Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (9): 1325-1330.doi: 10.3969/j.issn.2095-4344.2014.09.003
Previous Articles Next Articles
Analgesic effects of intraarticular cocktail versus intravenous parecoxib injection after total hip arthroplasty
Du Xue-ping1, Lu Jian-quan1, Xu Ping1, Zhu Yu-chang2, Dong Da-yong1
- 1 Qidong Hospital of Traditional Chinese Medicine (Qidong Branch, Tenth People’s Hospital, School of Medicine, Tongji University), Qidong 226200, Jiangsu Province, China; 2 Department of Orthopedics, Shanghai Tenth People’s Hospital, School of Medicine, Tongji University, Shanghai 200072, China
-
Online:2014-02-26Published:2014-02-26 -
Contact:Lu Jian-quan, Associate chief physician, Qidong Hospital of Traditional Chinese Medicine (Qidong Branch, Tenth People’s Hospital, School of Medicine, Tongji University), Qidong 226200, Jiangsu Province, China -
About author:Du Xue-ping, Studying for master’s degree, Attending physician, Qidong Hospital of Traditional Chinese Medicine (Qidong Branch, Tenth People’s Hospital, School of Medicine, Tongji University), Qidong 226200, Jiangsu Province, China
CLC Number:
Cite this article
Du Xue-ping, Lu Jian-quan, Xu Ping, Zhu Yu-chang, Dong Da-yong. Analgesic effects of intraarticular cocktail versus intravenous parecoxib injection after total hip arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(9): 1325-1330.
share this article
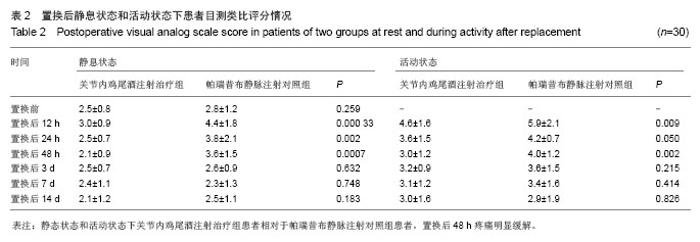
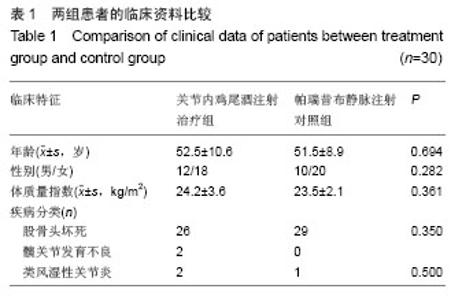
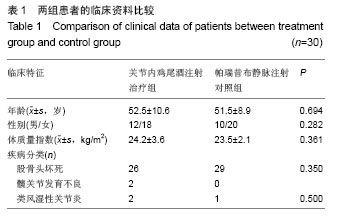
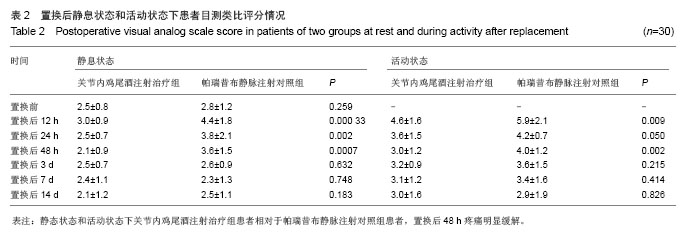
2.4 置换后疼痛目测类比评分 置换前关节内鸡尾酒注射治疗组与帕瑞昔布静脉注射对照组的目测类比评分分别为2.5±0.8及2.8±1.2,两者之间差异无显著性意义 (P > 0.05)。静息状态下关节内鸡尾酒注射治疗组患者置换后12,24,48 h及置换后3,7,14 d的目测类比评分依次为3.0±0.9,2.5±0.7,2.1±0.9,2.5±0.7,2.4±1.1及2.1±1.2分,而帕瑞昔布静脉注射对照组其置换后12,24,48 h及置换后3,7,14 d的目测类比评分则依 次为4.4±1.8,3.8±2.1,3.6±1.5,2.6±0.9,2.3±1.3及2.5±1.1分,关节内鸡尾酒注射治疗组患者置换后12,24,48 h疼痛较帕瑞昔布静脉注射对照组有明显缓解 (P < 0.05),而帕瑞昔布静脉注射对照组在置换后3,7,14 d疼痛程度虽较关节内鸡尾酒注射治疗组患者高,但二者之间差异无显著性意义(P > 0.05,表2)。 置换前关节内鸡尾酒注射治疗组患者置换后12,24,48 h及置换后3,7,14 d活动时疼痛目测类比评分依次为4.6±1.6,3.6±1.5,3.0±1.2,3.2±0.9,3.1±1.2及3.0±1.6,而帕瑞昔布静脉注射对照组患者置换后12,24,48 h及置换后3,7,14 d活动时疼痛目测类比评分依次为5.9±2.1,4.2±0.7,4.0±1.2,3.6±1.5,3.4±1.6及2.9±1.9分,治疗组患者置换后12,48 h活动疼痛较对照组有明显优势(P < 0.05,表2)。 2.5 手术时间和住院时间比较 关节内鸡尾酒注射治疗组和帕瑞昔布静脉注射对照组患者全髋置换从切皮到缝合结束的平均用时依次为(60.2±5.2) min及(55.2± 6.2) min,关节周围及关节腔内注射延长了手术时间,差异有显著性意义(P=0.001)。关节内鸡尾酒注射治疗组的住院时间为(10.4±2.1) d,帕瑞昔布静脉注射对照组的住院时间为(11.0±2.5) d,两组比较差异无显著性意义(P=0.318)。"
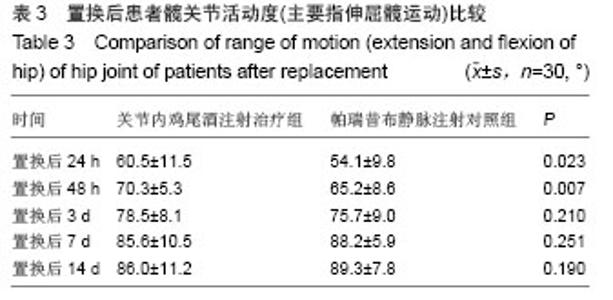
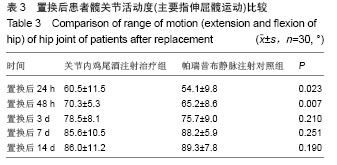
