Chinese Journal of Tissue Engineering Research ›› 2016, Vol. 20 ›› Issue (53): 8010-8021.doi: 10.3969/j.issn.2095-4344.2016.53.016
Previous Articles Next Articles
InterTan nail versus proximal femoral nail antirotation for femoral intertrochanteric fractures: a systematic review and meta-analysis
Hu Bing-yan1, Ai Jin-wei2, 3, Chen Qiong3, Yao Zhong-jun1
- 1Department of Hand, Foot, Microscopic Orthopedics, Taihe Hospital, Hubei University of Medicine, Shiyan 442000, Hubei Province, China; 2Department of Orthopedics, Xiangyang Hospital, Hubei University of Medicine, Xiangyang 441000, Hubei Province, China; 3Evidence-Based Medicine Center, Xiangyang Hospital, Hubei University of Medicine, Xiangyang 441000, Hubei Province, China
-
Revised:2016-10-31Online:2016-12-23Published:2016-12-23 -
Contact:Yao Zhong-jun, M.D., Chief physician, Professor, Department of Hand, Foot, Microscopic Orthopedics, Taihe Hospital, Hubei University of Medicine, Shiyan 442000, Hubei Province, China -
About author:Hu Bing-yan, Master, Attending physician, Department of Hand, Foot, Microscopic Orthopedics, Taihe Hospital, Hubei University of Medicine, Shiyan 442000, Hubei Province, China -
Supported by:the General Program of Health and Family Planning of Western Medicine in Hubei Province from 2015 to 2016, No. WJ2015MB187; the Key Project of Teaching and Research of Hubei University of Medicine, No. 2015025
CLC Number:
Cite this article
Hu Bing-yan, Ai Jin-wei, Chen Qiong, Yao Zhong-jun . InterTan nail versus proximal femoral nail antirotation for femoral intertrochanteric fractures: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2016, 20(53): 8010-8021.
share this article
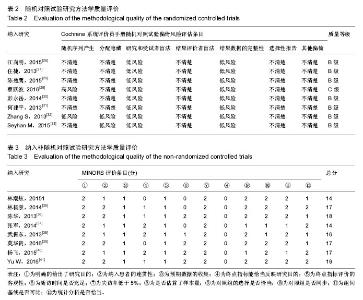
2.1 文献检索结果 各数据库初检出文献426篇,NoteExpress3.1软件排重后获文献216篇,经标题、摘要初筛获得可能纳入的文献45篇,再通过阅读全文复筛,最终纳入16个研究[26-41]。其中,随机对照试验8篇[26-33],非随机对照试验8篇[34-41];中文文献13篇[26-31,34-40], 英文文献3篇[32,33,41]。 2.2 纳入研究基本特征 纳入的16个临床对照试验涉及1 323例股骨转子间骨折患者。其中,InterTan钉组658例,PFNA组665例。各研究患者平均年龄均> 50岁,骨折分型方法包括改良Evans分型和AO分型。各研究均描述两组在患者年龄、性别、骨折分型、麻醉风险评估等方面差异无统计学意义(P > 0.05)。结局指标主要包括:治疗优良率、手术时间、术中出血量、下地活动时间(卧床时间)、骨折愈合时间、髋关节Harris评分、并发症率等。纳入研究基本特征见表1。 2.3 纳入研究方法质量学评价 纳入的8个随机临床对照试验方法学质量评价[26-33],见表2;8个非随机临床对照试验方法学质量评价[34-41],见表3,总体为中等质量研究。"


