Chinese Journal of Tissue Engineering Research ›› 2016, Vol. 20 ›› Issue (35): 5216-5223.doi: 10.3969/j.issn.2095-4344.2016.35.007
Previous Articles Next Articles
Adjacent segment degeneration after anterior cervical corpectomy and fusion
Zhai Peng-fei1, Liu Wei1, Sun Zhi-ming1, Zhang Xue-li2
- 1Department of Neurosurgery and Spine Surgery, Tianjin Huanhu Hospital, Tianjin 300350, China; 2Department of Spine Surgery, Tianjin People’s Hospital, Tianjin 300121, China
-
Revised:2016-06-12Online:2016-08-26Published:2016-08-26 -
Contact:Zhang Xue-li, Professor, Master’s supervisor, Department of Spine Surgery, Tianjin People’s Hospital, Tianjin 300121, China -
About author:Zhai Peng-fei, Master, Physician, Department of Neurosurgery and Spine Surgery, Tianjin Huanhu Hospital, Tianjin 300350, China
CLC Number:
Cite this article
Zhai Peng-fei, Liu Wei, Sun Zhi-ming, Zhang Xue-li. Adjacent segment degeneration after anterior cervical corpectomy and fusion[J]. Chinese Journal of Tissue Engineering Research, 2016, 20(35): 5216-5223.
share this article
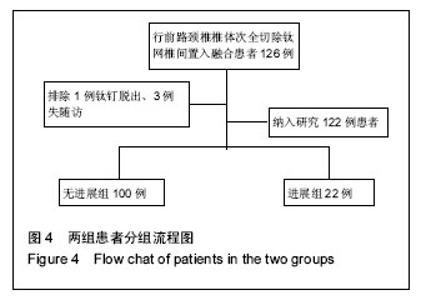
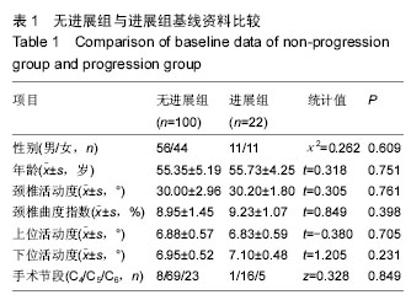
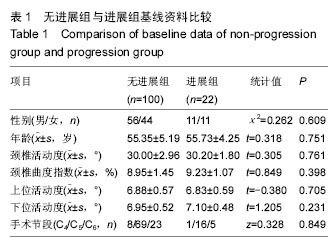
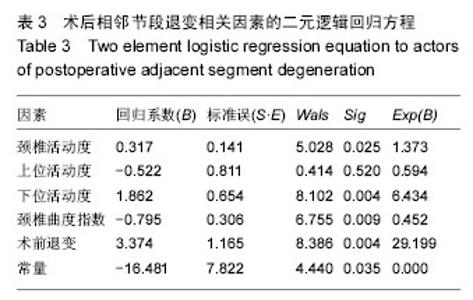
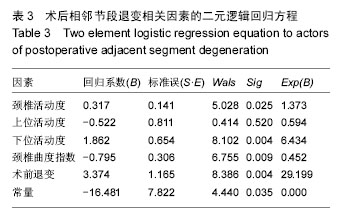
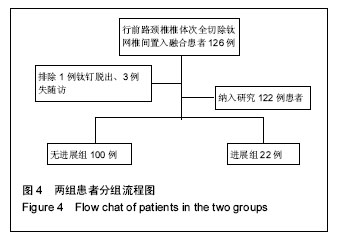
2.1 参与者数量分析 纳入行经前路椎体次全切钛网置入植骨融合术的126例颈椎病患者中,因钛钉脱出,行二次手术去除钢板1例,失访3例,共122例患者获完整随访资料,均获得融合。病例包含男性67例,年龄(55.72±5.17)岁;女性55例,年龄(55.05±4.85)岁。随访时间为3年。 2.2 患者一般情况 术中共涉及122个椎体及244个间盘,置入122个钛网及122个钛板。椎体一端退变发生进展则认定为进展,上下端均存在进展,则以进展快的定级。 相邻节段退变根据Hilibrand退变分级标准[14],相邻节段退变非进展组100例,其中3例相邻节段退变,为2级;97例相邻节段退变1级,终末随访期均未进展。相邻节段退变进展组22例,其中9例为2级上升到3级,1例为1级上升到3级,12例为1级上升到2级;退变类型为:椎间隙轻度狭窄,无骨赘12例,椎间隙狭窄大于正常高度50%,伴骨赘10例。分组流程图见图4。"
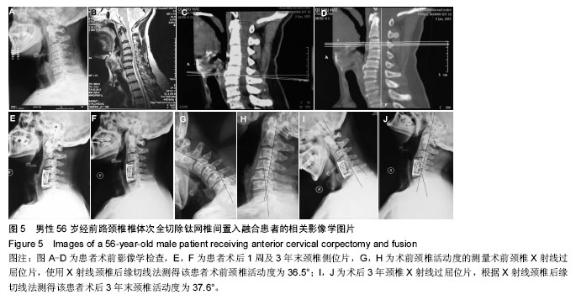
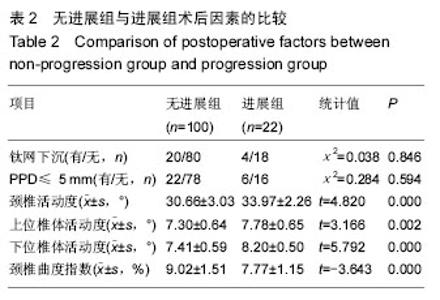
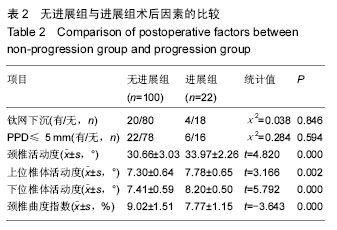
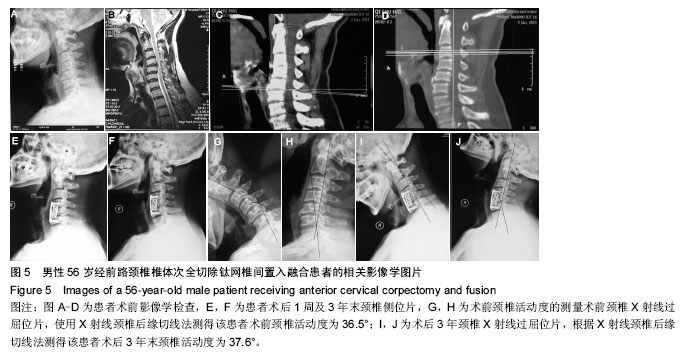
2.6 典型病例 男性患者,56岁,主因“四肢麻木无力3年,加重伴行走受限1个月”入院。专科检查提示:四肢肌张力相应减低,肌腱反射亢进。可查及躯体感觉减退平面。辅助检查:X射线提示:颈椎曲度轻度反屈,C5、C6椎体骨赘形成;颈椎CT提示:椎管狭窄(图5A)。颈椎MRI提示:C4/5后纵韧带增生,压迫相应脊髓,椎管狭窄,明确诊断为颈椎病(图5B-D),行ACCF治疗。 患者术后3 d,复查颈椎X射线,颈椎侧位片显示C6椎体下缘骨赘形成,成“唇样变”,C7椎体上缘骨赘形成,成“唇样变”。钛网融合良好,结构稳定,钛板固定(图5E)。根据Hilibrand退变分级的影像学分级标准定义相邻节段退变为Ⅱ级。术后3年随访,颈椎侧位片显示C6椎体下缘骨赘形成,C7椎体上缘骨赘形成,并与C6椎体下缘骨赘形成“桥接”。钛网融合良好,结构稳定,钛板固定(图5F)。根据Hilibrand退变分级的影像学分级标准定义由术前退变Ⅱ级进展到术后Ⅲ级。该患者行ACCF术后3年末相邻节段退变由术前退变Ⅱ级进展到术后Ⅲ级。患者术前术后颈椎活动度的变化见图5G-J。 2.7 不良事件 随访期间未出现血液、组织、免疫等反应,无组织包膜形成,无细胞质的改变、无钛合金腐蚀、磨损等材料的情况发生。"
| [1] Dorai Z, Morgan H, Coimbra C. Titanium cage reconstruction after cervical corpectomy. Neurosurg Spine. 2003;99:3-7. [2] Thalgott JS, Xiongsheng C, Giuffre JM. Single stage anterior cervical reconstruction with titanium mesh cages, local bone graft,and anterior plating.Spine. 2003;3:294-300. [3] Sevki K, Mehmet T, Ufuk T, et al. Results of surgical treatment for degenerative cervical myelopathy: anterior cervical corpectomy and stabilization. Spine. 