2.6 置换后髋关节功能评分比较 置换前髋关节活动度(主要指伸屈髋运动)两组间差异无显著性意义(P > 0.05),置换后48 h关节内鸡尾酒注射治疗组髋关节活动度大于帕瑞昔布静脉注射对照组,置换后3,7,14 d两组间髋关节活动度比较差异无显著性意义(P > 0.05,表3)。 2.7 置换后止痛药的用量及相关并发症的比较 置换后24 h到置换后第3天,治疗组的平均盐酸曲马多的用量为(650.0±50.2) mg,而对照组患者则为(700.0±85.8) mg,对照组需要消耗明显多的止痛药来维持患者的功能锻炼(P < 0.05)。 所有60例患者中,未出现术中或者术后栓塞,无肺部感染,无死亡患者。治疗组有1例患者出现髋关节深部血肿,后经引流后症状改善痊愈,1例注射部位的组织坏死,经局部切开引流后痊愈。治疗组及对照组分别有9及12例患者出现药物相关的恶心、呕吐反应,停药或者减量后症状改善,两组并发症发生率差异无显著性意义。"
| [1]Kerr DR, Kohan L. Local infiltration analgesia: a technique for the control of acute postoperative pain following knee and hip surgery: a case study of 325 patients.Acta Orthop. 2008;79(2): 174-183.[2]Chitre AR, Fehily MJ, Bamford DJ.Total hip replacement after intra-articular injection of local anaesthetic and steroid.J Bone Joint Surg Br. 2007;89(2):166-168.[3]Lunn TH, Husted H, Solgaard S,et al.Intraoperative local infiltration analgesia for early analgesia after total hip arthroplasty: a randomized, double-blind, placebo-controlled trial.Reg Anesth Pain Med. 2011;36(5):424-429. [4]刘伟,吴宇黎,吴海山,等.关节内注射镇痛混合剂在全髋关节置换术后的应用[J].实用骨科杂志,2011,17(12): 1077-1080,1113.[5]Klop C, de Vries F, Lalmohamed A,et al.COX-2-selective NSAIDs and risk of hip or knee replacements: a population-based case-control study.Calcif Tissue Int. 2012;91(6):387-394.[6]周红梅,祝胜美.静脉注射帕瑞昔布联合股神经阻滞用于老年病人膝关节置换术后镇痛及膝关节功能康复的效果[J]. 中华麻醉学杂志, 2011,31(8): 929-931.[7]Hightower CE, Riedel BJ, Feig BW,et al.A pilot study evaluating predictors of postoperative outcomes after major abdominal surgery: Physiological capacity compared with the ASA physical status classification system.Br J Anaesth. 2010; 104(4):465-471.[8]Schaffer I.Postoperative pain as the fifth vital parameter.Med Pregl. 2001;54(5-6):283-287.[9]徐卫东,吴岳嵩.人工全髋关节置换术后疼痛的原因分析[J].中国矫形外科杂志,2000,7(8): 804-805.[10]蒙辉能,张旭光,周伟俊,等.12例人工髋关节置换术后并发疼痛分析[J].广西中医学院学报,2005,8(1):30-31.[11]陈跃平,苏波,滕居赞,等.人工髋关节置换术后患肢早期疼痛原因分析[J].广西中医学院学报,2006,9(1):9-11.[12]黄伟,梁熙,孟纯阳,等.人工髋关节置换术后早期腹股沟区疼痛原因分析[J].中华创伤杂志,2006,22(11):811-814.[13]李晓华,周维江,吴海山,等.非骨水泥全髋关节置换与大腿痛[J].中国矫形外科杂志,2001,8(8):820-821.[14]张雷,杨国敬,郑进佑.人工髋关节置换术后大腿疼痛的研究现状[J].中华创伤骨科杂志,2007,9(2):177-180.[15]戴闽,艾江波,帅浪, 等.全髋关节置换术后疼痛评估[J].国际骨科学杂志,2010,31(3):133-136.[16]Jiang J, Teng Y, Fan Z,et al.The efficacy of periarticular multimodal drug injection for postoperative pain management in total knee or hip arthroplasty.J Arthroplasty. 2013;28(10): 1882-1887. [17]Wiesmann T, Steinfeldt T, Wagner G,et al.Supplemental single shot femoral nerve block for total hip arthroplasty - Impact on early postoperative care, pain management and lung function.Minerva Anestesiol. 2013. [Epub ahead of print][18]Lugeder A, Häring E, Müller A,et al.Total hip arthroplasty with the cementless spiron femoral neck prosthesis.Oper Orthop Traumatol. 2013;25(4):388-397.[19]Kerr DR, Kohan L.Local infiltration analgesia: a technique for the control of acute postoperative pain following knee and hip surgery: a case study of 325 patients.Acta Orthop. 