Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (6): 911-916.doi: 10.12307/2023.903
Previous Articles Next Articles
Proximal femoral nail antirotation for femoral intertrochanteric fractures with lateral wall integrity and lateral wall risk
Wu Zhonghan1, 2, Wang Jingkun1, 2, Li Tao1, 2, Xu Xinzhong1, 2, Yu Shuisheng1, 2, Cheng Li1, 2, Tian Dasheng1, 2, Tang Jian1, 2 , 3, Jing Juehua1, 2
- 1Department of Orthopedics, 2Institute of Orthopedics of Research Center for Translational Medicine, Second Hospital of Anhui Medical University, Hefei 230601, Anhui Province, China; 3Department of Orthopedics, First Hospital of Anhui Medical University, Hefei 230000, Anhui Province, China
-
Received:2022-11-22Accepted:2023-01-10Online:2024-02-28Published:2023-07-12 -
Contact:Jing Juehua, MD, Professor, Chief physician, Doctoral supervisor, Department of Orthopedics, and Institute of Orthopedics of Research Center for Translational Medicine, Second Hospital of Anhui Medical University, Hefei 230601, Anhui Province, China -
About author:Wu Zhonghan, Master candidate, Department of Orthopedics, and Institute of Orthopedics of Research Center for Translational Medicine, Second Hospital of Anhui Medical University, Hefei 230601, Anhui Province, China -
Supported by:Scientific Research Foundation Program of Anhui Medical University in 2019, No. xkj2019131 (to XXZ)
CLC Number:
Cite this article
Wu Zhonghan, Wang Jingkun, Li Tao, Xu Xinzhong, Yu Shuisheng, Cheng Li, Tian Dasheng, Tang Jian, Jing Juehua. Proximal femoral nail antirotation for femoral intertrochanteric fractures with lateral wall integrity and lateral wall risk[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 911-916.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
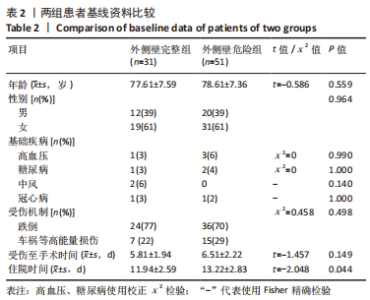
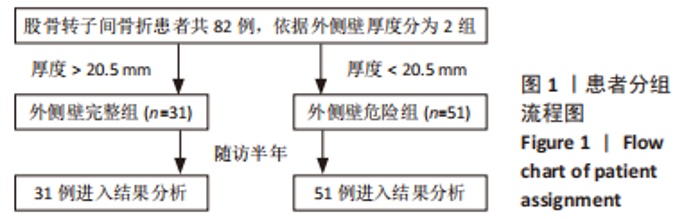
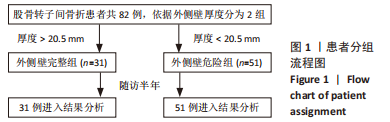
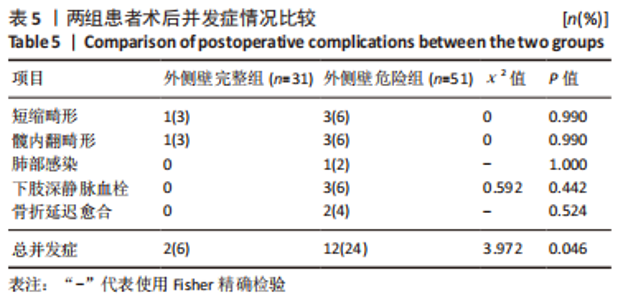
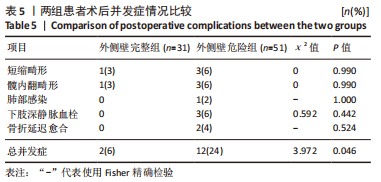
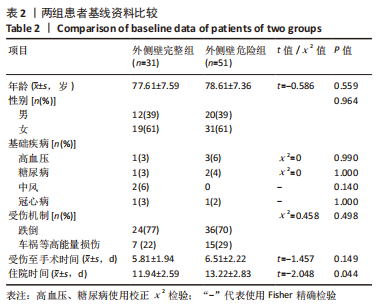
2.1 参与者数量分析 该项研究包括82例急诊入院的外侧壁非破裂型转子间骨折患者,依据术前三维CT表现将所有患者按外侧壁厚度分为2组,随访期间均无脱落,全部进入结果分析。 2.2 患者基线资料比较 两组患者在年龄、性别及受伤机制的构成比上无明显差异。受伤机制主要为跌倒,其次是车祸、高处坠落等在内的高能量损伤。两组患者的基础疾病包括高血压、糖尿病、脑卒中、冠心病等差异无显著性意义(P > 0.05)。受伤至手术时间:外侧壁完整组为(5.81±1.94) d低于外侧壁危险组(6.51±2.22) d,差异无显著性意义(P > 0.05)。术后住院天数:外侧壁危险型为(13.22±2.83) d,相较外侧壁完整型(11.94±2.59) d明显延长(P < 0.05)。患者术前详细资料见表2;患者分组流程图见图1。"
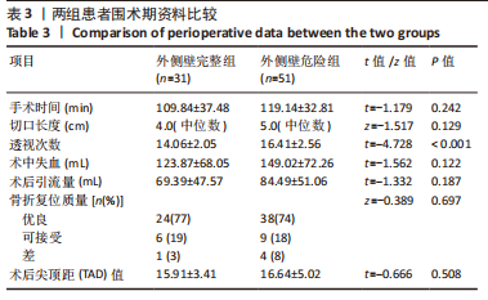
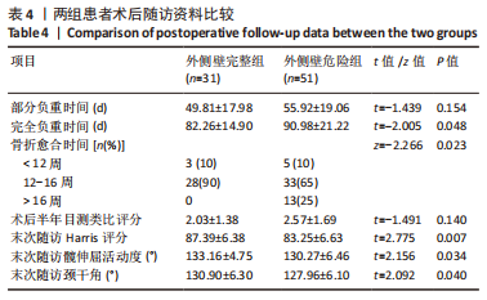
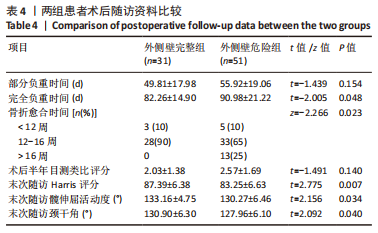
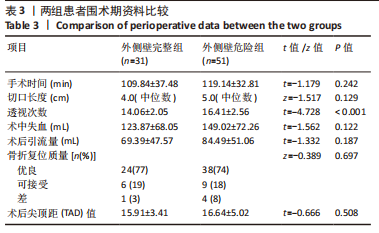
