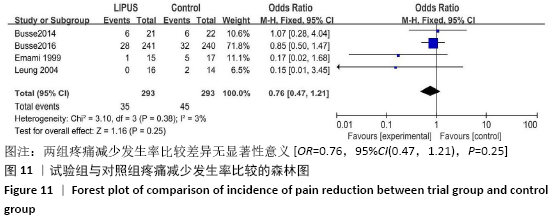
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (12): 1944-1950.doi: 10.3969/j.issn.2095-4344.3794
Previous Articles Next Articles
Low-intensity pulsed ultrasound in treatment of fractures: a systematic review and meta-analysis
Xia Sijie, Liao Qi
- Department of Orthopedics, the Third Affiliated Hospital of Nanchang University, Nanchang 330000, Jiangxi Province, China
-
Received:2020-04-03Revised:2020-04-14Accepted:2020-06-03Online:2021-04-28Published:2020-12-26 -
Contact:Liao Qi, Professor, Department of Orthopedics, the Third Affiliated Hospital of Nanchang University, Nanchang 330000, Jiangxi Province, China -
About author:Xia Sijie, Master candidate, Department of Orthopedics, the Third Affiliated Hospital of Nanchang University, Nanchang 330000, Jiangxi Province, China
CLC Number:
Cite this article
Xia Sijie, Liao Qi. Low-intensity pulsed ultrasound in treatment of fractures: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1944-1950.
share this article
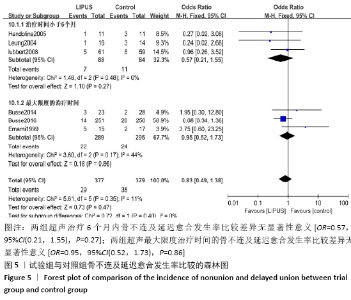
2.4.2 骨折后骨不连及延迟愈合发生率 纳入的11文献中有3篇报道了超声治疗6个月内骨不连及延迟愈合发生 率[16-17,20],文献间无异质性(Chi2=1.48,df=2,I2=0%,P=0.48),采用固定效应模型。Meta分析结果显示,两组超声治疗6个月内骨不连及延迟愈合发生率比较差异无显著性意义[OR=0.57,95%CI(0.21,1.55),P=0.27]。纳入的11篇文献中有3篇报道了最大限度治疗时间的骨不连及延迟愈合发生率[15,18-19],文献间无异质性(Chi2=3.6,df=2,I2=44%,P=0.17),采用固定效应模型。Meta分析结果显示,两组超声最大限度治疗时间的骨不连及延迟愈合发生率比较差异无显著性意义[OR=0.95,95%CI(0.52,1.73),P=0.86],见图5。"


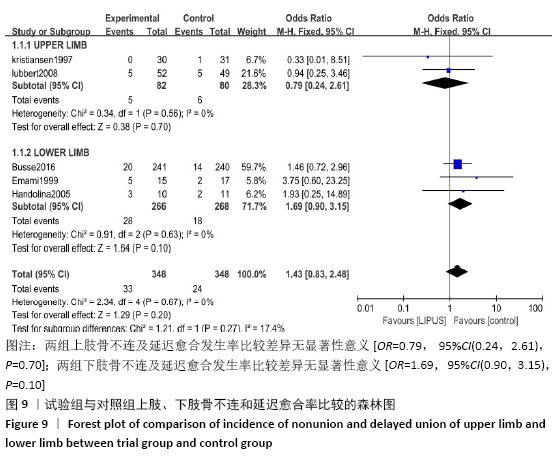
2.4.6 上肢及下肢骨不连及延迟愈合发生率 纳入的11篇文献中有2篇报道了上肢骨不连及延迟愈合发生率[20,23],文献间无异质性(Chi2=0.34,df=1,I2=0%, P=0.56),采用固定效应模型。Meta分析结果显示,两组上肢骨不连及延迟愈合发生率比较差异无显著性意义[OR=0.79, 95%CI(0.24,2.61),P=0.70],见图9。纳入的11篇文献中有3篇报道了下肢骨不连及延迟愈合发生率[15,17,19],文献间无异质性(Chi2=0.91,df=2,I2=0%, P=0.63),采用固定效应模型。Meta分析结果显示,两组下肢骨不连及延迟愈合发生率比较差异无显著性意义[OR=1.69, 95%CI(0.90,3.15),P=0.10],见图9。 "
| [1] EINHORN TA. Enhancement of fracture-healing. J Bone Joint Surg. 1995;77(6): 940-956. [2] DONALDSON LJ, SCHOLES S, SHELTON NJ, et al. The epidemiology of fractures in England. J Epidemiol Community Health. 2008;62(2):174-180. [3] CHILDS SG. Stimulators of Bone Healing: Biologic and Biomechanical. Orthop Nurs. 2003;22(6):421-428. [4] TROCK DH. Electromagnetic fields and magnets. Investigational treatment for musculoskeletal disorders. Rheum Dis Clin North Am. 2000;26(1):51-62. [5] GUO Y, YU X, KANG Q, et al. Effects and mechanisms of mechanical stress on secondary fracture healing. Front Biosci (Landmark Ed). 2013;18:1344-1348. [6] BUSSE JW, BHANDARI M. Therapeutic ultrasound and fracture healing: a survey of beliefs and practices. Arch Phys Med Rehabil. 2004;85(10):1653-1656. [7] MALIZOS KN, HANTES ME, PROTOPAPPAS V, et al. Low-intensity pulsed ultrasound for bone healing: an overview. Injury. 