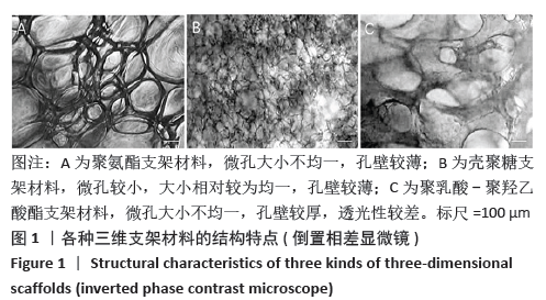
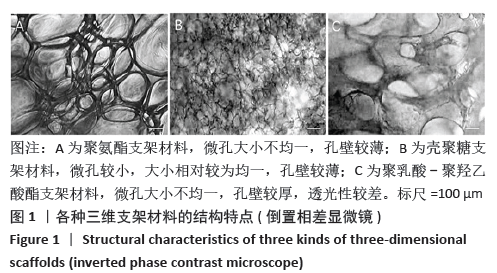
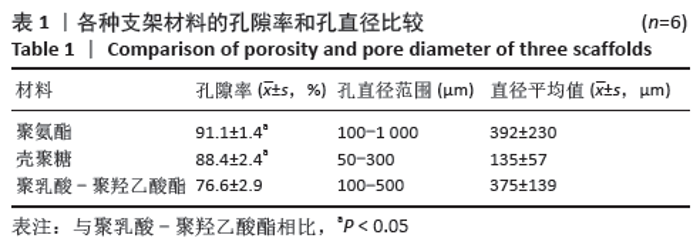
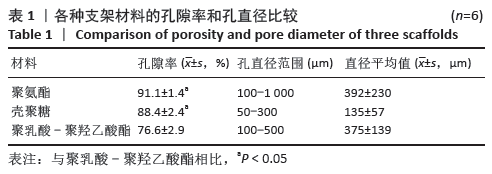
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (28): 4429-4434.doi: 10.12307/2021.053
Screening and optimization of three-dimensional scaffolds for the construction of bioartificial liver bioreactor
Chen Li1, Huang Lei2, Yu Mengyao2, Zhang Guoying1, Zhang Shichang2,3
- 1Department of Obstetrics, 2Department of Laboratory Medicine, the First Affiliated Hospital of Nanjing Medical University, Nanjing 210029, Jiangsu Province, China; 3Department of Infectious Diseases, Southwest Hospital, Third Military Medical University, Chongqing 400038, China
-
Received:2020-06-15Revised:2020-06-18Accepted:2020-07-29Online:2021-10-08Published:2021-05-14 -
Contact:Zhang Shichang, MD, Associate professor, Master’s supervisor, Department of Laboratory Medicine, the First Affiliated Hospital of Nanjing Medical University, Nanjing 210029, Jiangsu Province, China; Department of Infectious Diseases, Southwest Hospital, Third Military Medical University, Chongqing 400038, China E-mail:zsc78@yeah.net -
About author:Chen Li, MD, Associate professor, Department of Obstetrics, the First Affiliated Hospital of Nanjing Medical University, Nanjing 210029, Jiangsu Province, China -
Supported by:the National Natural Science Foundation of China, No. 81671836 (to ZSC)
CLC Number:
Cite this article
Chen Li, Huang Lei, Yu Mengyao, Zhang Guoying, Zhang Shichang. Screening and optimization of three-dimensional scaffolds for the construction of bioartificial liver bioreactor[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(28): 4429-4434.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
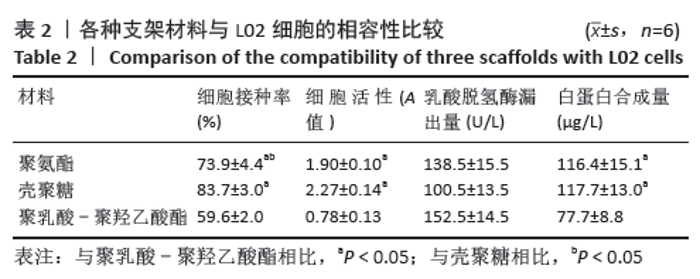

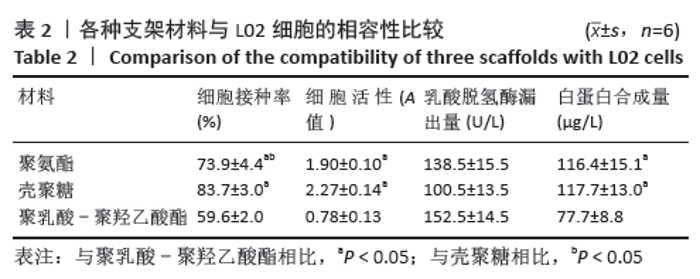
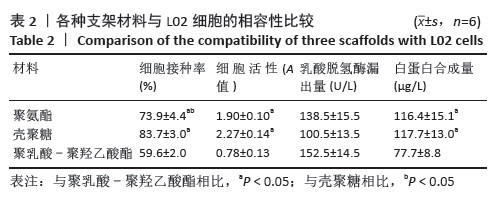
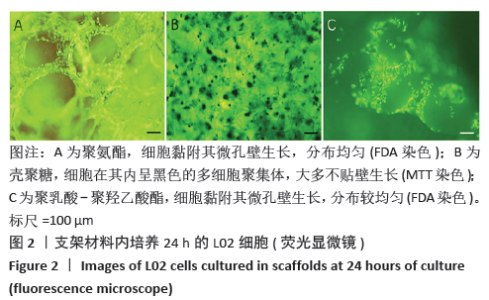
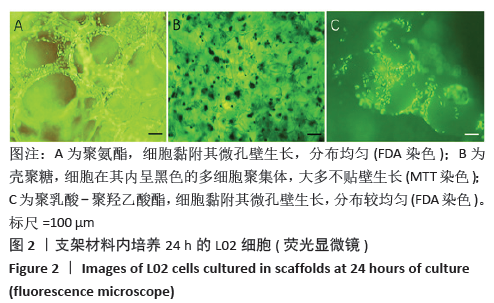
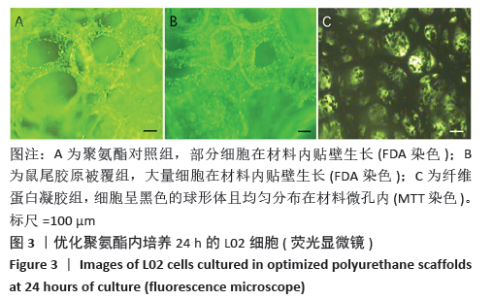
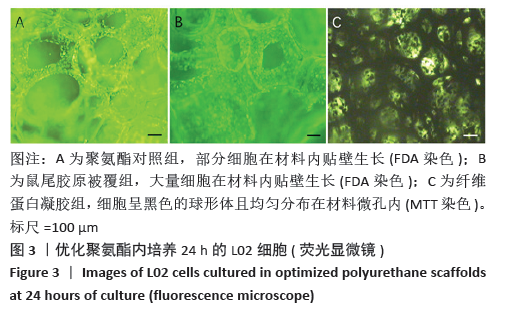
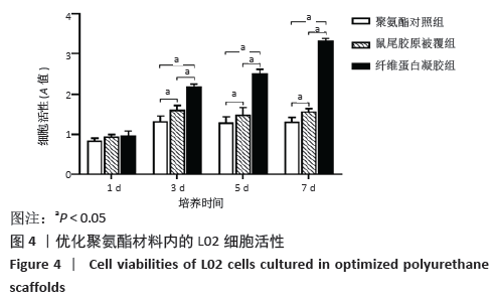
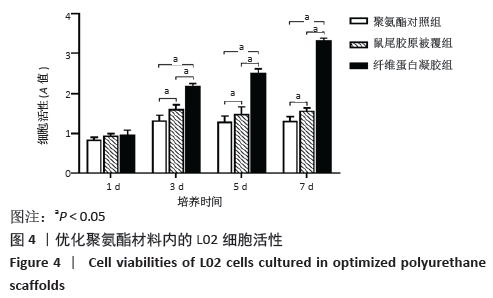
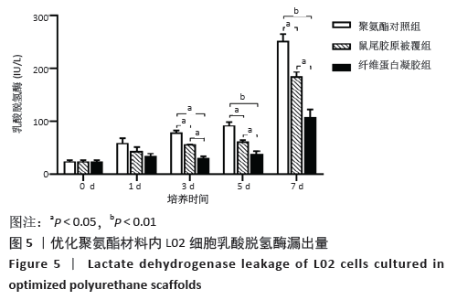
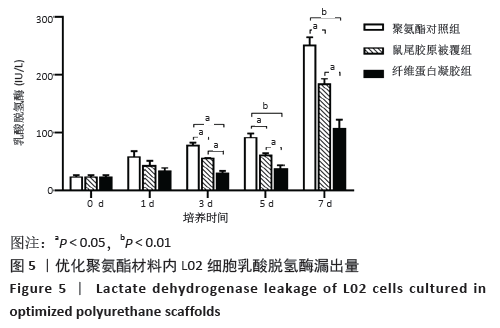
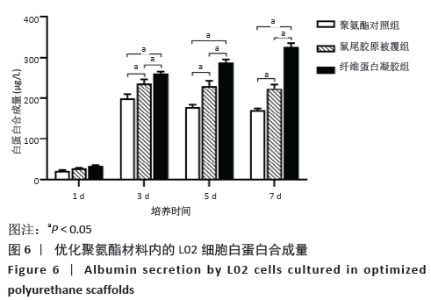
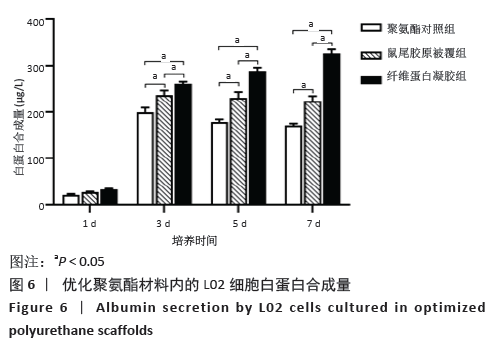
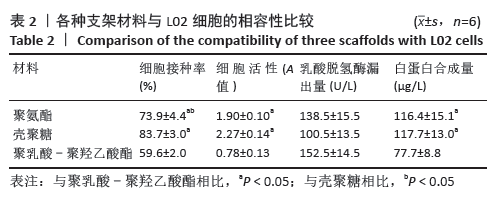
