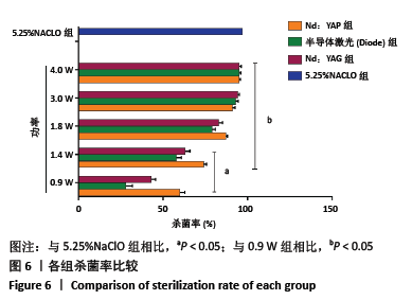
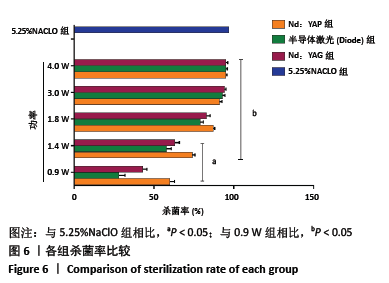
[1] LEMOS JA, PALMER SR, ZENG L, et al. The Biology of Streptococcus mutans. Microbiol Spectr. 2019;7(1):10.
[2] PHILIP N, SUNEJA B, WALSH L. Beyond Streptococcus mutans: clinical implications of the evolving dental caries aetiological paradigms and its associated microbiome. Br Dent J. 2018;224(4):219-225.
[3] BYUN R, NADKARNI MA, CHHOUR KL, et al. Quantitative analysis of diverse Lactobacillus species present in advanced dental caries. J Clin Microbiol. 2004;42(7):3128-3136.
[4] WASFI R, ABD EL-RAHMAN OA, ZAFER MM, et al. Probiotic Lactobacillus sp. inhibit growth, biofilm formation and gene expression of caries-inducing Streptococcus mutans. J Cell Mol Med. 2018;22(3):1972-1983.
[5] MANSKI RJ, MEYERHOEFER CD. Projecting the Demand for Dental Care in 2040. J Dent Educ. 2017;81(8):eS133-eS145.
[6] 周学东,凌均棨,梁景平,等.龋病临床治疗难度因素及处理[J].华西口腔医学杂志,2017,35(1):1-7.
[7] MCLEOD FS, SIMMONDS RS. Penicillin facilitates the entry of antisense constructs into Streptococcus mutans. FEMS Microbiol Lett. 2013; 349(1):25-31.
[8] PROSSER BL, TAYLOR D, DIX BA, et al. Method of evaluating effects of antibiotics on bacterial biofilm. Antimicrob Agents Chemother. 1987; 31:1502-1506.
[9] 陈才香.硝酸银和碘伏消毒后牙敏感中龋窝洞的临床疗效[J].海南医学,2005,16(4):53-48.
[10] 杨金洪.丁香油消毒龋洞引起过敏一例[J].华西口腔医学杂志, 1990,8(4):275.
[11] AZIZI A, SHOHRATI P, GOUDARZI M, et al. Comparison of the effect of photodynamic therapy with curcumin and methylene Blue on streptococcus mutans bacterial colonies. Photodiagnosis Photodyn Ther. 2019;27:203-209.
[12] TERRA GARCIA M, CORREIA PEREIRA AH, FIGUEIREDO-GODOI LMA, et al. Photodynamic therapy mediated by chlorin-type photosensitizers against Streptococcus mutans biofilms. Photodiagnosis Photodyn Ther. 2018;24:256-261.
[13] AYTAC BAL F, OZKOCAK I, CADIRCI BH, et al. Effects of photodynamic therapy with indocyanine green on Streptococcus mutans biofilm. Photodiagnosis Photodyn Ther. 2019;26:229-234.
[14] NEMEZIO MA, DE SOUZA FARIAS SS, BORSATTO MC, et al. Effect of methylene blue-induced photodynamic therapy on a Streptococcus mutans biofilm model. Photodiagnosis Photodyn Ther. 2017;20:234-237.
[15] LIU T, HUANG Z, JU Y, et al. Bactericidal efficacy of three parameters of Nd:YAP laser irradiation against Enterococcus faecalis compared with NaOCl irrigation. Lasers Med Sci. 2019;34(2):359-366.
[16] GRZECH-LEŚNIAK K, SCULEAN A, GAŠPIRC B. Laser reduction of specific microorganisms in the periodontal pocket using Er:YAG and Nd:YAG lasers: a randomized controlled clinical study. Lasers Med Sci. 2018;33(7):1461-1470.
[17] GRANEVIK LINDSTRÖM M, WOLF E, FRANSSON H. The Antibacterial Effect of Nd:YAG Laser Treatment of Teeth with Apical Periodontitis: A Randomized Controlled Trial. J Endod. 2017;43(6):857-863.
[18] MATARESE G, RAMAGLIA L, CICCIÙ M, et al. The Effects of Diode Laser Therapy as an Adjunct to Scaling and Root Planing in the Treatment of Aggressive Periodontitis: A 1-Year Randomized Controlled Clinical Trial. Photomed Laser Surg. 2017;35(12):702-709.
[19] SARDA RA, SHETTY RM, TAMRAKAR A, et al. Antimicrobial efficacy of photodynamic therapy, diode laser, and sodium hypochlorite and their combinations on endodontic pathogens. Photodiagnosis Photodyn Ther. 2019;28:265-272.