2008; 79(2):174-183.[20]赵欣,李彦平,李树人,等.连续腰大肌间隙阻滞用于髋关节置换术后镇痛的临床观察[J].中国疼痛医学杂志,2001,7(3):148-148.[21]吴秀玲,曹金莉,刘爱萍.左旋布比卡因用于老年髋关节置换术后硬膜外自控镇痛的临床观察[J].临床麻醉学杂志,2007,23(5): 423. [22]翁文杰,王锋,陈东阳,等.全髋关节置换术中局部注射混合镇痛液疗效的临床对照试验[J].中国骨伤,2008,21(11):834-836.[23]王权光,陈婵娟,陈丽梅,等.连续腰丛神经阻滞联合夜间单次加强用于病人髋关节置换术后镇痛的效果[J].中华麻醉学杂志, 2012,32(12):1441-1444.[24]Axelsson K, Johanzon E, Essving P,et al. Postoperative extradural analgesia with morphine and ropivacaine. A double-blind comparison between placebo and ropivacaine 10 mg/h or 16 mg/h.Acta Anaesthesiol Scand. 2005;49(8): 1191-1199.[25]Neto JO, Machado MD, de Almeida Correa M,et al. Methadone patient-controlled analgesia for postoperative pain: a randomized, controlled, double-blind study.J Anesth. 2014. [Epub ahead of print][26]Zoric L, Cuvillon P, Alonso S,et al.Single-shot intraoperative local anaesthetic infiltration does not reduce morphine consumption after total hip arthroplasty: a double-blinded placebo-controlled randomized study.Br J Anaesth. 2014. [Epub ahead of print][27]Fowler SJ, Christelis N.High volume local infiltration analgesia compared to peripheral nerve block for hip and knee arthroplasty-what is the evidence?Anaesth Intensive Care. 2013;41(4):458-462.[28]张金山,李毅中.选择性COX-2抑制剂在髋关节置换术围术期镇痛中的应用[J].中国老年学杂志,2013,33(11):2514-2516.[29]McCarthy D, Iohom G.Local Infiltration Analgesia for Postoperative Pain Control following Total Hip Arthroplasty: A Systematic Review.Anesthesiol Res Pract. 2012;2012: 709531.[30]Kuchálik J, Granath B, Ljunggren A,et al. Postoperative pain relief after total hip arthroplasty: a randomized, double-blind comparison between intrathecal morphine and local infiltration analgesia.Br J Anaesth. 2013 ;111(5):793-799. [31]Breindahl T, Simonsen O, Hindersson P,et al.Autologous blood transfusion after local infiltration analgesia with ropivacaine in total knee and hip arthroplasty.Anesthesiol Res Pract. 2012;2012:458795.[32]Rikalainen-Salmi R, Förster JG, Mäkelä K,et al.Local infiltration analgesia with levobupivacaine compared with intrathecal morphine in total hip arthroplasty patients.Acta Anaesthesiol Scand. 2012;56(6):695-705.[33]Morin AM, Wulf H.High volume local infiltration analgesia (LIA) for total hip and knee arthroplasty: a brief review of the current status.Anasthesiol Intensivmed Notfallmed Schmerzther. 2011; 46(2):84-86. [34]符培亮,吴宇黎,吴海山,等.全膝置换术后关节内注射鸡尾酒式镇痛混合剂对镇痛效果的评价[J].中华骨科杂志,2008,28(7): 541-545. [35]Stein C, Comisel K, Haimerl E,et al.Analgesic effect of intraarticular morphine after arthroscopic knee surgery.N Engl J Med. 1991;325(16):1123-1126.