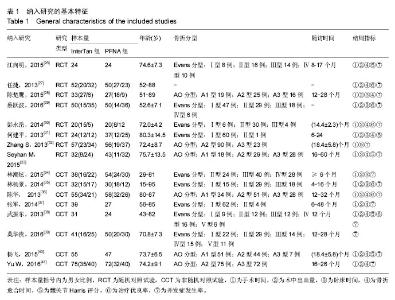
2.4 Meta分析结果 2.4.1 手术时间 15个研究报告了两组手术时间差 异[26-38,40-41],合计样本量1 236例,其中InterTan组617例,PFNA组619例。异质性检验显示研究间存在异质性(P < 0.01,I2=94.6%)。采用随机效应模型进行统计分析(图1),结果显示InterTan组手术时间长于PFNA组[MD=11.51,95%CI(6.41,16.62),P < 0.01]。按研究类型进行亚组分析,8个随机对照试验[26-33][MD=7.50,95%CI(0.10,14.62),P=0.04]和7个非随机对照试验 [MD=16.27,95%CI(9.09,23.45)[34-38,40-41],P < 0.01]合并结果均显示两治疗组在手术时间上有差异,亦说明InterTan手术时间长于PFNA组。 2.4.2 术中出血量 13个研究报告了两组术中出血量差异[26-31,34-38,40-41],合计样本量1 048例,其中InterTan组528例,PFNA组520例。异质性检验显示研究间存在异质性(P < 0.01,I2=98.2%),采用随机效应模型进行统计分析(图2),结果显示两组术中出血量比较差异无显著性意义[MD=6.06,95%CI(-20.91,33.02),P=0.66]。按研究类型进行亚组分析,6个随机对照试验[26-31] [MD=15.17,95%CI(-40.48,70.82),P=0.59]和7个非随机对照试验[34-38,40-41] [MD=1.95,95%CI(-19.49,23.39),P=0.86]合并结果均显示两治疗组在术中出血量上无明显差异。"

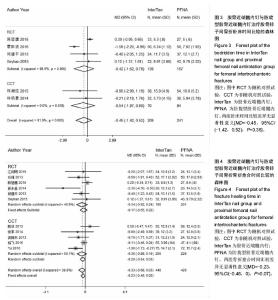
2.4.3 卧床时间 6个研究报告了两治疗组术后患者卧床时间[28-29,31,33-35],合计样本量450例,其中IinterTan组209例,PFNA组241例。异质性检验显示研究间存在异质性(P < 0.01,I2=81.9%)。采用随机效应模型进行统计分析(图3),结果显示两组卧床时间比较差异无显著性意义[MD=-0.45,95%CI(-1.42,0.52),P=0.36]。按研究类型进行亚组分析,4个随机对照试验[28-29,31,33] [MD=-0.42,95%CI(-1.62,0.78),P=0.50]和2个非随机对照试验[34-35] [MD=-0.54,95%CI(-1.97,0.90),P=0.46]合并结果均显示两治疗组在卧床时间上无明显差异。 2.4.4 骨折愈合时间 11个研究报告了两治疗组患者骨折愈合时间[26-28,30-31,33,36-38,40-41],合计样本量869例,其中IinterTan组440例,PFNA组429例。异质性检验显示研究间无明显异质性(P=0.12,I2=39.8%)。采用固定效应模型进行统计分析(图4),结果显示两组骨折愈合时间比较差异无显著性意义[MD=-0.23,95%CI(-0.46,0),P=0.07]。按研究类型进行亚组分析,6个随机对照试验[26-28,30-31,33][MD=-0.17,95%CI (-0.55,0.22),P=0.25]和5个非随机对照试验[36-38, 40-41] [MD=-0.36,95%CI(-0.88,0.16),P=0.18]合并结果均显示两组在骨折愈合时间上无明显差异。 "
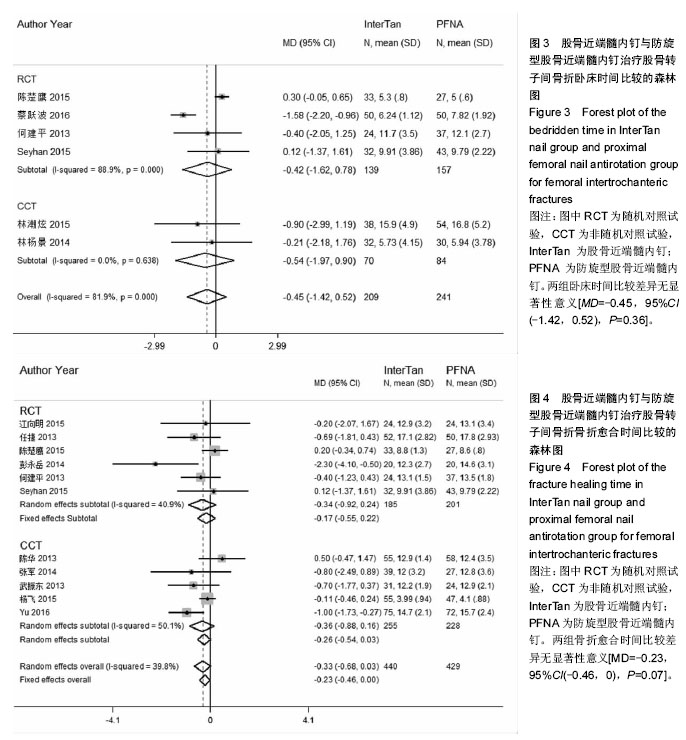

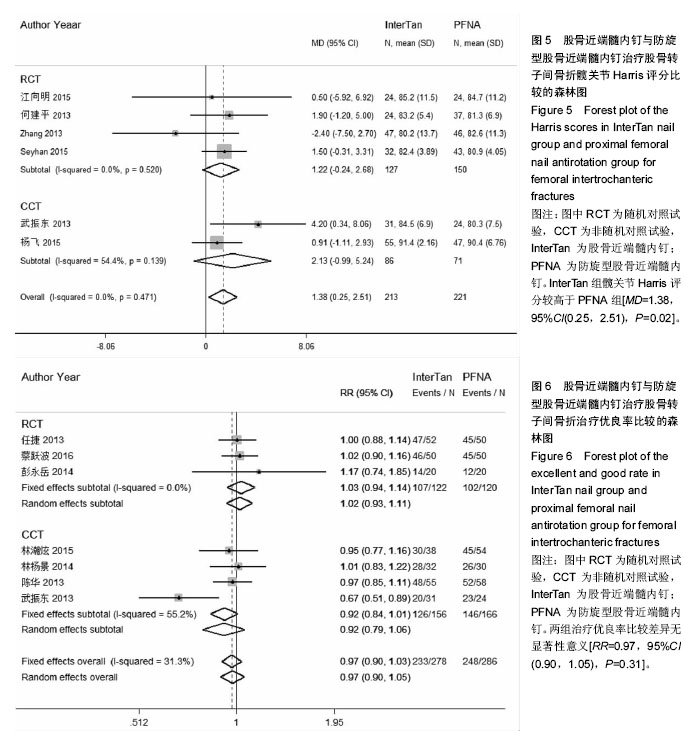
2.4.5 髋关节Harris评分 6个研究报告了两治疗组患者髋关节Harris评分[26,31-33,38,40],合计样本量434例,其中IinterTan组213例,PFNA组221例。异质性检验显示研究间无明显异质性(P=0.47,I2=0.0%)。采用固定效应模型进行统计分析(图5),结果显示InterTan组髋关节Harris评分高于PFNA组[MD=1.38,95%CI(0.25,2.51),P=0.02]。按研究类型进行亚组分析,4个随机对照试验[26,31-33] [MD=1.22,95%CI(-0.24,2.68),P=0.10]和2个非随机对照试验[38,40][MD=2.13,95%CI(-0.99,5.24), P=0.18]合并结果均显示两组髋关节Harris评分无明显差异。 2.4.6 治疗优良率 7个研究以髋关节Harris评分为评价标准[27,29-30,34-36,38],报告了两组治疗优良率,合计样本量564例,其中IinterTan组278例,PFNA组286例。异质性检验显示研究间无明显异质性(P=0.31,I2=31.3%)。采用固定效应模型进行统计分析(图6),结果显示两组治疗优良率比较差异无显著性意义[RR=0.97,95%CI(0.90,1.05),P=0.31]。按研究类型进行亚组分析,3个随机对照试验[27,29-30][RR=1.02,95%CI(0.93,1.11),P=0.53]和4个非随机对照试验[34-36,38][MD=0.92,95%CI(0.79,1.06),P=0.07]合并结果均显示两组治疗优良率无明显差异。"
