Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (18): 2939-2946.doi: 10.12307/2024.049
Previous Articles Next Articles
Biomechanics characteristics during sitting up in knee osteoarthritis patients of different ages: a systematic review and meta-analysis
Wang Ke, Zhang Zeyi, Zhang Liwen, Zhang Meizhen
- College of Physical Education, Taiyuan University of Technology, Taiyuan 030024, Shanxi Province, China
-
Received:2023-03-27Accepted:2023-04-28Online:2024-06-28Published:2023-08-26 -
Contact:Zhang Meizhen, PhD, Professor, College of Physical Education, Taiyuan University of Technology, Taiyuan 030024, Shanxi Province, China -
About author:Wang Ke, Master candidate, College of Physical Education, Taiyuan University of Technology, Taiyuan 030024, Shanxi Province, China -
Supported by:Shanxi Provincial Basic Research Program (Free Exploration Project) No. 202103021224109 (to ZMZ); The First Batch of New Liberal Arts Research and Reform Practice Project, No. 2021050026 (to ZMZ); Discipline Construction Funds of Taiyuan University of Technology (to SDB)
CLC Number:
Cite this article
Wang Ke, Zhang Zeyi, Zhang Liwen, Zhang Meizhen. Biomechanics characteristics during sitting up in knee osteoarthritis patients of different ages: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2939-2946.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

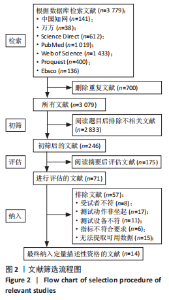
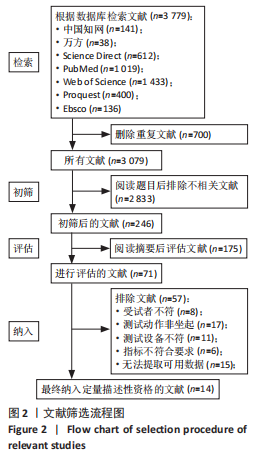
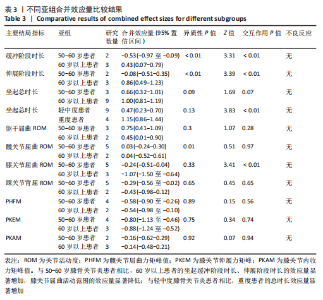
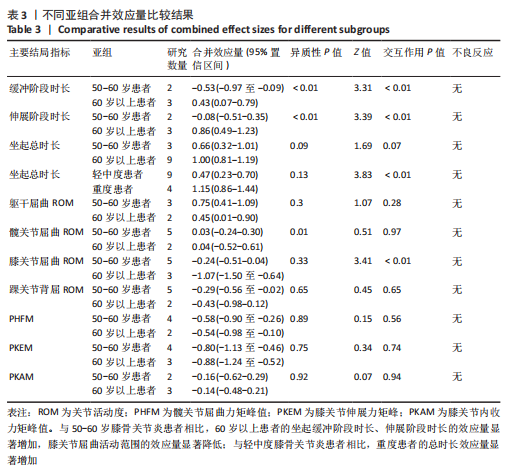
2.3 Meta分析结果 2.3.1 两组受试者坐起缓冲阶段时长、伸展阶段时长以及总时长的差异 有4篇文献分析两组坐起缓冲阶段时长差异[15,25,30,33],异质性偏低(I2=71.9%,P=0.007),两组缓冲阶段时长无显著性差异(SMD=0.04,95%CI:-0.23-0.32,P=0.754)。此外,4篇文献分析两组人群伸展阶段时长差异[15,25,30,33],异质性较低(I2=63.7%,P=0.026),相比健康人,膝骨关节炎患者坐起伸展阶段时长增加(SMD=0.46,95%CI:0.18-0.74,P=0.001),且60岁以上膝骨关节炎患者(I2=0.0%,P=0.739)的时长增加较健康人更为明显(SMD=0.86,95%CI:0.49-1.23,P < 0.001),见图3。"


有9篇文献分析两组坐起总时长差异[14,24,26-30,33-34],异质性较高(I2=81.0%,P < 0.001),相比健康人,膝骨关节炎患者坐起总时长更久(SMD=0.92,95%CI:0.76-1.09,P < 0.001),重度患者(SMD=1.15,95%CI:0.86-1.44,P < 0.001)较健康人的时长增加更明显,60岁以上患者(SMD=1.00,95%CI:0.81-1.19,P < 0.001)较健康人的时长增加更明显,见图3。 2.3.2 两组受试者躯干、下肢各关节屈曲关节活动度的差异 有4篇文献分析两组坐起躯干屈曲关节活动度差异[15,25-26,30],异质性较低(I2=15.9%,P=0.313),膝骨关节炎患者躯干屈曲关节活动度比对照组更大(SMD=0.64,95%CI:0.37-0.91,P < 0.001)。另有6篇膝关节屈曲关节活动度文献[15,16,26,27,29,31],异质性偏低(I2=69.3%,P=0.002),相比对照组,膝骨关节炎患者膝关节屈曲关节活动度较小(SMD=-0.47,95%CI:-0.70至-0.24,P < 0.001),且60岁以上患者(SMD=-1.07,95%CI:-1.50至-0.64,P < 0.001)较健康人膝关节屈曲关节活动度下降更明显。5篇文献分析踝关节屈曲(背屈)关节活动度[15,16,26-27,29],异质性较低(I2=43.1%,P=0.103),相比健康人,膝骨关节炎患者踝关节屈曲(背屈)关节活动度更小(SMD=-0.32,95%CI:-0.56至-0.08,P=0.01),且50-60岁患者踝关节屈曲(背屈)关节活动度下降更明显(SMD=-0.29,95%CI: -0.56至-0.02,P=0.034],见图4。"


