39] TANG L, XIE S, WANG D, et al. Astragalus polysaccharide/carboxymethyl chitosan/sodium alginate based electroconductive hydrogels for diabetic wound healing and muscle function assessment. Carbohydr Polym. 2025;350:123058.
[40] ZHU ZQ, WANG L, PENG YO, et al. Continuous Self-Oxygenated Double-Layered Hydrogel under Natural Light for Real-Time Infection Monitoring, Enhanced Photodynamic Therapy, and Hypoxia Relief in Refractory Diabetic Wounds Healing. Adv Funct Mater. 2022;32(32):2201875.
[41] KONDEJ K, ZAWRZYKRAJ M, CZERWIEC K, et al.
Bioengineering Skin Substitutes for Wound Management-Perspectives and Challenges. Int J Mol Sci. 2024;25(7):3702.
[42] LI Z, SONG P, LI G, et al. AI energized hydrogel design, optimization and application in biomedicine. Mater Today Bio. 2024;25:101014.
[43] SZYMANSKI NJ, RENDY B, FEI Y, et al. An autonomous laboratory for the accelerated synthesis of novel materials. Nature. 2023; 624(7990):86-91.
|