Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (33): 5300-5306.doi: 10.3969/j.issn.2095-4344.2893
Previous Articles Next Articles
Comparison of lumbar-pelvic sagittal parameters after single-level and double-level posterior lumbar interbody fusion
Wei Yangyang1, Chen Jiacheng1, Sun Jun1, Wang Qiuan1, Yuan Feng2
1Graduate School of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China; 2Department of Orthopedics of Affiliated Hospital of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China
-
Received:2020-02-10Revised:2020-02-15Accepted:2020-03-13Online:2020-11-28Published:2020-09-29 -
Contact:Yuan Feng, Professor, MD, Chief physician, Department of Orthopedics of Affiliated Hospital of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China -
About author:Wei Yangyang, Physician, Graduate School of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China -
Supported by:the Science and Technology Fund of Jiangsu Province, No. BE2016647
CLC Number:
Cite this article
Wei Yangyang, Chen Jiacheng, Sun Jun, Wang Qiuan, Yuan Feng. Comparison of lumbar-pelvic sagittal parameters after single-level and double-level posterior lumbar interbody fusion[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(33): 5300-5306.
share this article
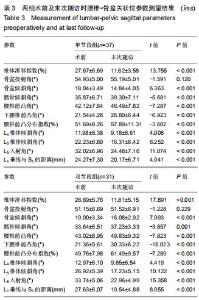
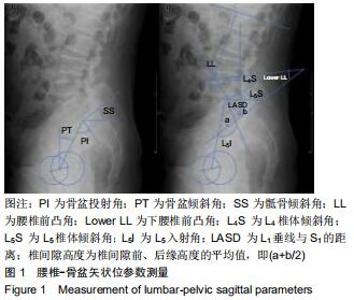
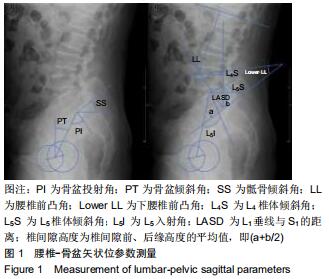
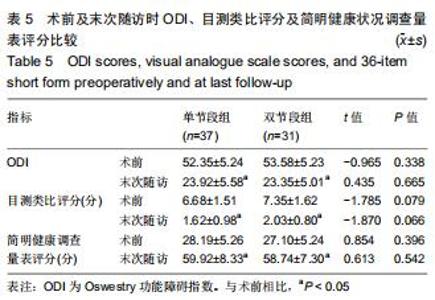
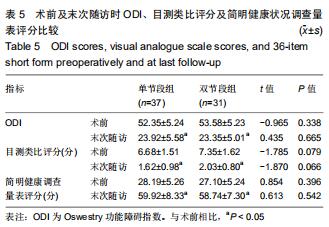
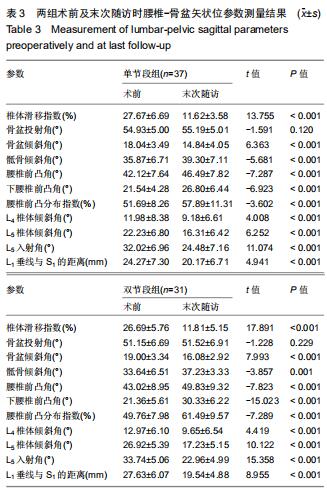
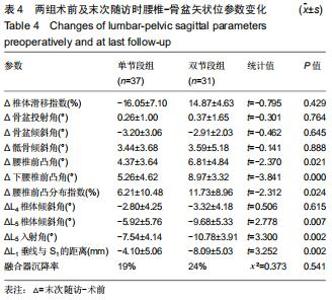
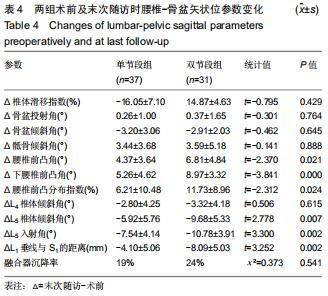
2.4.1 术前及末次随访时腰椎矢状位参数变化 2组患者影像测量结果见表3,4。单节段组与双节段组椎体滑移指数均较术前明显改善(P < 0.05),2组间改善程度差异无显著性意义(P > 0.05)。与术前相比,2组骨盆倾斜角显著减小(P < 0.05),骶骨倾斜角显著增大(P < 0.05),但2组之间差异无显著性意义(P > 0.05)。与术前相比,腰椎前凸角、下腰椎前凸角、腰椎前凸分布指数2组均较术前明显增加,双节段组增加值均显著大于单节段组(P < 0.05)。2组患者L4椎体倾斜角均较术前明显减小(P<0.05),但2组间差异无显著性意义(P > 0.05)。与术前相比,L5入射角、L5椎体倾斜角、L1垂线与S1距离均明显减小,且双节段组减小值显著大于单节段组(P < 0.05)。 "
2.4.1 术前及末次随访时腰椎矢状位参数变化 2组患者影像测量结果见表3,4。单节段组与双节段组椎体滑移指数均较术前明显改善(P < 0.05),2组间改善程度差异无显著性意义(P > 0.05)。与术前相比,2组骨盆倾斜角显著减小(P < 0.05),骶骨倾斜角显著增大(P < 0.05),但2组之间差异无显著性意义(P > 0.05)。与术前相比,腰椎前凸角、下腰椎前凸角、腰椎前凸分布指数2组均较术前明显增加,双节段组增加值均显著大于单节段组(P < 0.05)。2组患者L4椎体倾斜角均较术前明显减小(P<0.05),但2组间差异无显著性意义(P > 0.05)。与术前相比,L5入射角、L5椎体倾斜角、L1垂线与S1距离均明显减小,且双节段组减小值显著大于单节段组(P < 0.05)。 "
|
[1] WANG YX, DENG M, GRIFFITH JF, et al. Lumbar Spondylolisthesis Progression and De Novo Spondylolisthesis in Elderly Chinese Men and Women: A Year-4 Follow-up Study. Spine (Phila Pa 1976). 2016;41(13): 1096-1103.