2.3.3 两组受试者膝关节力学指标的差异 有4篇文献分析两组PHFM差异[15,27,30,33],异质性偏低(I2=14.2%,P=0.324),相较对照组,膝骨关节炎患者的PHFM较低(SMD=-0.57,95%CI:-0.83至-0.31,P < 0.001)。另有5篇文献分析两组PKEM的差异[15,27,30,32-33],异质性较小(I2=5.0%,P=0.389),相比对照组,膝骨关节炎患者PKEM较低(SMD=-0.83,95%CI:-1.08至-0.59,P < 0.001)。4篇文献分析两组PKAM差异[27,31-33],异质性较高(I2=80.4%,P < 0.001),PKAM无显著差异(SMD=-0.15,95%CI:-0.42-0.13,P=0.29),见图5。"

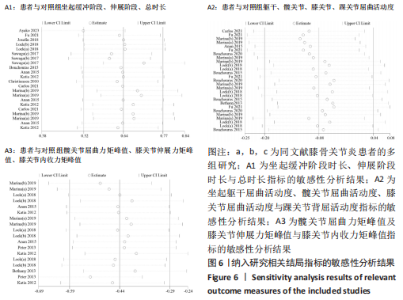
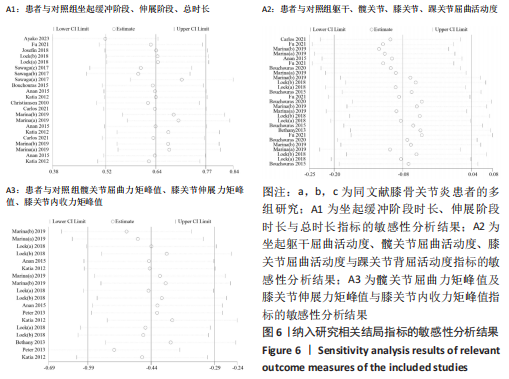
2.5 敏感性分析及异质性来源分析结果 YOKOTA[24] (2023)和SAWAGA[14] (2017)数据对坐起总时长的异质性结果贡献较高,PETRELLA等[15](2019)数据对伸展阶段时长的异质性结果贡献较高,剔除该部分数据后效应量由0.924和0.463变为0.737和0.857,异质性I2由81.0%和63.7%降至0%和0%。FU等[26] (2021)、PETRELLA等[15] (2019)以及VERLAAN等[27] (2018)部分数据对膝关节屈曲关节活动度指标的异质性亦贡献较大,剔除数据后效应量由-0.473变为-0.969,异质性I2由69.3%降至0%。此外,WORSLEY等[32] (2013)和LARSEN等[31] (2013)数据对PKAM异质性贡献较高,剔除该数据后效应量由-0.148变为-0.153,异质性I2由80.4%降至0%,见图6。"
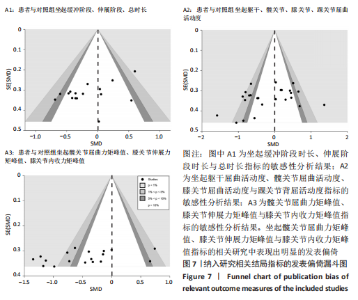
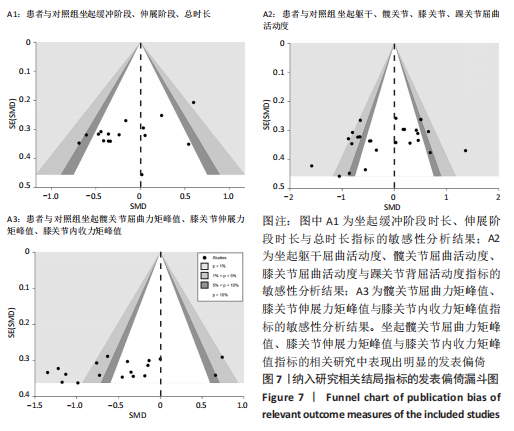
2.6 发表偏倚分析 两组坐起伸展阶段和总时长研究中,SAGAWA等[14] (2017)a可能存在发表偏倚,漏斗图出现不对称,剔除后所有研究均分布于漏斗图内。两组髋、膝关节屈曲关节活动度研究中PETRELLA等[15] (2019)b,BOUCHOURAS等[16] (2020)可能存在发表偏倚,剔除后所有研究均呈现对称分布在漏斗图内。此外,两组PHFM,PKEM以及PKAM的相关研究中VERLAAN等[27] (2018)b,PETRELLA等[15](2019)b,TURCOT等[33] (2012)及LARSEN等[31] (2013)文献可能存在发表偏倚,剔除后所有研究均分布于漏斗图内,见图7。"
| [1] 陈百成,张静.骨关节炎[M].北京:人民卫生出版社,2014:18. [2] LI D, LI S, CHEN Q, et al. The prevalence of symptomatic knee osteoarthritis in relation to age, sex, area, region, and body mass index in China: a systematic review and Meta-analysis. Front Med. 2020;7(1):304. [3] DANTAS LO, SALVINI TF, MCALINDON TE. Knee osteoarthritis: key treatments and implications for physical therapy. Braz J Phys Ther. 2021;25(2):135-146. [4] VISSERS MM, BUSSMANN JBJ, DE GROOT IB, et al. Walking and chair rising performed in the daily life situation before and after total hip arthroplasty. Osteoarthritis Cartilage. 2011;19(9):1102-1107. [5] KATZ JN, ARANT KR, LOESER RF. Diagnosis and treatment of hip and knee osteoarthritis: a review. JAMA. 2021;325(6):568-578. [6] 王攀, 霍洪峰. 老年人坐立转换时股骨近端应力分布的有限元分析[J].医用生物力学, 2022,37(2):312-316, 322. [7] SKOU ST, GRøNNE DT, ROOS EM. Prevalence, severity, and correlates of pain flares in response to a repeated sit-to-stand activity: a cross-sectional study of 14902 patients with knee and hip osteoarthritis in primary care. J Orthop Sports Phys Ther. 2020;50(6):309-318. [8] PRIMORAC D, MOLNAR V, ROD E, et al. Knee osteoarthritis: a review of pathogenesis and state-of-the-art non-operative therapeutic considerations. Genes. 2020;11(8):854. [9] 安丙辰,戴尅戎.