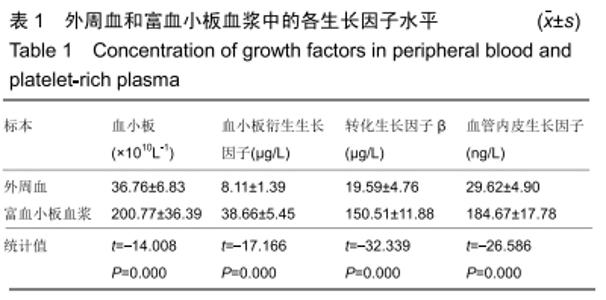
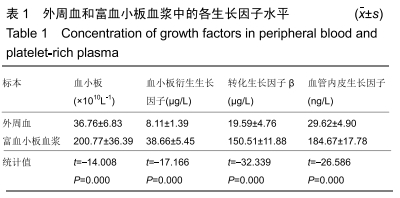
Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (14): 2205-2210.doi: 10.3969/j.issn.2095-4344.2594
Previous Articles Next Articles
Platelet-rich plasma interferes with changes in articular cartilage and synovium of rabbits with knee osteoarthritis
Qiu Hao, Chen Shimou, Weng Zheng, Zhu Yun, Liu Dun, Chen Yu
- Center for Traumatology, Ninth People’s Hospital of Chongqing, Chongqing 400700, China
-
Received:2019-07-10Revised:2019-08-21Accepted:2019-10-24Online:2020-05-18Published:2020-03-15 -
Contact:Chen Yu, MD, Chief physician, Center for Traumatology, Ninth People’s Hospital of Chongqing, Chongqing 400700, China -
About author:Qiu Hao, Master, Center for Traumatology, Ninth People’s Hospital of Chongqing, Chongqing 400700, China -
Supported by:the Scientific Research Project of Chongqing Beibei District Science and Technology Commission, No. 2018-8
CLC Number:
Cite this article
Qiu Hao, Chen Shimou, Weng Zheng, Zhu Yun, Liu Dun, Chen Yu. Platelet-rich plasma interferes with changes in articular cartilage and synovium of rabbits with knee osteoarthritis[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(14): 2205-2210.
share this article
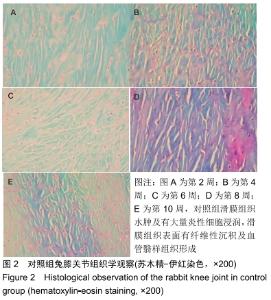
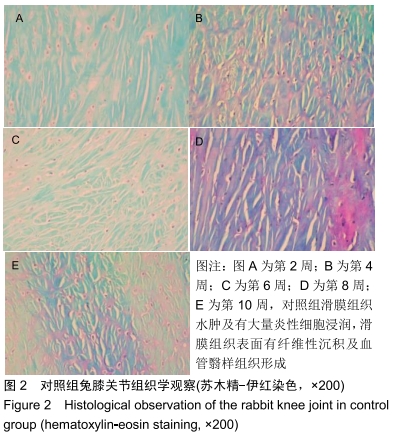
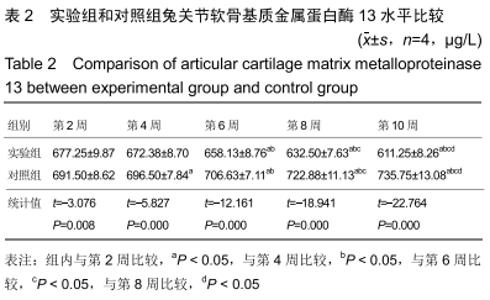
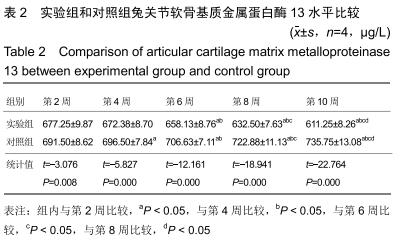
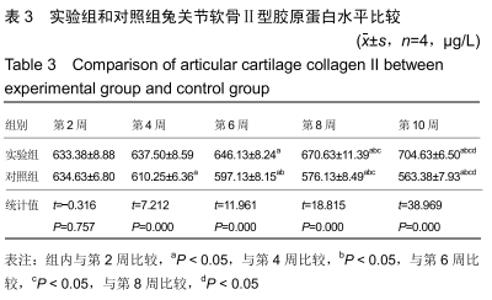
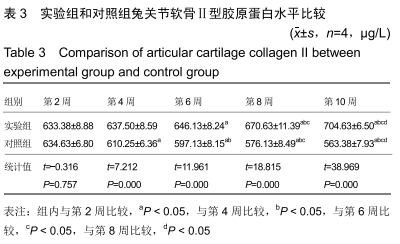
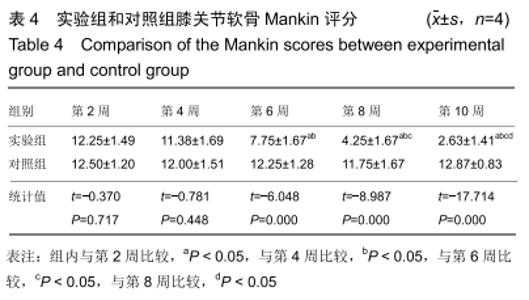
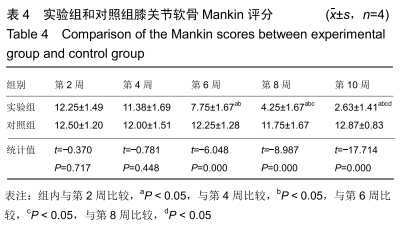
2.3 一般情况 所有实验动物无死亡,实验动物双侧肢体无骨性关节炎以外的其他症状。 2.4 大体观察及组织学观察 第2周,实验组及对照组双侧膝关节的软骨均出现软骨变薄、软化、色泽暗淡等现象。实验组动物的滑膜组织稍水肿并伴随炎性反应,局部可见少量绒毛样的组织形成;对照组可见水肿伴渗出的滑膜组织,局部可见大量绒毛样的组织形成,外观呈黄褐色,部分融合成肉芽肿结节,细胞数目增多伴肥大,滑膜全层均有巨噬细胞、淋巴细胞等炎性细胞浸润。 第4周,实验组动物的双侧膝关节软骨情况与第2周相似,对照组动物的双侧膝关节软骨可见糜烂及裂隙等现象。实验组动物的滑膜组织水肿较前缓解,局部仍可见绒毛样的组织,而对照组滑膜组织水肿明显伴渗出,可见炎性细胞浸润,滑膜表面可见血管翳样组织。 第6周,实验组软骨色泽较为暗淡,无裂隙等现象,对照组软骨色泽暗,可见糜烂、裂隙等现象。实验组动物的滑膜组织水肿比之间缓解明显,其中可见部分新生的血管,对照组滑膜组织明显水肿,有较多新生的血管及炎性组织,其中还可见纤维性沉积及血管翳样组织。 第8周,实验组软骨及滑膜组织情况较前仍好转,对照组软骨及滑膜组织情况仍较差。 第10周,实验组软骨色泽略暗淡,其他情况接近正常的软骨组织,对照组软骨色泽灰暗,出现糜烂及裂隙等现象。实验组滑膜组织接近正常滑膜组织,对照组滑膜组织水肿及渗出,出现大量炎性细胞浸润,滑膜组织表面有纤维性沉积及血管翳样组织形成。见图1,2。 "
| [1] BERENBAUM F, GRIFFIN TM, LIU-BRYAN R. Review: Metabolic Regulation of Inflammation in Osteoarthritis. Arthritis Rheumatol.2017; 69(1): 9-21. [2] MOURA MDEL G, LOPES LC, BIAVATTI MW, et al. Brazilian oral herbal medication for osteoarthritis: a systematic review protocol.Syst Rev.2016; 5:86. [3] MALFAIT AM. Osteoarthritis year in review 2015: biology. Osteoarthritis Cartilage.2016;24(1): 21-26. [4] NI GX. Development and Prevention of