2004;29:2493-2500. [4] 宋科冉,袁文,王新伟.椎体次全切除与椎间隙减压治疗多节段颈椎病的疗效比较[J].脊柱外科杂志,2011, 9(2): 102-107. [5] Song KJ, Choi BW, Jeon TS, et al. Adjacent segment degenerative disease: is it due to disease progression or a fusion associated phenomenon? Comparison between segments adjacent to the fused and non-fused segments. Eur Spine J. 2011;20:1940-1945. [6] Hilibrand AS, Carlson GD, Palumbo MA, et al. Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. Bone Joint Surg Am. 1999;81:519-528. [7] Dohler JR, Kahn MR, Hughes SP. Instability of the cervical spine after anterior interbody fusion. A study on its incidence and clinical significance in 21 patients. Arch Orthop Trauma Surg. 1985;104: 247-250. [8] Katsuura A, Hukuda S, Saruhashi Y, et al. Kyphotic malalignment after anterior cervical fusion is one of the factors promoting the degenerative process in adjacent intervertebral levels. Eur Spine J. 2001;10: 320-324. [9] Baba H,Furusawa N,Imura S,et al. Late rasiographic findings after anterior cervical fusion for spongylotic myeloradiculopathy. Spine (Phila Pa 1976). 1993;18: 2167-2173. [10] Goffin J, van Loon J, Van Calenbergh F, et al. Long-term results after anterior cervical fusion and osteosynthetic stabilization for fractures and/or dislocations of the cervical spine. Spinal Disord. 1995;8:500-508. [11] Kaplan EL, Meier P. Nonparametric estimation from incomplete observations. Am Stat Assoc. 1958;53: 457-481. [12] McGrory BJ, Klassen RA. Arthrodesis of the cervical spine for fractures and dislocations in children and adolescents. A long-term follow-up study. Bone Joint Surg Am. 1994;76:1606-1616. [13] Komura S, Miyamoto K, Hosoe H, et al. Lower incidence of adjacent segment degeneration after anterior cervical fusion found with those fusing C5-6 and C6-7 than those leaving C5-6 or C6-7 as an adjacent level. Spinal Disord Tech. 2012;25:23-29. [14] Song JS, Choi BW, Song KJ. Risk factors for the development of adjacent segment disease following anterior cervical arthrodesis for degenerative cervical disease:Comparison between fusion methods. J Clin Neurosci. 2014;21(5):794-798. [15] Park JB, Watthanaaphisit T, Riew KD. Timing of development of adjacent-level ossification after anterior cervical arthrodesis with plates. Spine. 2007;7(6):633-636. [16] 王辉,丁文元,申勇,等.颈椎后纵韧带骨化症间接减压术后轴性症状分析[J].中华外科杂志,2012,50(7):601-606. [17] lshibara A. Roetgenographic studies on the normal pattern of the cervical curvature. Nihon Seikeigeka Gakkai Zasshi. 1968;42: 1033-1044. [18] Wu JC,Liu L,Hang WC,et al. The Incidence of adiacent segment disease requriring surgery after anterior cervical discectomy and fusion:estimation using an eleven-year comprehensive nationwide database in Taiwan. Neurosurgery. 2011;2011VN. [19] Lee JC, Lee SH, Peters C, et al. Adjacent segment pathology requiring reoperation after anterior cervical arthrodesis: the influence of smoking, sex, and number of operated levels. Spine. 