Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (10): 1533-1539.doi: 10.12307/2024.319
Previous Articles Next Articles
Artificial dermis combined with autologous scar epidermis composite transplantation in repair of joint site scar deformities in the later stage of extensive burns
Fu Quanyou, Xing Fuxi, Li Lin, Li Yong, Liu Jisong
- Bengbu Third People’s Hospital Affiliated to Bengbu Medical College, Bengbu 233000, Anhui Province, China
-
Received:2023-03-30Accepted:2023-05-15Online:2024-04-08Published:2023-08-18 -
Contact:Liu Jisong, MD, Associate chief physician, Bengbu Third People’s Hospital Affiliated to Bengbu Medical College, Bengbu 233000, Anhui Province, China -
About author:Fu Quanyou, Master candidate, Physician, Bengbu Third People’s Hospital Affiliated to Bengbu Medical College, Bengbu 233000, Anhui Province, China -
Supported by:Scientific Research Project of Anhui Provincial Health Commission, No. (2021)74 (to LJS)
CLC Number:
Cite this article
Fu Quanyou, Xing Fuxi, Li Lin, Li Yong, Liu Jisong. Artificial dermis combined with autologous scar epidermis composite transplantation in repair of joint site scar deformities in the later stage of extensive burns[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(10): 1533-1539.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
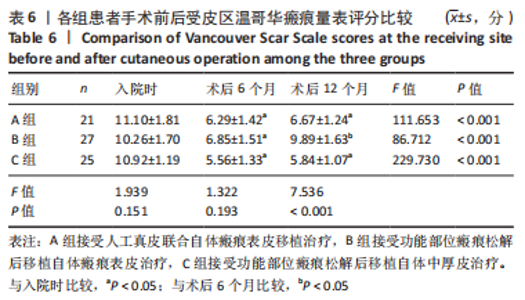
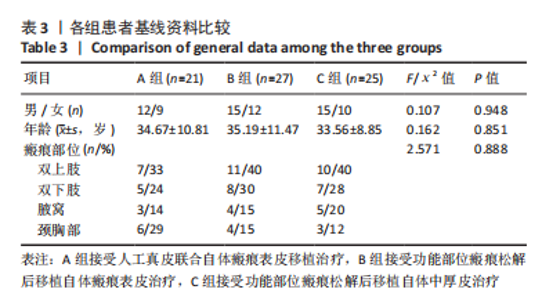
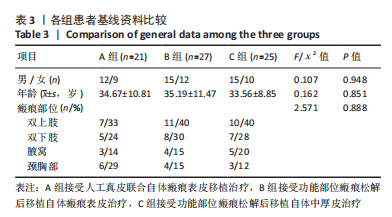
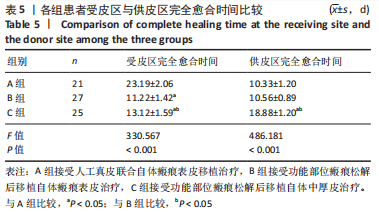
单因素方差分析结果显示,3 组患者受皮区与供皮区完全愈合时间比较差异均有显著性意义(P < 0.05);进一步采用LSD法两两比较结果显示,A组患者受皮区完全愈合时间长于B、C组(P < 0.05),C组患者受皮区完全愈合时间长于B组,C组患者供皮区完全愈合时间长于A、B组(P < 0.05)。 2.6 各组患者手术前后受皮区VSS评分比较 各组患者入院时及术后6,12 个月受皮区VSS评分比较结果,见表6。单因素方差分析结果显示,3 组患者入院时受皮区VSS评分比较差异无显著性意义(P > 0.05);独立样本t检验结果显示,A组与B组患者术后6 个月受皮区VSS评分比较差异无显著性意义(P > 0.05),B组患者术后12 个月受皮区VSS评分明显高于A、C组(P < 0.05)。"
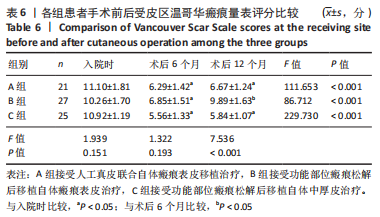
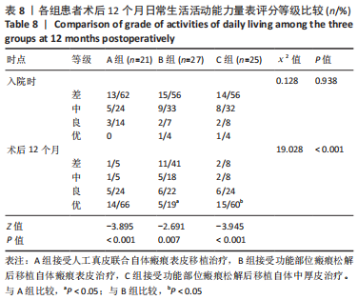
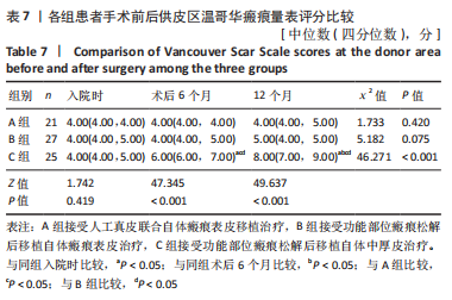
Friedman检验结果显示,A、B组组内,患者入院时及术后6,12 个月供皮区VSS评分比较差异无显著性意义(P > 0.05);C组患者入院时及术后6,12 个月供皮区VSS评分比较差异有显著性意义(P < 0.001),进一步采用Nemenyi法进行两两比较结果显示,患者术后6,12 个月供皮区VSS评分高于入院时(P < 0.05),术后12 个月供皮区VSS评分高于术后6 个月(P < 0.05)。 Kruskal-Wallis H检验结果显示,3 组患者入院时供皮区VSS评分比较差异无显著性意义(P > 0.05),3 组患者术后6,12 个月供皮区VSS评分比较差异有显著性意义(P < 0.001),进一步采用Nemenyi法进行两两比较结果显示,C组患者术后6,12 个月时供皮区VSS评分均高于A、B组(P < 0.05)。 2.8 各组患者关节部位功能改善情况 各组患者入院时及术后12 个月关节部位功能改善分析,见表8。Kruskal-Wallis H检验结果显示,3 组患者入院时ADL评分等级比较差异无显著性意义(P > 0.05),3 组患者术后12 个月ADL评分等级比较差异差异有显著性意义(P < 0.001);进一步采用Nemenyi法进行两两比较结果显示,A、C组优等级比例高于B组(P < 0.05)。"