2006;37(66):S56-562. [8] LUO GY, SUN L, WEI EX, et al. The effects of low-intensity He-Ne laser irradiation on erythrocyte metabolism. Lasers Med Sci. 2015;30(9):2313-2318. [9] ALYESSARY AS, YAP AUJ, OTHMAN SA, et al. Effect of Piezoelectric Sutural Ostectomies on Accelerated Bone-Borne Sutural Expansion. J Oral Maxillofac Surg. 2018; 76(3):616-630. [10] GOPALAN A, PANNEERSELVAM E, DOSS GT, et al. Evaluation of Efficacy of Low Intensity Pulsed Ultrasound in Facilitating Mandibular Fracture Healing-A Blinded Randomized Controlled Clinical Trial. J Oral Maxillofac Surg. 2020;78(6):997.e1-997.e7. [11] WATANABE Y, MATSUSHITA T, BHANDARI M, et al. Ultrasound for fracture healing: current evidence. J Orthop Trauma. 2010; 24(6):56-61. [12] LOU S, LV H, LI Z, et al. Effect of low-intensity pulsed ultrasound on distraction osteogenesis: a systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. 2018;13(1):205. [13] BUSSE JW, MORTON E, LACCHETTI C, et al. Current management of tibial shaft fractures: a survey of 450 Canadian orthopedic trauma surgeons. Acta Orthop. 2008;79(5):689-694. [14] BUSSE JW, KAUR J, MOLLON B, et al. Low intensity pulsed ultrasonography for fractures: systematic review of randomised controlled trials. BMJ. 2009;33(8):351. [15] EMAMI A, PETRÉN-MALLMIN M, LARSSON S. No effect of low-intensity ultrasound on healing time of intramedullary fixed tibial fractures. J Orthop Trauma. 1999;13(4): 252-257. [16] LEUNG KS, LEE WS, TSUI HF, et al. Complex tibial fracture outcomes following treatment with low-intensity pulsed ultrasound. Ultrasound Med Biol. 2004;30(3):389-395. [17] HANDOLINA L, KILJUNEN V, ARNALA I, et al. Effect of ultrasound therapy on bone healing of lateral malleolar fractures of the ankle joint fixed with bioabsorbable screws. J Orthop Sci. 2005;10(4):391-395. [18] BUSSE JW, BHANDARI M, EINHORN TA, et al. Trial to re-evaluate ultrasound in the treatment of tibial fractures (TRUST): a multicenter randomized pilot study. Trials. 2014;15(8):20-26. [19] BUSSE JW, MOHIT BHANDARI M, EINHORN TA, et al. Re-evaluation of low intensity pulsed ultrasound in treatment of tibial fractures (TRUST): randomized clinical trial. BMJ. 2016;35(5):53-51. [20] LUBBERT PH, VAN DER RIJT RH, HOORNTJE LE, et al. Low-intensity pulsed ultrasound (LIPUS) in fresh clavicle fractures: a multi-centre double blind randomised controlled trial. Injury. 2008;39(12):1444-1452. [21] MAYR E, RUDZKI MM, RUDZKI M, et al. [Does low intensity, pulsed ultrasound speed healing of scaphoid fractures?]. Handchir Mikrochir Plast Chir. 2000;32(2):115-122. [22] LIU Y, WEI X, KUANG Y, et al. Ultrasound treatment for accelerating fracture healing of the distal radius. A control study. Acta Cir Bras. 2014;29(11):765-770. [23] KRISTIANSEN TK, RYABY JP, MCCABE J, et al. Accelerated healing of distal radial fractures with the use of specific, low-intensity ultrasound. A multicenter, prospective, randomized, double-blind, placebo-controlled study. J Bone Joint Surg Am. 1997;79(7): 961-973. [24] TARRIDE JE, HOPKINS RB, BLACKHOUSE G, et al. Low-intensity pulsed ultrasound for treatment of tibial fractures: an economic evaluation of the TRUST study. Bone Joint J. 2017;99(11):1526-1532. [25] SIMPSON AH, KEENAN G, NAYAGAM S, et al. Low-intensity pulsed ultrasound does