[36]Badner NH, Bourne RB, Rorabeck CH,et al.Intra-articular injection of bupivacaine in knee-replacement operations. Results of use for analgesia and for preemptive blockade.J Bone Joint Surg Am. 1996;78(5):734-738.[37]Allen GC, St Amand MA, Lui AC,et al.Postarthroscopy analgesia with intraarticular bupivacaine/morphine. A randomized clinical trial.Anesthesiology. 1993;79(3):475-480.[38]Tanaka N, Sakahashi H, Sato E,et al.The efficacy of intra-articular analgesia after total knee arthroplasty in patients with rheumatoid arthritis and in patients with osteoarthritis.J Arthroplasty. 2001;16(3):306-311.[39]Rasmussen GL, Steckner K, Hogue C,et al. Intravenous parecoxib sodium foracute pain after orthopedic knee surgery.Am J Orthop (Belle Mead NJ). 2002;31(6):336-343.[40]Baharuddin KA, Rahman NH, Wahab SF,et al. Intravenous parecoxib sodium as an analgesic alternative to morphine in acute trauma pain in the emergency department.Int J Emerg Med. 2014;7(1):2.[41]卢园园,徐红党,周密,等.帕瑞昔布钠用于老年髋关节置换术后的镇痛效果和安全性[J].医学研究杂志,2012,41(1):120-123.[42]胡承方,陈云苏,王琦,等.帕瑞昔布钠对全膝全髋关节置换术后镇痛的疗效分析[J].中华创伤杂志,2011,27(12):1090-1095. [43]Viscusi ER, Gimbel JS, Halder AM,et al.A multiple-day regimen of parecoxib sodium 20 mg twice daily provides pain relief after total hip arthroplasty.Anesth Analg. 2008;107(2): 652-660. [44]吴新民,岳云,张利萍,等.术后镇痛中帕瑞昔布钠对吗啡用量的节俭作用和安全性 前瞻性、多中心、随机、双盲、安慰剂对照、平行分组研究[J].中华麻醉学杂志,2007,27(1):7-10.[45]赵晓红,熊君,宇俞卉,等.帕瑞昔布对老年全髋关节置换术患者的术后镇痛效果[J].实用疼痛学杂志,2012,8(3):205-207. |
| [1] | Chen Ziyang, Pu Rui, Deng Shuang, Yuan Lingyan. Regulatory effect of exosomes on exercise-mediated insulin resistance diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 4089-4094. |
| [2] | Chen Yang, Huang Denggao, Gao Yuanhui, Wang Shunlan, Cao Hui, Zheng Linlin, He Haowei, Luo Siqin, Xiao Jingchuan, Zhang Yingai, Zhang Shufang. Low-intensity pulsed ultrasound promotes the proliferation and adhesion of human adipose-derived mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3949-3955. |
| [3] | Yang Junhui, Luo Jinli, Yuan Xiaoping. Effects of human growth hormone on proliferation and osteogenic differentiation of human periodontal ligament stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3956-3961. |
| [4] | Sun Jianwei, Yang Xinming, Zhang Ying. Effect of montelukast combined with bone marrow mesenchymal stem cell transplantation on spinal cord injury in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3962-3969. |
| [5] | Gao Shan, Huang Dongjing, Hong Haiman, Jia Jingqiao, Meng Fei. Comparison on the curative effect of human placenta-derived mesenchymal stem cells and induced islet-like cells in gestational diabetes mellitus rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3981-3987. |