2.3.3 三维支架材料内的细胞活性 聚氨酯和壳聚糖内的L02细胞活性均较高,两者之间比较差异无显著性意义(P > 0.05);聚乳酸-聚羟乙酸酯内的L02细胞活性较低,低于聚氨酯和壳聚糖(P < 0.05),见表2。 2.3.4 三维支架材料内的细胞乳酸脱氢酶漏出量 聚乳酸-聚羟乙酸酯内的细胞乳酸脱氢酶漏出量稍高于聚氨酯和壳聚糖,但三者之间比较差异无显著性意义(P > 0.05),见表2。 2.3.5 三维支架材料的细胞白蛋白合成量 3种三维支架材料内的L02细胞均能合成大量白蛋白,聚氨酯与壳聚糖内的细胞白蛋白合成量比较差异无显著性意义(P > 0.05),但聚乳酸-聚羟乙酸酯内的细胞白蛋白合成量低于壳聚糖和聚氨酯(P < 0.05),见表2。"

| [1] HE YT, QI YN, ZHANG BQ, et al. Bioartificial liver support systems for acute liver failure: A systematic review and meta-analysis of the clinical and preclinical literature. World J Gastroenterol. 2019;25(27):3634-3648. [2] STRAIN AJ, NEUBERGER JM. A bioartificial liver--state of the art. Science. 2002; 295(5557):1005-1009. [3] SHI XL, GAO Y, YAN Y, et al. Improved survival of porcine acute liver failure by a bioartificial liver device implanted with induced human functional hepatocytes. Cell Res. 2016;26(2):206-216. [4] LI LJ, DU WB, ZHANG YM, et al. Evaluation of a bioartificial liver based on a nonwoven fabric bioreactor with porcine hepatocytes in pigs. J Hepatol. 2006;44(2):317-324. [5] KATAOKA K, NAGAO Y, NUKUI T, et al. An organic-inorganic hybrid scaffold for the culture of HepG2 cells in a bioreactor. Biomaterials. 2005;26(15):2509-2516. [6] DAVIDSON AJ, ELLIS MJ, CHAUDHURI JB. A theoretical method to improve and optimize the design of bioartificial livers. Biotechnol Bioeng. 2010;106(6):980-988. [7] ZHANG SC, LIU T, WANG YJ. Porous and single-skinned polyethersulfone membranes support the growth of HepG2 cells: a potential biomaterial for bioartificial liver systems. J Biomater Appl. 2012;27(3):359-366. [8] ZHANG S, LIU T, CHEN L, et al. Bifunctional polyethersulfone hollow fiber with a porous, single-layer skin for use as a bioartificial liver bioreactor. J Mater Sci Mater Med. 2012;23(8):2001-211. [9] YE H, XIA Z, FERGUSON DJ, et al. Studies on the use of hollow fibre membrane bioreactors for tissue generation by using rat bone marrow fibroblastic cells and a composite scaffold. J Mater Sci Mater Med. 2007;18(4):641-648. [10] ROZGA J, WILLIAMS F, RO MS, et al. Development of a bioartificial liver: properties and function of a hollow-fiber module inoculated with liver cells. Hepatology. 1993;17(2):258-265. [11] DE BARTOLO L, SALERNO S, CURCIO E, et al. Human hepatocyte functions in a crossed hollow fiber membrane bioreactor. Biomaterials. 2009;30(13):2531-2543. [12] YE SH, WATANABE J, TAKAI M, et al. Design of functional hollow fiber membranes modified with phospholipid polymers for application in total hemopurification system. Biomaterials. 