Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (48): 8419-8428.doi: 10.3969/j.issn.2095-4344.2013.48.020
Previous Articles Next Articles
Allograft cancellous bone combined with autologous red marrow for treatment of periarticular fractures
Kong Zhi-gang, Chen Yong-bao, Sun Lei
- Department of Orthopedics, the Third Affiliated Hospital of Hebei Medical University, Hebei Orthopaedic Biomechanics Laboratory, Shijiazhuang 050051, Hebei Province, China
-
Online:2013-11-26Published:2013-11-26 -
Contact:Kong Zhi-gang, Professor, Master’s supervisor, Department of Orthopedics, the Third Affiliated Hospital of Hebei Medical University, Hebei Orthopaedic Biomechanics Laboratory, Shijiazhuang 050051, Hebei Province, China kzg2005@tom.com -
About author:Kong Zhi-gang, Professor, Master’s supervisor, Department of Orthopedics, the Third Affiliated Hospital of Hebei Medical University, Hebei Orthopaedic Biomechanics Laboratory, Shijiazhuang 050051, Hebei Province, China kzg2005@tom.com -
Supported by:the Scientific and Technological Research Program of Hebei Provincial Health Bureau, No. 20090417*
CLC Number:
Cite this article
Kong Zhi-gang, Chen Yong-bao, Sun Lei. Allograft cancellous bone combined with autologous red marrow for treatment of periarticular fractures[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(48): 8419-8428.
share this article
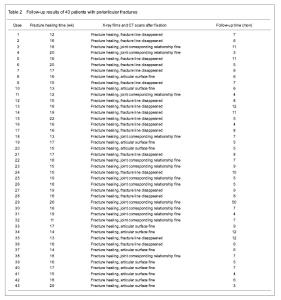
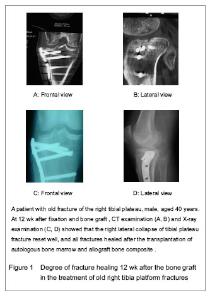
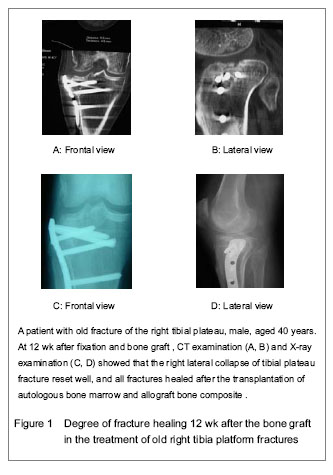
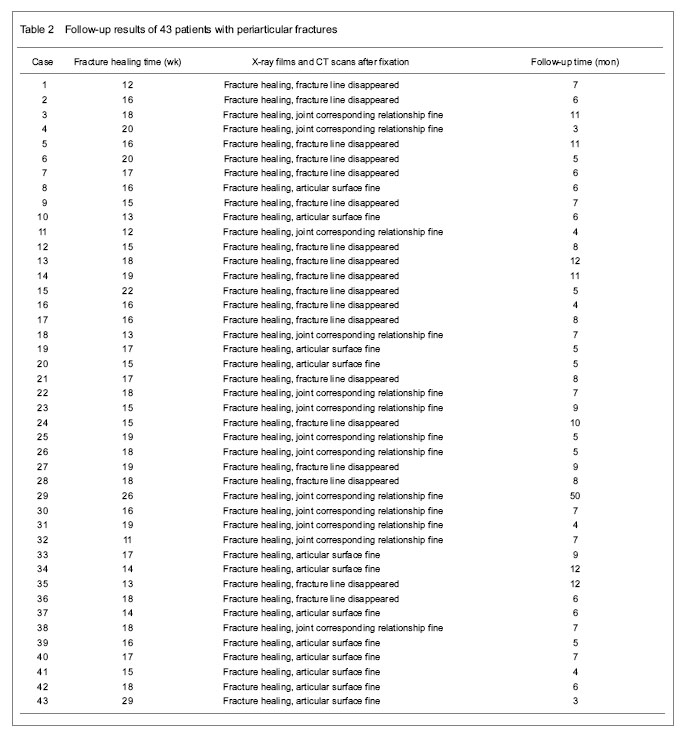
Quantitative analysis of participants Forty-three cases were involved with complete follow-up data, and all of them entered the result analysis, with no withdrawal. The follow-up results of the patients receiving the locking plate fixation and transplantation of allogeneic bone combined with autologous red marrow Forty-three cases were followed up for 12 months to 6 years, average 4.3 years, and the fractures were all healed (Table 2). Forty-three patients were followed up for 12 months to 6 years, an average of 4.3 years. The review of X-ray and CT showed that the collapse fracture reset well, and all fractures healed after allograft bone composite and autologous bone marrow transplantation. As shown in Figure 1, the fresh fracture healing time was 2-6 months, an average of 4 months; the old fracture healing time was 3 to 7 months, an average of 5.5 months. Fusion condition of bone graft and the host bone Evaluation criteria of X-ray radiography for bone fusion between the graft and the host bone[12]: the bone graft and the host bone get fused well, which is defined as fracture healing; the bone graft and the host bone are not fused, which is defined as nonunion; the transplant bone is absorbed > 30%, which is defined as transplanted bone resorption; the bone mineral density around the transplantation bone decreases, which is defined as osteoporosis; the bone mineral density around the transplantation bone increases, which is defined as osteosclerosis. Results found that the fresh fracture healing time was 2-6 months, an average of 4 months; the old fracture healing time was 3 to 7 months, an average of 5.5 months."