2.3 围术期指标比较 外侧壁完整组在手术时间、切口长度、术中失血以及术后引流量方面表现更好,但两组患者数据差异无显著性意义(P > 0.05)。值得注意的是,两组患者在术中透视次数上存在明显差异,外侧壁危险组(16.41±2.56)次较外侧壁完整组(14.06±2.05)次明显增多(P < 0.05),分析可能是因为医生为了避免医源性外侧壁骨折而增加了透视次数,以期使内固定位置准确而牢固。两组患者在术后拍摄的X射线正侧位片中观察到的骨折复位质量和尖顶距(tip apex distance,TAD)的数据相近(为了确保术后的骨盆平片位置及一致性,拍摄时使骶骨中线通过耻骨联合,骶髂关节左右对称),差异无显著性意义。患者未发生围术期死亡。详细资料见表3。"
| [1] PLAZA-CARMONA M, REQUENA-HERNÁNDEZ C, JIMÉNEZ-MOLA S, et al. Good practices in the recovery of ambulation in octogenarian women with hip fractures. Rev Assoc Med Bras (1992).2020;66(10):1417-1422. [2] DUNN J, KUSNEZOV N, BADER J, et al. Long versus short cephalomedullary nail for trochanteric femur fractures (OTA 31-A1, A2 and A3): a systematic review. J Orthop Traumatol. 2016;17(4):361-367. [3] ADEYEMI A, DELHOUGNE G. Incidence and Economic Burden of Intertrochanteric Fracture: A Medicare Claims Database Analysis. JB JS Open Access. 2019;4(1):e0045. [4] KLABER I, BESA P, SANDOVAL F, et al. The new AO classification system for intertrochanteric fractures allows better agreement than the original AO classification. Injury. 2021;52(1):102-105. [5] CHO JW, KENT WT, YOON YC, et al. Fracture morphology of AO/OTA 31-A trochanteric fractures: A 3D CT study with an emphasis on coronal fragments. Injury. 2017;48(2):277-284. [6] CHANG SM, HOU ZY, HU SJ, et al. Intertrochanteric Femur Fracture Treatment in Asia: What We Know and What the World Can Learn. Orthop Clin North Am. 2020;51(2):189-205. [7] GOTFRIED Y. Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation. J Bone Joint Surg Am. 2007;89(11): 2552-2553. [8] GAO Z, LV Y, ZHOU F, et al. Risk factors for implant failure after fixation of proximal femoral fractures with fracture of the lateral femoral wall. Injury. 2018;49(2):315-322. [9] HSU CE , SHIH CM , WANG CC , et al. Lateral femoral wall thickness. A reliable predictor of post-operative lateral wall fracture in intertrochanteric fractures. Bone Joint J. 2013;95-B(8):1134-1138. [10] POLAT G , AKGUL T , EKINCI M , et al. A biomechanical comparison of three fixation techniques in osteoporotic reverse oblique intertrochanteric femur fracture with fragmented lateral cortex (vol 45, pg 499, 2019). Eur J Trauma Emerg Surg. 2019;45(3):499-505. [11] 胡茂华,田纪伟,陈晓庆.外侧壁危险型股骨粗隆间骨折两种内固定比较[J].中国矫形外科杂志,2021,29(20):1838-1842. [12] KUMAR P, RAJNISH RK, SHARMA S, et al. Proximal femoral nailing is superior to hemiarthroplasty in AO/OTA A2 and A3 intertrochanteric femur fractures in the elderly: a systematic literature review and meta-analysis. Int Orthop. 2020; 44(4):623-633. [13] CHEN WH, GUO WX, GAO SH, et al. Arthroplasty vs proximal femoral nails for unstable intertrochanteric femoral fractures in elderly patients: a systematic review and metaanalysis. World J Clin Cases. 