Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (48): 7769-7774.doi: 10.3969/j.issn.2095-4344.2014.48.011
Previous Articles Next Articles
Analgesic effect of ropivacaine complex liquid injection around the wound in lumbar fusion surgery
Wang Shi-jun1, Li Yu-ting2, Li Chun-de1, Liu Xian-yi1, Sun Hao-lin1, Wang Tian-long2
- 1Department of Orthopedics, Peking University First Hospital, Beijing 100034, China; 2Department of Anesthesiology, Xuanwu Hospital of Capital Medical University, Beijing 100053, China
-
Received:2014-10-23Online:2014-11-26Published:2014-11-26 -
Contact:Li Chun-de, Doctoral supervisor, Chief physician, Department of Orthopedics, Peking University First Hospital, Beijing 100034, China -
About author:Wang Shi-jun, M.D., Attending physician, Department of Orthopedics, Peking University First Hospital, Beijing 100034, China
CLC Number:
Cite this article
Wang Shi-jun, Li Yu-ting, Li Chun-de, Liu Xian-yi, Sun Hao-lin, Wang Tian-long. Analgesic effect of ropivacaine complex liquid injection around the wound in lumbar fusion surgery[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(48): 7769-7774.
share this article
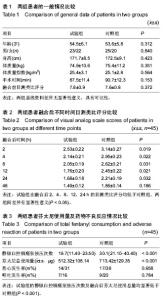
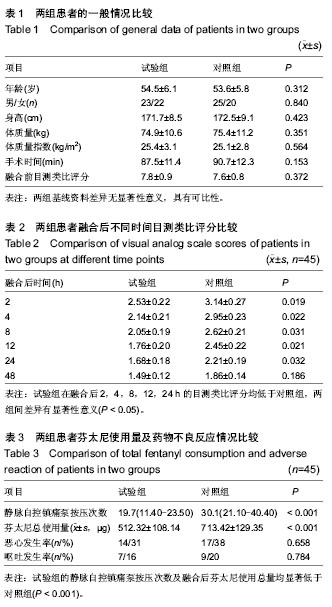
2.1 参与者数量分析 按意向性处理,纳入腰椎管狭窄症患者90例,按随机数字表法分为两组:试验组45例,对照组45例。全部进入结果分析,无脱落。 2.2 基线资料比较 共纳入90例患者,两组患者的年龄、男女比例、身高、体质量、体质量指数、手术时间及融合前目测类比评分等资料比较差异均无显著性意义,具有可比性 (表1)。 2.3 术后目测类比评分 试验组和对照组融合后目测类比评分均在融合后2 h最高,之后随着时间推移逐渐减少。试验组在融合后2,4,8,12,24 h的目测类比评分均低于对照组,两组间差异有显著性意义(P < 0.05,表2)。 2.4 术后芬太尼使用量及药物不良反应情况 试验组的静脉自控镇痛泵按压次数低于对照组,两组间差异有显著性意义(P < 0.001)。 试验组的融合后芬太尼使用总量低于对照组,两组间差异有显著性意义(P < 0.001)。试验组的恶心、呕吐发生率低于对照组,但差异无显著性意义(P > 0.05),见表3。 两组间均未出现心律失常、低血压及过敏反应。"
| [1] Carvalho B, Lemmens HJ, Ting V,et al.Postoperative subcutaneous instillation of low-dose ketorolac but not hydromorphone reduces wound exudate concentrations of interleukin-6 and interleukin-10 and improves analgesia following cesarean delivery.J Pain. 2013;14(1):48-56. [2] Raw DA, Beattie JK, Hunter JM,et al. Anaesthesia for spinal surgery in adults. Br J Anaesth.2003;91(6):886-904. [3] Ishikawa Y, Imashuku Y, Kitagawa H,et al. Evaluation of the side effects of intravenous patient controlled analgesia after spine surgery. Masui. 2011; 60(8):920-923. [4] McDaid C, Maund E, Rice S, et al.Paracetamol and selective and non-selective non-steroidal anti-inflammatory drugs (NSAIDs) for the reduction of morphine-related side effects after major surgery: a systematic review.Health Technol Assess. 2010;14(17):151-153. [5] Maund E, McDaid C, Rice S, et al.Paracetamol and selective and non-selective non-steroidal antiinflammatory drugs for the reduction in morphine-related sideeffects after major surgery: a systematic review. Br J Anaesth.2011; 106: 292-297. [6] Wickerts L, Warren Stomberg M, Brattwall M, et al.Coxibs: is there a benefit when compared to traditional nonselective NSAIDs in postoperative pain management? Minerva Anestesiol.2011;77:1-2. [7] Oh JH, Rhee KY, Kim SH,et al.Comparison of analgesic efficacy between single interscalene block combined with a continuous intra-bursal infusion of ropivacaine and continuous interscalene block after arthroscopic rotator cuff repair.Clin Orthop Surg. 2009;1(1):48-53. [8] Costantini R, Affaitati G, Fabrizio A, et al. Controlling pain inthe post-operative setting. Int J Clin Pharmacol Ther.2011; 49(2):116-127. [9] Haller Y, Gantenbein AR, Willimann P,et al.Systemic ropivacaine diminishes pain sensitization processes: a randomized, double-blinded, placebo-controlled, crossover study in healthy volunteers.Pain Ther. 2014;3(1): 