Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (4): 678-682.doi: 10.3969/j.issn.2095-4344.2013.04.018
Previous Articles Next Articles
Evaluation on X-ray measurement methods of hallux valgus angle and 1-2 intermetatarsal angle after hallux valgus surgery
Sun Wei-dong, Wu Shou-chang, Wen Jian-min
- Department of Orthopedics, Wangjing Hospital of China Academy of Chinese Medical Sciences, Beijing 100102, China
-
Received:2012-04-25Revised:2012-06-18Online:2013-01-22Published:2013-03-05 -
Contact:Wen Jian-min, Chief physician, Professor, Doctoral supervisor, Department of Orthopedics, Wangjing Hospital of China Academy of Chinese Medical Sciences, Beijing 100102, China -
About author:Sun Wei-dong☆, Doctor, Associate chief physician, Department of Orthopedics, Wangjing Hospital of China Academy of Chinese Medical Sciences, Beijing 100102, China sunweidong8239@yahoo.com.cn
CLC Number:
Cite this article
Sun Wei-dong, Wu Shou-chang, Wen Jian-min. Evaluation on X-ray measurement methods of hallux valgus angle and 1-2 intermetatarsal angle after hallux valgus surgery[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(4): 678-682.
share this article
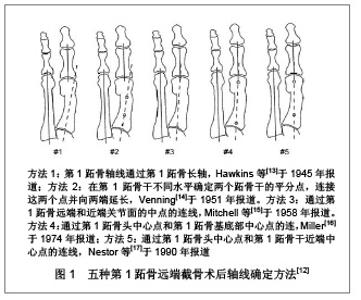
2.1 拇外翻负重位摄片方法 无论是术前还是术后,拇外翻均要求拍摄负重位片,标准的负重正位片是拇外翻术后X射线准确测量的前提。标准的拇外翻负重正位片的测量方法如Smith等[4]及Shima等[5]所述球管指向中足与第3跖骨中线交界处,X射线方向与在矢状面上的垂线成15°-20°夹角,以纠正和代偿站立时跖骨在水平面的倾斜。球管在冠状面上与片盒的垂直距离为100 cm。 2.2 拇外翻术后第1跖骨轴线的确定方法 从检索获得的有关拇外翻的文献资料看,国内拇外翻X射线测量方法介绍均局限在术前角度的测量上[6-7]。拇外翻术后疗效评价方面的论文,绝大部分未提及其所用的测量方法[8-10]。从国外文献资料看拇外翻术后第1跖骨轴线的确定方法大体分3类[11]:①根据第1跖骨近端和远端骨干的中点确定轴线,即经典方法。②根据跖骨头中心和基底部中心确定轴线。③根据第1跖骨两端关节面的中点确定轴线。最好的测量方法是其标记点必须是易于确定,可重复性好,应尽量避免受到截骨部位及跖骨本身解剖变异的影响。拇外翻术后X射线测量方法目前多用到center-of-head方法,跖骨头中心确定临床常用一种几何测量工具莫斯球[3],由直径相差2 mm同心圆组成,圆心有2 mm小孔。确定跖骨头中心时,根据跖骨头的内侧边、外侧边和顶端3个点选择合适的圆,圆心即为跖骨头中心。 2.2.1 第1跖骨远端截骨轴线的确定方法 Schneider 等[12]鉴于临床上不同拇外翻X射线测量方法测量结果相互冲突的状况,分别对临床5种常用测量方法进行了验证和评价,见图1。"
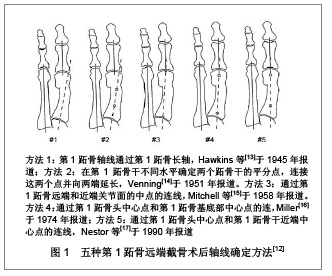
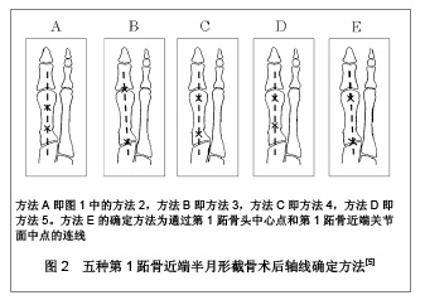
他们分别使用5种方法对20例术前和远端截骨术后(Chevron手术)患者的负重X射线片进行测量,评估这5种方法的测量精度,结果发现术前在5种方法之间的差异微小;术后评估在5种方法之间表现出很大的差别。研究提出对于跖骨远端截骨术X射线测量,不建议把跖骨轴作为第1跖骨轴线参考使用,这种方法测量精度差,尤其是术后。研究发现Miller于1974年描述的方法(即方法4)是测量拇外翻第1跖骨远端截骨术后角度的最准确的方法,这有别于作者以前推荐的方法3[18]。进一步分析认为方法4是“头部中心/基底部中心(center head/center base)”测量方法,受第1跖骨解剖变异和术后改变影响最小,故较为准确。方法3存在关节面内外侧缘确定困难情况,这就决定了关节面中心点的确定困难,因而影响其准确性。方法4因其准确可靠作者推荐作为拇外翻跖骨远端截骨术后临床测量使用。 2.2.2 第1跖骨近端截骨轴线的确定方法 Allen等[19]回顾了分析了第1跖骨近端截骨术后第1-2跖骨间角的测量方法资料,跖骨轴线的确定方法除去未明确说明之外,绝大部分采用跖骨解剖轴法(方法1),个别采用头部中心/基底部中心法(方法4)。作者使用这两种方法对21例拇外翻跖骨近端斜形截骨术后患者进行测量,结果表明两种测量方法,其结果存在显著的差异。认为头部中心/基底部中心法可能较解剖轴法更准确,但需要更多的临床研究结果支持。Randhawa等[20]报告了使用开放楔形截骨术L型钢板内固定治疗拇外翻,对于第1-2跖骨间角的术后测量采用的是Venning等[14]的方法,即平分第1,2跖骨干轴线交角。对于拇外翻角的术后测量则采用了头部中心/基底部中心法。Shima等[5]报道,通过5种测量方法对20例拇外翻行第1跖骨基底部新月形截骨术后的X射线片测量,见图2。作者在文中强调测量方法E是首次提出,但实际上Resch等[3]早在1989年就提出该方法。"

