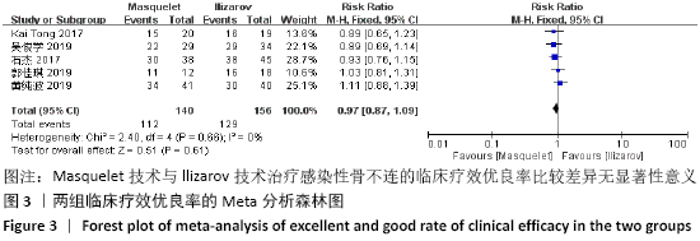
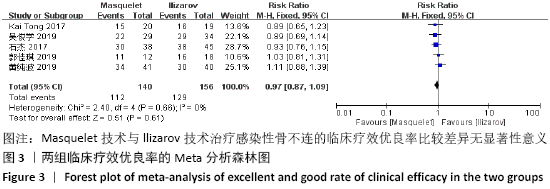
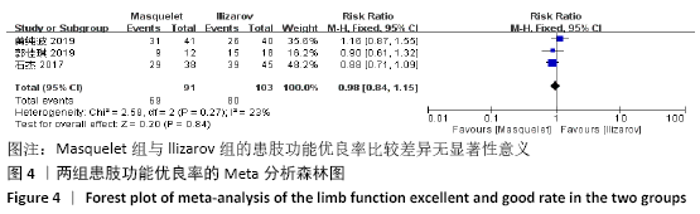
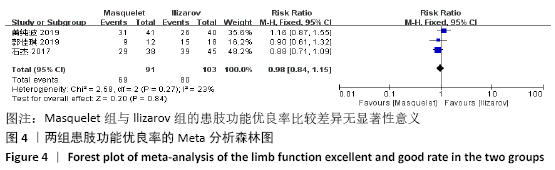
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (15): 2445-2452.doi: 10.3969/j.issn.2095-4344.3822
Previous Articles Next Articles
Masquelet technique in treatment of infectious nonunion: a meta-analysis
Xu Canhong1, Meng Lin2, Dong Panfeng1, Zhan Huasong1, Song Shilei1
- 1Ruikang Hospital, Guangxi University of Chinese Medicine, Nanning 530011, Guangxi Zhuang Autonomous Region, China; 2Guangxi Orthopedics Hospital, Nanning 530001, Guangxi Zhuang Autonomous Region, China
-
Received:2020-07-11Revised:2020-07-14Accepted:2020-08-13Online:2021-05-28Published:2021-01-05 -
Contact:Meng Lin, MD, Master’s supervisor, Associate chief physician, Guangxi Orthopedics Hospital, Nanning 530001, Guangxi Zhuang Autonomous Region, China -
About author:许灿宏,男,1995年生,广东省人,汉族,广西中医药大学在读硕士,主要从事骨与关节疾病及运动损伤研究。 -
Supported by:National Training Project for Innovative Talents of Traditional Chinese Medicine, No. Guo TCM Human Education Letter [2019] 128, (to ML); Guangxi Health Commission Medical Self-financing Scientific Research Project, No. Z20190482 (to DPF); the Graduate Education Innovation Program of Guangxi University of Chinese Medicine in 2019, No. YCSY201900106 (to XCH)
CLC Number:
Cite this article
Xu Canhong, Meng Lin, Dong Panfeng, Zhan Huasong, Song Shilei. Masquelet technique in treatment of infectious nonunion: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2445-2452.
