Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (30): 4767-4773.doi: 10.12307/2021.259
Previous Articles Next Articles
Effects of internal fixation types and osteoporosis on oblique lateral interbody fusion: three-dimensional finite element analysis
Qin Yichuan1, 2, Zhao Bin1, Yuan Jie1, Xu Chaojian1, Lü Jie1, 2, Hao Jiaqi1, 2, Wang Yongfeng1
- 1Department of Orthopedics, Second Hospital of Shanxi Medical University, Taiyuan 030001, Shanxi Province, China; 2Shanxi Medical University, Taiyuan 030001, Shanxi Province, China
-
Received:2021-01-04Revised:2021-01-06Accepted:2021-02-18Online:2021-10-28Published:2021-07-29 -
Contact:Wang Yongfeng, MD, Chief physician, Master’s supervisor, Department of Orthopedics, Second Hospital of Shanxi Medical University, Taiyuan 030001, Shanxi Province, China -
About author:Qin Yichuan, Master candidate, Department of Orthopedics, Second Hospital of Shanxi Medical University, Taiyuan 030001, Shanxi Province, China; Shanxi Medical University, Taiyuan 030001, Shanxi Province, China -
Supported by:Natural Science Foundation of Shanxi Province, No. 201801D121220 (to WYF)
CLC Number:
Cite this article
Qin Yichuan, Zhao Bin, Yuan Jie, Xu Chaojian, Lü Jie Hao Jiaqi Wang Yongfeng. Effects of internal fixation types and osteoporosis on oblique lateral interbody fusion: three-dimensional finite element analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4767-4773.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
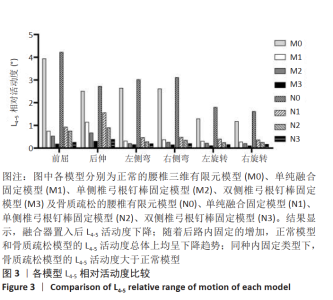
2.2 各运动状态下L4-L5节段腰椎相对活动度 随着后路内固定的增加,手术节段的活动度总体上呈下降趋势。正常模型中,相比M0,M1模型的L4-5活动度在各运动状态下均明显下降,最大降低了87.85%,为左侧弯时;M2的L4-5活动度在M1的基础上再次减小,后伸时减少最多,为40.01%;M3的L4-5活动度相比M2进一步下降,最多为前屈时的64.56%。骨质疏松模型中的情况类似,相比N0,N1的L4-5活动度均下降,最大降幅为左侧弯时的84.41%;相比于N1,N2的L4-5活动度在各运动状态均下降,在后伸时出现最大降幅,为42.10%;与N2比较,N3的L4-5活动度均降低,前屈时同样出现最大降幅,为64.78%(图3)。 同种后路内固定下,骨质疏松模型的L4-5活动度均比正常模型大;N1相比M1最大升高了46.58%,N2相比M2最大升高了41.19%,N3相比M3最大升高了55.36%(图3)。 "
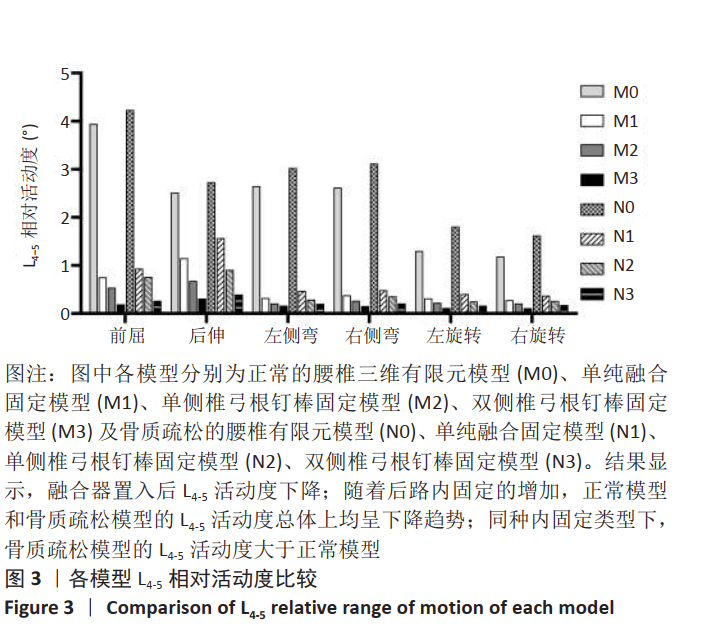
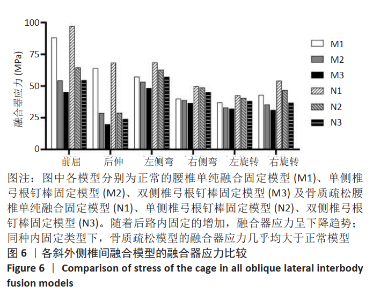
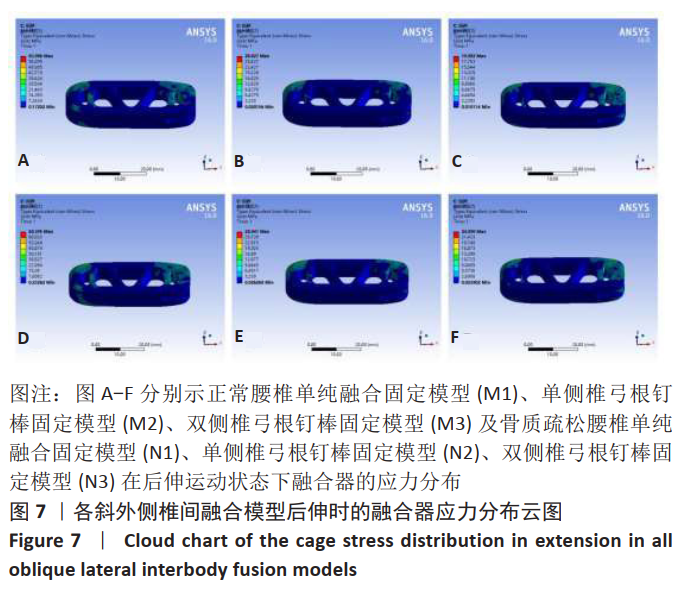
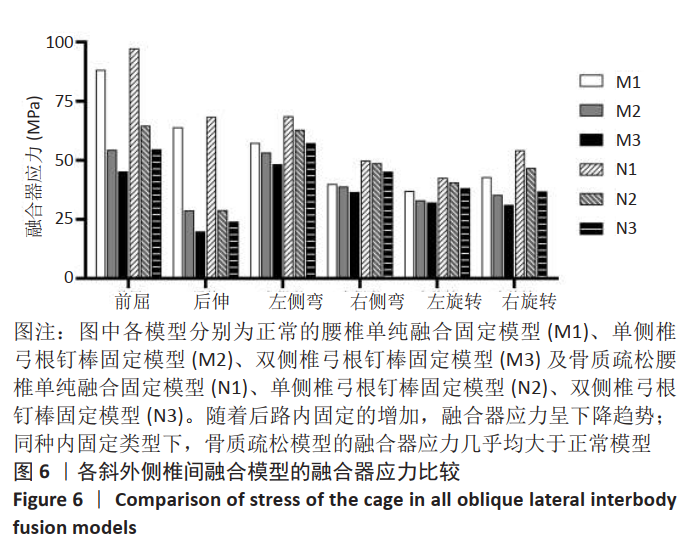
2.4 各运动状态下融合器应力峰值 随着后路内固定的增加,融合器应力呈现下降趋势。正常模型中,M2融合器的应力峰值相比于M1在各种运动状态下均明显减小,其中后伸时降幅达到了54.95%,前屈时降幅为38.30%;与M2相比,M3融合器的应力峰值在各种运动状态下均减小,尤以前屈及后伸为甚,其中后伸时降幅达到了30.68%,前屈时降幅为16.83%。骨质疏松模型中,N2相比于N1在各种运动状态下的融合器应力峰值均减小,在后伸时降幅最大,为57.69%,前屈状态下为33.56%;与N2相比,N3在各种运动状态下的融合器应力峰值均减小,在右旋转时降幅最大,为21.09%,后伸时为16.73%,见图6。"
| [1] SCHIZAS C, KULIK G, KOSMOPOULOS V. Disc degeneration: current surgical options. Eur Cell Mater. 2010;20:306-315. [2] PALEPU V, HELGESON M, MOLYNEAUX-FRANCIS M, et al. The effects of bone microstructure on subsidence risk for ALIF, LLIF, PLIF, and TLIF spine cages [published online ahead of print, 2018 dec 5]. J Biomech Eng. 2018;10.1115/1.4042181. [3] KUNZE B, DRASSECK T, KLUBA T. Posteriore und transforaminale lumbale interkorporelle Fusion (PLIF/TLIF) zur Therapie des lokalisierten Segmentaufbrauchs der LWS [Posterior and transforaminal lumbar interbody fusion (PLIF/TLIF) for the treatment of localised segment degeneration of lumbar spine. Z Orthop Unfall. 