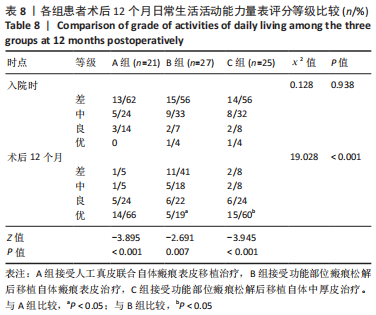
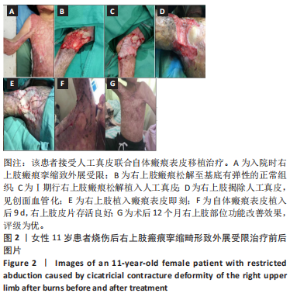
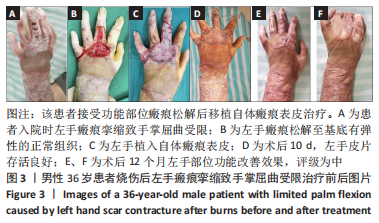
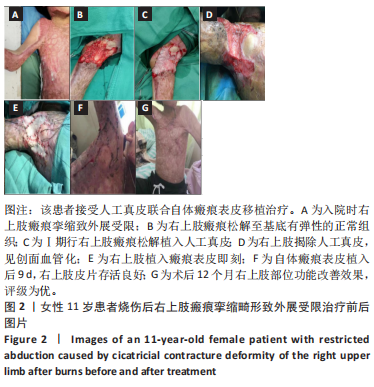
Wilcoxon符号秩检验结果显示,3 组患者术后12 个月ADL评分等级均优于入院时(P < 0.05,P < 0.001)。 2.9 不良反应 3 组患者随访结束后未发生与人工真皮及自体皮相关的不良反应。 2.10 典型病例 病例1:11 岁女性患者,因火焰烧伤面颈部、躯干、四肢2 年余入院。入院诊断:烧伤面积50%总体表面积,右上肢瘢痕挛缩畸形致外展受限。入院后完善相关检查,Ⅰ期行右腋窝部位瘢痕松解植入人工真皮,术后7 d去除加压敷料,观察术区人工真皮有无积血积液及血管化情况。术后14 d行Ⅱ期手术,去除包扎敷料,确认外层硅胶膜与其下组织完全分离后揭除人工真皮;将取皮刀取皮厚度调整至 0.2 mm,于右大腿切取相应面积瘢痕表皮,移植于血管化的人工真皮上,皮钉固定。术后5 d去除加压敷料,观察术区皮片存活情况。出院后6,12 个月分别进行随访,受皮区VSS评分较入院时明显降低,供皮区VSS评分较入院时无明显差异,右上肢外展障碍得到纠正,ADL评级为优。该患者治疗前后资料图片,见图2。"
| [1] HENDRIKS T, BOTMAN M, DE HAAS L, et al. Burn scar contracture release surgery effectively improves functional range of motion, disability and quality of life: A pre/post cohort study with long-term follow-up in a Low- and Middle-Income Country. Burns. 2021; 47(6):1285-1294. [2] ZAHOREC P, SARKOZYOVA N, FERANCIKOVA N, et al. Autologous mesenchymal stem cells application in post-burn scars treatment: a preliminary study. Cell Tissue Bank. 2021;22(1):39-46. [3] KONDO A, DOHI T, IZUMI N, et al. Anterior Neck-scar Contracture Reconstruction Using a Long Skin-pedicled Flap. Plast Reconstr Surg Glob Open. 2021;9(2):e3404. [4] XIAO H, LIU R, LIU X, et al. Reconstruction of Severe Neck Scar Contracture After Electrical Injury. J Craniofac Surg. 2022;33(1):203-205. [5] DE FRANCESCO F, BUSATO A, MANNUCCI S, et al. Artificial dermal substitutes for tissue regeneration: comparison of the clinical outcomes and histological findings of two templates. J Int Med Res. 2020;48(8):1220745060. [6] DI HP, MU XL, SHI JJ, et al. [A prospective randomized controlled study of the effectiveness of artificial dermis combined with split-thickness skin for repairing wounds with bone and tendon exposure in hands and feet]. Zhonghua Shao Shang Za Zhi. 2021;37(12):1130-1136. [7] CHEN L, WU YT, GU XY, et al. Magnolol, a natural aldehyde dehydrogenase-2 agonist, inhibits the proliferation and collagen synthesis of cardiac fibroblasts. Bioorg Med Chem Lett. 2021;43: 128045. [8] SARKOZYOVA N, DRAGUNOVA J, BUKOVCAN P, et al. Preparation and processing of human allogenic dermal matrix for utilization in reconstructive surgical procedures. Bratisl Lek Listy. 2020;121(6): 386-394. [9] SONMEZ ES. A New Splint for Dorsal Foot Burns. J Burn Care Res. 2018; 39(2):308-310. [10] 靳雪义,张宏,张岿.人工真皮联合瘢痕断层皮片修复治疗在烧伤后四肢大关节部位瘢痕增生挛缩畸形患者中的应用[J].中国医疗美容,2020,10(12):49-53. [11] 刘洋,张宜澜,黄亚兰,等.