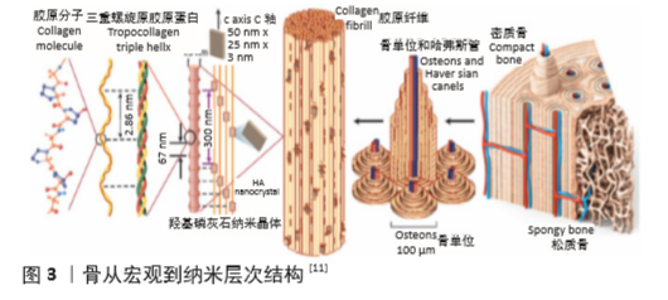
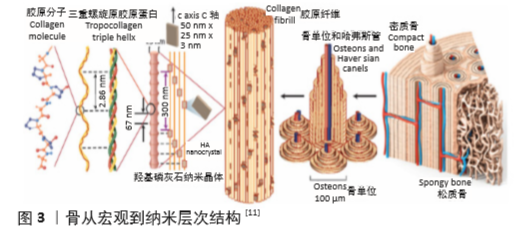
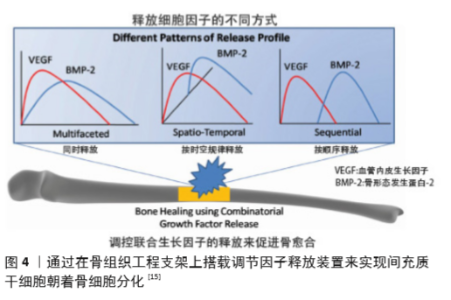
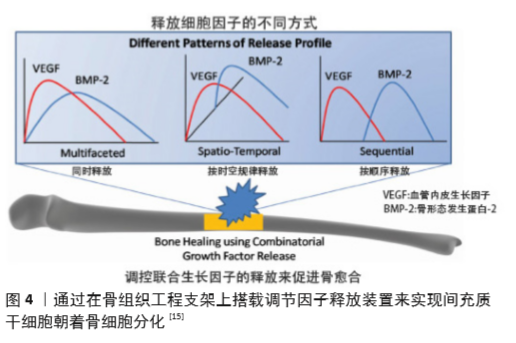
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (28): 4553-4560.doi: 10.12307/2021.072
Previous Articles Next Articles
Progress and challenges of bone tissue engineering scaffolds
Liao Xinyu, Wang Fuke, Wang Guoliang
- Department of Sports Medicine, the First Affiliated Hospital of Kunming Medical University, Kunming 650032, Yunnan Province, China
-
Received:2020-10-21Revised:2020-10-24Accepted:2020-11-21Online:2021-10-08Published:2021-05-21 -
Contact:Wang Fuke, Chief physician, Professor, Department of Sports Medicine, the First Affiliated Hospital of Kunming Medical University, Kunming 650032, Yunnan Province, China -
About author:Liao Xinyu, Master candidate, Department of Sports Medicine, the First Affiliated Hospital of Kunming Medical University, Kunming 650032, Yunnan Province, China -
Supported by:General Project of the Joint Special Fund for Applied Basic Research of Yunnan Provincial Department of Science and Technology and Kunming Medical University, No. 201701UH00095 (to WFK); Joint Special Fund for Applied Basic Research of Yunnan Provincial Department of Science and Technology and Kunming Medical University, No. 40220127 (to WGL)
CLC Number:
Cite this article
Liao Xinyu, Wang Fuke, Wang Guoliang. Progress and challenges of bone tissue engineering scaffolds[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(28): 4553-4560.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
| [1] LI J J, EBIED M, XU J, et al. Current Approaches to Bone Tissue Engineering: The Interface between Biology and Engineering. Adv Healthc Mater. 2018;7(6):e1701061. [2] RANALLETTA M, TANOIRA I, BERTONA A, et al. Autologous Tricortical Iliac Bone Graft for Failed Latarjet Procedures. Arthrosc Tech. 2019;8(3): e283-e289. [3] LIANG Y, LUAN X, LIU X. Recent advances in periodontal regeneration: A biomaterial perspective. Bioact Mater. 2020;5(2):297-308. [4] WANG F, YANG G, XIAO Y, et al. Effect of SDF-1 with biphasic ceramic-like bone graft on the repair of rabbit radial defect. J Orthop Surg Res. 2019;14(1):231. [5] PARK JY, PARK SH, KIM MG, et al. Biomimetic Scaffolds for Bone Tissue Engineering. Adv Exp Med Biol. 2018;1064:109-121. [6] HORAS K, ARNHOLDT J, STEINERT AF, et al. Acetabular defect classification in times of 3D imaging and patient-specific treatment protocols. Orthopade. 2017;46(2):168-178. [7] KUMAR A, MANDAL S, BARUI S, et al. Low temperature additive manufacturing of three dimensional scaffolds for bone-tissue engineering applications: Processing related challenges and property assessment. Mater Sci Eng R. 2016;103:1-39. [8] YEUNG M, ABDULMAJEED A, CARRICO CK, et al. Accuracy and precision of 3D-printed implant surgical guides with different implant systems: An in vitro study. J Prosthet Dent. 2020;123(6):821-828. [9] HAN C, LI Y, WANG Q, et al. Continuous functionally graded porous titanium scaffolds manufactured by selective laser melting for bone implants. J Mech Behav Biomed Mater. 2018;80:119-127. [10] WUBNEH A, TSEKOURA EK, AYRANCI C, et al. Current State of Fabrication Technologies and Materials for Bone Tissue Engineering. Acta Biomater. 