| [1] Rimondini L, Nicoli-Aldini N, Fini M, et al. In vivo experimental study on bone regeneration in critical bone defects using an injectable biode-gradable PLA/PGA copolymer. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;99(2):148-154. [2] Kon E, Muraglia A, Corsi A, et al. Autologus bone marrow stromal, cells loaded onto porous hydroxyapatite ceramic accelerate bone repair in critical-size defects of sheep long bones. J Biomed Mater Res. 2000;49(3):328-337. [3] Zasacki W. The efficacy of application of lyophilized, radiation sterilized bone graft in orthopaedic surgery. Clin Orthop Relat Res. 1991;272:82-87. [4] Zhang L, Xu ZH, Yang ZL. Transplantation combined with autologous bone marrow to repair non-infected nonunion. Zhongguo Xiufu Chongjia Waike Zazhi. 2005;19(7):590-591. [5] Hernigou P, Poignard A, Manicom O, et al. The use of percutaneous autologous bone marrow transplantation in nonunion and avascular necrosis of bone. J Bone Joint Surg (Br). 2005;87(7):896-902. [6] Burwell RG. The function of bone marrow in the corporation of a bone graft. Clin Orthop Relat Res. 1985;200(2):125-141. [7] Burwell RG. Studies in transplantation of bone. Clin Orthop Relat Res. 1999;(367 Suppl):S5-11;discussion S2-4. [8] Zhao JJ, Li QZ. The preparation of the grafting material of homologous cancellus/autologous red marrow and clinical applicarion. Shiyong Guke Zazhi. 2005(2):123-125. [9] Kong ZG, Tian DH. Treatment of traumatic bone defect with graft material of allogenic cancellus combined with autologous red marrow. Zhongguo Xiufu Chongjia Waike Zazhi. 2008;(10):1251-1254. [10] Yin WF, Chen S. Allogeneic bone combined with autologous concentrated red bone marrow graft for treatment of benign bone tumors and tumor-like lesions. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2009;16(24):3149-3152. [11] Sudkamp N, Bayer J, Hepp P, et al. Open reduction and internal fixation of proximal humeral fractures with use ofthe locking proximal humerus plate. Results of a prospective, multicenter, observational study. J Bone Joint Surg (Am). 2009;91(6):1320-1328. [12] Andersen JR, Detlie T, Griffiths HJ. The radiology of bone allografts. Radiol Clin North Am. 1995;33(2):391-400. [13] Mankin HJ, Gebhardt MC, Tomford WW. The use of frozen cadaveric allografts in the management of patients with bone Tumors of the extremities. Orthop Clin North Am. 1987;18(2):275-289. [14] Komender J, Malczewska H, Komender A. Therapeutic effects of transplantation of lyophilized and radiation- sterilized, allogeneic bone. Clin Orthop Relat Res. 1991; (272):38-49. [15] Huang JJ, Zhang JM, Zhuo XL, et al. Treatment of senile Colles fracture with anatomic locking plate combined with allogeneic bone transplantation. Zhongguo Gu yu Guanjie Sunshang Zazhi. 2011;26(1):78-79. [16] Bennett WF, Browner B. Tibial plateau fractures: a study of associated soft tissue injuries. J OrthopTrauma. 1994;8(3): 183-185. [17] Feng W, Fu L, Liu JG. Bone allograft for tibial plateau fractures in 22 cases. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2009;13(15):2984-2987. [18] Cao Y, Yuan ZM, Yan P, et al. Characteristics of nano-artificial bone grafr in treatment of tibial plateau fracture. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2011;15(38):7189-7192. [19] Laurencin C, Khan Y, El-Amin SF. Bone graft substitutes. Expert Rev Med Deviecs. 2006;3(1):49-57. [20] Wraighte PJ, Howard PW. Femoral impaction bone allografting with an Exeter cemented collarless, polished, tapered stem in revision hip replacement: a mean follow-up of 10.5 years. J Bone Joint Surg (Br). 2008;90(8): 1000-1004. [21] De Long WG Jr, Einhorn TA, Koval K, et al. Bone grafts and bone graft substitutes in orthopaedic trauma surgery. J Bone Joint Surg (Am). 