2021;9(32):9878-9888. [14] KIRIAKOPOULOS E, MCCORMICK F, NWACHUKWU BU, et al. In-hospital mortality risk of intertrochanteric hip fractures: a comprehensive review of the US Medicare database from 2005 to 2010. Musculoskelet Surg. 2017;101(3):213-218. [15] LAN H, TAN Z, LI KN, et al. Intramedullary Nail Fixation Assisted by Orthopaedic Robot Navigation for Intertrochanteric Fractures in Elderly Patients. Orthop Surg. 2019;11(2):255-262. [16] LUO X, HE S, LI Z, et al. Quantification and influencing factors of perioperative hidden blood loss during intramedullary fixation for intertrochanteric fractures in the elderly. Arch Orthop Trauma Surg. 2020;140(10):1339-1348. [17] CHO Y, LEE I, HA SH, et al. Comparison of hip subregion bone mineral density to the type of proximal femur fracture. Arch Osteoporos. 2020;15(1):122. [18] DELBAR A, PFLIMLIN A, DELABRIÈRE I, et al. Persistence with osteoporosis treatment in patients from the Lille University Hospital Fracture Liaison Service. Bone. 2021;144:115838. [19] NIU E, YANG A, HARRIS AH, et al. Which Fixation Device is Preferred for Surgical Treatment of Intertrochanteric Hip Fractures in the United States? A Survey of Orthopaedic Surgeons. Clin Orthop Relat Res. 2015;473(11):3647-3655. [20] KIM JT, KIM HH, KIM JH, et al. Mid-Term Survivals After Cementless Bipolar Hemiarthroplasty for Unstable Intertrochanteric Fractures in Elderly Patients. J Arthroplasty. 2018;33(3):777-782. [21] PARK JH, SHON HC, CHANG JS, et al. How can MRI change the treatment strategy in apparently isolated greater trochanteric fracture? Injury. 2018;49(4):824-828. [22] ELZOHAIRY MM, KHAIRY HM. Fixation of Intertrochanteric Valgus Osteotomy with T Plate in Treatment of Developmental Coxa Vara. Clin Orthop Surg. 2016; 8(3):310-315. [23] 袁加斌,朱宗东,唐孝明,等.难复性股骨转子间骨折的解剖分型与复位策略[J].中国组织工程研究,2022,26(9):1341-1345. [24] VANWAGNER MJ, PORTER SB, SPAULDING AC, et al. Intertrochanteric fracture fixation in solid organ transplant patients: outcomes and survivorship. Arch Orthop Trauma Surg. 2022;142(10):2739-2745. [25] CHA YH, YOO JI, HWANG SY, et al. Biomechanical Evaluation of Internal Fixation of Pauwels Type III Femoral Neck Fractures: A Systematic Review of Various Fixation Methods. Clin Orthop Surg. 2019;11(1):1-14. [26] 孙辉,范致远,靳颖哲,等.加压支撑螺钉与部分螺纹空心螺钉固定青壮年股骨颈骨折术后并发症的前瞻性队列研究[J].中华创伤骨科杂志,2021, 23(6):470-476. [27] HAQ RU, MANHAS V, PANKAJ A, et al. Proximal femoral nails compared with reverse distal femoral locking plates in intertrochanteric fractures with a compromised lateral wall; a randomised controlled trial. Int Orthop. 2014;38(7): 1443-1449. [28] SOCCI AR, CASEMYR NE, LESLIE MP, et al. Implant options for the treatment of intertrochanteric fractures of the hip: rationale, evidence, and recommendations. Bone Joint J. 2017;99-B(1):128-133. [29] 吴钟汉,许新忠,张积森,等.