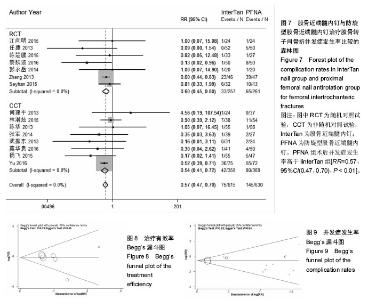
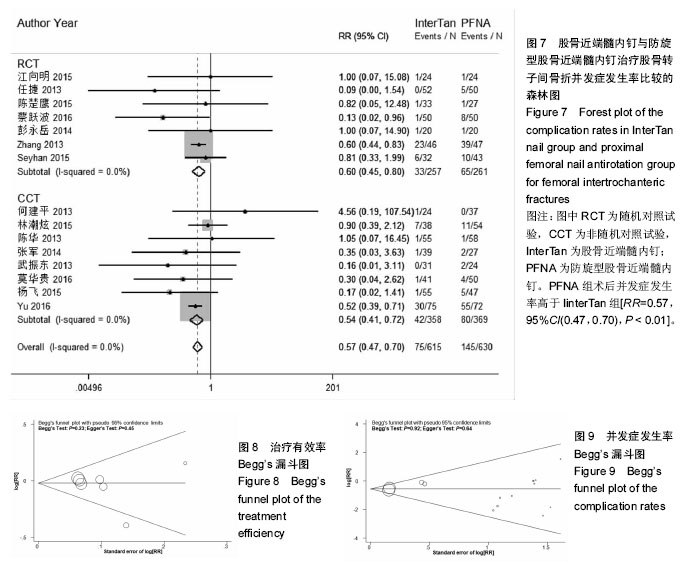
2.4.7 术后并发症发生率 15个研究报告了两组术后并发症发生率[26-30,32-41],合计样本量1 245例,其中IinterTan组615例,PFNA组630例。异质性检验显示研究间无明显异质性(P=0.70,I2=0.0%)。采用固定效应模型进行统计分析(图7),结果显示PFNA组术后并发症发生率较高于IinterTan组[RR=0.57,95%CI(0.47,0.70),P < 0.01]。按研究类型进行亚组分析,7个随机对照试验[26-30,32-33][RR=0.60,95%CI(0.45,0.80),P < 0.01]和8个非随机对照试验[34-41][MD=0.54,95%CI(0.41,0.72),P < 0.01]合并结果均显示PFNA组术后并发症发生率高于InterTan组。 2.5 发表偏倚 对各结局指标分析绘制Begg’s漏斗图识别发表偏倚,各漏斗图基本对称,说明本研究存在发表偏倚可能性小。以治疗优良率和并发症发生率为例显示漏斗图,见图8,9。"
| [1] Fernandez M,Griffin X,Costa M.Hip fracture surgery: improving the quality of the evidence base. Bone Joint J.2015;97(7):875-879.[2] Florschutz A,Langford J,Haidukewych G,et al.Femoral neck fractures: current management.J Orthop Trauma. 2015;29(3):121-129.[3] Roberts K,Brox W,Jevsevar D,et al.Management of hip fractures in the elderly. J Am Acad Orthop Surg.2015; 23(2):131-137.[4] Sprague S,Slobogean G,Scott T,et al.Young femoral neck fractures: are we measuring outcomes that matter? Injury.2015;46(3):507-514.[5] 贾励军,刘强.老年股骨转子间骨折的治疗进展[J].广西医学,2014,16(9):110-112.[6] Bajpai J,Maheshwari R,Bajpai A,et al.Treatment options for unstable trochanteric fractures: Screw or helical proxima femoral nail.Chin J Traumatol.2015; 18(6):342-346.[7] Roberts K,Brox W.AAOS Clinical Practice Guideline: Management of Hip Fractures in the Elderly.J Am Acad Orthop Surg.2015;23(2):138-140.[8] Davidovitch R,Jordan C,Egol K,et al.Challenges in the treatment of femoral neck fractures in the nonelderly adult.J Trauma.2010;68(1):236-242.[9] Butler M,Forte M,Joglekar S,et al.Evidence summary: systematic review of surgical treatments for geriatric hip fractures.J Bone Joint Surg Am.2011;93(12): 1104-1115.[10] Kaplan K,Miyamoto R,Levine B,et al.Surgical management of hip fractures: an evidence-based review of the literature. II: intertrochanteric fractures.J Am Acad Orthop Surg.2008;16(11): 665-673.