Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (6): 908-913.doi: 10.12307/2022.175
Previous Articles Next Articles
Mid-term effect of Isobar EVO non-fusion dynamic fixation in the treatment of adjacent segment disease after lumbar fusion
Song Jiawei, Yang Yongdong, Yu Xing, Yang Jizhou, Wang Fengxian, Qu Yi, Bi Lianyong
- Department of Orthopedics, Dongzhimen Hospital, Beijing University of Chinese Medicine, Beijing 100700, China
-
Received:2021-04-30Revised:2021-05-11Accepted:2021-06-15Online:2022-02-28Published:2021-12-07 -
Contact:Yu Xing, Doctoral supervisor, Chief physician, Professor, Department of Orthopedics, Dongzhimen Hospital, Beijing University of Chinese Medicine, Beijing 100700, China -
About author:Song Jiawei, Master candidate, Department of Orthopedics, Dongzhimen Hospital, Beijing University of Chinese Medicine, Beijing 100700, China Yang Yongdong, MD, Associate researcher, Department of Orthopedics, Dongzhimen Hospital, Beijing University of Chinese Medicine, Beijing 100700, China Song Jiawei and Yang Yongdong contributed equally to this article. -
Supported by:the Weifang Aojing Biomimetic Bone Multi-center Clinical Research Project (to YX)
CLC Number:
Cite this article
Song Jiawei, Yang Yongdong, Yu Xing, Yang Jizhou, Wang Fengxian, Qu Yi, Bi Lianyong. Mid-term effect of Isobar EVO non-fusion dynamic fixation in the treatment of adjacent segment disease after lumbar fusion[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 908-913.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
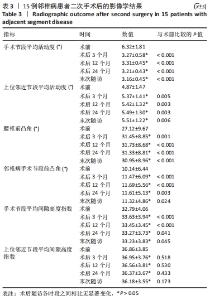
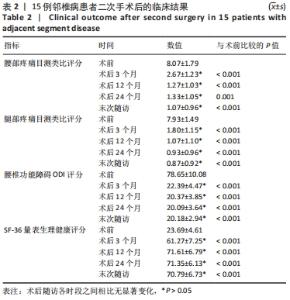
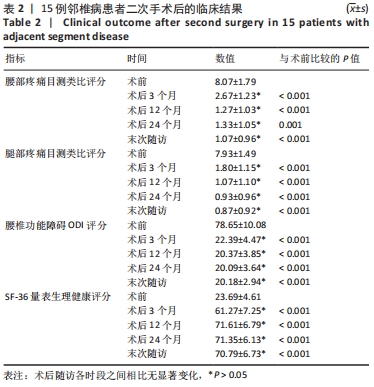
2.3 影像学结果 手术后至末次随访时,所有15例患者的腰椎X射线片均显示无内置物松动。影像学测量结果见表 3:术后3个月手术节段平均活动度(β)显著下降(P < 0.05),至末次随访时平均活动度较术前均明显下降(P < 0.05),与术后3个月比较差异无显著性意义(P > 0.05)。术后3个月上位邻近节段平均活动度(γ)、手术节段平均前凸角(α)、平均腰椎前凸角(LL)及手术节段平均间隙高度指数(DHo)均较术前明显增加(P < 0.05),末次随访时上述4个指标均较术前显著增加(P < 0.05),但与术后3个月比较差异无显著性意义(P > 0.05)。术后3个月至末次随访,上位邻近节段平均间隙高度比(DHu)表现出逐渐下降的趋势,但未到达统计学差异(P > 0.05)。"
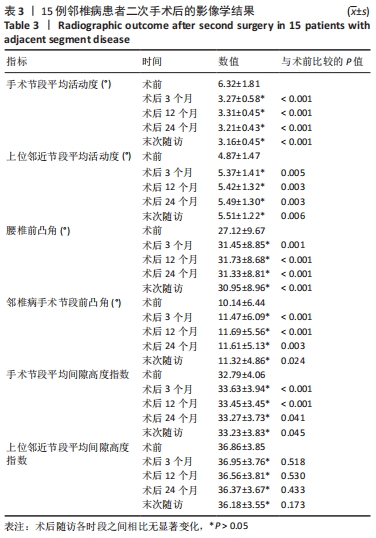
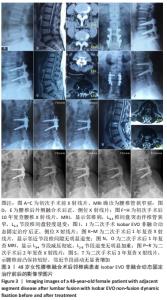
2.4 典型病例 48岁女性,因腰椎管狭窄症在北京中医药大学东直门医院行腰椎后外侧融合(L5-S1)手术,术后症状缓解并恢复正常生活。于初次术后7年出现腰腿痛,行腰椎MRI后诊断为腰椎融合术后邻椎病,予保守治疗后症状减轻。后症状间断发作并于初次术后10年症状加重,复查腰椎MRI示L3-4椎间盘突出伴椎管狭窄较之前加重,L2-3节段椎间盘轻度退变。遂于初次术后10年再手术取出原内固定,减压L3-4节段并使用Isobar EVO非融合动态固定。再手术后症状缓解,1年后复查腰椎X射线片示腰椎前凸保持良好,腰椎活动度及椎间活动度良好,邻近节段椎间隙无明显退变。腰椎MRI示L3-4节段减压彻底,L2-3节段退变无明显加重。再手术后2年和3年时复查腰椎X射线片示腰椎前凸保持较好,邻近节段活动无显著增加,患者手术前后的影像学图片,见图3。"

| [1] PARK P, GARTON HJ, GALA VC, et al. Adjacent segment disease after lumbar or lumbosacral fusion: review of the literature. Spine. 2004;29:1938-1944. [2] HASHIMOTO K, AIZAWA T, KANNO H, et al. Adjacent segment degeneration after fusion spinal surgery-a systematic review. Int Orthop. 2019;43:987-993. [3] 刘明,勘武生,李鹏,等.髓核摘除联合Isobar非融合内固定治疗腰椎间盘突出症[J].中国修复重建外科杂志,2011,25(2):229-234. [4] 张晓哲,王庆甫,赵子义,等.Isobar TTL系统治疗腰椎退行性疾病的疗效及术后融合率的探讨[J].中国骨伤,2019,32(10):914-918. [5] OHNHAUS EE, ADLER R. Methodological problems in the measurement of pain: a comparison between the verbal rating scale and the visual analogue scale. Pain. 1975;1(4):379-384. [6] FAIRBANK JC, PYNSENT PB. The Oswestry Disability Index. Spine (Phila Pa 1976). 