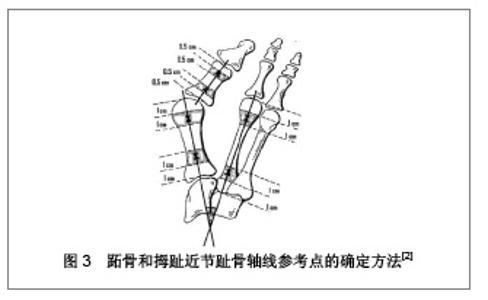
研究发现方法A和D在5种方法中可靠性较差,可能与跖骨近端标志点位于截骨部位,无法准确确定有关。方法B虽较前两法稍好,但因为第1跖骨头关节面,特别是外侧关节面边缘确定困难,影响其可靠性。方法C与方法E相较,其近端标志点靠近截骨端,方法E近端标志点在近端关节面中点,不受截骨端的影响,因此方法E具有更高的可靠性。作者认为该方法还可用于跖骨近端Chevron手术、开放楔形截骨术、闭合楔形截骨术、Scarf截骨术的测量。同时也指出这种方法的短处,如果是跖楔关节融合术后病例将为确定关节面的中心带来困难。 2.2.3 其他术式跖骨轴线的确定方法 Kopp等[21]对32例38足的改良Lapidus手术治疗拇外翻的随访和X射线的前后对比中,其使用的测量方法参照了Coughlin等[22]的拇外翻畸形角度测量的评价。Aminian 等[23]对27例Scarf截骨术后的患者进行了拇外翻角和第1-2跖骨间角测量,用的测量方法为跖骨干不同水平确定两个跖骨干的干垢端的平分点,连接这两个点并向两端延长(方法2)。作者认为该方法对骨干的截骨方式具有其特定测量意义。Srivastava等[11]在其有关拇外翻X射线测量的综述里则推荐通过第1跖骨头中心点和第1跖骨基底部中心点的连线的测量方法(方法4),用之进行Scarf术后拇外翻角和第1-2跖骨间角的测量。目前,未见对拇外翻联合截骨手术(如第1跖骨基底部闭合截骨联合Akin手术等)术后X射线测量方法的报道。这些术式的术后测量方法,仅见于小样本病例报道,未见大宗病例的对照研究和系统评价,因此,对于其有效性和可靠性仍需进一步验证与评价。 2.3 第2跖骨及拇趾近节趾骨轴线的确定方法 Coughlin等[2]出版了美国足与踝关节协会(AOFAS)角度测量专门委员会的报告,推荐了第1跖骨、第2跖骨和拇趾近节趾骨轴线参考点的确定方法,见图3。"
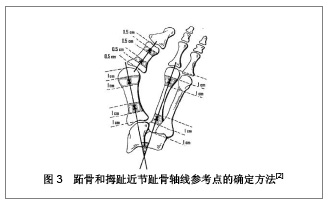

报告认为参考点靠近关节面不是十分可靠,建议将参考点尽量向跖骨干部靠近。对于第1跖骨轴线参考点的确定,应该位于干骺端,远端位于距离远端关节面近端1.0-2.0 cm范围内,近端位于距离近端关节面远端1.0-2.0 cm范围内,其1 cm的范围可以适合各种尺码的足。第2跖骨轴线参考点的确定与第1跖骨轴线的确定方法相同。对于拇趾近节趾骨轴线的确定他们推荐远端参考点位于距离远端关节面近端0.5- 1.0 cm范围内,近端参考点位于距离近端关节面远端0.5-1.0 cm范围内。拇趾远节趾骨轴线同近节趾骨。 2.4 计算机测量技术的应用 拇外翻的X射线测量一般都是在X射线片上手工绘线测量,其可靠性很不确定,可重复性较差,特别是同一张片子需要几种方法测量并需要多次重复时,反复多次画线往往对片子造成损伤,而且用刻度尺测量时由于各参考点均需手工测定和连接,增加了测量偏倚。随着计算机应用软件的发展和提高,出现了许多专业的图像测量软件,这些软件可以方便的画线、画圆,可以自由调整长度、大小和位置等,无限次重复。测量长度、角度等并能自动给出测量值,测量值可精确到小数点后3位数。这些为拇外翻的X射线测量提供了有力的工具。 有关使用电脑专业测量软件进行拇外翻角度测量的报道很多[24-26]。Srivastava等[27]一项对拇外翻角的手动测量和计算机测量的比较研究,比较了两种方法的时间和可靠性,研究证明手动的测量方法容易出错,并且耗时,计算机程序辅助测量可靠和高效。Piqué-Vidal等[28]评估了手动和电脑程序在拇外翻的X射线角度测量之间的差异,运用散点分析结果认为电脑程序Autocad技术的测量更为可靠,准确性高。Beasley等[29]对X-PoDite数字化X射线片分析仪使用的研究,认为能最大限度地准确的影像学测量、体现了其再现性和实用性,此外,所需要的时间也显著降低,是临床医生和科研的一项新技术。"

| [1] Deenik AR, de Visser E, Louwerens JW,et al. Hallux valgus angle as main predictor for correction of hallux valgus.BMC Musculoskelet Disord. 2008;9:70.[2] Coughlin MJ, Freund E.Roger A. Mann Award. The reliability of angular measurements in hallux valgus deformities. Foot Ankle Int. 2001;22(5):369-379.[3] Resch S, Stenström A, Egund N. Proximal closing wedge osteotomy and adductor tenotomy for treatment of hallux valgus. Foot Ankle. 1989;9(6):272-280.[4] Smith RW, Reynolds JC, Stewart MJ. Hallux valgus assessment: report of research committee of American Orthopaedic Foot and Ankle Society. Foot Ankle. 1984;5(2):92-103.