share this article
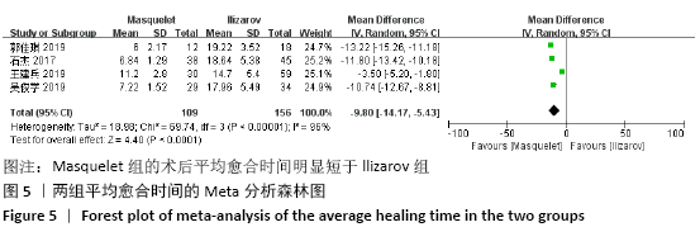
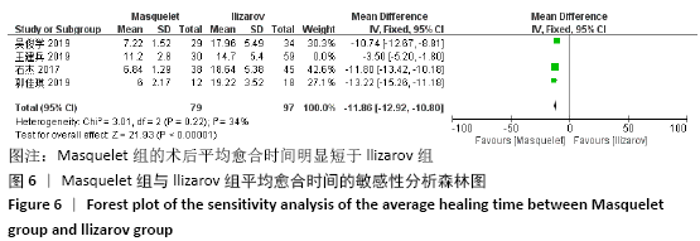
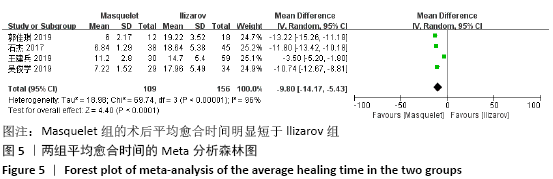
2.4.3 各组平均愈合时间的差异 有4项研究报道了术后平均愈合时 间[13,15,21-22],共包括265例患者,其中Masquelet组109例,Ilizarov组156例,异质性分析显示,各研究之间存在明显异质性(I2=96%,P < 0.000 01),故采用随机效应模型进行Meta分析。结果显示,Masquelet组的术后平均愈合时间明显短于Ilizarov组(MD=-9.80,95%CI:-14.17至-5.43,P < 0.000 01),见图5。进行敏感性分析发现,剔除王建兵等[13]的研究后异质性明显降低(I2=34%,P=0.22),但对结果无实质性改变,森林图方向也未发生变化,说明此Meta分析结果较可靠稳定(MD=-11.86,95%CI:-12.92至-10.80,P < 0.000 01),见图6。 "
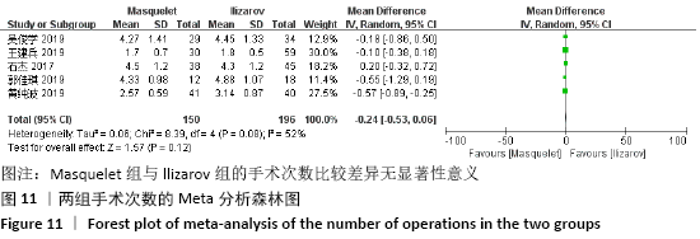
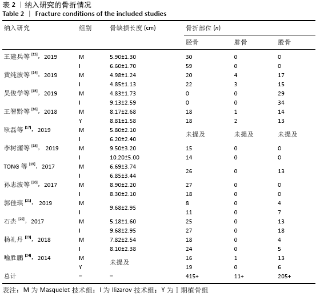
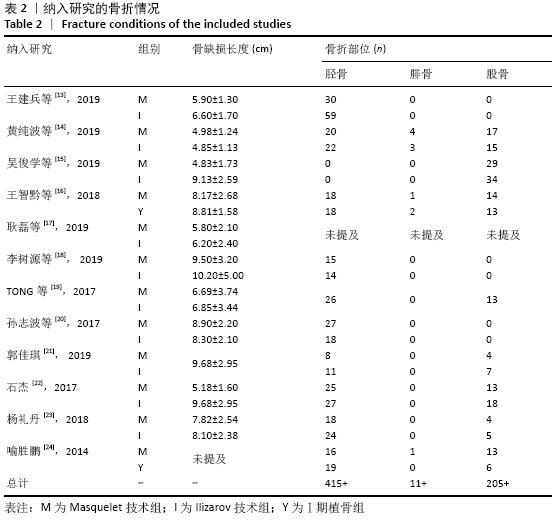
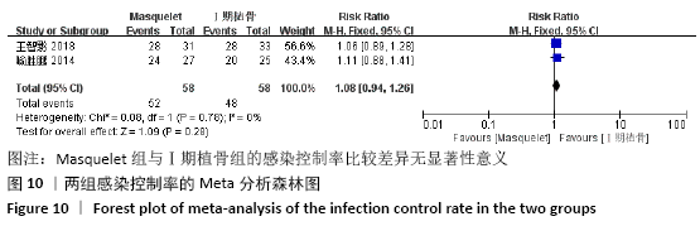
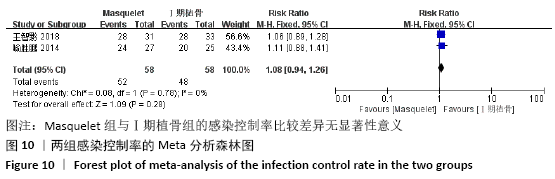
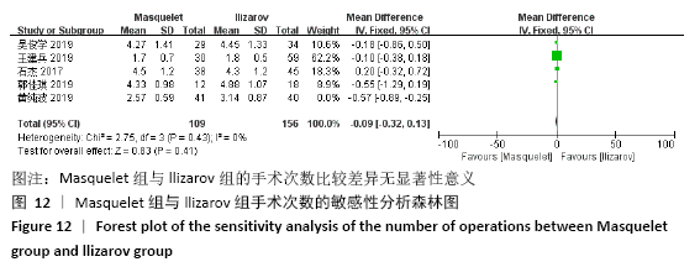
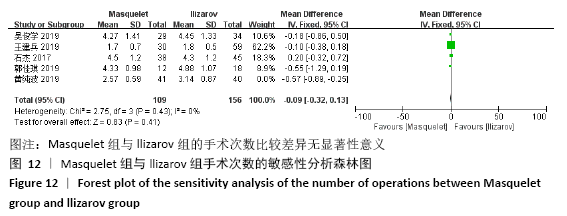
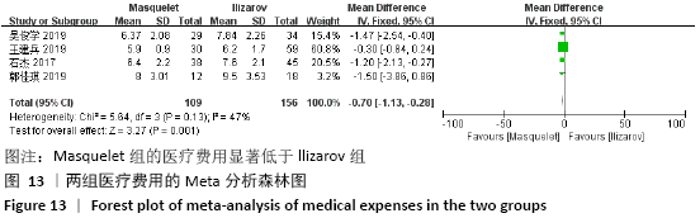
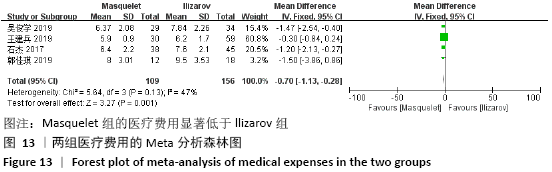
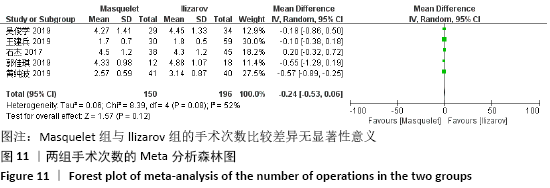
2.4.7 各组手术次数的差异 有5项研究报道了手术次数[13-15,21-22],共包括346例患者,其中Masquelet组150例,Ilizarov组196例,异质性分析显示,各研究之间存在明显异质性(I2=52%,P=0.08),故采用随机效应模型进行Meta分析。结果显示Masquelet组与Ilizarov组的手术次数比较差异无显著性意义(MD=-0.24,95%CI:-0.53-0.06,P=0.12),见图11。进行敏感性分析,发现剔除黄纯波[14]的研究后,异质性显著降低(I2=0%,P=0.43),但对结果无实质性改变,森林图方向亦未发生变化,说明此结果较稳定可靠(MD= -0.09,95%CI:-0.32-0.13,P=0.41),见图12。 "
| [1] TARNG YW, LIN KC. Management of bone defects due to infected non-union or chronic osteomyelitis with autologous non-vascularized free fibular grafts. Injury. 2020;51:294-300. [2] DHAR SA, DAR TA, MIR NA. Management of Infected Nonunion of the Forearm by the Masquelet Technique. Strategies Trauma Limb Reconstr. 2019;14:1-5. [3] MOTSITSI NS. Management of infected nonunion of long bones: the last decade (1996-2006). Injury. 2008;39:155-160. [4] KHANFOUR AA, EL-SAYED MM. Efficacy of a compliant semicircular Ilizarov pin fixator module for treating infected nonunion of the femoral diaphysis. Strategies Trauma Limb Reconstr. 2014;9:101-9. [5] STRUIJS PA, POOLMAN RW, BHANDARI M, et al. Infected Nonunion of the Long Bones. J Orthop Trauma. 