[11] Kazemian G,Manafi A,Najafi F,et al.Treatment of intertrochanteric fractures in elderly highrisk patients: dynamic hip screw vs. external fixation.Injury. 2014; 45(3): 568-572.[12] Parker M,Handoll H.Gamma and other cephalocondylic intramedullary nails versus extramedullary implants for extracapsular hip fractures in adults. Cochrane Database Syst Rev.2010;2010(9): D93.[13] 李意,李新志.股骨粗隆间骨折内固定手术治疗的研究进展[J].重庆医学,2013,42(10): 1172-1175.[14] Shen L,Zhang Y,Shen Y,et al.Antirotation proximal femoral nail versus dynamic hip screw for intertrochanteric fractures: a meta-analysis of randomized controlled studies. Orthop Traumatol Surg Res.2013;99(4):377-383.[15] Evaniew N,Bhandari M.Cochrane in CORR (R): Intramedullary nails for extracapsular hip fractures in adults (review).Clin Orthop Relat Res.2015;473(3): 674-767.[16] Queally J,Harris E,Handoll H,et al.Intramedullary nails for extracapsular hip fractures in adults (review).Cochrane Database Syst Rev.2014;2014(9): D4961.[17] 张伟强,祁宝昌,邓鹏飞,等.老年股骨粗隆间骨折治疗的临床进展[J].中国老年学杂志,2015;35(1): 266-268.[18] 张晓东,杨广忠.高龄股骨粗隆间骨折的治疗进展[J].中国骨与关节损伤杂志, 2012,43(3):282-285.[19] 何小鹏,张亚斌,王小春.股骨粗隆间骨折的临床手术治疗进展[J].航空航天医学杂志, 2013,24(7):843-853.[20] 李永奖,张力成,杨国敬,等.高龄患者股骨粗隆间骨折治疗进展[J].浙江创伤外科, 2014,30(6):875-876.[21] 刘存欢,张建华.股骨转子间骨折治疗的研究进展[J].中医药临床杂志,2015,27(11): 1627-1630.[22] 魏建仝,张钟,苏秦柳晔,等.股骨粗隆间骨折髓内内固定治疗进展[J].生物骨科材料与临床研究,2015,12(3):67-69.[23] Moher D,Liberati A,Tetzlaff J,et al.Reprint--preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement.Phys Ther. 2009;89(9): 873-880.[24] Zeng X,Zhang Y,Kwong J,et al.The methodological quality assessment tools for preclinical and clinical studies, systematic review and meta-analysis, and clinical practice guideline: a systematic review.J Evid Based Med.2015;8(1):2-10.[25] 曾宪涛,庄丽萍,杨宗国,等.Meta分析系列之七:非随机实验性研究、诊断性试验及动物实验的质量评价工具[J].中国循证心血管医学杂志,2012,4(6):496-499.[26] 江向明,刘文国.InterTan与PFNA治疗老年人股骨转子间骨折的疗效分析[J].华南国防医学杂志,2015,29(10): 754-757.[27] 任捷,尹昆.PFNA和InterTan方法治疗老年股骨粗隆间骨折的疗效分析[J].中国医学创新, 2013,10(23):6-8.[28] 陈楚鹰,何永盛.应用InterTan与PFNA治疗老年患者股骨粗隆间骨折疗效分析[J].中国继续医学教育,2015,7(18): 137-139.[29] 蔡跃波.InterTan髓内钉内固定治疗股骨粗隆间骨折的临床观察[J].