2011;149(3):312-316. [4] HEY HW, HEE HT. Lumbar degenerative spinal deformity: Surgical options of PLIF, TLIF and MI-TLIF. Indian J Orthop. 2010;44(2):159-162. [5] WANG HW, HU YC, WU ZY, et al. Minimally Invasive Transforaminal Lumbar Interbody Fusion and Unilateral Fixation for Degenerative Lumbar Disease. Orthop Surg. 2017; 9(3):277-283. [6] MOBBS RJ, PHAN K, MALHAM G, et al. Lumbar interbody fusion: techniques, indications and comparison of interbody fusion options including PLIF, TLIF, MI-TLIF, OLIF/ATP, LLIF and ALIF. J Spine Surg. 2015;1(1):2-18. [7] SILVESTRE C, MAC-THIONG JM, HILMI R, et al. Complications and Morbidities of Mini-open Anterior Retroperitoneal Lumbar Interbody Fusion: Oblique Lumbar Interbody Fusion in 179 Patients. Asian Spine J. 2012;6(2):89-97. [8] MEHREN C, MAYER HM, ZANDANELL C, et al. The Oblique Anterolateral Approach to the Lumbar Spine Provides Access to the Lumbar Spine With Few Early Complications. Clin Orthop Relat Res. 2016;474(9):2020-2027. [9] KIM MC, CHUNG HT, CHO JL, et al. Subsidence of polyetheretherketone cage after minimally invasive transforaminal lumbar interbody fusion. J Spinal Disord Tech. 2013;26(2):87-92. [10] OH KW, LEE JH, LEE JH, et al. The Correlation Between Cage Subsidence, Bone Mineral Density, and Clinical Results in Posterior Lumbar Interbody Fusion. Clin Spine Surg. 2017;30(6):E683-E689. [11] HE W, HE D, SUN Y, et al. Standalone oblique lateral interbody fusion vs. combined with percutaneous pedicle screw in spondylolisthesis. BMC Musculoskelet Disord. 2020;21(1):184. [12] LE TV, BAAJ AA, DAKWAR E, et al. Subsidence of polyetheretherketone intervertebral cages in minimally invasive lateral retroperitoneal transpsoas lumbar interbody fusion. Spine (Phila Pa 1976). 2012;37(14):1268-1273. [13] JOSEPH JR, SMITH BW, LA MARCA F, et al. Comparison of complication rates of minimally invasive transforaminal lumbar interbody fusion and lateral lumbar interbody fusion: a systematic review of the literature. Neurosurg Focus. 2015;39(4):E4. [14] POLIKEIT A, NOLTE LP, FERGUSON SJ. The effect of cement augmentation on the load transfer in an osteoporotic functional spinal unit: finite-element analysis. Spine (Phila Pa 1976). 2003;28(10):991-996. [15] KIM HJ, KANG KT, CHANG BS, et al. Biomechanical analysis of fusion segment rigidity upon stress at both the fusion and adjacent segments: a comparison between unilateral and bilateral pedicle screw fixation. Yonsei Med J. 2014;55(5):1386-1394. [16] LU T, LU Y. Comparison of Biomechanical Performance Among Posterolateral Fusion and Transforaminal, Extreme, and Oblique Lumbar Interbody Fusion: A Finite Element Analysis. World Neurosurg. 