2005;26(24):5032-5041. [13] SAKIYAMA R, HAMADA H, BLAU B, et al. Evaluation of the mass transfer rate using computer simulation in a three-dimensional interwoven hollow fiber-type bioartificial liver. Biotechnol Lett. 2018;40(11-12):1567-1578. [14] CHEN G, PALMER AF. Mixtures of hemoglobin-based oxygen carriers and perfluorocarbons exhibit a synergistic effect in oxygenating hepatic hollow fiber bioreactors. Biotechnol Bioeng. 2010;105(3):534-542. [15] FLENDRIG LM, LA SOE JW, JORNING GG, et al. In vitro evaluation of a novel bioreactor based on an integral oxygenator and a spirally wound nonwoven polyester matrix for hepatocyte culture as small aggregates. J Hepatol. 1997;26(6):1379-1392. [16] ZHANG S, CHEN L, LIU T, et al. Integration of single-layer skin hollow fibers and scaffolds develops a three-dimensional hybrid bioreactor for bioartificial livers. J Mater Sci Mater Med. 2014;25(1):207-216. [17] NAHMIAS Y, BERTHIAUME F, YARMUSH ML. Integration of technologies for hepatic tissue engineering. Adv Biochem Eng Biotechnol. 2007;103:309-329. [18] HOU YT, HSU CC. Development of a 3D porous chitosan/gelatin liver scaffold for a bioartificial liver device. J Biosci Bioeng. 2020;129(6):741-748. [19] MORGAN SM, TILLEY S, PERERA S, et al. Expansion of human bone marrow stromal cells on poly-(DL-lactide-co-glycolide) (PDL LGA) hollow fibres designed for use in skeletal tissue engineering. Biomaterials. 2007;28(35):5332-5343. [20] BELANGER MC, MAROIS Y, ROY R, et al. Selection of a polyurethane membrane for the manufacture of ventricles for a totally implantable artificial heart: blood compatibility and biocompatibility studies. Artif Organs. 2000;24(11):879-888. [21] SEO SJ, CHOI YJ, AKAIKE T, et al. Alginate/galactosylated chitosan/heparin scaffold as a new synthetic extracellular matrix for hepatocytes. Tissue Eng. 2006;12(1):33-44. [22] DE BARTOLO L, CATAPANO G, DELLA VOLPE C, et al. The effect of surface roughness of microporous membranes on the kinetics of oxygen consumption and ammonia elimination by adherent hepatocytes. J Biomater Sci Polym Ed. 1999;10(6):641-655. [23] GRANT MH, MORGAN C, HENDERSON C, et al. The viability and function of primary rat hepatocytes cultured on polymeric membranes developed for hybrid artificial liver devices. J Biomed Mater Res A. 2005;73(3):367-375. [24] HASIRCI V, BERTHIAUME F, BONDRE SP, et al. Expression of liver-specific functions by rat hepatocytes seeded in treated poly(lactic-co-glycolic) acid biodegradable foams. Tissue Eng. 2001;7(4):385-394. [25] CONCARO S, NICKLASSON E, ELLOWSSON L, et al. Effect of cell seeding