人工真皮联合碱性成纤维细胞生长因子在瘢痕和皮肤深度创面整复中的临床应用[J].中华烧伤杂志, 2016,32(4):198-203. [12] 高磊,秦新愿,李天博,等.脱细胞同种异体真皮与自体刃厚皮联合移植修复糖尿病足创面[J].中国组织工程研究,2022,26(14): 2138-2143. [13] 刘继松,宋德恒,赵刚宏,等.新型生物敷料Ⅱ型在二度烧伤创面中的应用[J].中华全科医学,2018,16(5):740-743. [14] KANAPATHY M, MOSAHEBI A. Comparative study on the donor site aesthetic outcome between epidermal graft and split-thickness skin graft. Int Wound J. 2019;16(2):354-359. [15] 王建强,刘江月.脱细胞异体真皮与PELNAC分别联合表皮移植治疗烧伤瘢痕的效果对比[J].中国实用医刊,2022,49(3):39-42. [16] POWELL HM, NEDELEC B. Mechanomodulation of Burn Scarring Via Pressure Therapy. Adv Wound Care (New Rochelle). 2022;11(4): 179-191. [17] WANG J, WU J, XU M, et al. A comprehensive reconstruction strategy for moderate to severe faciocervical scar contractures. Lasers Med Sci. 2021;36(6):1275-1282. [18] 席云峰,张斌,苏伟,等.微粒皮移植异种脱细胞真皮基质敷料覆盖术治疗大面积烧伤创面的效果[J]. 临床医学研究与实践,2019, 4(31):6-8. [19] CHANG LS, KIM YH, KIM SW. Reconstruction of burn scar contracture deformity of the extremities using thin thoracodorsal artery perforator free flaps. ANZ J Surg. 2021;91(9):E578-E583. [20] SCUDERI N, FIORAMONTI P, FANELLI B, et al. The use of dermal regeneration template (Pelnac(R)) in a complex upper limb trauma: the first Italian case report. Eur Rev Med Pharmacol Sci. 2019;23(13): 5531-5534. [21] MEULI JN, PANTET O, BERGER MM, et al. Massive Burns: Retrospective Analysis of Changes in Outcomes Indicators Across 18 Years. J Burn Care Res. 2022;43(1):232-239. [22] CHEN XD, RUAN SB, LIN ZP, et al. Effects of porcine acellular dermal matrix treatment on wound healing and scar formation: Role of Jag1 expression in epidermal stem cells. Organogenesis. 2018;14(1):25-35. [23] HAHN HM, COOK KH, LEE IJ, et al. Use of Acellular Dermal Matrix in Treatment of Congenital Muscular Torticollis in Patients Over Eight Years of Age. J Craniofac Surg. 2017;28(3):610-615. [24] MATSUMURA H, MATSUSHIMA A, UEYAMA M, et al. Application of the cultured epidermal autograft “JACE((R)”) for treatment of severe burns: Results of a 6-year multicenter surveillance in Japan. Burns. 2016;42(4):769-776. [25] CHENG G, HARDY M, ZIELONKA J, et al. Mitochondria-targeted magnolol inhibits OXPHOS, proliferation, and tumor growth via modulation of energetics and autophagy in melanoma cells. Cancer Treat Res Commun. 2020;25:100210. [26] 李兵园,许明火,宋慧锋,等.瘢痕表皮角蛋白的变化规律及正常表皮细胞培养液对成纤维细胞胶原合成的影响[J].感染、炎症、修复,2013,14(2):80-83. [27] 周杰,罗艺,徐刚,等.脱细胞真皮基质加自体瘢痕表皮在瘢痕挛缩畸形整复中的应用[J].中国美容医学,2012,21(11):1498. [28] 崔泽龙.烧伤瘢痕表皮结合组织工程真皮治疗瘢痕的临床研究[D].