中国医学创新. 2016,13(5):132-135.[30] 彭永岳,黄燕峰,孙华. InterTAN钉与股骨近端防旋髓内钉治疗不稳定股骨转子间骨折的临床疗效[J].上海医学, 2014, 37(11):927-930.[31] 何建平,张树明,乔林,等.老年骨质疏松股骨粗隆间骨折髓内固定选择对比研究[J].中国骨质疏松杂志,2013,19(3): 268-270.[32] Zhang S,Zhang K,Jia Y,et al.InterTan Nail Versus Proximal Femoral Nail Antirotation-Asia in the Treatment of Unstable Trochanteric Fractures. Orthopedics. 2013;36(3):e182-e292.[33] Seyhan M,Turkmen I,Unay K,et al.Do PFNA devices and Intertan nails both have the same effects in the treatment of trochanteric fractures? A prospective clinical study. J Orthop Sci.2015;20(6):1053-1061.[34] 林潮炫,牛维,孙志涛,等.两种不同髓内固定治疗股骨转子骨折的疗效比较[J].临床骨科杂志,2015,18(4):452-454.[35] 林杨景,李杰,林炎水,等. InterTAN、PFNA和DHS治疗股骨转子间骨折的疗效比较[J].暨南大学学报(自然科学与医学版),2014,5(3):294-298.[36] 陈华,尹云生,陈越,等. DHS、PFNA和INTERTAN钉治疗老年股骨粗隆间骨折的疗效分析[J].中国医药指南,2013, 11(35):405-406.[37] 张军,武永刚,陈炜.InterTan和PFNA内固定治疗股骨粗隆间骨折的疗效分析[J].中国骨与关节损伤杂志,2014, 29(8): 817-818.[38] 武振东,王超,朱东,等.InterTan系统与防旋型股骨近端髓内钉治疗老年人股骨粗隆间骨折的临床疗效评价[J].中国老年学杂志,2013,33(3):497-500.[39] 莫华贵,黄远翘,陈元庄,等.三种髓内固定技术治疗老年股骨粗隆间骨折对患者股骨头旋转与固定钉滑脱的影响[J].海南医学,2016,27(6):920-923.[40] 杨飞,韩启明,杨凤明,等.老年股骨粗隆间骨折微创INTERTAN髓内钉与PFNA-Ⅱ髓内钉临床疗效分析[J].中国矫形外科杂志,2015,23(10):897-901.[41] Yu W,Zhang X,Zhu X,et al.A retrospective analysis of the InterTan nail and proximal femoral nail anti-rotation-Asia in the treatment of unstable intertrochanteric femur fractures in the elderly.J Orthop Surg Res.2016;11:10. [42] Huang H,Xin J,Ma B.Analysis of complications of intertrochanteric fracture treated with Gamma 3 intramedullary nail.Int J Clin Exp Med.2014;7(10): 3687-3693.[43] Nyholm A, Palm H, Malchau H, et al. Lacking evidence for performance of implants used for proximal femoral fractures-A systematic review. Injury. 2016;47(3): 586-594.[44] Pascarella R,Fantasia R,Maresca A,et al.How evolution of the nailing system improves results and reduces orthopedic complications: more than 2000 cases of trochanteric fractures treated with the Gamma Nail System.Musculoskelet Surg. 2016;100(1):1-8.[45] Voleti P,Liu S,Baldwin K,et al.Intertrochanteric Femur Fracture Stability: A Surrogate for General Health in Elderly Patients? Geriatr Orthop Surg Rehabil. 