45-58. [10] Li M, Wan L, Mei W, et al.Update on the clinical utility and practical use of ropivacaine in Chinese patients.Drug Des Devel Ther. 2014;8:1269-1276. [11] Newton DJ, McLeod GA, Khan F, et al. The effect of adjuvant epinephrine concentration on the vasoactivity of the local anesthetics bupivacaine and levobupivacaine in human skin.Reg Anesth Pain Med. 2004;29:307-311. [12] Liu X, Zhao X, Lou J,et al.Parecoxib added to ropivacaine prolongs duration of axillary brachial plexus blockade and relieves postoperative pain.Clin Orthop Relat Res. 2013; 471(2):562-568. [13] Carvalho B, Lemmens HJ, Ting V,et al.Postoperative subcutaneous instillation of low-dose ketorolac but not hydromorphone reduces wound exudate concentrations of interleukin-6 and interleukin-10 and improves analgesia following cesarean delivery.J Pain. 2013;14(1):48-56. [14] Blumenthal S, Borgeat A, Pasch T,et al.Ropivacaine decreases inflammation in experimental endotoxin-induced lung injury. Anesthesiology. 2006;104(5):961-969. [15] Piegeler T, Dull RO, Hu G, et al.Ropivacaine attenuates endotoxin plus hyperinflation-mediated acute lung injury via inhibition of early-onset Src-dependent signaling.BMC Anesthesiol. 2014;19(14)57. [16] Kawaguchi Y, Matsui H, Tsuji H. Back muscle injury after posterior lumbar spine surgery. A histologic and enzymatic analysis. Spine. 1996;21:941-944. [17] Genevay S, Atlas SJ.Lumbar Spinal Stenosis.Best Pract Res Clin Rheumatol. 2010;24(2): 253-265. [18] Kawaguchi Y, Matsui H, Tsuji H. Changes in serum creatine phosphokinase MM isoenzyme after lumbar spine surgery. Spine. 1997;22: 1018-1023. [19] Kotil K, Tunckale T, Tatar Z, et al. Serum creatine phosphokinase activity and histological changes in the multifidus muscle: a prospective randomized controlled comparative study of discectomy with or without retraction. J Neurosurg Spine. 2007;6:121-125. [20] Shin DA, Kim KN, Shin HC, et al. The efficacy of microendoscopic discectomy in reducing iatrogenic muscle injury. J Neurosurg Spine. 2008;8:39-43. [21] Borsook D. Neurological diseases and pain.Brain.2012; 135(2):320-344. [22] Sinatra R. Role of COX-2 inhibitors in the evolution of acute pain management. J Pain Sysmptom Manage. 2002;24: S18-S27. [23] Elvir-Lazo OL, White PF. Postoperative pain management after ambulatory surgery: role of multimodal analgesia. Anesthesiol Clin. 2010;28(2): 217-224. [24] Kang H, Kim BG. Intravenous lidocaine for effective pain relief after inguinal herniorrhaphy: a prospective, randomized, double-blind, placebo-controlled study. J Int Med Res.2011;39: 435-445. [25] Marques EM, Jones HE, Elvers KT, et al.Local anaesthetic infiltration for peri-operative pain control in total hip and knee replacement: systematic review and meta-analyses of short- and long-term effectiveness.BMC Musculoskelet Disord. 2014; 15:220. [26] Wylde V, Gooberman-Hill R, Horwood J, et al. The effect of local anaesthetic wound infiltration on chronic pain after lower limb joint replacement: aprotocol for a double-blind randomised controlled trial. BMC Musculoskelet Disord.2011; 12:53. [27] Bisgaard T,Klarskov B, Kristiansen VB,et al.Multi-regional local anesthetic infiltration during laparoscopic cholecystectomy in patients receiving prophylactic mufti-modal analgesia:a randomized,double-blinded, placebo-controlled study. Anesth Analg.1999;89(4): 1017-1024. [28] Aguitte J,Baulig B,Ekatodramis G,et al. Continuous epicapsular ropivacaine 0.3% infusion after minimally invasive hip arthroplasty: a prospective, randomized,double-blinded, placebo-controlled study comparing continuous wound infusion with morphine patient-controlled analgesia. Anesth Analg. 