| [6] | Hao Xiaona, Zhang Yingjie, Li Yuyun, Xu Tao. Bone marrow mesenchymal stem cells overexpressing prolyl oligopeptidase on the repair of liver fibrosis in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3988-3993. |
| [7] | Liu Jianyou, Jia Zhongwei, Niu Jiawei, Cao Xinjie, Zhang Dong, Wei Jie. A new method for measuring the anteversion angle of the femoral neck by constructing the three-dimensional digital model of the femur [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3779-3783. |
| [8] | Meng Lingjie, Qian Hui, Sheng Xiaolei, Lu Jianfeng, Huang Jianping, Qi Liangang, Liu Zongbao. Application of three-dimensional printing technology combined with bone cement in minimally invasive treatment of the collapsed Sanders III type of calcaneal fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3784-3789. |
| [9] | Qian Xuankun, Huang Hefei, Wu Chengcong, Liu Keting, Ou Hua, Zhang Jinpeng, Ren Jing, Wan Jianshan. Computer-assisted navigation combined with minimally invasive transforaminal lumbar interbody fusion for lumbar spondylolisthesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3790-3795. |
| [10] | Hu Jing, Xiang Yang, Ye Chuan, Han Ziji. Three-dimensional printing assisted screw placement and freehand pedicle screw fixation in the treatment of thoracolumbar fractures: 1-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3804-3809. |
| [11] | Shu Qihang, Liao Yijia, Xue Jingbo, Yan Yiguo, Wang Cheng. Three-dimensional finite element analysis of a new three-dimensional printed porous fusion cage for cervical vertebra [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3810-3815. |
| [12] | Wang Yihan, Li Yang, Zhang Ling, Zhang Rui, Xu Ruida, Han Xiaofeng, Cheng Guangqi, Wang Weil. Application of three-dimensional visualization technology for digital orthopedics in the reduction and fixation of intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3816-3820. |
| [13] | Sun Maji, Wang Qiuan, Zhang Xingchen, Guo Chong, Yuan Feng, Guo Kaijin. Development and biomechanical analysis of a new anterior cervical pedicle screw fixation system [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3821-3825. |
| [14] | Lin Wang, Wang Yingying, Guo Weizhong, Yuan Cuihua, Xu Shenggui, Zhang Shenshen, Lin Chengshou. Adopting expanded lateral approach to enhance the mechanical stability and knee function for treating posterolateral column fracture of tibial plateau [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3826-3827. |
| [15] | Zhu Yun, Chen Yu, Qiu Hao, Liu Dun, Jin Guorong, Chen Shimou, Weng Zheng. Finite element analysis for treatment of osteoporotic femoral fracture with far cortical locking screw [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3832-3837. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||