Running-Related Osteoarthritis.Curr Sports Med Rep.2016; 15(5): 342-349. [5] STEADMAN JR, BRIGGS KK, POMEROY SM, et al. Current state of unloading braces for knee osteoarthritis. Knee Surg Sports Traumatol Arthrosc.2016; 24(1): 42-50. [6] YUN S, KU SK, KWON YS. Adipose-derived mesenchymal stem cells and platelet-rich plasma synergistically ameliorate the surgical-induced osteoarthritis in Beagle dogs.J Orthop Surg Res.2016; 11(1): 9. [7] ALSHAMI AM. Knee osteoarthritis related pain: a narrative review of diagnosis and treatment.Int J Health Sci (Qassim). 2014; 8(1): 85-104. [8] YU P, HUNTER DJ. Intra-articular therapies for osteoarthritis. Expert Opin Pharmacother.2016; 17(15): 2057-2071. [9] BENNELL KL, BUCHBINDER R, HINMAN RS. Physical therapies in the management of osteoarthritis: current state of the evidence.Curr Opin Rheumatol.2015; 27(3): 304-311. [10] WENHAM CY, MCDERMOTT M, CONAGHAN PG. Biological therapies in osteoarthritis.Curr Pharm Des.2015; 21(17): 2206-2215. [11] KALUNIAN KC. Current advances in therapies for osteoarthritis. Curr Opin Rheumatol.2016; 28(3): 246-250. [12] ROMAN-BLAS JA, BIZZI E, LARGO R, et al.An update on the up and coming therapies to treat osteoarthritis, a multifaceted disease.Expert Opin Pharmacother.2016; 17(13):1745-1756. [13] JEVSEVAR DS. Treatment of osteoarthritis of the knee: evidence-based guideline, 2nd edition. J Am Acad Orthop Surg. 2013; 21(9): 571-576. [14] SANCHEZ M, ANITUA E, DELGADO D, et al.A new strategy to tackle severe knee osteoarthritis: Combination of intra-articular and intraosseous injections of Platelet Rich Plasma.Expert Opin Biol Ther.2016; 16(5): 627-643. [15] JOHNSON CI, ARGYLE DJ, CLEMENTS DN. In vitro models for the study of osteoarthritis.Vet J.2016; 209:40-49. [16] ORNETTI P, NOURISSAT G, BERENBAUM F, et al. Does platelet-rich plasma have a role in the treatment of osteoarthritis?.Joint Bone Spine.2016; 83(1): 31-36. [17] FILARDO G, KON E, ROFFI A, et al. Platelet-rich plasma: why intra-articular? A systematic review of preclinical studies and clinical evidence on PRP for joint degeneration.Knee Surg Sports Traumatol Arthrosc.2015; 23(9): 2459-2474. [18] LI FX, LI Y, QIAO CW, et al. Topical use of platelet-rich plasma can improve the clinical outcomes after total knee arthroplasty: A systematic review and meta-analysis of 1316 patients.Int J Surg.2017; 38:109-116. [19] KENNEDY MI, WHITNEY K, EVANS T, et al. Platelet-Rich Plasma and Cartilage Repair[J]. Curr Rev Musculoskelet Med. 2018; 11(4): 573-582. [20] ABD EL, RAOUF M, WANG X, et al.Injectable-platelet rich fibrin using the low speed centrifugation concept improves