2012;114(2):456-461. [29] Campo MM, Kerkhoffs GM, Sierevelt IN, et al.A randomised controlled trial for the effectiveness of intra-articular Ropivacaine and Bupivacaine on pain after knee arthroscopy: the DUPRA (DUtch Pain Relief after Arthroscopy)-trial.Knee Surg Sports Traumatol Arthrosc. 2012;20(2):239-244. [30] Yun MJ, Oh JH, Yoon JP,et al.Subacromial patient-controlled analgesia with ropivacaine provides effective pain control after arthroscopic rotator cuff repair.Knee Surg Sports Traumatol Arthrosc. 2012;20(10):1971-1977. [31] Wang X, Jia D, Chen X,et al.Comparison of intra-articular low-dose sufentanil, ropivacaine, and combined sufentanil and ropivacaine on post-operative analgesia of isolated anterior cruciate ligament reconstruction.Knee Surg Sports Traumatol Arthrosc. 2013;21(5):1140-1145. [32] Haksever M, Özmen S, Akduman D,et al.Topical bupivacaine compared to bupivacaine infiltration for post-tonsillectomy pain relief in children: a prospective randomized controlled clinical study.Eur Arch Otorhinolaryngol. 2014;271(9): 2555-2559. [33] Moore SE, Reid KC, Draganic BD,et al.Randomized clinical trial of ropivacaine wound infusion following laparoscopic colorectal surgery.Tech Coloproctol. 2012;16(6):431-436. [34] Rabinow B, Werling J, Bendele A,et al.Intra-articular (IA) Ropivacaine Microparticle Suspensions Reduce Pain, Inflammation, Cytokine, and Substance P Levels Significantly More than Oral or IA Celecoxib in a Rat Model of Arthritis. Inflammation. 2014. [Epub ahead of print] [35] Yamashita A,Matsumoto M,Matsumoto S,et al.A comparison of the neurotoxic effects on the spinal cord of tetracaine, lidocaine,bupivaine,and ropivacaine administered intrathecally in rabbits. Anesth Analg. 2003;97:512-519. [36] Brodner G, Buerkle H, Van Aken H, et al. Postoperative analgesia after knee surgery: a comparison of three different concentrations of ropivacaine for continuous femoral nerve blockade.Anesth Analg. 2007;105:256-262. [37] Paauwe JJ, Thomassen BJ, Weterings J, et al. Femoral nerve block using ropivacaine 0.025%, 0.05% and 0.1%: effects on the rehabilitation programme following total knee arthroplasty: a pilot study.Anaesthesia. 2008;63:948-953. [38] Sato K, Adachi T, Shirai N, et al.Continuous versus single-injection sciatic nerve block added to continuous femoral nerve block for analgesia after total knee arthroplasty: a prospective, randomized, double-blind study. Reg Anesth Pain Med. 2014;39(3):225-229. [39] Gill AM, Scott NB, Abbas M, et al. Ropivacine plasma levels following local infiltration analgesia for primary total hip arthroplasty. Anaesthesia.2014;69(4):368-373. [40] Förster JG, Lumme HM, Palkama VJ,et al.Epinephrine 4 microg/mL added to a low-dose mixture of ropivacaine and fentanyl for lumbar epidural analgesia after total knee arthroplasty. Anesth Analg. 2008;106(1):301-304. [41] Ratajczak-Enselme M, Estebe JP, Rose FX,et al.Effect of epinephrine on epidural, intrathecal, and plasma pharmacokinetics of ropivacaine and bupivacaine in sheep.Br J Anaesth. 2007;99(6):881-890. |
| [1] | Yao Rubin, Wang Shiyong, Yang Kaishun. Minimally invasive transforaminal lumbar interbody fusion for treatment of single-segment lumbar spinal stenosis improves lumbar-pelvic balance [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1387-1392. |
| [2] | Tian Yang, Tang Chao, Liao Yehui, Tang Qiang, Ma Fei, Zhong Dejun. Consistency and repeatability of CT and MRI in measurement of spinal canal area in patients with lumbar spinal stenosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3882-3887. |