南宁:广西医科大学,2019. [29] HUANG W, CHEN Y, WANG N, et al. The Efficacy and Safety of Acellular Matrix Therapy for Diabetic Foot Ulcers: A Meta-Analysis of Randomized Clinical Trials. J Diabetes Res. 2020;2020:6245758. [30] KLAMA-BARYLA A, KITALA D, LABUS W, et al. Is Transgenic Porcine Skin as Good as Allogeneic Skin for Regenerative Medicine? Comparison of Chosen Properties of Xeno- and Allogeneic Material. Transplant Proc. 2020;52(7):2208-2217. [31] 贾晓明.异种(体)生物材料与创面修复[J].中华损伤与修复杂志(电子版),2020,15(5):341-346. [32] KASHIMURA T, NAGASAKI K, HORIGOME M, et al. Selection of Artificial Dermis for Shortening Treatment Period: Integra versus Pelnac. Plastic and reconstructive surgery. Global Open. 2021;9(6):e3599. [33] LV Z, YU L, WANG Q, et al. Dermal regeneration template and vacuum sealing drainage for treatment of traumatic degloving injuries of upper extremity in a single-stage procedure. ANZ J Surg. 2019;89(7-8): 950-954. [34] HALL C, HARDIN C, CORKINS CJ, et al. Pathophysiologic Mechanisms and Current Treatments for Cutaneous Sequelae of Burn Wounds. Compr Physiol. 2017;8(1):371-405. [35] LV Z, WANG Q, JIA R, et al. Pelnac(R) Artificial Dermis Assisted by VSD for Treatment of Complex Wound with Bone/Tendon Exposed at the Foot and Ankle, A Prospective Study. J Invest Surg. 2020;33(7):636-641. [36] ZHAO F, YANG X, LI W, et al. Classification of Obviously Asymmetric Palpebral Fissures and Correction Based on Double Eyelid Surgery of the Primary Type. J Craniofac Surg. 2020;31(2):404-407. [37] MA Z, MO R, CHEN C, et al. Surgical treatment of joint burn scar contracture: a 10-year single-center experience with long-term outcome evaluation. Ann Transl Med. 2021;9(4):303. [38] MURRAY RZ, WEST ZE, COWIN AJ, et al. Development and use of biomaterials as wound healing therapies. Burns Trauma. 2019;7:2. [39] HAO Z. Application of Pelnac(R) Artificial Dermis Combined with VSD in the Repair of Limb Wounds. J Invest Surg. 2020;33(7):642-643. [40] CHEN S, ZHENG LW, LIU W, et al. [Clinical effects of artificial dermis combined with vacuum sealing drainage and autologous split-thickness skin graft in repair of scar contracture deformity after extensive burn]. Zhonghua Shao Shang Za Zhi. 2019;35(8):608-610. |
| [1] | Zhou Ying, Zhang Huan, Liao Song, Hu Fanqi, Yi Jing, Liu Yubin, Jin Jide. Immunomodulatory effects of deferoxamine and interferon gamma on human dental pulp stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1012-1019. |