[20] KORKUT E, TORLAK E, GEZGIN O, et al. Antibacterial and Smear Layer Removal Efficacy of Er:YAG Laser Irradiation by Photon-Induced Photoacoustic Streaming in Primary Molar Root Canals: A Preliminary Study. Photomed Laser Surg. 2018;36(9):480-486.
[21] GRZECH-LEŚNIAK K, MATYS J, JURCZYSZYN K, et al. Histological and Thermometric Examination of Soft Tissue De-Epithelialization Using Digitally Controlled Er:YAG Laser Handpiece: An Ex Vivo Study. Photomed Laser Surg. 2018;36(6):313-319.
[22] SANTIS LR, SILVA TM, HADDAD BA, et al. Influence of dentin thickness on intrapulpal temperature under simulated pulpal pressure during Nd:YAG laser irradiation. Lasers Med Sci. 2017;32(1):161-167.
[23] KHOUJA F, ABDELAZIZ M, BORTOLOTTO T, et al. Intra-pulpal and subsurface temperature rise during tooth irradiation with 808 nm diode laser: an in vitro study. Eur J Paediatr Dent. 2017;18(1):56-60.
[24] CHO H, LEE RC, CHAN KH, et al. Assessment of radicular dentin permeability after irradiation with CO2 laser and endodontic irrigation treatments with thermal imaging. Proc SPIE Int Soc Opt Eng. 2017; 10044:100440K.
[25] KIVANC BH, ARISU HD, SAĞLAM BC, et al. Evaluation of antimicrobial and thermal effects of diode laser on root canal dentin. Niger J Clin Pract. 2017;20(12):1527-1530.
[26] BALDISSARA P, CATAPANO S, SCOTTI R. Clinical and histological evaluation of thermal injury thresholds in human teeth: preliminary study. J Oral Rehabil. 1997;24:791-801.
[27] ZACH L, COHEN G. Pulp response to externally applied heat. Oral Surg Oral Med Oral Pathol. 1965;19(4):515-530.
[28] NAMOUR A, GEERTS S, ZEINOUN T, et al. Safety Irradiation Parameters of Nd:YAP Laser Beam for Endodontic Treatments: An InVitro Study. Biomed Res Int. 2016;2016:4741516.
[29] NAMOUR A, NAMMOUR S, PEREMANS A, et al. Treatment of dentinal hypersensitivity by means of Nd: YAP Laser: a preliminary in vitro study. Sci World J. 2014;2014:323604.
[30] TABATABAEI MH, CHINIFORUSH N, HASHEMI G, et al. Efficacy Comparison of Nd:YAG laser, diode laser and dentine bonding agent in dentine hypersensitivity reduction: a clinical trial. Laser Ther. 2018;27(4):265-270.
[31] AFKHAMI F, AKBARI S, CHINIFORUSH N. Entrococcus faecalis Elimination in Root Canals Using Silver Nanoparticles, Photodynamic Therapy, Diode Laser, or Laser-activated Nanoparticles: An In Vitro Study. J Endod. 2017;43(2):279-282.
[32] BLUM JY, MICHAILESCO P, ABADIE MJ. An evaluation of the bactericidal effect of the Nd:YAP laser. J Endod. 1997;23(9):583-585.
[33] GRZECH-LEŚNIAK K, NOWICKA J, PAJĄCZKOWSKA M, et al. Effects of Nd:YAG laser irradiation on the growth of Candida albicans and Streptococcus mutans: in vitro study. Lasers Med Sci. 2019;34(1):129-137.
[34] MASUDA Y, SAKAGAMI H, HORIIKE M, et al. Photodynamic Therapy with Pyoktanin Blue and Diode Laser for Elimination of Enterococcus faecalis. In Vivo. 2018;32(4):707-712.
[35] LÓPEZ-JIMÉNEZ L, ARNABAT-DOMÍNGUEZ J, VIÑAS M, et al. Atomic force microscopy visualization of injuries in Enterococcus faecalis surface caused by Er,Cr:YSGG and diode lasers. Med Oral Patol Oral Cir Bucal. 2015;20(1):e45-e51.
[36] HUANG YJ, CHEN YF, CHEN WD, et al. Comparative study of intracavity KTP-based Raman generation between Nd:YAP and Nd:YAG lasers operating on the (4)F(3/2) → (4)I(13/2) transition. Opt Express. 2015; 23(8):10435-10443.
[37] GRZECH-LEŚNIAK K, SCULEAN A, GAŠPIRC B. Laser reduction of specific microorganisms in the periodontal pocket using Er:YAG and Nd:YAG lasers: a randomized controlled clinical study. Lasers Med Sci. 2018;33(7):1461-1470.
[38] TABATABAEI MH, CHINIFORUSH N, HASHEMI G, et al. Efficacy Comparison of Nd:YAG laser, diode laser and dentine bonding agent in dentine hypersensitivity reduction: a clinical trial. Laser Ther. 2018;27(4):265-270.
[39] SIQUEIRA JF JR, RÔÇAS IN, FAVIERI A, et al. Chemomechanical reduction of the bacterial population in the root canal after instrumentation and irrigation with 1%, 2.5%, and 5.25% sodium hypochlorite. J Endod. 2000;26(6):331-334.
[40] CAFER T, MAHIR G, MURAT K. Effect of CO2, Nd:YAG, and ArF Excimer Lasers on Dentin Morphology and Pulp Chamber Temperature: An In Vitro Study. J Endod. 2000;26(11):644-648. |