Chinese Journal of Tissue Engineering Research ›› 2016, Vol. 20 ›› Issue (22): 3315-3321.doi: 10.3969/j.issn.2095-4344.2016.22.017
Previous Articles Next Articles
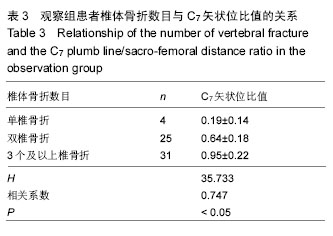
Osteoporotic vertebral compression fractures: correlation between number of fractured vertebrae and C7 plumb line/sacro-femoral distance ratio
Zhang Yi-long, Sun Zhi-jie, Wang Ya-hui, Ren Lei, Sun He
- Department of Spine Surgery, the Affiliated Hospital of Chengde Medical College, Chengde 067000, Hebei Province, China
-
Revised:2016-04-10Online:2016-05-27Published:2016-05-27 -
Contact:Sun He, Chief physician, Department of Spine Surgery, the Affiliated Hospital of Chengde Medical College, Chengde 067000, Hebei Province, China -
About author:Zhang Yi-long, Master, Associate chief physician, Department of Spine Surgery, the Affiliated Hospital of Chengde Medical College, Chengde 067000, Hebei Province, China -
Supported by:the Scientific Research Youth Foundation of Affiliated Hospital of Chengde Medical College, No. 201406
CLC Number:
Cite this article
Zhang Yi-long, Sun Zhi-jie, Wang Ya-hui, Ren Lei, Sun He . Osteoporotic vertebral compression fractures: correlation between number of fractured vertebrae and C7 plumb line/sacro-femoral distance ratio[J]. Chinese Journal of Tissue Engineering Research, 2016, 20(22): 3315-3321.
share this article
| [1] Ettinger MP. Aging bone and osteoporosis: strategies for preventing fractures in the elderly. Arch Intern Med. 2003;163(18): 2237-2246. [2] 安珍,杨定焯,张祖君,等.骨质疏松性脊椎压缩性骨折流行病学调查分析[J].中国骨质疏松杂志, 2002,8(1): 82-83. [3] Suzuki N, Ogikubo O, Hansson T. The prognosis for pain, disability, activities of daily living and quality of Life after an acute osteoporotic vertebral body fracture: its relation to fracture level, type of fracture and grade of fracture deformation. Eur Spine J. 2009;18(1): 77-88. [4] Nishimura A, Akeda K, Kato K, et al. Osteoporosis, vertebral fractures and mortality in a Japanese rural community. Mod Rheumatol. 2014;24(5): 840-843. [5] 邱勇,殷刚,曹兴兵,等.特发性胸椎侧凸患者的胸椎后凸状态对腰骶椎矢状面形态的影响[J].中华外科杂志, 2008, 46(16):1237-1340. [6] 刘辉,希腊本大,郑召民,等.腰椎间盘退变与脊柱-骨盆矢状面平衡的相关性[J].中华医学杂志,2013,93(15): 1123-1128. [7] Mac-Thiong J, Roussouly P, Berthonnaud E, et al. Sagittal paramefers of global spinal balance: normative values from a prospective cohort of seven hundred nine Caucasian asympomatic adults. Spine. 2010;35(22): E1193-1198. [8] Clement JL, Geoffray A, Yagoubi F, et al. Relationship between thoracic hypokyphosis, lumbar lordosis and sagittal pelvic parameters in adolescent idiopathic scoliosis. Eur Spine J. 2013;22(11):2414-2420. [9] Yang X, Kong Q, Song Y, et al. The characteristics of spinopelvic sagittal alignment in patients with lumbar disc degenerative diseases. Eur Spine J. 2014; 23(3): 569-575. [10] Passias PG, Poorman CE, Yang S, et al. Surgical Treatment Strategies for High-Grade Spondylolisthesis: A Systematic Review. Int J Spine Surg. 2015;9:50. [11] Barrey C, Jund J, Noseda O. Sagittal balance of the pelvis-spine complex and lumbar degenerative diseases. A comparative study about85 cases. Eur Spine J. 2007;16(9): 1459-1467. [12] Lafage V, Schwab F, Skalli W, et al. Standing balance and sagittal plane spinal deformity: analysis of spinopelvic and gravity line parameters. Spine. 2008; 33(14):1572-1578. [13] Briggs AM, Wrigley TV, Van Dieën JH, et al. The effect of osteoporotic vertebral fracture on predicted spinal loads in vivo. Eur Spine J. 2006;15(12): 1785-1795. [14] Schwab F, Patel A, Ungar B, et al. Adult spinal deformity-postoperative standing imbalance: how much can you tolerate? An overview of key parameters in assessing alignment and planning corrective surgery. Spine. 