Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (27): 4393-4399.doi: 10.3969/j.issn.2095-4344.0279
Previous Articles Next Articles
Changes in the flexion and extension muscle strength and motor function of the knee joint after anterior cruciate ligament reconstruction
Liu Zhi-cheng, Li Yan, Zhang Qi-liang
- Department of Bone Joint and Sports Medicine, Qingdao Municipal Hospital, Qingdao University, Qingdao 266000, Shandong Province, China
-
Online:2018-09-28Published:2018-09-28 -
Contact:Zhang Qi-liang, M.D., Associate chief physician, Department of Bone Joint and Sports Medicine, Qingdao Municipal Hospital, Qingdao University, Qingdao 266000, Shandong Province, China -
About author:Liu Zhi-cheng, Master, Department of Bone Joint and Sports Medicine, Qingdao Municipal Hospital, Qingdao University, Qingdao 266000, Shandong Province, China
CLC Number:
Cite this article
Liu Zhi-cheng, Li Yan, Zhang Qi-liang. Changes in the flexion and extension muscle strength and motor function of the knee joint after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(27): 4393-4399.
share this article
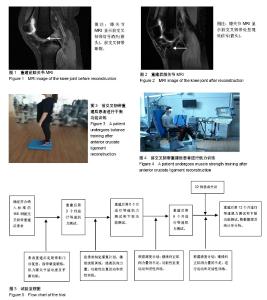
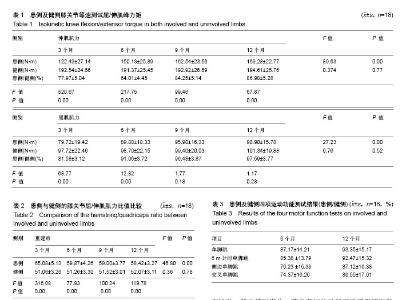
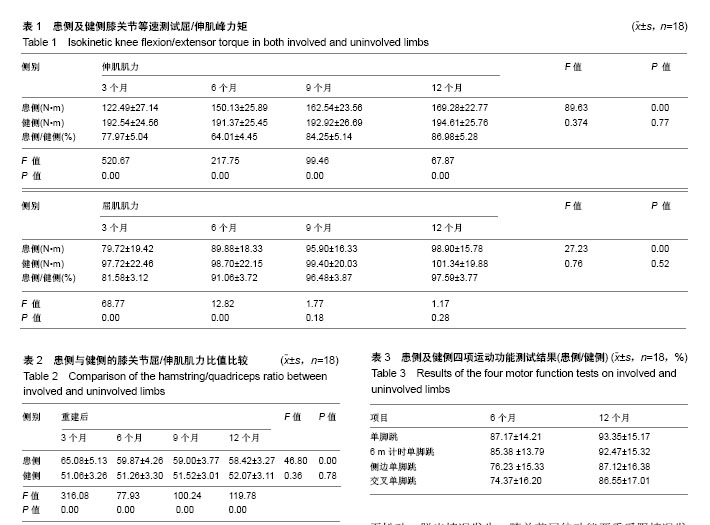
2.1 参与者数量分析 纳入随访研究对象150例,研究对象中只有118例完成全部测试,32例由于各种原因失访,失访率21.33%,见图5。 2.2 患者一般情况 根据纳入标准共150例患者进入随访研究,由于各种原因造成失访32例。118例患者完成随访,其中男性78例,女性40例,年龄(25.66±5.18)岁,体质量指数 (24.16±3.28) kg/m2。右膝68例,左膝50例;损伤原因:交通伤48例,运动伤70例。 2.3 双侧膝关节屈肌及伸肌肌力情况 双侧肢体屈、伸肌力的等速测试结果见表1。单因素重复测量结果显示:重建后不同时间,患肢伸肌的肌力有显著差异,随时间延长,肌力逐渐恢复(F=89.63,P=0.00);采用Bonferroni检验两两比较证实,重建后3-6个月期间、6-9个月期间,肌力均有显著改变,其中3-6个月期间肌力恢复更快(P3-6=0.00, P-9=0.001);重建后9-12期间肌力改变不显著(P9-12=0.22)。重建后不同时间,患肢屈肌的肌力有显著差异,随时间延长,肌力逐渐恢复(F=27.23,P=0.00);采用Bonferroni检验两两比较证实,重建后3-6个月期间屈肌肌力有显著改变(P3-6=0.00),重建后6-9个月期间、重建后9-12期间肌力改变不显著(P6-9=0.10,P9-12=0.18)。重建后不同时间,健侧屈肌、伸肌肌力均无显著差异(F=0.76,P=0.52;F=0.37,P=0.77)。双因素重复测量结果证实,患侧肢体的屈、伸肌力与健侧肢体比较,有显著性差异(F=47.66,P=0.00;F=932.70,P=0.00);采用多变量方差分析对每个时间点上患侧与健侧屈、伸肌力的比较结果证实,患侧伸肌肌力在重建后3,6,9,12个月时均显著低于健侧伸肌肌力(F=520.67,P=0.00;F=217.75,P=0.00;F=99.46,P=0.00;F=67.87,P=0.00) ;患侧屈肌肌力在重建后3,6个月时明显低于健侧屈肌肌力(F=68.76,P=0.00;F=12.82,P=0.00),患侧屈肌肌力在9,12个月时与健侧相比无显著差异(F=1.77,P=0.18;F=1.176,P=0.28)。 2.4 双侧膝关节屈/伸肌肌力比值情况 双侧膝关节屈/伸肌力比值见表2,经单因素重复测量结果证实,随重建后康复时间延长,患侧膝关节屈/伸肌肌力比值逐渐下降(F=46.80,P=0.00),重建后3,6,9,12个月时健侧膝关节屈/伸肌肌力比值无显著差异(F=0.36,P=0.78)。双因素重复测量结果证实,患侧肢体的膝关节屈/伸肌肌力比值与健侧肢体比较,有显著性差异(F=528.23,P=0.00),患侧膝关节屈/伸肌肌力比值显著高于健侧。 采用多变量方差分析对每个时间点上膝关节屈/伸肌肌力比值的比较结果证实,患侧膝关节屈/伸肌肌力比值在重建后3,6,9,12个月时均显著高于健侧(F=316.08,P=0.00;F=177.93,P=0.00;F=100.24,P=0.00;F=119.78,P=0.00)。 2.5 患者下肢功能测试结果 双侧单脚跳、6 m计时单脚跳、侧边单脚跳及交叉单脚跳等四项运动功能结果的对称指数见表3,重建后第6个月时单脚跳、6 m计时单脚跳、侧边单脚跳及交叉单脚跳运动功能实验测试均低于对侧肢体的90%;重建后12个月时,单脚跳及6 m计时单脚跳超过对侧肢体的90%,但侧边单脚跳及交叉单脚跳仍低于对侧肢体的90%。 2.6 不良反应发生情况 2例患者重建后胫前区轻度肿胀,无明显压痛,考虑系关节渗液经由空心钛挤压螺钉渗入胫前组织间隙所致,经消肿、对症治疗后症状好转。所有患者随访期间未发生韧带松动断裂,钛螺钉固定良好,无松动、脱出情况发生,膝关节屈伸功能严重受限情况发生。 "

| [1] Brady MP. Clinical diagnostic tests versus MRI diagnosis of ACL tears. J Sport Rehabil. 2017;15:1-14.[2] Mather RC, Koenig L, Kocher MS, et al. Societal and economic impact of anterior cruciate ligament tears. J Bone Joint Surg. 2013; 95:1751-1759.[3] Tourville TW, Jarrell KM, Naud S, et al. Relationship between isokinetic strength and tibiofemoral joint space width changes after anterior cruciate ligament reconstruction. Am J Sports Med. 2014;42:302-311. [4] Chung KS, Ha JK, Ra HJ, et al. Does synovialization after anterior cruciate ligament reconstruction have a positive effect on functional performance, outcomes scores, stability and muscle strength? A 2-year follow-up study after reconstruction. Arch Orthop Trauma Surg. 2017;137(12):1725-1733[5] Burks RT, Crim J, Fink BP, et al. The effects of semitendinosus and gracilis harvest in anterior cruciate ligament reconstruction. Arthroscopy.2005;21:1177-1185.