[2] PHAN K, NAZARETH A, HUSSAIN AK, et al. Relationship between sagittal balance and adjacent segment disease in surgical treatment of degenerative lumbar spine disease: meta-analysis and implications for choice of fusion technique. Eur Spine J. 2018; 27(8): 1981-1991.
[3] LAFAGE R, OBEID I, LIABAUD B, et al. Location of correction within the lumbar spine impacts acute adjacent-segment kyphosis. J Neurosurg Spine. 2018; 30(1): 69-77.
[4] CHO JH, JOO YS, LIM C, et al. Effect of one- or two-level posterior lumbar interbody fusion on global sagittal balance. Spine J. 2017; 17(12): 1794-1802.
[5] ISHIHARA Y, MORISHITA M, MIYAKI J, et al. Comparison of transforaminal lumbar interbody fusion using the boomerang-shaped cage with traditional posterior lumbar interbody fusion for lumbar spondylolisthesis. Spine Surg Relat Res. 2019; 3(1): 71-78.
[6] MEYERDING HW. Spondylolisthesis; surgical fusion of lumbosacral portion of spinal column and interarticular facets; use of autogenous bone grafts for relief of disabling backache. J Int Coll Surg. 1956; 26(5 Part 1): 566-591.
[7] FRYMOYER JW. Low back pain. The role of spine fusion. Neurosurg Clin N Am. 1991; 2(4): 933-954.
[8] 黄诚谦,韦文,陆文忠,等. CARDS分型D型和非D型退变性腰椎滑脱临床特点及经椎间孔椎体间融合手术疗效的对比分析[J]. 中国骨与关节杂志, 2019, 8(7): 531-536.
[9] YILGOR C, SOGUNMEZ N, BOISSIERE L, et al. Global alignment and proportion (GAP) score: development and validation of a new method of analyzing spinopelvic alignment to predict mechanical complications after adult spinal deformity surgery. J Bone Joint Surg Am. 2017;99(19): 1661-1672.
[10] KIM MC, CHUNG HT, CHO JL, et al. Subsidence of polyetheretherketone cage after minimally invasive transforaminal lumbar interbody fusion. J Spinal Disord Tech. 2013; 26(2): 87-92.
[11] SUK SI, LEE CK, KIM WJ, et al. Adding posterior lumbar interbody fusion to pedicle screw fixation and posterolateral fusion after decompression in spondylolytic spondylolisthesis. Spine. 1997; 22(2): 210-219.
[12] SHEAHAN PJ, NELSON-WONG EJ, FISCHER SL. A review of culturally adapted versions of the Oswestry Disability Index: the adaptation process, construct validity, test-retest reliability and internal consistency. Disabil Rehabil. 2015; 37(25): 2367-2374.
[13] CONSTANT CR, MURLEY AH. A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res. 1987; (214): 160-164.
[14] SALIM S, YAMIN M, ALWI I, et al. Validity and Reliability of the Indonesian Version of SF-36 Quality of Life Questionnaire on Patients with Permanent Pacemakers. Acta Med Indones. 2017;49(1): 10-16.