粉碎性股骨逆转子间骨折一期重建外侧壁:如何提高修复后骨生物力学稳定性[J].中国组织工程研究,2021,25(36): 5838-5843. [30] 卫禛,张凯,张世民.股骨近端外侧壁厚度的概念及研究进展[J].中国临床解剖学杂志,2020,38(6):739-742. [31] MU W, ZHOU J. PFNA-II Internal Fixation Helps Hip Joint Recovery and Improves Quality of Life of Patients with Lateral-Wall Dangerous Type of Intertrochanteric Fracture. Biomed Res Int. 2021;2021:5911868. [32] SONG H, CHEN SY, CHANG SM. What should be filled in the blank of 31A2.1 in AO/OTA-2018 classification. Injury. 2020;51(6):1408-1409. [33] SEYHAN M, TURKMEN I, UNAY K, et al. Do PFNA devices and Intertan nails both have the same effects in the treatment of trochanteric fractures? A prospective clinical study. J Orthop Sci. 2015;20(6):1053-1061. [34] 徐金渭,韩雷,胡云根,等.股骨近端解剖锁定钢板治疗伴外侧壁骨折的股骨转子间骨折中期疗效随访[J].中国骨伤,2017,30(3):256-260. [35] PALM H, LYSÉN C, KRASHENINNIKOFF M, et al. Intramedullary nailing appears to be superior in pertrochanteric hip fractures with a detached greater trochanter: 311 consecutive patients followed for 1 year. Acta Orthop. 2011;82(2):166-170. [36] HONGKU N, WORATANARAT P, NITIWARANGKUL L, et al. Fracture fixation versus hemiarthroplasty for unstable intertrochanteric fractures in elderly patients: A systematic review and network meta-analysis of randomized controlled trials. Orthop Traumatol Surg Res. 2022;108(1):102838. [37] WANG ZH, LI KN, LAN H, et al. A Comparative Study of Intramedullary Nail Strengthened with Auxiliary Locking Plate or Steel Wire in the Treatment of Unstable Trochanteric Fracture of Femur. Orthop Surg. 2020;12(1):108-115. [38] HAO Y, ZHANG Z, ZHOU F, et al. Risk factors for implant failure in reverse oblique and transverse intertrochanteric fractures treated with proximal femoral nail antirotation (PFNA). J Orthop Surg Res. 2019;14(1):350. [39] TIAN Z, CHEN J, ZHANG Y, et al. A Retrospective Study of 98 Elderly Patients with High-Risk Lateral Femoral Wall Intertrochanteric Hip Fractures to Compare Outcomes Following Surgery with Proximal Femoral Nail Antirotation (PFNA) Versus Dynamic Hip Screw (DHS). Med Sci Monit. 2022;28:e936923. [40] 蒋臻,郑明军,赵小波,等.不稳定股骨粗隆间骨折PFNA-Ⅱ术后效果的影响因素分析[J].中华全科医学,2021,19(12):2016-2019+2101. [41] 阮冠龙,姜自伟,岳志军,等.股骨转子间骨折外侧壁完整性对股骨近端防旋髓内钉治疗效果的影响[J].临床骨科杂志,2020,23(5):723-726. [42] 周平辉,乐意,张知理,等.PFNA联合抗骨质疏松药物治疗高龄患者股骨转子间骨折的疗效比较[J].中华全科医学,2019,17(6):920-923. [43] 沈浩,王伟,何继业,等.老年髋部骨折术前合并急性脑梗塞的危险因素分析[J].中华老年骨科与康复电子杂志,2017,3(5):275-280. [44] DENG HL, CONG YX, HUANG H, et al. The Effect of Integrity of Lateral Wall on the Quality of Reduction and Outcomes in Elderly Patients with Intertrochanteric Fracture: A Controlled Study. Biomed Res Int. 2021;2021:6563077. [45] 吉浩宇.