2015;40(10):E571-577. [20] Goffin J, Geusens E, Vantomme N, et al. Long-term follow-up after interbody fusion of the cervical spine. J Spinal Disord Tech. 2004;17(2):79-85. [21] 马志兵,冯虎,袁锋,等.颈椎前路减压固定融合术后钢板固定位置对相邻节段退变的影响[J].中国脊柱脊髓杂志, 2010, 20(3):201-204. [22] Chen Y,Chen D,Guo Y,et al. Subsidence of titanium mesh cage: a study based on 300 cases. Spinal Disord Tech. 2008;21(7):489-492. [23] Van Jonbergen HP,Spruit M,Anderson PG,et al. Anterior cervical interbody fusion with a titanium box cage: early radiological assessment of fusion and subsidence. Spine J. 2005;5(6):645-649. [24] 王志海.120例脊髓型颈椎病前路手术并发症临床观察[J].现代诊断与治疗,2013,24(10):2346-2347. [25] 谢宁,贾连顺,孙建国,等.颈椎不稳对颈椎病早期发病的影响[J].第二军医大学学报,2000,21(7):10-11. [26] Lee JH,Kim JS,Lee JH,et al.Comparison of cervical kinematics between patients with cervical artificial disc replacement and anterior cervical discectomy and fusion for cervical disc hernia tion. Spine J. 2014; 14(7):1199-1204. [27] Aghayev K, Doulgeris JJ, Gonzalez-Blohm SA, et al. Biomechanical comparison of a two-level anterior discectomy and a one-level corpectomy, combined with fusion and anterior plate reconstruction in the cervical spine. Clin Biomech. 2014;29(1):21-25. [28] Elsawaf A, Mastronardi L, Roperto R, et al. Effect of cervical dynamics on adjacent segment degeneration after anterior cervical fusion with cages. Neurosurg Rev. 2009;32(2):215-224. [29] Eck JC,Humphreys SC,Lim TH,et al. Biomechanical study on the effect of cervical spine fusion on adjacent-level intradiscal pressure and segmental motion. Spine. 2002;27(22):2431-2434. [30] 杨晋才,海涌,裴葆,等.颈前路融合节段数对上位邻近节段影响的生物力学研究[J].中华外科杂志,2014,9,52(9):692-696. [31] Katsuura A,Hukuda S,Saruhashi Y,et al. Kyphotic malalignment after anterior cervical fusion is one of the factors promoting the degenerative process in adjacent intervertebral levels. Eur Spine. 2001;10 :320–324. [32] Lee SE, Jahng TA, Kim HJ. Correlation between cervical lordosis and adjacent segment pathology after anterior cervical spinal surgery. Eur Spine J. 2015; 24(12): 1-11. |
| [1] | Shi Bin, An Jing, Chen Long-gang, Zhang Nan, Tian Ye . Influencing factors for pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 993-997. |
| [2] | Wang Xian-xun. Impact of local compression cryotherapy combined with continuous passive motion on the early functional recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 998-1003. |
| [3] | Yuan Wei, Zhao Hui, Ding Zhe-ru, Wu Yu-li, Wu Hai-shan, Qian Qi-rong. Association between psychological resilience and acute mental disorders after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1015-1019. |
| [4] | Chen Qun-qun, Qiao Rong-qin, Duan Rui-qi, Hu Nian-hong, Li Zhao, Shao Min. Acu-Loc®2 volar distal radius bone plate system for repairing type C fracture of distal radius [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1025-1030. |