2007;89(3):649-658. [22] Jerosch J, Muchow H, Clahsen H. Stability of human bone cortex following various preservation and sterilization methods. Z Orthop Ihre Grenzgeb. 1991;129(4):295-301. [23] Wang ZQ, Wang Q, Su LX, et al. Clinical application of morselized allogeneic bone processed by lyophilization and radiation. Zhonghua Guke Zazhi. 2004;24(10):590-596. [24] Song HP, Wang ZQ. Study on the application of allogeneic bone transplantation. Zhongguo Xiufu Chongjia Waike Zazhi. 2006;20(1):77-80. [25] Xu ST. Practical Orthopedics. 2nd ed. Beijing: People’s Medical Publishing House. 2002. [26] Hernigou P, Poignard A, Beaujean F, et al. Percutaneous autologous bone-marrow grafting for nonunions. In uence of the number and concentra-tion of progenitor cells. J Bone Joint Surg (Am). 2005;87(7):1430-1437. [27] Yang GS, Xu YB. Bone mesenchymal stem cells and their utilization advances. Zhonghua Chuangshang Guke Zazhi. 2004;6(7):824-827. [28] Gu ZC, Li QH. An experimental study on the marrow stromal cells and biomaterial composites in repair of segmental defects of rabbit ulna. Zhonghua Chuangshang Guke Zazhi. 2004;6(6):651-656. [29] Cao JT, Li QJ, Song HP, et al. Study of the biocompatibility on allogeneic freeze-dried bone particles and bone marrow stromal cells-derived osteoblasts in vitro. Zhongguo Jiaoxing Waike Zazhi. 2010;18(12):1023-1026. [30] Fu M, Liang HX. Treatment of bone defect bone allograft with bone marrow stem cell in animal experiment. Zhongshan Daxue Xuebao (Medical Sciences). 2007;28(5): 515-519. [31] Zhang SQ, Liu AQ, Xiao DM, et al. Unicameral bone cysts treated by percutaneous injection of autologous bone marrow and allogeneic bone powder grafting. Zhongguo Guzhongliu Gubing. 2006;5(5):273-275. [32] Li B, Chen J, Que XY, et al. Massive bone allograft combined with autologous bone marrow transplantation for proximal femoral defects resulting from tumor resection. Zhongguo Zuzhi Gongcheng Yanjiu. 2012;16(5):831-834. [33] Lin JP, Song SF, Li ZM, et al. Treatment of bone defects with autologous bone marrow transplantation combined with bone allograft. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2011;15(26):4891-4894. [34] Wei JR, Zhang Y, Lin YL, et al. Xenogeneic cancellous bone for repairing segmental defects in rabbit radius. Zhongguo Zuzhi Gongcheng Yanjiu. 2012;16(29):5379- 5381. [35] Fang ZH, Tan JH, Zeng XT, et al. Effect of bone marrow mesenchymal stem cells combined with various scaffold materials: a systematic review. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2011;49(15): 9249-9253. [36] Yi HC, Tang LH, Zhang XP. Experimental study on bone defected by combined autologous bone marrow transplantation, cut-tebone, and sodium hyaluronate. Zhongguo Zhongxiyi Jiehe Zazhi. 2011;31(8):1122-1126. [37] State Council of the People’s Republic of China. Administrative Regulations on Medical Institution. 1994-09-01. |
| [1] | Wang Liang, Huang Zhaozhao, Yu Jiaona, Gu Weidong, Wang Ren, Qian Zhiyi. Biomechanical characteristics of bridge-link type combined internal fixation system with mixed-rod versus double-rod in the treatment of femoral and tibial fractures [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(6): 888-892. |
| [2] | Liu Ting, Yang Tingting, Ma Xiaona, Ma Haibin, Jin Yiran, Liang Xueyun. Immunoregulation of allograft rejection: a role played by human CD200+ sub-population from human placenta-derived mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(13): 2068-2073. |