[6] Keays SL, Bullock-Saxton J, Keays AC, et al. Muscle strength and function before and after anterior cruciate ligament reconstruction using semitendinosus and gracilis. The Knee. 2001; 8: 229-234.[7] Chao WC, Shih JC, Chen KC, et al. The effect of functional movement training after anterior cruciate ligament reconstruction-a Randomized controlled trial. J Sport Rehabil. 2017;24:1-18.[8] Hsiao SF, Chou PH, Hsu HC, et al. Changes of muscle mechanics associated with anterior cruciate ligament deficiency and reconstruction. J Strength Cond Res. 2014;28:390-400.[9] Knezevic OM, Mirkov DM, Kadija M, et al. Evaluation of isokinetic and isometric strength measures for monitoring muscle function recovery after anterior cruciate ligament reconstruction. J Strength Cond Res. 2013;28:1722-1731.[10] Knezevic OM, Mirkov DM, Kadija M, et al. Asymmetries in explosive strength following anterior cruciate ligament reconstruction. Knee.2014;21(6):1039-1045.[11] Pamukoff DN, Pietrosimone BG, Ryan ED, et al. Quadriceps function and hamstrings co-activation after anterior cruciate ligament reconstruction. J Athl Train. 2017;52:422-428.[12] Setuain I, Izquierdo M, Idoate F, et al. Differential effects of two rehabilitation programs following anterior cruciate ligament reconstruction. J Sport Rehabil. 2016;19:1-37. [13] Kuenze C, Hertel J, Hart JM. Effects of exercise on lower extremity muscle function after anterior cruciate ligament reconstruction. J Sport Rehabil. 2013;22(1):33-40.[14] Goetschius J. Knee-extension torque variability and subjective knee function in patients with a history of anterior cruciate ligament reconstruction. J Athl Train. 2016;51:22-27[15] Hohmann E, Bryant A. Strength does not influence knee function in the ACL-deficient knee but is a correlate of knee function in the and ACL-reconstructed knee. J Orthop Trauma.2016; 136(4): 477-483.[16] Wipfler B, Donner S, Zechmann CM, et al. Anterior cruciate ligament reconstruction using patellar tendon versus hamstring tendon: a prospective comparative study with 9-year follow-up. Arthroscopy. 2011;27:653-665.[17] Kim DK, Park WH. The correlation of the evaluation of quality of life depends on knee strength after 1-year anterior cruciate ligament reconstruction. J Kor Sports Med.2014; 32: 139-143. [18] Hortobagyi T, Westerkamp L, Beam S, et al. Altered hamstring-quadriceps muscle balance in patients with knee osteoarthritis. Clin Biomech (Bristol, Avon). 2005; 20: 97-104.[19] Kim HJ, Lee JH, Ahn SE, et al. Influence of anterior cruciate ligament tear on thigh muscle strength and hamstring-to-quadriceps ratio: a Meta-analysis. PLoS One. 2016;11:e0146234. [20] Adams D, Logerstedt DS, Hunter-Giordano A, et al. Current concepts for anterior cruciate ligament reconstruction: a criterion-based rehabilitation progression. J Orthop Sports Phys Ther. 2012;42(7):601-614.[21] Kadija M, Knezevi? OM, Milovanovi? D, et al. The effect of anterior cruciate ligament reconstruction on hamstring and quadriceps muscle function outcome ratios in male athletes. Srp Arh Celok Lek. 2016;144(3-4):151-157.[22] Fischer F, Fink C, Herbst E, et al. Higher hamstring-to-quadriceps isokinetic strength ratio during the first post-operative months in patients with quadriceps tendon compared to hamstring tendon graft following ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. 