呼和浩特市1638例股骨转子间骨折流行病学分布特征分析[J].中国组织工程研究,2017,21(16):2467-2471. [46] 刘刚,杨明辉,张京,等.北京地区老年髋部骨折的流行病学分布特点:多中心2 071例患者分析[J].中华创伤骨科杂志,2022,24(9):759-765. [47] 王志钢,田纪伟,史法见,等.股骨近端外侧壁完整性对股骨近端髓内钉固定的影响[J].中国矫形外科杂志,2020,28(20):1870-1874. [48] 陶金.PFNA治疗外侧壁完整型和外侧壁危险型股骨粗隆间骨折疗效比较[D].扬州:扬州大学,2020. [49] GUPTA RK, SANGWAN K, KAMBOJ P, et al. Unstable trochanteric fractures: the role of lateral wall reconstruction. Int Orthop. 2010;34(1):125-129. [50] 朱锦宇,朱庆生,韩一生,等.老年不稳定型转子间骨折的内固定选择及术后并发症原因分析[J].中华创伤骨科杂志,2005,7(6):505-507. [51] SHETTY A, BALLAL A, SADASIVAN AK, et al. Dynamic Hip Screw with Trochanteric Stablization Plate Fixation of Unstable Inter-Trochanteric Fractures: A Prospective Study of Functional and Radiological Outcomes. J Clin Diagn Res. 2016;10(9): RC06-RC08. |
| [1] | Zhang Qianlong, Maihemuti•Yakufu, Song Chenhui, Liu Xiuxin, Ren Zheng, Liu Yuzhe, Muyashaer•Abudushalamu, Sajidan•Aikebaier, Ran Jian. Finite element analysis of the effect of the distribution position and content of bone cement on the stress and displacement of reverse femoral intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(3): 336-340. |
| [2] | Li Guangsheng, Lin Weimin, Zhang Shenshen, Lin Wang, Lin Chengshou. Finite element analysis of unstable intertrochanteric fractures repaired with proximal femoral nail anti-rotation combined with anterolateral reconstruction plate [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(36): 5753-5759. |
| [3] | Zhou Long, Wang Liang, Xu Rui, Bao Yidong, He Shuangjian, Xu Xibin. Finite element analysis of femoral intertrochanteric fracture treated with intramedullary nail with different lateral wall classifications [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(29): 4652-4657. |
| [4] | He Shiping, Jia Dazhou, Li Xiaolei, Wang Qiang. Establishment of prediction model of blood transfusion after proximal femoral nail anti-rotation fixation of femoral intertrochanteric fracture in elderly adults [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 929-933. |
| [5] | Zhang Xinlong, Ci Wentao, Luo Kaiwen, Yan shi. Internal fixation failure after proximal femoral nail antirotation: causes and reoperation strategies [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 973-979. |
| [6] | Zhang Huabin, Zhang Muchen, Liu Chang, Xu Manman, Yin Qichuan, Zhang Aijun. Viability of different fat derivatives in vitro and the outcome after transplantation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(24): 3779-3784. |