not influence bone healing by distraction osteogenesis: a multicentre double-blind randomised control trial. Bone Joint J. 2017; 99(4):494-502. [26] DUDKIEWICZ I, HEIM M, SALAI M, et al. Ultrasonographic evaluation of union in long bones fractures. J Musculoskelet Res. 2009;12(2):105-112. [27] NMATSUMOTO K, SHIMO T, KURIO N, et al. Low-intensity pulsed ultrasound stimulation promotes osteoblast differentiation through hedgehog signaling. J Cell Biochem. 2018; 119(6):4352-4360. [28] CHAPMAN IV, MACNALLY NA, TUCKER S. Ultrasound-induced changes in rates of influx and efflux of potassium ions in rat thymocytes in vitro. Ultrasound Med Biol. 1980;6(1):47-58. [29] LI JK, LIN JC, LIU HC, et al. Cytokine release from osteoblasts in response to different intensities of pulsed electromagnetic field stimulation. Electromagn Biol Med. 2007; 26(3):153-165. [30] HADJIARGYROU M, MCLEOD K, RYABY JP, et al. Enhancement of fracture healing by low intensity ultrasound. Clin Orthop Relat Res. 1998;35(8):216-229. [31] YANG KH, PARVIZI J, WANG SJ, et al. Exposure to low-intensity ultrasound increases aggrecan gene expression in a rat femur fracture model. J Orthop Res. 1996; 14(5):802-809. [32] MIYAMOTO K ,AN HS, SAH RL, et al. Exposure to Pulsed Low Intensity Ultrasound Stimulates Extracellular Matrix Metabolism of Bovine Intervertebral Disc Cells Cultured in Alginate Beads. Spine (Phila Pa 1976). 2005;30(21):2398-2405. [33] MALLAKPOUR S, KHODADADZADEH L. Ultrasonic-assisted fabrication of starch/MWCNT-glucose nanocomposites for drug delivery. Ultrason Sonochem. 2018; 40(6):402-409. [34] MCKENNA RT, DOVE JC, RATZLAFF RA, et al. A 3-Dimensional Printed Ultrasound Probe Visuospatial Trainer. Ultrasound Q. 2018;34(2):103-105. [35] 张婷婷,高明霞,夏鹏,等.低强度脉冲超声与吡格列酮对骨关节炎软骨细胞的影响[J].中华物理医学与康复杂志,2018, 40(3):167-173. [36] ALIABOUZAR M, LEE SJ, ZHOU X, et al. Effects of scaffold microstructure and low intensity pulsed ultrasound on chondrogenic differentiation of human mesenchymal stem cells. Biotechnol Bioeng. 2018;115(2): 495-506. [37] BANIASAD F, MAKKIABADI B, SOLGI R, et al. Transcranial Focused Ultrasound Modulates Electrical Behavior of the Neurons: Design and Implementation of a Model. J Biomed Phys Eng. 2020;10(1):65-74. [38] BAYRAM S, KENDIRCI AŞ, KIRAL D, et al. Isokinetic Strength Comparison of Tuberosity Fractures of the Proximal Fifth Metatarsal Treated With Elastic Bandage vs Cast. Foot Ankle Int. 2020; 41(6):211-222. [39] 余章斌.重新评价meta分析在临床科研中的作用[J].中华围产医学杂志, 2015, 18(3):210-213. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [8] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [9] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [10] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [11] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [12] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [13] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [14] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [15] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||