| [3] | Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao. Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 796-802. |
| [4] | Wang Jing, Xu Shuai, Liu Haiying. Hidden blood loss during posterior lumbar interbody fusion in lumbar spinal stenosis patients with and without rheumatoid arthritis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5307-5314. |
| [5] | Zhang Chunlin, Shang Lijie, Yan Xu, Cao Zhengming, Shao Chenglong, Feng Yang. Mid-long-term effect of only placed expandable interbody fusion cage in the treatment of lumbar spinal stenosis with vertebral instability using micro-endoscopic discectomy system [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 335-341. |
| [6] | Liu Jinyu, Ding Yu, Jiang Qiang, Cui Hongpeng, Lu Zhengcao. A finite element model of full endoscope lumbar fenestration and biomechanical characteristics [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(27): 4291-4296. |
| [7] | Shen Canghai, Feng Yongjian, Song Yancheng, Liu Gang, Liu Zhiwei, Wang Ling, Dai Haiyang. Value of quantitative MRI T2WI parameters in predicting surgical outcome of thoracic ossification of the ligamentum flavum [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(18): 2893-2899. |
| [8] | Fu Jiaxin, Xiao Lianping, Wang Shusen, Li Xiaodong, Han Liqiang, Wang Tonghao. Therapeutic effects of paraspinal approach combined with internal fixation through pedicle of fractured vertebra versus traditional AF screw-rod system for thoracolumbar fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1177-1181. |
| [9] | Qiu Zhongpeng, Li Ke, Li Gang, Liu Keyu, Du Xinhui, Meng Defeng, Shi Chenhui, Wang Weishan. Different treatments for two-part and three-part proximal humeral fractures by Neer classification: follow-up results analyzed using clinical economics [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1188-1195. |
| [10] | Ke Wei, Li Ke, Wang Sibo, Du Xinhui, Qiu Zhongpeng, Kang Zhilin, Wang Weishan, Li Gang . Open reduction and plate fixation versus closed reduction and external fixation for distal radius fractures: scores and linear regression analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1196-1202. |
| [11] | Tian Jie, Ru Jiangying. Preservation of the spinous process ligament complex in expanded decompression of lumbar spinal canal: advantages and disadvantages [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1228-1234. |
| [12] | Fan Zhirong, Peng Jiajie, Zhong Degui, Zhou Lin, Su Haitao, Huang Yongquan, Wu Jianglin, Liang Yihao. Suture anchor combined with open reduction and internal fixation versus open reduction and internal fixation for ankle fracture combined with deltoid ligament injury: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1307-1312. |
| [13] | Zhou Yu, Liu Yuehong, Liu Shuping, Chen Xi, Qin Wei, Li Qifeng. Spinal stability of intervertebral grafting reinforced by five or six augmenting screws versus transvertebral grafting reinforced by four augmenting screws for thoracolumbar vertebral fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 505-511. |
| [14] | Li Xianzhou, Wang Qian, Zhang Cunxin . Lumbar spondylolisthesis: status and prospects of implant treatment [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 621-627. |
| [15] | He Da, Zhao Jingwei, Liu Bo, Tian Wei. Comparison of limited fusion and full curve fusion for mild lumbar degenerative scoliosis with stenosis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(36): 5811-5817. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||