2007;21(7):507-511. [6] SCHMAL H, BRIX M, BUE M, et al. Nonunion-consensus from the 4th annual meeting of the Danish Orthopaedic Trauma Society. EFORT Open Rev. 2020;5:46-57. [7] WANG J, YIN Q, GU S, et al. Induced membrane technique in the treatment of infectious bone defect: a clinical analysis. Orthop Traumatol Surg Res. 2019;105: 535-539. [8] MASQUELET AC, FITOUSSI F, BEGUE T, et al. Reconstruction of the long bones by the induced membrane and spongy autograft. Ann Chir Hast Esthet. 2000;45(3):346-353. [9] KONDA SR, GAGE M, FISHER N, et al. Segmental bone defect treated with the induced membrane technique. J Orthop Trauma. 2017;31:S21-S22. [10] Masquelet AC. Induced membrane technique: pearls and pitfaIls. J Orthop Trauma. 2017;31:S36-S38. [11] WALKER M, SHARAREH B, MITCHEIL SA. Masquelet Reconstruction for Posttraumatic Segmental Bone Defects in the Forearm. J Hand Surg Am. 2019;44:342.e1-342.e8. [12] GIANNOUDIS PV, HARWOOD PJ, TOSOUNIDIS T, et al. Restoration of long bone defects treated with the induced membrane technique: protocol and outcomes. Injury. 2016;47S6:S53-S61. [13] 王建兵,顾三军,周子红,等.骨搬运与诱导膜技术修复胫骨大段骨缺损的疗效比较[J].中华创伤骨科杂志, 2019,21(5): 398-404. [14] 黄纯波,夏先强,刘永峰.Masquelet和Ilizarov技术治疗感染性骨不连的临床效果比较[J].检验医学与临床,2019,16(4): 523-525. [15] 吴俊学,李毓灵,陈果.Ilizarov技术与Masquelet技术治疗股骨感染性骨不连的疗效[J].西部医学,2019,31(8):1237-1241. [16] 王智黔,张一,王远政,等.Masquelet技术与一期骨移植治疗感染性骨缺损的炎症控制效果比较[J].中国现代医学杂志, 2018,28(24):108-113. [17] 耿磊,程前勇,董志远.Masquelet术与Ilizarov骨搬移术治疗感染性骨缺损的疗效比较[J].中国骨与关节损伤杂志,2019, 34(10):1094-1096. [18] 李树源,周琦石,陈超,等.诱导膜技术与骨搬运技术治疗胫骨创伤性骨髓炎的疗效比较[J].中国中医骨伤科杂志,2019, 27(1):17-21. [19] TONG K, ZHONG Z, PENG Y, et al. Masquelet technique versus Ilizarov bone transport for reconstruction of lower extremity bone defects foIlowing posttraumatic osteomyelitis. Injury. 2017;48(7):1616-1622. [20] 孙志波,郭骏,陈荣,等.Masquelet技术与Ilizarov技术治疗成人胫骨慢性骨髓炎的早期临床疗效比较[J].骨科,2017,8(5): 349-353,359. [21] 郭佳琪.感染性骨不愈合中应用Masquelet技术与Ilizarov技术的疗效分析[D].太原:山西医科大学,2019. [22] 石杰.Ilizarov技术与Masquelet技术治疗感染性骨不连骨缺损的疗效分析[D].兰州:甘肃中医药大学,2017. [23] 杨礼丹.Masquelet与Ilizarov技术治疗成人下肢长骨慢性感染性骨缺损临床疗效分析[D].遵义:遵义医学院,2018. [24] 喻胜鹏.Masquelet技术与Ⅰ期骨移植治疗下肢创伤后骨髓炎的疗效比较[D].重庆:第三军医大学,2014. [25] TOTH Z, ROI M, EVANS E, et al. Masquelet technique: effects of spacer material and micro-topography on factor expression and bone regeneration. Ann Biomed Eng. 2019;47:174-189. [26] SASAKI G, WATANABE Y, MIYAMOTO W, et al. Induced membrane technique using beta-tricalcium phosphate for reconstruction of femoral and tibial segmental bone loss due to infection: technical tips and preliminary clinical results. Int Orthop. 