concentration on the quality of tissue engineered constructs loaded with adult human articular chondrocytes. J Tissue Eng Regen Med. 2008;2(1):14-21. [26] SHI C, ZHU Y, RAN X, et al. Therapeutic potential of chitosan and its derivatives in regenerative medicine. J Surg Res. 2006;133(2):185-192. [27] GRIFFON DJ, SEDIGHI MR, SENDEMIR-URKMEZ A, et al. Evaluation of vacuum and dynamic cell seeding of polyglycolic acid and chitosan scaffolds for cartilage engineering. Am J Vet Res. 2005;66(4):599-605. [28] KARAGEORGIOU V, KAPLAN D. Porosity of 3D biomaterial scaffolds and osteogenesis. Biomaterials. 2005;26(27):5474-5491. [29] DU Y, HAN R, WEN F, et al. Synthetic sandwich culture of 3D hepatocyte monolayer. Biomaterials. 2008;29(3):290-301. [30] DU Y, CHIA SM, HAN R, et al. 3D hepatocyte monolayer on hybrid RGD/galactose substratum. Biomaterials. 2006;27(33):5669-5680. [31] UNDERHILL GH, CHEN AA, ALBRECHT DR, et al. Assessment of hepatocellular function within PEG hydrogels. Biomaterials. 2007;28(2):256-270. [32] NONAKA H, ISE H, SUGIHARA N, Et al. Development of highly functional long-term culture method of liver slice embedded in agarose gel for bioartificial liver. Cell Transplant. 2003;12(5):491-498 [33] LIU TSANG V, CHEN AA, CHO LM, et al. Fabrication of 3D hepatic tissues by additive photopatterning of cellular hydrogels. FASEB J. 2007;21(3):790-801. |
| [1] | Jiang Hongying, Zhu Liang, Yu Xi, Huang Jing, Xiang Xiaona, Lan Zhengyan, He Hongchen. Effect of platelet-rich plasma on pressure ulcers after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1149-1153. |
| [2] | Zou Gang, Xu Zhi, Liu Ziming, Li Yuwan, Yang Jibin, Jin Ying, Zhang Jun, Ge Zhen, Liu Yi. Human acellular amniotic membrane scaffold promotes ligament differentiation of human amniotic mesenchymal stem cells modified by Scleraxis in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1037-1044. |
| [3] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [4] | Zhang Bin, Sun Lihua, Zhang Junhua, Liu Yusan, Cui Caiyun. A modified flap immediate implant is beneficial to soft tissue reconstruction in maxillary aesthetic area [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 707-712. |
| [5] | Fu Shuanhu, Qin Kai, Lu Dahan, Qin Haibiao, Gu Jin, Chen Yongxi, Qin Haoran, Wei Jiading, Wu Liang, Song Quansheng. Lumbar spinal tuberculosis implanted with artificial bone with streptomycin sulfate and percutaneous pedicle screw under transforaminal endoscopy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 493-498. |