影响膝骨关节炎发病及进展的生物力学因素[J].国际骨科学杂志, 2012,33(3):153-156. [10] 汤雨婷,安丙辰,郑洁皎.膝骨关节炎生物力学参数的研究进展[J].中国康复理论与实践,2020,26(12):1417-1421. [11] TENG HL, CALIXTO N, MACLEOD T, et al. Associations between patellofemoral joint cartilage T1ρ and T2 and knee flexion moment and impulse during gait in individuals with and without patellofemoral joint osteoarthritis. Osteoarthritis Cartilage. 2016;24(9):1554-1564. [12] BURN E, MURRAY D, HAWKER G, et al. Lifetime risk of knee and hip replacement following a GP diagnosis of osteoarthritis: a real-world cohort study. Osteoarthritis cartilage. 2019;27(11):1627-1635. [13] DOWNIE C. Biomechanical, physiological and cognitive factors in balance recovery in older adults with knee osteoarthritis. Melbourne: Victoria University. 2021. [14] SAGAWA Y, BONNEFOY-MAZURE A, ARMAND S, et al. Variable compensation during the sit-to-stand task among individuals with severe knee osteoarthritis. Ann Phys Rehabil Med. 2017;60(5):312-318. [15] PETRELLA M, DA SILVA SERRãO PRM, SELISTRE LFA, et al. Individual joint contributions to the total support moment during the sit-to-stand task differentiate mild and moderate knee osteoarthritis. Clin Biomech. 2019;70(1):52-58. [16] BOUCHOURAS G, SOFIANIDIS G, PATSIKA G, et al. Women with knee osteoarthritis increase knee muscle co-contraction to perform stand to sit. Aging Clin Exp Res. 2020;32(4):655-662. [17] HIGGINS JP, THOMAS J, CHANDLER J, et al. Cochrane handbook for systematic reviews of interventions. John Wiley Sons. 2019. [18] MOHER D, LIBERATI A, TETZLAFF J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;151(4):264-269. [19] KELLGREN JH, LAWRENCE JS. Radiological assessment of osteo-arthrosis. Ann Rheum Dis. 1957;16(4):494-502. [20] CHUANG CH, KUO CC, CHIANG YF, et al. Enriched peripheral blood-derived mononuclear cells for treating knee osteoarthritis. Cell Transplant. 2023;32: 09636897221149445. [21] 张琦,梁媛,张冉,等.运动学对线技术对全膝关节置换术后关节活动度的效果[J].中国康复理论与实践,2022,28(7):764-769. [22] KHALAJ N, VICENZINO B, HEALES L J, et al. Is chronic ankle instability associated with impaired muscle strength? Ankle, knee and hip muscle strength in individuals with chronic ankle instability: a systematic review with meta-analysis. Br J Sport Med. 2020; 54(14):839-847. [23] 张天嵩,张苏贤.如何实现Meta分析中不同亚组合并效应量的比较[J].中国循证医学杂志,2017,17(12):1465-1470. [24] YOKOTA A, MAESHIMA E, SASAKI K, et al. Physical functions associated with health-related quality of life in older adults diagnosed with knee osteoarthritis. J Phys Ther Sci. 2023; 35(1):60-65. [25] RODRIGUEZ‐LOPEZ C, BECKWéE D, LUYTEN FP, et al. Reduced knee extensor torque production at low to moderate velocities in postmenopausal women with knee osteoarthritis. Scand J Med Sci Sports. 