2018;80:1-30. [11] WEGST UG, BAI H, SAIZ E, et al. Bioinspired structural materials. Nat Mater. 2015;14(1):23-36. [12] REZNIKOV N, SHAHAR R, WEINER S. Bone hierarchical structure in three dimensions. Acta Biomater. 2014;10(9):3815-3826. [13] DIMITRIOU R, TSIRIDIS E, GIANNOUDIS PV. Current concepts of molecular aspects of bone healing. Injury. 2005;36(12):1392-1404. [14] GANDOLFI MG, ZAMPARINI F, DEGLI ESPOSTI M, et al. Polylactic acid-based porous scaffolds doped with calcium silicate and dicalcium phosphate dihydrate designed for biomedical application. Mater Sci Eng C Mater Biol Appl. 2018;82:163-181. [15] KIM HD, AMIRTHALINGAM S, KIM SL, et al. Biomimetic Materials and Fabrication Approaches for Bone Tissue Engineering. Adv Healthc Mater. 2017;6(23):1-18. [16] MONDSCHEIN RJ, KANITKAR A, WILLIAMS CB, et al. Polymer structure-property requirements for stereolithographic 3D printing of soft tissue engineering scaffolds. Biomaterials. 2017;140:170-188. [17] SALMORIA GV, PEREIRA RV, FREDEL MC, et al. Properties of PLDLA/bioglass scaffolds produced by selective laser sintering. Polym Bull (Berl). 2017;75(3):1299-1309. [18] SHEIKH Z, HAMDAN N, IKEDA Y, et al. Natural graft tissues and synthetic biomaterials for periodontal and alveolar bone reconstructive applications: a review. Biomater Res. 2017;21:9. [19] SHUAI C, SHUAI C, FENG P, et al. Antibacterial Capability, Physicochemical Properties, and Biocompatibility of nTiO₂Incorporated Polymeric Scaffolds. Polymers (Basel). 2018;10(3):328. [20] ARUMUGAM B, BALAGANGADHARAN K, SELVAMURUGAN N. Syringic acid, a phenolic acid, promotes osteoblast differentiation by stimulation of Runx2 expression and targeting of Smad7 by miR-21 in mouse mesenchymal stem cells. J Cell Commun Signal. 2018;12(3):561-573. [21] CHEN J, ZHANG D, ZHANG T, et al. Effect of the vascularized bone components on the survival of vascularized composite allografts. J Surg Res. 2018;224:132-138. [22] MURPHY CM, HAUGH MG, O’BRIEN FJ. The effect of mean pore size on cell attachment, proliferation and migration in collagen-glycosaminoglycan scaffolds for bone tissue engineering. Biomaterials. 2010;31(3):461-466. [23] PRASADH S, WONG RCW. Unraveling the mechanical strength of biomaterials used as a bone scaffold in oral and maxillofacial defects. Oral Sci Int. 2018;15(2):48-55. [24] SCHREIVOGEL S, KUCHIBHOTLA V, KNAUS P, et al. Load-induced osteogenic differentiation of mesenchymal stromal cells is caused by mechano-regulated autocrine signaling. J Tissue Eng Regen Med. 2019;13(11):1992-2008. [25] SU X, WANG J, KANG H, et al. Effects of dynamic radial tensile stress on fibrocartilage differentiation of bone marrow mesenchymal stem cells. Biomed Eng Online. 2020;19(1):8. [26] AAMODT JM, GRAINGER DW. Extracellular matrix-based biomaterial scaffolds and the host response. Biomaterials. 2016;86:68-82. [27] MONTALBANO G, BORCIANI G, PONTREMOLI C, et al. Development and Biocompatibility of Collagen-Based Composites Enriched with Nanoparticles of Strontium Containing Mesoporous Glass. Materials (Basel). 