cartilage regeneration when compared to platelet-rich plasma. Platelets.2019; 30(2): 213-221. [21] HOKUGO A, OZEKI M, KAWAKAMI O, et al. Augmented bone regeneration activity of platelet-rich plasma by biodegradable gelatin hydrogel.Tissue Eng.2005; 11(7-8): 1224-1233. [22] STOOP R, BUMA P, VAN DER KRAAN PM, et al.Type II collagen degradation in articular cartilage fibrillation after anterior cruciate ligament transection in rats. Osteoarthritis Cartilage. 2001; 9(4): 308-315. [23] MANKIN HJ, DORFMAN H, LIPPIELLO L, et al. Biochemical and metabolic abnormalities in articular cartilage from osteoarthritis human hips. II. Correlation of morphology with biochemical and metabolic data.J Bone Joint Surg (Am).1971; 53(3): 523-537. [24] BENNELL KL, HUNTER DJ, PATERSON KL. Platelet-Rich Plasma for the Management of Hip and Knee Osteoarthritis. Curr Rheumatol Rep.2017; 19(5): 24. [25] MARUYAMA M, SATAKE H, SUZUKI T, et al. Comparison of the Effects of Osteochondral Autograft Transplantation With Platelet-Rich Plasma or Platelet-Rich Fibrin on Osteochondral Defects in a Rabbit Model.Am J Sports Med.2017; 45(14): 3280-3288. [26] LITTLE CB, BARAI A, BURKHARDT D, et al. Matrix metalloproteinase 13-deficient mice are resistant to osteoarthritic cartilage erosion but not chondrocyte hypertrophy or osteophyte development. Arthritis Rheum. 2009; 60(12): 3723-3733. [27] THOMA DS, LIM HC, SAPATA VM, et al. Recombinant bone morphogenetic protein-2 and platelet-derived growth factor-BB for localized bone regeneration. Histologic and radiographic outcomes of a rabbit study.Clin Oral Implants Res.2017; 28(11): e236-e243. [28] DEPRES-TREMBLAY G, CHEVRIER A, TRAN-KHANH N, et al. Chitosan inhibits platelet-mediated clot retraction, increases platelet-derived growth factor release, and increases residence time and bioactivity of platelet-rich plasma in vivo.Biomed Mater.2017; 13(1): 015005. [29] SARBAN S, TABUR H, BABA ZF, et al. The positive impact of platelet-derived growth factor on the repair of full-thickness defects of articular cartilage.Eklem Hastalik Cerrahisi.2019; 30(2): 91-96. [30] COSTA ELD,TEIXEIRA LEM,PADUA BJ,et al.Biomechanical study of the effect of platelet rich plasma on the treatment of medial collateral ligament lesion in rabbits.Acta Cir Bras.2017; 32(10): 827-835. [31] SPREAFICO A, CHELLINI F, FREDIANI B, et al. Biochemical investigation of the effects of human platelet releasates on human articular chondrocytes.J Cell Biochem.2009; 108(5): 1153-1165. [32] PETTERSSON S, WETTERO J, TENGVALL P, et al. Human articular chondrocytes on macroporous gelatin microcarriers form structurally stable