2019;129:e890-e899. [17] SHIM CS, PARK SW, LEE SH, et al. Biomechanical evaluation of an interspinous stabilizing device, Locker. Spine (Phila Pa 1976).2008;33(22):E820-E827. [18] DREISCHARF M, ZANDER T, SHIRAZI-ADL A, et al. Comparison of eight published static finite element models of the intact lumbar spine: predictive power of models improves when combined together. J Biomech. 2014;47(8):1757-1766. [19] OHTORI S, ORITA S, YAMAUCHI K, et al. Mini-Open Anterior Retroperitoneal Lumbar Interbody Fusion:Oblique Lateral Interbody Fusion for Lumbar Spinal Degeneration Disease. Yonsei Med J. 2015;56(4):1051-1059. [20] MALHAM GM, PARKER RM, BLECHER CM, et al. Assessment and classification of subsidence after lateral interbody fusion using serial computed tomography. J Neurosurg Spine. 2015;23(5):589-597. [21] MARCHI L, ABDALA N, OLIVEIRA L, et al. Radiographic and clinical evaluation of cage subsidence after stand-alone lateral interbody fusion. J Neurosurg Spine. 2013;19(1):110-118. [22] SHASTI M, KOENIG SJ, NASH AB, et al. Biomechanical evaluation of lumbar lateral interbody fusion for the treatment of adjacent segment disease. Spine J. 2019;19(3):545-551. [23] RITZEL H, AMLING M, PÖSL M, et al. The thickness of human vertebral cortical bone and its changes in aging and osteoporosis: a histomorphometric analysis of the complete spinal column from thirty-seven autopsy specimens. J Bone Miner Res. 1997;12(1):89-95. [24] GIBSON LJ, ASHBY MF. Cellular solids: structure and properties. Cambridge University Press, 1997. [25] LIU X, MA J, PARK P, et al. Biomechanical comparison of multilevel lateral interbody fusion with and without supplementary instrumentation: a three-dimensional finite element study. BMC Musculoskelet Disord. 2017;18(1):63. [26] CAO Y, LIU F, WAN S, et al. Biomechanical evaluation of different surgical procedures in single-level transforaminal lumbar interbody fusion in vitro. Clin Biomech(Bristol, Avon). 2017;49:91-95. [27] QUILLO-OLVERA J, LIN GX, JO HJ, et al. Complications on minimally invasive oblique lumbar interbody fusion at L2-L5 levels: a review of the literature and surgical strategies. Ann Transl Med. 2018;6(6):101. [28] XU DS, WALKER CT, GODZIK J, et al. Minimally invasive anterior, lateral, and oblique lumbar interbody fusion: a literature review. Ann Transl Med. 2018;6(6):104. [29] MCLAIN RF, FRY MF, MOSELEY TA, et al. Lumbar pedicle screw salvage: pullout testing of three different pedicle screw designs. J Spinal Disord. 1995;8(1):62-68. [30] CHIBA M, MCLAIN RF, YERBY SA, et al. Short-segment pedicle instrumentation. Biomechanical analysis of supplemental hook fixation. Spine (Phila Pa 1976). 1996; 21(3):288-294. [31] WEN J, SHI C, YU L, et al. Unilateral Versus Bilateral Percutaneous Pedicle Screw Fixation in Oblique Lumbar Interbody Fusion. World Neurosurg. 2020;134:e920-e927. [32] 殷飞,马荣,蔡则成, 等.斜外侧椎间融合联合单侧椎弓根钉棒固定术的三维有限元分析[J].