2018;42:17-24. [27] SLIM K, NINI E, FORESTIER D, et al. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg. 2003;73:712-716. [28] LUCARELLI E, DONATI D, CENACCHI A, et al. Bone reconstruction of large defects using bone marrow derived autologous stem cells. Transfus Apher Sci. 2004;30(2): 169-174. [29] MA CH, CHIU YC, TU YK, et al. Three-stage treatment protocol for recalcitrant distal femoral nonunion. Arch Orthop Trauma Surg. 2017;137:489-498. [30] KOVOOR CC, JAYAKUMAR R, GEORGE V, et al. Vascularized fibular graft in infected tibial bone loss. Indian J Orthop. 2011;45: 330-335. [31] EL-HADIDI TT, SOLIMAN HM, FAROUK HA, et al. Staged bone grafting for the management of segmental long bone defects caused by trauma or infection using induced-membrane technique. Acta Orthop. Belg. 2018;84:384-396. [32] KHAN MS, RASHID H, UMER M, et al. Salvage of infected non-union of the tibia with an Ilizarov ring fixator. J Orthop Surg (Hong Kong). 2015;23:52-55. [33] WANG H, WEI X, LIU P, et al. Quality of life and complications at the different stages of bone transport for treatment infected nonunion of the tibia. Medicine (Baltimore). 2017;96:e8569. [34] YIN P, JI Q, LI T, et al. A systematic review and meta-analysis of ilizarov methods in the treatment of infected nonunion of tibia and femur. PLoS One. 2015;10:e0141973. [35] SIDDIQUI AA, SIDDIQUI F, BASHAR M, et al. Impact of ilizarov fixation technique on the limb functionality and self-esteem of patients with unilateral tibial fractures. Cureus. 2019;11:e5923. [36] YU YH, LEE D, HSU YH, et al. A Three-dimensional printed polycaprolactone scaffold combined with co-axially electrospun vancomycin/ceftazidime/bone morphological protein-2 sheath-core nanofibers for the repair of segmental bone defects during the masquelet procedure. Int J Nanomedicine. 