2000;25(22):2940-2953. [7] BRAZIER JE, HARPER R, JONES NM, et al. Validating the SF-36 health survey questionnaire: new outcome measure for primary care. BMJ. 1992;305(6846): 160-164. [8] SASANI M, AYDIN AL, OKTENOGLU T, et al. The combined use of a posterior dynamic transpedicular stabilization system and a prosthetic disc nucleus device in treating lumbar degenerative disc disease with disc herniations. SAS J. 2008;2:130-136. [9] FORMICA M, CAVAGNARO L, BASSO M, et al. Is it possible to preserve lumbar lordosis after hybrid stabilization? Preliminary results of a novel rigid-dynamic stabilization system in degenerative lumbar pathologies. Europ Spine J. 2015; 24 Suppl 7:849-854. [10] XIA XP, CHEN HL, CHENG HB. Prevalence of adjacent segment degeneration after spine surgery: a systematic review and meta-analysis. Spine. 2013;38: 597-608. [11] SEARS WR, SERGIDES IG, KAZEMI N, et al. Incidence and prevalence of surgery at segments adjacent to a previous posterior lumbar arthrodesis. Spine J. 2011;11(1):11-20. [12] OKUDA S, MIYAUCHI A, ODA T, et al. Surgical complications of posterior lumbar interbody fusion with total facetectomy in 251 patients. J Neurosurg Spine. 2006;4:304-309. [13] TELFEIAN AE. Transforaminal Endoscopic Surgery for Adjacent Segment Disease After Lumbar Fusion. World Neurosurg. 2017;97:231-235. [14] GREINER-PERTH R, SELLHAST N, PERLER G, et al. Dynamic posterior stabilization for degenerative lumbar spine disease: a large consecutive case series with long-term follow-up by additional postal survey. Eur Spine J. 2016;25:2563-2570. [15] VERESCIAGINA K, MEHRKENS A, SCHAREN S, et al. Minimum ten-year follow-up of spinal stenosis with degenerative spondylolisthesis treated with decompression and dynamic stabilization. J Spine Surg. 2018;4:93-101. [16] KANER T, OZER AF. Dynamic stabilization for challenging lumbar degenerative diseases of the spine: a review of the literature. Adv Orthop. 2013;2013: 753470. [17] NAKASHIMA H, KAWAKAMI N, TSUJI T, et al. Adjacent Segment Disease After Posterior Lumbar Interbody Fusion: Based on Cases With a Minimum of 10 Years of Follow-up. Spine. 2015;40:E831-841. [18] CHOI KC, KIM JS, SHIM HK, et al. Changes in the adjacent segment 10 years after anterior lumbar interbody fusion for low-grade isthmic spondylolisthesis. Clin Orthop Relat Res. 2014;472:1845-1854. [19] BYDON M, MACKI M, KEREZOUDIS P, et al. The incidence of adjacent segment disease after lumbar discectomy: A study of 751 patients. J Clin Neurosci. 2017;35:42-46. [20] CARREON LY, GLASSMAN SD, HOWARD J. Fusion and nonsurgical treatment for symptomatic lumbar degenerative disease: a systematic review of Oswestry Disability Index and MOS Short Form-36 outcomes. Spine J. 2008;8:747-755. [21] LEE JC, KIM Y, SOH JW, et al. Risk factors of adjacent segment disease requiring surgery after lumbar spinal fusion: comparison of posterior lumbar interbody fusion and posterolateral fusion. Spine 2014;39:E339-345. [22] PAN A, HAI Y, YANG J, et al. Adjacent segment degeneration after lumbar spinal fusion compared with motion-preservation procedures: a meta-analysis. Eur Spine J. 2016;25:1522-1532. [23] HEO Y, PARK JH, SEONG HY, et al. Symptomatic adjacent segment degeneration at the L3-4 level after fusion surgery at the L4-5 level: evaluation of the risk factors and 10-year incidence. Eur Spine J. 