[5] Shima H, Okuda R, Yasuda T,et al. Radiographic measurements in patients with hallux valgus before and after proximal crescentic osteotomy. J Bone Joint Surg Am. 2009; 91(6):1369-1376.[6] 周承涛,刘旭林,张光辉,等.拇外翻及正常足部的X线测量分析[J].医学影像学杂志,2003, 13(6):407-409.[7] 史思峰,董扬.拇外翻主要病理改变及组织修复方法的选择[J].中国组织工程研究与临床康复,2009,13(50):9958-9961.[8] 孙卫东,温建民,胡海威,等.微创截骨治疗拇外翻的远期疗效分析[J].中华骨科杂志,2010,30(11):1133-1137.[9] Sun WD, Wen JM, Hu HW,et al. Long term efficacy of minimal incision osteotomy for hallux abducto valgus. Orthop Surg. 2010;2(3):223-228.[10] 孙卫东,温建民,胡海威,等.康复疗法在中西医结合治疗拇外翻术后的应用效果观察[J].现代中西医结合杂志,2010, 19(22): 2731-2733.[11] Srivastava S, Chockalingam N, El Fakhri T. Radiographic measurements of hallux angles: a review of current techniques. Foot (Edinb). 2010;20(1):27-31.[12] Schneider W, Csepan R, Knahr K. Reproducibility of the radiographic metatarsophalangeal angle in hallux surgery. J Bone Joint Surg Am. 2003;85-A(3):494-499.[13] Hawkins FB, Mitchell CL, Hedrick DW. Correction of hallux valgus by metatarsal osteotomy. J Bone Joint Surg. 1945; 27:387-394.[14] Venning P.Sources of error in the production and measurement of standard radiographs of the foot.Br J Radiol. 1951;24(277):18-26.[15] Mitchell CL, Fleming JL, Allen R,et al. Osteotomy- bunionectomy for hallux valgus. J Bone Joint Surg Am. 1958; 40-A(1):41-58.[16] Miller JW. Distal first metatarsal displacement osteotomy. Its place in the schema of bunion surgery. J Bone Joint Surg Am. 1974;56(5):923-931.[17] Nestor BJ, Kitaoka HB, Ilstrup DM,et al. Radiologic anatomy of the painful bunionette. Foot Ankle. 1990;11(1):6-11.[18] Schneider W, Knahr K. Metatarsophalangeal and intermetatarsal angle: different values and interpretation of postoperative results dependent on the technique of measurement. Foot Ankle Int. 1998;19(8):532-536.[19] Allen DM, Nunley JA 2nd. Measurement of the first/second intermetatarsal angle following proximal oblique metatarsal osteotomy. Foot Ankle Int. 2002;23(1):64-67.[20] Randhawa S, Pepper D. Radiographic evaluation of hallux valgus treated with opening wedge osteotomy. Foot Ankle Int. 2009;30(5):427-431.[21] Kopp FJ, Patel MM, Levine DS,et al. The modified Lapidus procedure for hallux valgus: a clinical and radiographic analysis. Foot Ankle Int. 2005;26(11):913-917.[22] Coughlin MJ, Saltzman CL, Nunley JA 2nd. Angular measurements in the evaluation of hallux valgus deformities: a report of the ad hoc committee of the American Orthopaedic Foot & Ankle Society on angular measurements. Foot Ankle Int. 2002;23(1):68-74.