2010; 35(25):2224-2231. [15] Wang H, Ma L, Yang DL, et al. Radiological analysis of degenerative lumbar scoliosis in relation to pelvic incidence. Int J Clin Exp Med. 2015;8(12):22345-22351. [16] Barrey C, Roussouly P, Perrin G.Sagittal balance disorders in severe degenerative spine. Can we identify the compensatory mechanisms? Eur Spine J. 2011;20 Suppl 5:626-633. [17] Mehta VA, Amin A, Omeis I, et al. Implications of spinopelvic alignment for the spine surgeon. Neurosurgery.2012;70(3):707-721. [18] Mehta VA, Amin A, Omeis I, et al. Implications of spinopelvic alignment for the spine surgeon. Neurosurgery.2015;76 Suppl 1:S42-56. [19] Asai H, Tsuchiyama H, Hatakeyama T, et al. Age-related Changes in Maximum Pelvic Anteversion and Retroversion Angles Measured in the Sitting Position. J Phys Ther Sci. 2014;26(12): 1959-1961. [20] Barrey C, Roussouly P, Le Huec JC, et al. Compensatory mechanisms contributing to keep the sagittal balance of the spine. Eur Spine J. 2013;22 Suppl 6:S834-841. [21] Kobayashi T, Atsuta Y, Matsuno T, et al. A longitudinal study of congruent sagittal spinal alignment in an adult cohort. Spine. 2004;29(6):671-676. [22] Kim YB, Kim YJ, Ahn YJ, et al. A comparative analysis of sagittal spinopelvic alignment between young and old men without localized disc degeneration. Eur Spine J. 2014;23(7):1400-1406. [23] Barrey C, Jund J, Noseda O, et al. Sagittal balance of the pelvis-spine complex and lumbar degenerative diseases. a comparative study about 85 cases. Eur Spine J. 2007;16(9):1459-1467. [24] Kang KB, Kim YJ, Muzaffar N, et al. Changes of Sagittal Spinopelvic Parameters in Normal Koreans with Age over 50. Asian Spine J. 2010;4(2): 96-101. [25] Morita D, Yukawa Y, Nakashima H, et al. Range of motion of thoracic spine in sagittal plane. Eur Spine J. 2014;23(3): 673-678. [26] Baek SW, Kim C, Chang H. The relationship between the spinopelvic balance and the incidence of adjacent vertebral fractures following percutaneous vertebroplasty. Osteoporos Int. 2015;26(5):1507-1513. [27] Gaitanis IN, Carandang G, Phillips FM, et al. Restoring geometric and loading alignment of the thoracic spine with a vertebral compression fracture: effects of balloon (bone tamp) inflation and spinal extension. Spine. 2005;5(1):45-54. [28] Kanayama M. Sagittal plane correction in pedicle subtraction osteotomy using the Xia 3 SUK Direct Vertebral Rotation System: technical note. J Neurosurg Spine. 2013;19(4):507-514. [29] Suk SI, Kim JH, Lee SM, et al. Anterior-posterior surgery versus posterior closing wedge osteotomy in posttraumatic kyphosis with neurologic compromised osteoporotic fracture. Spine (Phila Pa 1976). 2003; 28(18):2170-2175. [30] Patil S, Rawall S, Singh D, et al. Surgical patterns in osteoporotic vertebral compression fractures. Eur Spine. 2013;22(4):883-891. [31] Galibert P, Deramond H, Rosat P, et al. Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty. Neurochirurgie. 1987;33(2): 166-168. [32] Josten C, Schmidt C, Spiegl U. Osteoporotic vertebral body fractures of the thoracolumbar spine. Diagnostics and therapeutic strategies. Chirurg. 2012;83(10): 866-874. [33] Yokoyama K, Kawanishi M, Yamada M, et al. Postoperative change in sagittal balance after Kyphoplasty for the treatment of osteoporotic vertebral compression fracture. Eur Spine J. 2015;24(4): 744-749. [34] Saxena BP, Shah BV, Joshi SP. Outcome of percutaneous balloon kyphoplasty in vertebral compression fractures. Indian J Orthop. 2015;49(4): 458-464. [35] 夏维财. 经皮椎体后凸成形术治疗老年骨质疏松性椎体压缩骨折[J]. 中国微创外科杂志, 2015,15(3):280-281, 288. [36] 于振和, 李东君. 经皮穿刺椎体后凸成形术治疗骨质疏松性椎体压缩性骨折的疗效观察[J]. 中国微创外科杂志, 2015,15(6):555-557. [37] Balkarli H, Demirtas H, Kilic M, et al. Treatment of osteoporotic vertebral compression fractures with percutaneous vertebroplasty under local anesthesia: clinical and radiological results. Int J Clin Exp Med. 2015;8(9): 16287-16293. [38] Roussouly P, Gollogly S, Berthonnaud E, et al. Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine. 2005;30(3):346-353. [39] Berthonnaud E, Dimnet J, Roussouly P, et al. Analysis of the sagittal balance of the spine and pelvis using shape and orientation parameters. J Spinal Disord Tech. 2005; 18(1):40-47. [40] Vaz G, Roussouly P, Berthonnaud E, et al. Sagittal morphology and equilibrium of pelvis and spine. Eur Spine J. 2002;11(1):80-87. |