| [3] | Yuan Bo, Wang Zhiwei, Tang Yifan, Zhou Shengyuan, Chen Xiongsheng, Jia Lianshun. Construction of polycaprolactone-tricalcium phosphate with different mixture ratios using three-dimensional printing technology and its osteoinductivity in vitro [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(6): 821-826. |
| [4] | Wei Wei, Liu Yanfei, Zhang Ling, Xiong Na . Self-assembling peptide hydrogel: hemostatic effect and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(2): 310-316. |
| [5] | Zhang Minbo, Peng Qifeng, Ma Yaping, Kong Weijun, Liao Wenbo. Physical properties and biocompatibility of 3D printed bone microparticle/poly(lactic-co-glycolic acid) scaffold [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2215-2222. |
| [6] | Li Zhi, Tan Chunhua, Cai Xianhua, Wang Huasong, Ding Xiaoming, Zhao Yanhong. Fabrication and biocompatibility assessment of the scaffold with biomimetic interconnected macropore structure [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2223-2227. |
| [7] | Bai Yulong, Gao Yufeng, Zhong Hongbin, Zhao Yantao, Guo Ruizhou, Li Li. Allogeneic and xenogeneic tissue repair materials: how to choose a suitable virus inactivation process [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2261-2268. |
| [8] | Luo Kai, Yang Yafeng, Ma Teng, Xia Bing, Huang Liangliang, Huang Jinghui, Luo Zhuojing. Effects of perfluorotributylamine/alginate/bioglass biomaterials on viability and osteogenic differentiation of adipose-derived stem cells [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(13): 1995-2001. |
| [9] | Wang Yuanyuan, Song Wenshan, Yu Dejun, Dai Yuankun, Li Bafang. Preparation and evaluation of fish skin acellular dermal matrix for oral guided tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(10): 1526-1532. |
| [10] | Liu Shaoyang, Zou Hanlin . Biocompatibility of anodic titanium oxide: an experimental research [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(10): 1575-1580. |
| [11] | Cai Yuhui, Hu Kesu, Zhang Yi. Biosafety evaluation of chitosan lactate/hyaluronate sponge [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(10): 1558-1563. |
| [12] | Zhao Zhi-hui, Ren Lin-hui, Li Yi, Lu Feng-cheng, Kifayat Ullah, Basanta Sapkota, Wang Yong-qing . Intramedullary nailing for proximal tibial fractures: anatomy, biomechanics and design principles of the nail [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(7): 1126-1132. |
| [13] | Zhang Lei, Zhou Song, Cheng Bao-chang. Actuality and challenge of biomaterials in annulus fibrosus repair [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(6): 958-963. |
| [14] | Li Zhi-yue, Zhu Zhi-bo, Zhao Qun, Xiang Si-yu, Zhao Peng, Xu Zhe-wei. Biocompatibility of basic fibroblast growth factor-poly(lactic-co-glycolic acid) microspheres/ hydroxyapatite/poly(l-lactic acid) porous materialsBiocompatibility of basic fibroblast growth factor-poly(lactic-co-glycolic acid) microspheres/ hydroxyapatite/poly(l-lactic acid) porous materials [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(6): 914-920. |
| [15] | Meng Ai, Wang Jian, Sui Lei. Effect of mixed acid reflux time on purification and biocompatibility of large-inner-diameter multi-walled carbon nanotubes [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(6): 896-901. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||