2019;12(22):2-17. [28] CUNNIFFE GM, DICKSON GR, PARTAP S, et al. Development and characterisation of a collagen nano-hydroxyapatite composite scaffold for bone tissue engineering. J Mater Sci Mater Med. 2010;21(8):2293-2298. [29] ZHOU C, YE X, FAN Y, et al. Biomimetic fabrication of a three-level hierarchical calcium phosphate/collagen/hydroxyapatite scaffold for bone tissue engineering. Biofabrication. 2014;6(3):035013. [30] LEE WK, LIM YY, LEOW AT, et al. Biosynthesis of agar in red seaweeds: A review. Carbohydr Polym. 2017;164:23-30. [31] ZHANG BG, MYERS DE, WALLACE GG, et al. Bioactive coatings for orthopaedic implants-recent trends in development of implant coatings. Int J Mol Sci. 2014;15(7):11878-11921. [32] MADHUMATHI K, SHALUMON KT, RANI VV, et al. Wet chemical synthesis of chitosan hydrogel-hydroxyapatite composite membranes for tissue engineering applications. Int J Biol Macromol. 2009;45(1):12-15. [33] WANG M, CHENG X, ZHU W, et al. Design of biomimetic and bioactive cold plasma-modified nanostructured scaffolds for enhanced osteogenic differentiation of bone marrow-derived mesenchymal stem cells. Tissue Eng Part A. 2014;20(5-6):1060-1071. [34] KANG SW, KIM JS, PARK KS, et al. Surface modification with fibrin/hyaluronic acid hydrogel on solid-free form-based scaffolds followed by BMP-2 loading to enhance bone regeneration. Bone. 2011;48(2):298-306. [35] CATANZANO O, SORIENTE A, LA GATTA A, et al. Macroporous alginate foams crosslinked with strontium for bone tissue engineering. Carbohydr Polym. 2018;202:72-83. [36] 孙磊,张柏青,陈磊,等.海藻酸钠凝胶复合异种骨构建组织工程骨及体内成骨[J].中国修复重建外科杂志,2008,22(6):732-736. [37] NANDITHA S, CHANDRASEKARAN B, MUTHUSAMY S, et al. Apprising the diverse facets of Platelet rich fibrin in surgery through a systematic review. Int J Surg. 2017;46:186-194. [38] SOUMYA S, SREEREKHA PR, MENON D, et al. Generation of a biomimetic 3D microporous nano-fibrous scaffold on titanium surfaces for better osteointegration of orthopedic implants. J Mater Chem. 2012;22(5):1904-1915. [39] ING Y, QUAN C, LIU B, et al. A Mini Review on the Functional Biomaterials Based on Poly(lactic acid) Stereocomplex. Polymers (Basel). 2016;56(2):262-286. [40] KIM DY, KWON DY, KWON JS, et al. Stimuli-Responsive InjectableIn situ-Forming Hydrogels for Regenerative Medicines. Polymers (Basel). 2015;55(3):407-452. [41] LIN Y J, HUANG CC, WAN W L, et al. Recent advances in CO(2) bubble-generating carrier systems for localized controlled release. Biomaterials. 2017;133:154-164. [42] 尹浩月,邓久鹏,马丽娟,等.冷冻干燥法制备聚乳酸多孔支架[J].生物医学工程研究,2019,38(2):215-218,246. [43] 王营,王曦龙,章俊,等.绿色荧光蛋白标记大鼠骨骼肌卫星细胞与聚羟基乙酸的生物相容性[J].中华实验外科杂志,2018,35(11): 2014-2016. [44] 黄天意,刘璐,王晓容.纤维增强聚甲基丙烯酸甲酯材料的研究进展[J].口腔医学,2019,39(8):753-756. [45] 高山,周方,吕扬,等.新型多孔聚甲基丙烯酸甲酯骨水泥的制备及性能分析[J].中国组织工程研究,2019,23(2):204-210. [46] 傅娜,罗晓丁,焦铁军,等.骨组织工程中应用的聚己内酯-聚乙二醇-聚己内酯静电纺丝支架[J].中国组织工程研究,2019,23(22): 3445-3450. [47] FREZZO JA, MONTCLARE JK. Natural Composite Systems for Bioinspired Materials. Adv Exp Med Biol. 2016;940:143-166. [48] KOUPAEI N, KARKHANEH A. Porous crosslinked polycaprolactone hydroxyapatite networks for bone tissue engineering. Tissue Eng Regen Med. 2016;13(3):251-260. [49] ISIKLI C, HASIRCI V, HASIRCI N. Development of porous chitosan-gelatin/hydroxyapatite composite scaffolds for hard tissue-engineering applications. J Tissue Eng Regen Med. 2012;6(2):135-43. [50] ZHANG H, MAO X, DU Z, et al. Three dimensional printed macroporous polylactic acid/hydroxyapatite composite scaffolds for promoting bone formation in a critical-size rat calvarial defect model. Sci Technol Adv Mater. 