2021; 31(11):2144-2155. [26] FU S, DUAN T, HOU M, et al. Postural balance in individuals with knee osteoarthritis during stand-to-sit task. Front Human Neurosci. 2021;15(1):760960. [27] VERLAAN L, BOEKESTEIJN RJ, OOMEN PW, et al. Biomechanical alterations during sit-to-stand transfer are caused by a synergy between knee osteoarthritis and obesity. Biomed Res Int. 2018;2018:3519498. [28] NAILI JE, BROSTRöM EW, GUTIERREZ-FAREWIK EM, et al. The centre of mass trajectory is a sensitive and responsive measure of functional compensations in individuals with knee osteoarthritis performing the five times sit-to-stand test. Gait Posture. 2018;62(1): 140-145. [29] BOUCHOURAS G, PATSIKA G, HATZITAKI V, et al. Kinematics and knee muscle activation during sit-to-stand movement in women with knee osteoarthritis. Clin Biomech (Bristol, Avon). 2015;30(6):599-607. [30] ANAN M, SHINKODA K, SUZUKI K, et al. Do patients with knee osteoarthritis perform sit-to-stand motion efficiently? Gait Posture. 2015;41(2):488-492. [31] LARSEN BL, JACOFSKY MC, BROWN JA, et al. Valgus bracing affords short-term treatment solution across walking and sit-to-stand activities. J Arthroplasty. 2013;28(5):792-797. [32] WORSLEY P, STOKES M, BARRETT D, et al. Joint loading asymmetries in knee replacement patients observed both pre-and six months post-operation. Clin Biomech. 2013;28(8): 892-897. [33] TURCOT K, ARMAND S, FRITSCHY D, et al. Sit-to-stand alterations in advanced knee osteoarthritis. Gait Posture. 2012;36(1): 68-72. [34] CHRISTIANSEN CL, STEVENS-LAPSLEY JE. Weight-bearing asymmetry in relation to measures of impairment and functional mobility for people with knee osteoarthritis. Arch Phys Med Rehabil. 2010;91(10): 1524-1528. [35] DOWNS SH, BLACK N. The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J Epidemiol commun health. 1998;52(6):377-384. [36] JANDRE REIS FJ, MACEDO AR. Influence of hamstring tightness in pelvic, lumbar and trunk range of motion in low back pain and asymptomatic volunteers during forward bending. Asian Spine J. 2015;9(4):535-540. [37] IIJIMA H, SUZUKI Y, AOYAMA T, et al. Interaction between low back pain and knee pain contributes to disability level in individuals with knee osteoarthritis: a cross-sectional study. Osteoarthritis Cartilage. 