| [2] | Chi Kai, Wu Lei, Chen Long-jin, Li Yong-lin. Tissue-engineered skin for skin wound repair: construction by human acellular dermal matrix combined with bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(26): 4179-4183. |
| [3] |
Sun Hui-zhe, Tian Wei, Zeng Liang, Qiu Jin-yun, Zhang Qian.
Preparation of porcine small intestinal submucosa sponge and observation of cell adhesion
[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(34): 5487-8492.
|
| [4] |
Qian Li-ke, Qian Ming-yuan.
Treatment outcomes of human epidermal stem cells/porcine acellular dermal tissue-engineered skin in the repair of full-thickness skin defects
[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(2): 227-231.
|
| [5] | Wang Tao, Zhang Tao, Feng Shi-qing, Guo Hong-gang, Zheng Yong-fa. Autologous skin grafting, vacuum sealing drainage and external fixation for repair of complex and severe open fracture of the elbow joint [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(30): 4915-4920. |
| [6] | Liu Xiao-zhou, Xu Hai-dong, Zhao Jian-ning. Vacuum-sealing drainages based on biological versus synthetic dressings in wound healing of skin grafting [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(8): 1295-1300. |
| [7] | Zhang Ming-zhu, Wang Jian-hua, Li Hu, Dong Yun-feng, Qi Chang-chun, Guo Bao-wen, Wang Yong-ling, Liu Xiao-yan, Li Yun-feng, Zhang Xiao-hui, Liu Ying, Li Xing-hua, Wang Hong-feng, Yu Qiang. Thin-thickness versus blade-thickness micro-skin pulping covered with heterogeneous skin for repair of burn wounds [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(46): 7417-7421. |
| [8] | Zhao Ji-hong, Fang Xin. Vacuum sealing drainage plus skin transplantation repair skin soft tissue defects in tibia and fibula complicated fractures [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(20): 3246-3251. |
| [9] | Tian Liang, Qiu Lin, Fu Yue-xian, Tian Xiao-fei, Liu Yan, Xiao Jun. New biological dermis cover Pelnac® in wound healing of children with severe trauma [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(16): 2601-2606. |
| [10] | Yao Hui, Lu Hua-ding, Xu Yi-chun, Zhao Hui-qing, Lv Lu-lu. Vacuum sealing drainage based on wound surface dressing biomaterials for repairing soft tissue defects of the foot and ankle [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(16): 2607-2612. |
| [11] | Cao Li-ying, Ding Xuan-xi, Yang Sheng-ping, Wang Guan, Jiang Ming-jing. Expression of transforming growth factor beta 1 of cryopreserved skin allograft [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(18): 3231-3238. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||