| [6] | Li Wenjing, Li Haobo, Liu Congna, Cheng Dongmei, Chen Huizhen, Zhang Zhiyong. Comparison of different bioactive scaffolds in the treatment of regenerative pulp of young permanent teeth [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 499-503. |
| [7] | Wang Yujiao, Liu Dan, Sun Song, Sun Yong. Biphasic calcium phosphate loaded with advanced platelet rich fibrin can promote the activity of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 504-509. |
| [8] | Chen Junyi, Wang Ning, Peng Chengfei, Zhu Lunjing, Duan Jiangtao, Wang Ye, Bei Chaoyong. Decalcified bone matrix and lentivirus-mediated silencing of P75 neurotrophin receptor transfected bone marrow mesenchymal stem cells to construct tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 510-515. |
| [9] | Li Chenjie, Lü Linwei, Song Yang, Liu Jingna, Zhang Chunqiu. Measurement and statistical analysis of trabecular morphological parameters of titanium alloy peri-prosthesis under preload [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 516-520. |
| [10] | Sun Qi, Zhou Yanan, Dong Xin, Li Ning, Yan Jiazhen, Shi Haojiang, Xu Sheng, Zhang Biao. Metal-ceramic interface characteristics of Co-Cr alloy fabricated by selective laser melting [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 521-525. |
| [11] | Liu Yang, Gong Yi, Fan Wei. Anti-hepatoma activity of targeted Pluronic F127/formononetin nanocomposite system in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 526-531. |
| [12] | Zhou Jihui, Yao Meng, Wang Yansong, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Influence of novel nanoscaffolds on biological behaviors of neural stem cells and the related gene expression [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 532-536. |
| [13] | Zhang Guomei, Zhu Jun, Hu Yang, Jiao Hongwei. Stress of three-dimensional finite element models of E-MAX porcelain inlay [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 537-541. |
| [14] | Liu Jiangfeng. Nano-hydroxyapatite/polyamide 66 composite filling combined with locking plate in the treatment of fibrous dysplasia of femoral bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 542-547. |
| [15] | Li Quanxi, Shen Yu, Wan Wei, Sun Shanzhi. Changes of abdominal wall mechanics and pain after tension-free inguinal hernia repair with polypropylene mesh [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 548-552. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||