2015; 6(3):192-196.[46] Rahimzadeh P,Imani F,Faiz S,et al.Effect of intravenous methylprednisolone on pain after intertrochanteric femoral fracture surgery.J Clin Diagn Res.2014;8(4):1-4.[47] Lee Y,Chung C,Park M,et al.Intramedullary nail versus extramedullary plate fixation for unstable intertrochanteric fractures: decision analysis. Arch Orthop Trauma Surg.2013;133(7):961-968.[48] Lal H,Sharma D,Mittal D.Intrapelvic migration of hip lag screw of proximal femoral nail-sequele to a paradoxical reverse Z effect and their critical analysis. J Clin Orthop Trauma.2012;3(1):48-53. |
| [1] | Shi Bin, An Jing, Chen Long-gang, Zhang Nan, Tian Ye . Influencing factors for pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 993-997. |
| [2] | Wang Xian-xun. Impact of local compression cryotherapy combined with continuous passive motion on the early functional recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 998-1003. |
| [3] | Yuan Wei, Zhao Hui, Ding Zhe-ru, Wu Yu-li, Wu Hai-shan, Qian Qi-rong. Association between psychological resilience and acute mental disorders after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1015-1019. |
| [4] | Chen Qun-qun, Qiao Rong-qin, Duan Rui-qi, Hu Nian-hong, Li Zhao, Shao Min. Acu-Loc®2 volar distal radius bone plate system for repairing type C fracture of distal radius [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1025-1030. |
| [5] | Huang Xiang-wang, Liu Hong-zhe. A new low elastic modulus of beta titanium alloy Ti2448 spinal pedicle screw fixation affects thoracic stability: biomechanical analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1031-1035. |
| [6] | Xie Qiang. Three-dimensional finite element model for biomechanical analysis of stress in knee inversion and external rotation after posterior cruciate ligament rupture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1036-1040. |
| [7] | He Ze-dong, Zhao Jing, Chen Liang-yu, Li Ke, Weng Jie. Multilevel finite element analysis on the biological tribology damage of water on bone tissue [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1041-1045. |