[23] Aminian A, Kelikian A, Moen T. Scarf osteotomy for hallux valgus deformity: an intermediate followup of clinical and radiographic outcomes. Foot Ankle Int. 2006;27(11):883-886.[24] Piqué-Vidal C, Maled-García I, Arabi-Moreno J,et al. Radiographic angles in hallux valgus: differences between measurements made manually and with a computerized program. Foot Ankle Int. 2006;27(3):175-180.[25] Farber DC, Deorio JK, Steel MW 3rd. Goniometric versus computerized angle measurement in assessing hallux valgus. Foot Ankle Int. 2005;26(3):234-238.[26] Panchbhavi VK, Trevino S. Comparison between manual and computer-assisted measurements of hallux valgus parameters. Foot Ankle Int. 2004;25(10):708-711.[27] Srivastava S, Chockalingam N, El Fakhri T. Radiographic angles in hallux valgus: comparison between manual and computer-assisted measurements. J Foot Ankle Surg. 2010; 49(6):523-528.[28] Piqué-Vidal C, Maled-García I, Arabi-Moreno J,et al. Radiographic angles in hallux valgus: differences between measurements made manually and with a computerized program. Foot Ankle Int. 2006;27(3):175-180.[29] Beasley BD, Grambart ST, King JE. X-ray evaluation using the X-PODite digital radiograph analyzer. A preliminary study. Clin Podiatr Med Surg. 2002;19(4):477-482. |
| [1] | Wei Zhiheng, Guan Tianmin, Liu Qing, Gong Jue, Xiang Xianxiang. Application of 3D printing accurate osteotomy guide combined with the revision of anterior cruciate ligament with abnormally increased posterior slope of tibial plateau [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(33): 7130-7136. |
| [2] | Zhao Xiaoliang, Sun Meilan, Yan Tianyuan, Zhang Shizhe, Niu Guochang, Guan Yulong, Li Hua. Quantitative analysis of three-dimensional deformity indexes of the first metatarsal bone after osteotomy and orthosis for hallux valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5302-5307. |
| [3] | Wang Hu, Feng Shuo, Zhang Qiang, Chen Jiahao, Chen Xiangyang. Effect of varus and valgus angles of tibial prosthesis on short-term outcome of fixed bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(24): 3827-3832. |
| [4] | Tang Zhi, Lang Lei, Wang Renyuan, Gu Song. Construction of finite element model of hallux valgus foot and biomechanical analysis of the first metatarsophalangeal joint [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(27): 4283-4290. |
| [5] | Yang Jun, Kong Weifeng, Yuan Xiaoqing, Jin Rongzhong, Li Guijun. Finite element analysis of stress changes after elastic fixation between metatarsal bones for correction of hallux valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2809-2813. |