| [1] | Shi Bin, An Jing, Chen Long-gang, Zhang Nan, Tian Ye . Influencing factors for pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 993-997. |
| [2] | Wang Xian-xun. Impact of local compression cryotherapy combined with continuous passive motion on the early functional recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 998-1003. |
| [3] | Yuan Wei, Zhao Hui, Ding Zhe-ru, Wu Yu-li, Wu Hai-shan, Qian Qi-rong. Association between psychological resilience and acute mental disorders after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1015-1019. |
| [4] | Chen Qun-qun, Qiao Rong-qin, Duan Rui-qi, Hu Nian-hong, Li Zhao, Shao Min. Acu-Loc®2 volar distal radius bone plate system for repairing type C fracture of distal radius [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1025-1030. |
| [5] | Huang Xiang-wang, Liu Hong-zhe. A new low elastic modulus of beta titanium alloy Ti2448 spinal pedicle screw fixation affects thoracic stability: biomechanical analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1031-1035. |
| [6] | Xie Qiang. Three-dimensional finite element model for biomechanical analysis of stress in knee inversion and external rotation after posterior cruciate ligament rupture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1036-1040. |
| [7] | He Ze-dong, Zhao Jing, Chen Liang-yu, Li Ke, Weng Jie. Multilevel finite element analysis on the biological tribology damage of water on bone tissue [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1041-1045. |
| [8] | Jiang Zi-wei, Huang Feng, Cheng Si-yuan, Zheng Xiao-hui, Sun Shi-dong, Zhao Jing-tao, Cong Hai-chen,Sun Han-qiao, Dong Hang. Design and finite element analysis of digital splint [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1052-1056. |
| [9] | Wang Fei, Liu Zhi-bin, Tao Hui-ren, Zhang Jian-hua, Li Chang-hong, Cao Qiang, Zheng Jun, Liu Yan-xiong, Qu Xiao-peng. Clinical efficacy of preoperative osteotomy designs using paper-cut technology versus photoshop software for ankylosing spondylitis with kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1057-1063. |
| [10] | Li Hui, Ma Jun-yi, Ma Yuan, Zhu Xu . Establishment of a three-dimensional finite element model of ankylosing spondylitis kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1069-1073. |
| [11] | Ling Guan-han, Ou Zhi-xue, Yao Lan, Wen Li-chun, Wang Guo-xiang, Lin Heng-feng. Establishment of simulating three-dimensional model of China-Japan Friendship Hospital Classification for L type osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1074-1079. |
| [12] | Fu Wei-min, Wang Ben-jie. Assessing the degree of necrotic femoral head, and association of blood supply with pathlogical changes: study protocol for a diagnostic animal trial [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1086-1091. |
| [13] | Zhang Wen-qiang, Ding Qian, Zhang Na. Associations between alpha angle and herniation pit on oblique axial magnetic resonance imaging in asymptomatic hip joints of adults [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1098-1103. |
| [14] | Sun Xiao-xin1, Zhou Wei2, Zuo Shu-ping3, Liu Hao1, Song Jing-feng1, Liang Chun-yu1. Morphological characteristics for the magnetic resonance imaging assessment of discoid lateral meniscal tears in children [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1104-1109. |
| [15] | Lin Han-wen, Wen Jun-mao, Huang Chao-yuan, Zhou Chi, Tang Hong-yu. Correlation between the changes in lower limb power line and pain area in the knee osteoarthritis patients: imaging evaluation [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1110-1114. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||