2020;15:913-925. [37] BOSEMARK P , PERDIKOURI C , PELKONEN M, et al. The masquelet induced membrane technique with BMP and a synthetic scaffold can heal a rat femoral critical size defect. J Orthop Res. 2015;33(4):488-495. [38] GUPTA S, MALHOTRA A, JINDAL R, et al. Role of beta tri-calcium phosphate-based composite ceramic as bone-graft expander in masquelet’s-induced membrane technique. Indian J Orthop. 2019;53:63-69. [39] MI M, PAPAKOSTIDIS C, WU X, et al. Mixed results with the masquelet technique: a fact or a myth? Injury. 2020;51:132-135. [40] SIKARY AK, KUMAR M, DHAKA S, et al. A rare fatal complication of ilizarov procedure. J Forensic Sci. 2018;63:1895-1898. [41] MORELLI I, DRAGO L, GEORGE DA, et al. Masquelet technique: myth or reality? A systematic review and meta-analysis. Injury. 2016;47 Suppl 6:S68-S76. [42] YEGANEH A, MAHMODI M, FARAHINI H, et al. Short-term outcomes of induced membrane technique in treatment of long bone defects in Iran. Med Arch. 2016;70: 284-287. [43] WANG X, LUO F, HUANG K, et al. Induced membrane technique for the treatment of bone defects due to post-traumatic osteomyelitis. Bone Joint Res. 2016;5: 101-105. [44] SAXER F, ECKARDT H. Rekonstruktion ossärer defekte mit der masquelet-technik. Der Orthopäde. 2017;46(8):665-672. [45] AHO OM, LEHENKARI P, RISTINIEMI J, et al. The mechanism of action of induced membranes in bone repair. J Bone Joint Surg Am. 2013;95:597-604. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [5] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [6] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [7] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [8] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [9] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [10] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [11] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [12] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [13] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [14] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [15] | Liang Yan, Zhao Yongfei, Xu Shuai, Zhu Zhenqi, Wang Kaifeng, Liu Haiying, Mao Keya. Imaging evaluation of short-segment fixation and fusion for degenerative lumbar scoliosis assisted by highly selective nerve root block [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1423-1427. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||