2015;24:2474-2480. [24] KAITO T, HOSONO N, FUJI T, et al. Disc space distraction is a potent risk factor for adjacent disc disease after PLIF. Arch Orthop Trauma Surg. 2011;131:1499-1507. [25] AIKI H, OHWADA O, KOBAYASHI H, et al. Adjacent segment stenosis after lumbar fusion requiring second operation. J Orthop Sci. 2005;10:490-495. [26] CHEN BL, WEI FX, UEYAMA K, et al. Adjacent segment degeneration after single-segment PLIF: the risk factor for degeneration and its impact on clinical outcomes. Eur Spine J. 2011;20:1946-1950. [27] BAE JS, LEE SH, KIM JS, et al. Adjacent segment degeneration after lumbar interbody fusion with percutaneous pedicle screw fixation for adult low-grade isthmic spondylolisthesis: minimum 3 years of follow-up. Neurosurgery. 2010;67:1600-1607; discussion 1607-1608. [28] DISCH AC, SCHMOELZ W, MATZIOLIS G, et al. Higher risk of adjacent segment degeneration after floating fusions: long-term outcome after low lumbar spine fusions. J Spinal Disord Tech. 2008;21:79-85. [29] LU K, LILIANG PC, WANG HK, et al. Reduction in adjacent-segment degeneration after multilevel posterior lumbar interbody fusion with proximal DIAM implantation. Journal of neurosurgery. Spine. 2015;23:190-196. [30] PARKER SL, MENDENHALL SK, SHAU D, et al. Determination of minimum clinically important difference in pain, disability, and quality of life after extension of fusion for adjacent-segment disease. J Neurosurg Spine. 2012;16:61-67. [31] MASHALY H, PASCHEL EE, KHATTAR NK, et al. Posterior lumbar dynamic stabilization instead of arthrodesis for symptomatic adjacent-segment degenerative stenosis: description of a novel technique. Neurosurg Focus. 2016;40:E5. [32] BERTAGNOLI R, YUE JJ, FENK-MAYER A, et al. Treatment of symptomatic adjacent-segment degeneration after lumbar fusion with total disc arthroplasty by using the prodisc prosthesis: a prospective study with 2-year minimum follow up. J Neurosurg Spine. 2006;4:91-97. [33] BARREY C, PERRIN G, CHAMPAIN S. Pedicle-Screw-Based Dynamic Systems and Degenerative Lumbar Diseases: Biomechanical and Clinical Experiences of Dynamic Fusion with Isobar TTL. ISRN Orthop. 2013;2013:183702. [34] LI Z, LI F, YU S, et al. Two-year follow-up results of the Isobar TTL Semi-Rigid Rod System for the treatment of lumbar degenerative disease. J Clin Neurosci. 2013;20:394-399. [35] JI ZS, YANG H, YANG YH, et al. Analysis of clinical effect and radiographic outcomes of Isobar TTL system for two-segment lumbar degenerative disease: a retrospective study. BMC Surgery. 2020;20(1):15. [36] 曹宗锐,郑博,屈波,等.ISObar TTL动态固定系统治疗双节段腰椎椎间盘突出症:8年随访[J].中国组织工程研究,2019,23(32):5110-5116. |
| [1] | Guo Xiaohui, Song Xizheng, Xiang Hanrui, Kang Zhaorong, Li Daming, Kang Yu, Hu Jun, Sheng Kai. External spinal fixation elastic stress in the treatment of jumping spinal fracture [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 919-923. |
| [2] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [3] | Cai Xuan, Qin Jie, He Xijing, Dong Jun, Zhang Ting, Yang Wenlong, Wang Xiongxun, Wang Zili, Wang Dong, Li Haopeng, He Gaole, Lu Teng, Li Lingjiang. Three-dimensional printing motion-preserving cervical joint system implantation for treatment of cervical myelopathy: the first case report [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(36): 5810-5813. |