2018;26(10):1319-1325. [38] IIJIMA H, SHIMOURA K, AOYAMA T, et al. Low back pain as a risk factor for recurrent falls in people with knee osteoarthritis. Arthritis Care Res. 2021;73(3):328-335. [39] YOSHIZUKA H, TANIGUCHI T, FUKUTA K, et al. Decrease in medial meniscal extrusion after physical therapy to improve knee pain and range of motion in patients with knee osteoarthritis: a retrospective study. PLos One. 2022;17(11):e0277628. [40] ROSADI R, JANKAEW A, WU PT, et al. Factors associated with falls in patients with knee osteoarthritis: a cross-sectional study. Medicine. 2022;101(48):e32146. [41] ZAJDMAN ORB, FLAXMAN TE, BIGHAM HJ, et al. Females with knee osteoarthritis use a detrimental knee loading strategy when squatting. Knee. 2022;38(1):9-18. [42] BERTEAU JP. Knee pain from osteoarthritis: pathogenesis, risk factors, and recent evidence on physical therapy interventions. J Clin Med. 2022;11(12):3252. [43] YAMADA T, DEMURA S, SHIN S. The influence of various upper limb supports on the output of leg muscle strength and the rating of perceived exertion during sit-to-stand movements. Japan Journal of Test and Measurement in Health and Physical Education. 2019;9(1):33-38. [44] HUNT MA, WRIGLEY TV, HINMAN RS, et al. Individuals with severe knee osteoarthritis (OA) exhibit altered proximal walking mechanics compared with individuals with less severe OA and those without knee pain. Arthritis Care Res. 2010;62(10):1426-1432. |
| [1] | Zhong Jun, Wang Wen. Network meta-analysis of different anatomical repair strategies to improve chronic lateral ankle instability [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1470-1476. |
| [2] | Li Zhifei, Yang Yin, Chen Hualong, Liang Qinqiu, Zhong Yuanming, Zhang Yisheng. Finite element analysis of the correlation between tilt angle of titanium cage and postoperative subsidence of titanium cage after anterior subtotal cervical corpectomy, decompression and fusion [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1313-1319. |
| [3] | Yang Junliang, Lu Tan, Xu Biao, Jiang Yaqiong, Wang Fucheng. Three-dimensional finite element analysis of effects of partial anterior cruciate ligament rupture on knee joint stress [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1347-1353. |
| [4] | Li Yongjie, Fu Shenyu, Xia Yuan, Zhang Dakuan, Liu Hongju. Correlation of knee extensor muscle strength and spatiotemporal gait parameters with peak knee flexion/adduction moment in female patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1354-1358. |
| [5] | Wu Jing, Yao Yingce, Yang Xiaowei, Xue Boshi, Zhao Jianbin, Yang Chen, Luan Tianfeng, Zhou Zhipeng. Intervention of muscle strength training combined with neuromuscular electrical stimulation on lower limb function and biomechanical changes in patients with patellofemoral pain [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1365-1371. |