| [5] | Huang Xiang-wang, Liu Hong-zhe. A new low elastic modulus of beta titanium alloy Ti2448 spinal pedicle screw fixation affects thoracic stability: biomechanical analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1031-1035. |
| [6] | Xie Qiang. Three-dimensional finite element model for biomechanical analysis of stress in knee inversion and external rotation after posterior cruciate ligament rupture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1036-1040. |
| [7] | He Ze-dong, Zhao Jing, Chen Liang-yu, Li Ke, Weng Jie. Multilevel finite element analysis on the biological tribology damage of water on bone tissue [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1041-1045. |
| [8] | Jiang Zi-wei, Huang Feng, Cheng Si-yuan, Zheng Xiao-hui, Sun Shi-dong, Zhao Jing-tao, Cong Hai-chen,Sun Han-qiao, Dong Hang. Design and finite element analysis of digital splint [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1052-1056. |
| [9] | Wang Fei, Liu Zhi-bin, Tao Hui-ren, Zhang Jian-hua, Li Chang-hong, Cao Qiang, Zheng Jun, Liu Yan-xiong, Qu Xiao-peng. Clinical efficacy of preoperative osteotomy designs using paper-cut technology versus photoshop software for ankylosing spondylitis with kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1057-1063. |
| [10] | Li Hui, Ma Jun-yi, Ma Yuan, Zhu Xu . Establishment of a three-dimensional finite element model of ankylosing spondylitis kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1069-1073. |
| [11] | Ling Guan-han, Ou Zhi-xue, Yao Lan, Wen Li-chun, Wang Guo-xiang, Lin Heng-feng. Establishment of simulating three-dimensional model of China-Japan Friendship Hospital Classification for L type osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1074-1079. |
| [12] | Fu Wei-min, Wang Ben-jie. Assessing the degree of necrotic femoral head, and association of blood supply with pathlogical changes: study protocol for a diagnostic animal trial [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1086-1091. |
| [13] | Zhang Wen-qiang, Ding Qian, Zhang Na. Associations between alpha angle and herniation pit on oblique axial magnetic resonance imaging in asymptomatic hip joints of adults [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1098-1103. |
| [14] | Sun Xiao-xin1, Zhou Wei2, Zuo Shu-ping3, Liu Hao1, Song Jing-feng1, Liang Chun-yu1. Morphological characteristics for the magnetic resonance imaging assessment of discoid lateral meniscal tears in children [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1104-1109. |
| [15] | Lin Han-wen, Wen Jun-mao, Huang Chao-yuan, Zhou Chi, Tang Hong-yu. Correlation between the changes in lower limb power line and pain area in the knee osteoarthritis patients: imaging evaluation [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1110-1114. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||