2018;26(2):418-425. [23] Streich NA, Friedrich K, Gotterbarm T. Reconstruction of the ACL with a semitendinosus tendon graft: a prospective randomized single blinded comparison of double-bundle versus single-bundle technique in male athletes. Knee Surg Sports Traumatol Arthrosc . 2008;16:232-238.[24] Ardern CL, Webster KE, Taylor NF. Return to the preinjury level of competitive sport after anterior cruciate ligament reconstruction surgery: two-thirds of patients have not returned by 12 months after surgery. Am J Sports Med. 2011;39:538-543.[25] Ardern CL, Taylor NF, Feller JA. Return-to-sport outcomes at 2 to 7 years after anterior cruciate ligament reconstruction surgery.Am J Sports Med. 2012;40:41-48. [26] Goetschius J, Kuenze CM, Hart JM. Knee extension torque variability after exercise in ACL reconstructed knees. J Orthop Res. 2015;33(8):1165-1170.[27] Xergia SA, Pappas E. Association of the single-limb hop test with Isokinetic, kinematic, and kinetic asymmetries in patients after anterior cruciate ligament reconstruction. Sports Health. 2015;7: 217-223. [28] Lepley LK. Deficits in quadriceps strength and patient-oriented outcomes at return to activity after ACL reconstruction: a review of the current literature. Sports Health. 2015;7:231-238.[29] Hsieh CJ, Indelicato PA, Moser MW, et al. Speed, not magnitude, of knee extensor torque production is associated with self-reported knee function early after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2015; 23(11):3214-3220.[30] Camp CL, Lebaschi A, Cong GT, et al. Timing of postoperative mechanical loading affects healing following anterior cruciate ligament reconstruction: analysis in a murine model. J Bone Joint Surg Am. 2017;99:1382-1391.[31] Hart JM,Pietrosimone B,Hertel J.Quadriceps activation following knee injuries: a systematic review.J Athl Train 2010;45:87-97.[32] Konishi Y,Ikeda K,Nishino A,et al.Relationship between quadriceps femoris muscle volume and muscle torque after anterior cruciate ligament repair.Scand J Med Sci Sports 2007; 17:656-661.[33] Abrams GD, Harris JD, Gupta AK, et al. Functional performance testing after anterior cruciate ligament reconstruction: a systematic review. Orthop J Sports Med. 2014;21;2(1): 2325967113518305. .[34] Nicky EM, Robert EH, Tony G. Functional performance 2–9 years after ACL reconstruction: cross-sectional comparison between athletes with bone–patellar tendon–bone, semitendinosus/gracilis and healthy controls. Knee Surg Sports Traumatol Arthrosc. 2017; 25:1-12. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [3] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [4] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [5] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [6] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [7] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [8] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [9] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [10] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [11] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [12] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [13] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| [14] | Zhang Nianjun, Chen Ru. Analgesic effect of cocktail therapy combined with femoral nerve block on total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 866-872. |
| [15] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||