2016;17(1):136-148. [51] ZHANG H, MAO X, ZHAO D, et al. Three dimensional printed polylactic acid-hydroxyapatite composite scaffolds for prefabricating vascularized tissue engineered bone: An in vivo bioreactor model. Sci Rep. 2017; 7(1):15255. [52] 段钢,陈宏亮,郭开,等.3D打印β-磷酸三钙仿生骨支架修复兔股骨髁骨缺损[J].骨科临床与研究杂志,2020,5(4):243-250. [53] 胡爽,李春梅,张帅源,等.口腔修复膜和β-磷酸三钙治疗颌骨囊肿术后骨缺损的临床价值[J].华西口腔医学杂志,2020,38(5):541-545. [54] DOROZHKIN SV. Bioceramics of calcium orthophosphates. Biomaterials. 2010;31(7):1465-1485. [55] SMITH BT, SHUM J, WONG M, et al. Bone Tissue Engineering Challenges in Oral & Maxillofacial Surgery. Adv Exp Med Biol. 2015;881:57-78. [56] 王福科,李彦林,王国梁,等.复合骨形成蛋白和碱性成纤维细胞生长因子的双相陶瓷样生物活性骨修复指骨缺损[J].中国组织工程研究与临床康复,2010,14(47):8885-8888. [57] ZHANG G, LIU W, WANG R, et al. The Role of Tantalum Nanoparticles in Bone Regeneration Involves the BMP2/Smad4/Runx2 Signaling Pathway. Int J Nanomedicine. 2020;15:2419-2435. [58] 王茜,滕雪峰,甘洪全,等.国产多孔钽对兔成骨细胞生物学行为及功能的影响[J].中国组织工程研究,2018,22(30):4757-4762. [59] WANG X, ZHU Z, XIAO H, et al. Three-Dimensional, MultiScale, and Interconnected Trabecular Bone Mimic Porous Tantalum Scaffold for Bone Tissue Engineering. ACS Omega. 2020;5(35):22520-22528. [60] 杨伽捷,朱裕昌,杨春喜.多孔金属骨组织支架的研究进展[J].实用骨科杂志,2018,24(2):148-152. [61] 李大成,付莹,陈望军,等.多孔钛合金支撑棒在踝关节损伤中的应用及生物力学性能[J].中国组织工程研究,2017,21(34): 5413-5417. [62] CLAINCHE TL, LINKLATER D, WONG S, et al. Mechano-Bactericidal Titanium Surfaces for Bone Tissue Engineering. ACS Appl Mater Interfaces. 2020;12(43):48272-48283. [63] ZHANG X, CHEN Q, MAO X. Magnesium Enhances Osteogenesis of BMSCs by Tuning Osteoimmunomodulation. Biomed Res Int. 2019; 2019:7908205. [64] 王勇平,刘小荣,张炳春,等.镁合金支架对成骨细胞功能的影响[J].中国组织工程研究,2016,20(34):5021-5026. [65] ZHANG YQ, LI Y, LIU H, et al. Mechanical and Biological Properties of a Biodegradable Mg-Zn-Ca Porous Alloy. Orthop Surg. 2018;10(2): 160-168. [66] SOHN HS, OH JK. Review of bone graft and bone substitutes with an emphasis on fracture surgeries. Biomater Res. 2019;23:9. [67] TURNBULL G, CLARKE J, PICARD F, et al. 3D bioactive composite scaffolds for bone tissue engineering. Bioact Mater. 2018;3(3):278-314 |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [3] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [4] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [5] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [6] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [7] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [8] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [9] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [10] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [11] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [12] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [13] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [14] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [15] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||