| [6] | Yuan Jing, Sun Xiaohu, Chen Hui, Qiao Yongjie, Wang Lixin. Digital measurement and analysis of the distal femur in adults with secondary knee valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 881-885. |
| [7] | Ma Chao, Wang Fei, Liu Xiaomin, Wang Ziyun, Xu Kui, Yang Wendong, Feng Wei. Quantification of the objective index of lumbar disc herniation with body surface topography map: three-dimensional angulation of the elastically fixed turning point of the lower back curve [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 924-928. |
| [8] | Li Guijun, Fang Xiaohui, Kong Weifeng, Yuan Xiaoqing, Jin Rongzhong, Yang Jun. Finite element analysis of the treatment of hallux valgus deformity by microplate combined with super strong suture elastic fixation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 938-942. |
| [9] | Gao Yi, Ma Yue, Zhao Zeyu. Foot bone self-regulation under weight-bearing standing analyzed by medical imaging measurement [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 959-962. |
| [10] | Bi Jingwei, Ren Jiabin, Liu Xin, Sun Ning, Li Rui, Li Yuefei, Sun Zhaozhong. 3D-CT-guided unilateral biportal endoscopic localization of L5 and S1 nerve roots and intervertebral space [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(33): 5283-5289. |
| [11] | Liu Jiali, Suo Hairui, Yang Han, Wang Ling, Xu Mingen. Influence of lay-down angles on mechanical properties of three-dimensional printed polycaprolactone scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(16): 2492-2497. |
| [12] | Wang Wencheng, Zhang Xingfei, Xu Yajun. Relationship between inclination angle of the transverse osteotomy line and the strength of hallux valgus orthopedic in Scarf osteotomy: analysis of three-dimensional bone reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(27): 4265-4270. |
| [13] | Wang Wencheng, Zhang Xingfei, Xu Yajun. Application of digital technology in the treatment of hallux valgus [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1911-1916. |
| [14] | Li Guijun, Huang Kai, An Jinyu, Zhang Lei, Gao Libo, Gao Lei, Wu Yixiong, Lu Jiajun. New application of Endobutton suspension plate in hallux valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1365-1370. |
| [15] |
Xie Fei, Li Yanle, Lin Xinxiao, Hu Haiwei, Sang Zhicheng, Sun Yongsheng, Jiang Kewei, Cheng Ying, Wen Guannan, Wen Jianmin, Sun Weidong.
Mechanism underlying mechanical stress regulating fibroblasts-derived
exosomes at the osteotomized end following hallux valgus correction |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||