constructs with blood-derived biological glues in vitro. J Tissue Eng Regen Med.2009; 3(6): 450-460. [33] ANGOORANI H, MAZAHERINEZHAD A, MARJOMAKI O, et al.Treatment of knee osteoarthritis with platelet-rich plasma in comparison with transcutaneous electrical nerve stimulation plus exercise: a randomized clinical trial.Med J Islam Repub Iran.2015; 29:223. [34] MEHEUX CJ, MCCULLOCH PC, LINTNER DM, et al. Efficacy of Intra-articular Platelet-Rich Plasma Injections in Knee Osteoarthritis: A Systematic Review.Arthroscopy.2016; 32(3): 495-505. |
| [1] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [2] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [3] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [4] | Jiang Hongying, Zhu Liang, Yu Xi, Huang Jing, Xiang Xiaona, Lan Zhengyan, He Hongchen. Effect of platelet-rich plasma on pressure ulcers after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1149-1153. |
| [5] | Wu Xun, Meng Juanhong, Zhang Jianyun, Wang Liang. Concentrated growth factors in the repair of a full-thickness condylar cartilage defect in a rabbit [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1166-1171. |
| [6] | Liu Xiangxiang, Huang Yunmei, Chen Wenlie, Lin Ruhui, Lu Xiaodong, Li Zuanfang, Xu Yaye, Huang Meiya, Li Xihai. Ultrastructural changes of the white zone cells of the meniscus in a rat model of early osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1237-1242. |
| [7] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| [8] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [9] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [10] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| [11] | Ma Zetao, Zeng Hui, Wang Deli, Weng Jian, Feng Song. MicroRNA-138-5p regulates chondrocyte proliferation and autophagy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 674-678. |
| [12] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [13] | Cao Xuhan, Bai Zixing, Sun Chengyi, Yang Yanjun, Sun Weidong. Mechanism of “Ruxiang-Moyao” herbal pair in the treatment of knee osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 746-753. |
| [14] | Li Yonghua, Feng Qiang, Tan Renting, Huang Shifu, Qiu Jinlong, Yin Heng. Molecular mechanism of Eucommia ulmoides active ingredients treating synovitis of knee osteoarthritis: an analysis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 765-771. |
| [15] | Song Shan, Hu Fangyuan, Qiao Jun, Wang Jia, Zhang Shengxiao, Li Xiaofeng. An insight into biomarkers of osteoarthritis synovium based on bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 785-790. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||