| [6] | Xi Jintao, Lu Qilin, Wang Yang, Wang Xiaojuan, Lyu Peng, Chen Long, Shi Zhen, Xie Wei, Zhu Yiliang, Li Xugui. Risk factors for cage retropulsion following transforaminal lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1394-1398. |
| [7] | Niu Hegang, Yang Kun, Zhang Jingjing, Yan Yizhu, Zhang Yinshun. Design of a new posterior atlas fracture reduction and internal fixation system [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1399-1402. |
| [8] | Du Changling, Shi Hui, Zhang Shoutao, Meng Tao, Liu Dong, Li Jian, Cao Heng, Xu Chuang. Efficacy and safety of different applications of tranexamic acid in high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1409-1413. |
| [9] | Wang Weiqing, Zhou Yue. Chronic inflammation regulates adipose tissue fibrosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1307-1312. |
| [10] | Shen Jiangyong, He Xi, Tang Yuting, Wang Jianjun, Liu Jinyi, Chen Yuanyuan, Wang Xinyi, Liu Tong, Sun Haoyuan. RAS-selective lethal small molecule 3 inhibits the fibrosis of pathological scar fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1168-1173. |
| [11] | Huang Xiarong, Hu Lizhi, Sun Guanghua, Peng Xinke, Liao Ying, Liao Yuan, Liu Jing, Yin Linwei, Zhong Peirui, Peng Ting, Zhou Jun, Qu Mengjian. Effect of electroacupuncture on the expression of P53 and P21 in articular cartilage and subchondral bone of aged rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1174-1179. |
| [12] | Zhao Garida, Ren Yizhong, Han Changxu, Kong Lingyue, Jia Yanbo. Mechanism of Mongolian Medicine Erden-uril on osteoarthritis in rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1193-1199. |
| [13] | Zuo Xinwei, Liu Gang, Bai Huizhong, Xu Lin, Zhao Yi, Ren Jingpei, Hu Chuanyu, Mu Xiaohong. Relationship between lumbar spine development and hip development in children with spastic cerebral palsy [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1247-1252. |
| [14] | Zhuang Xinyi, Peng Yuanhao, Yu Ting, Lyu Dongmei, Wen Xiujie, Cheng Qian. Cone-beam CT evaluation of bone mass in the external oblique line of the mandible in adolescents with different cervical vertebral bone ages [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1253-1258. |
| [15] | Ma Shuwei, He Sheng, Han Bing, Zhang Liaoyun. Exosomes derived from mesenchymal stem cells in treatment of animals with acute liver failure: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1137-1142. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||