| [4] | Wu Chao, Gao Mingjie, Wang Jianzhong, Zhang Yunfeng, Yu Jinghong, Cai Yongqiang, Wang Haiyan, He Yujie, Tong Ling, Li Jiawei, Gao Shang, Wang Xing, Wu Min, Li Zhijun, Li Xiaohe. Finite element analysis of stress and displacement of Lenke 3 adolescent idiopathic scoliosis thoracolumbar spine [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(33): 5273-5280. |
| [5] | Huang Chenyi, Li Jingchi, Xu Wenqiang, Zhang Xiaoyu, Fang Zhongxin, Liu Zongchao. Capsule protection reduces the incidence risk of adjacent segment diseases after percutaneous endoscopic discectomy: a biomechanical analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4818-4822. |
| [6] | Gu Honglin, Zheng Xiaoqing, Liang Changxiang, Zeng Shixing, Zhan Shiqiang, Chang Yunbing. Long-term survival rate and reoperation of Wallis interspinous dynamic stabilization system for treatment of lumbar degenerative disc disease [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4863-4869. |
| [7] | Qin Yichuan, Zhao Bin, Yuan Jie, Xu Chaojian, Lü Jie Hao Jiaqi Wang Yongfeng. Effects of internal fixation types and osteoporosis on oblique lateral interbody fusion: three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4767-4773. |
| [8] | Yang Qin, Zhou Honghai, Chen Longhao, Zhong Zhong, Xu Yigao, Huang Zhaozhi. Research status and development trend of pelvic reconstruction techniques: a bibliometric and visual analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3718-3724. |
| [9] | Zhao Hongshun, A Jiancuo, Wang Deyuan, Xu Zhihua, Gao Shunhong. Factors affecting the height of early intervertebral space after lumbar interbody fusion via lateral approach [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3332-3336. |
| [10] | Zhang Chongfeng, Li Xianlin, Peng Weibing, Jia Hongsheng, Cai Lei. Treating lumbar disc herniation of blood stasis type with Chinese herbs, acupuncture, moxibustion, and massage: a Bayesian network Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(17): 2781-2788. |
| [11] |
Zhang Cong, Zhao Yan, Du Xiaoyu, Du Xinrui, Pang Tingjuan, Fu Yining, Zhang Hao, Zhang Buzhou, Li Xiaohe, Wang Lidong.
Biomechanical analysis of the lumbar spine and pelvis in adolescent
idiopathic scoliosis with lumbar major curve |
| [12] | Tuerhongjiang·Abuduresiti, Meng Xiangyu, Maihemuti·Yakufu, Wang Tiantang, Xieraili·Maimaiti, Dai Jifang, Wang Wei. Biomechanical advantages of percutaneous endoscopic lumbar discectomy for lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5768-5773. |
| [13] | Wang Jing, Xu Shuai, Liu Haiying. Hidden blood loss during posterior lumbar interbody fusion in lumbar spinal stenosis patients with and without rheumatoid arthritis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5307-5314. |
| [14] | Feng Fan, Cai Yi, Li Yingbo, Dong Junli, Wu Qun, Fan Yongzhi, Yan Hong. Comparison of seven surgical interventions for lumbar disc herniation: a network meta-analysis#br# [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 453-459. |
| [15] | Li You, Zheng Bengbeng, Wang Jiaming, Ma Yongsheng. Research and application of artificial cervical disc [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(12): 1941-1948. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||