| [7] | Yan Xinhao, Pang Fengxiang, Zhong Yuan, Chen Xiaojun, He Xiaoming, Hong Zhinan, Li Ziqi, Luo Zhihong, He Wei, Wei Qiushi. Correlation between the retention angle of the anterior and lateral wall of the femoral head and the progression of the femoral head collapse [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(36): 5827-5831. |
| [8] | Wu Zhonghan, Xu Xinzhong, Zhang Jisen, Zhao Yao, Ye Shuming, Yu Shuisheng, Sun Jian, Jing Juehua. One-stage reconstruction of the lateral wall of comminuted reverse oblique intertrochanteric fractures: how to improve the biomechanical stability of bone after repair [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(36): 5838-5843. |
| [9] | Lü Jiaxing, Bai Leipeng, Yang Zhaoxin, Miao Yuesong, Jin Yu, Li Zhehong, Sun Guangpu, Xu Ying, Zhang Qingzhu. Evaluation of internal fixation with proximal femoral nail antirotation in elderly knee osteoarthritis patients with femoral intertrochanteric fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 391-396. |
| [10] | Zhang Haiyang, Liu Jianzhang, Kan Na, Li Hongxia, Wang Junfeng, Jiang Haiwei, Qiu Chengyu, Xiao Zhen. Effect of excess resin adhesive removal method on the marginal integrity of all-ceramic crowns with different marginal gaps [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(28): 4480-4484. |
| [11] | Wang Hao, Wang Yitao, Lü Zexiang, Li Tengfei, Wang Shaolong, Wang Yehua. Effect of repeated intravenous tranexamic acid in the perioperative period of proximal femoral nail antirotation for femoral intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3319-3323. |
| [12] | Tian Kechao, Wang Lei, Tao Yong, Yao Tao. Proximal femoral nail antirotation combined with posteromedial wall reconstruction for the treatment of type A2 intertrochanteric fracture in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3337-3342. |
| [13] | Chen Sheng, Zheng Zhihui, Guan Keli, Li Xiaowu, Cai Peibiao, Chen Haibo, Zheng Xun, Zeng Qingqiang. Safety of reducing nausea and vomiting by intravenous infusion of tropisetron hydrochloride after internal fixation with proximal femoral nail antirotation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1869-1873. |
| [14] | Tao Jin, Xiong Guirun, Liu Pengran, Jiao Rui, Li Xiaolei, Yan Lianqi. Clinical significance of external wall of femoral intertrochanteric fracture and the treatment of internal fixation [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(30): 4854-4859. |
| [15] | Han Bing, Liu Hongbin, Zhang Chuankai, Sun Yiyan, Feng Hui, Zhao Riguang, Wang Ying. Artificial femoral head arthroplasty versus proximal femoral nail antirotation for the injured lateral wall intertrochanteric fracture in elderly adults [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 329-334. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||