| [8] | Jiang Zi-wei, Huang Feng, Cheng Si-yuan, Zheng Xiao-hui, Sun Shi-dong, Zhao Jing-tao, Cong Hai-chen,Sun Han-qiao, Dong Hang. Design and finite element analysis of digital splint [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1052-1056. |
| [9] | Wang Fei, Liu Zhi-bin, Tao Hui-ren, Zhang Jian-hua, Li Chang-hong, Cao Qiang, Zheng Jun, Liu Yan-xiong, Qu Xiao-peng. Clinical efficacy of preoperative osteotomy designs using paper-cut technology versus photoshop software for ankylosing spondylitis with kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1057-1063. |
| [10] | Li Hui, Ma Jun-yi, Ma Yuan, Zhu Xu . Establishment of a three-dimensional finite element model of ankylosing spondylitis kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1069-1073. |
| [11] | Ling Guan-han, Ou Zhi-xue, Yao Lan, Wen Li-chun, Wang Guo-xiang, Lin Heng-feng. Establishment of simulating three-dimensional model of China-Japan Friendship Hospital Classification for L type osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1074-1079. |
| [12] | Fu Wei-min, Wang Ben-jie. Assessing the degree of necrotic femoral head, and association of blood supply with pathlogical changes: study protocol for a diagnostic animal trial [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1086-1091. |
| [13] | Zhang Wen-qiang, Ding Qian, Zhang Na. Associations between alpha angle and herniation pit on oblique axial magnetic resonance imaging in asymptomatic hip joints of adults [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1098-1103. |
| [14] | Sun Xiao-xin1, Zhou Wei2, Zuo Shu-ping3, Liu Hao1, Song Jing-feng1, Liang Chun-yu1. Morphological characteristics for the magnetic resonance imaging assessment of discoid lateral meniscal tears in children [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1104-1109. |
| [15] | Lin Han-wen, Wen Jun-mao, Huang Chao-yuan, Zhou Chi, Tang Hong-yu. Correlation between the changes in lower limb power line and pain area in the knee osteoarthritis patients: imaging evaluation [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1110-1114. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||