中国脊柱脊髓杂志,2019,29(8):732-740. [33] DUBOUSSET J. Early failure of short-segment pedicle instrumentation for thoracolumbar fractures. A preliminary report. J Bone Joint Surg Am. 1995;77(4):648-649. [34] DAVNE SH, MYERS DL. Complications of lumbar spinal fusion with transpedicular instrumentation. Spine (Phila Pa 1976). 1992;17(6 Suppl):S184-S189. [35] 陈志明,马华松,赵杰,等.腰椎单侧椎弓根螺钉固定的三维有限元分析[J].中国脊柱脊髓杂志,2010,20(8):684-688. [36] 严亚波,裴国献,桑宏勋,等.螺钉-骨抗拔出力试验有限元模型的建立与验证[J].中华创伤骨科杂志,2013,15(1):28-31. [37] HOU Y, LUO Z. A study on the structural properties of the lumbar endplate: histological structure, the effect of bone density, and spinal level. Spine (Phila Pa 1976). 2009;34(12):E427-E433. [38] LIN JF, IUNDUSI R, TARANTINO U. Intravertebral plate and cage system via lateral trajectory for lumbar interbody fusion-a novel combined device. Spine J. 2010;10:S86. [39] KIM JS, CHOI WS, SUNG JH. 314 Minimally invasive oblique lateral interbody fusion for L4-5: clinical outcomes and perioperative complications.Neurosurgery. 2016;63:190-191. [40] SATO J, OHTORI S, ORITA S, et al. Radiographic evaluation of indirect decompression of mini-open anterior retroperitoneal lumbar interbody fusion: oblique lateral interbody fusion for degenerated lumbar spondylolisthesis. Eur Spine J. 2017;26(3): 671-678. [41] FUJIBAYASHI S, HYNES RA, OTSUKI B, et al. Effect of indirect neural decompression through oblique lateral interbody fusion for degenerative lumbar disease. Spine (Phila Pa 1976). 2015;40(3):E175-E182. [42] 陈意磊,朱志海,王玉康,等.斜侧方椎间融合术与经椎间孔椎间融合术在腰椎退变性疾病中前凸矫正效果的对比研究[J].中华医学杂志,2018,98(25): 1990-1995. |
| [1] | Li Zhifei, Yang Yin, Chen Hualong, Liang Qinqiu, Zhong Yuanming, Zhang Yisheng. Finite element analysis of the correlation between tilt angle of titanium cage and postoperative subsidence of titanium cage after anterior subtotal cervical corpectomy, decompression and fusion [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1313-1319. |
| [2] | Ouyang Beiping, Ma Xiangyang, Luo Chunshan, Zou Xiaobao, Lu Tingsheng, Chen Qiling. Three-dimensional finite element analysis of a new horizontal screw-screw crosslink in posterior atlantoaxial internal fixation [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1320-1324. |
| [3] | Liang Cheng, Zhang Linqi, Wang Guan, Li Wen, Duan Ke, Li Zhong, Lu Xiaobo, Zhuo Naiqiang. Finite element and biomechanical analysis of different implants in repair for unilateral unstable pelvic posterior ring injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1336-1341. |
| [4] | Guo Sutong, Feng Dehong, Guo Yu, Wang Ling, Ding Yujian, Liu Yi, Qian Zhengying, Li Mingyang. Construction and finite element analysis of normal and osteoporotic hip models [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1342-1346. |
| [5] | Yang Junliang, Lu Tan, Xu Biao, Jiang Yaqiong, Wang Fucheng. Three-dimensional finite element analysis of effects of partial anterior cruciate ligament rupture on knee joint stress [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1347-1353. |
| [6] | Niu Hegang, Yang Kun, Zhang Jingjing, Yan Yizhu, Zhang Yinshun. Design of a new posterior atlas fracture reduction and internal fixation system [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1399-1402. |
| [7] | Wang Menghan, Qi Han, Zhang Yuan, Chen Yanzhi. Three kinds of 3D printed models assisted in treatment of Robinson type II B2 clavicle fracture [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1403-1408. |
| [8] | Zhang Xiaoyun, Liu Hua, Chai Yuan, Chen Feng, Zeng Hao, Gao Zhengang, Huang Yourong. Effect of Yishen Gushu Formula on bone metabolic markers and clinical efficacyn in patients with osteoporosis of kidney deficiency and blood stasis type [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1155-1160. |
| [9] | Dai Yuexing, Zheng Liqin, Wu Minhui, Li Zhihong, Li Shaobin, Zheng Desheng, Lin Ziling. Effect of vessel number on computational fluid dynamics in vascular networks [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1206-1210. |
| [10] | Xiaheida·Yilaerjiang, Nijiati·Tuerxun, Reyila·Kuerban, Baibujiafu·Yelisi, Chen Xin. Three-dimensional finite element analysis of the distribution pattern of stress in bone tissues with different characteristics [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1277-1282. |
| [11] | Wang Qiang, Li Shiyun, Xiong Ying, Li Tiantian. Biomechanical changes of the cervical spine in internal fixation with different anterior cervical interbody fusion systems [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 821-826. |
| [12] | Wei Yuanbiao, Lin Zhan, Chen Yanmei, Yang Tenghui, Zhao Xiao, Chen Yangsheng, Zhou Yanhui, Yang Minchao, Huang Feiqi. Finite element analysis of effects of sagittal cervical manipulation on intervertebral disc and facet joints [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 827-832. |
| [13] | Zhang Rui, Wang Kun, Shen Zicong, Mao Lu, Wu Xiaotao. Effects of endoscopic foraminoplasty and laminoplasty on biomechanical properties of intervertebral disc and isthmus [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 833-839. |
| [14] | Kang Zhijie, Cao Zhenhua, Xu Yangyang, Zhang Yunfeng, Jin Feng, Su Baoke, Wang Lidong, Tong Ling, Liu Qinghua, Fang Yuan, Sha Lirong, Liang Liang, Li Mengmeng, Du Yifei, Lin Lin, Wang Haiyan, Li Xiaohe, Li Zhijun. Finite element model establishment and stress analysis of lumbar-sacral intervertebral disc in ankylosing spondylitis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 840-846. |
| [15] | Zhang Min, Peng Jing, Zhang Qiang, Chen Dewang. Mechanical properties of L3/4 laminar decompression and intervertebral fusion in elderly osteoporosis patients analyzed by finite element method [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 847-851. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||