[15] LABELLE H, ROUSSOULY P, BERTHONNAUD E, et al. Spondylolisthesis, pelvic incidence, and spinopelvic balance: a correlation study. Spine (Phila Pa 1976). 2004; 29(18): 2049-2054.
[16] JACKSON RP, MCMANUS AC. Radiographic analysis of sagittal plane alignment and balance in standing volunteers and patients with low back pain matched for age, sex, and size. A prospective controlled clinical study. Spine (Phila Pa 1976). 1994; 19(14): 1611-1618.
[17] YIJIAN Z, HAO L, HUILIN Y, et al. Comparison of posterolateral fusion and posterior lumbar interbody fusion for treatment of degenerative spondylolisthesis: Analysis of spino-pelvic sagittal balance and postoperative chronic low back pain. Clin Neurol Neurosurg. 2018; 171: 1-5.
[18] MAROUBY S, COULOMB R, MAURY E, et al. Prospective evaluation of spino-pelvic parameters with clinical correlation in patients operated with an anterior lumbar interbody fusion. Asian Spine J. 2020; 14(1): 88-96.
[19] 尹刚辉,金大地,陈方尧,等. 新的脊柱-骨盆矢状面测量参数:骶骨骨盆角的提出及意义[J]. 中国脊柱脊髓杂志, 2014, 24(8): 704-709.
[20] FENG Y, CHEN L, GU Y, et al. Influence of the posterior lumbar interbody fusion on the sagittal spino-pelvic parameters in isthmic L5-S1 spondylolisthesis. J Spinal Disord Tech.2014;27(1): E20-E25. [21] CHALEAT-VALAYER E, MAC-THIONG JM, PAQUET J, et al. Sagittal spino-pelvic alignment in chronic low back pain. Eur Spine J. 2011; 20 Suppl 5: 634-640.
[22] KEPLER CK, RIHN JA, RADCLIFF KE, et al. Restoration of lordosis and disk height after single-level transforaminal lumbar interbody fusion. Orthop Surg. 2012; 4(1): 15-20.
[23] ZHAO X, DU L, XIE Y, et al. Effect of Lumbar Lordosis on the Adjacent Segment in Transforaminal Lumbar Interbody Fusion: A Finite Element Analysis. World Neurosurg. 2018;114: e114-e120.
[24] TIAN H, WU A, GUO M, et al. Adequate Restoration of Disc Height and Segmental Lordosis by Lumbar Interbody Fusion Decreases Adjacent Segment Degeneration. World Neurosurg. 2018; 118: e856-e864.
[25] KIM KH, LEE SH, SHIM CS, et al. Adjacent segment disease after interbody fusion and pedicle screw fixations for isolated L4-L5 spondylolisthesis: a minimum five-year follow-up. Spine (Phila Pa 1976). 2010; 35(6): 625-634.
[26] OHBA T, EBATA S, OBA H, et al. Correlation between postoperative distribution of lordosis and reciprocal progression of thoracic kyphosis and occurrence of proximal junctional kyphosis following surgery for adult spinal deformity. Clin Spine Surg. 2018;31(9): E466-E472.
[27] KIM WJ, MA CH, KIM SH, et al. Prevention of adjacent segmental disease after fusion in degenerative spinal disorder: correlation between segmental lumbar lordosis ratio and pelvic incidence-lumbar lordosis mismatch for a minimum 5-year follow-up. Asian Spine J. 2019;13(4): 654-662.
[28] ZHU F, BAO H, LIU Z, et al. Analysis of L5 incidence in normal population use of L5 incidence as a guide in reconstruction of lumbosacral alignment. Spine (Phila Pa 1976). 2014;39(2): E140-146.
[29] ROUSSOULY P, GOLLOGLY S, BERTHONNAUD E, et al. Sagittal alignment of the spine and pelvis in the presence of L5-s1 isthmic lysis and low-grade spondylolisthesis. Spine (Phila Pa 1976). 2006;31(21): 2484-2490.
[30] LABELLE H, ROUSSOULY P, CHOPIN D, et al. Spino-pelvic alignment after surgical correction for developmental spondylolisthesis. Eur Spine J. 2008; 17(9): 1170-1176.
[31] SEBAALY A, EL RACHKIDI R, GROBOST P, et al. L5 incidence: an important parameter for spinopelvic balance evaluation in high-grade spondylolisthesis. Spine J. 2018;18(8): 1417-1423.
[32] FUNAO H, TSUJI T, HOSOGANE N, et al. Comparative study of spinopelvic sagittal alignment between patients with and without degenerative spondylolisthesis. Eur Spine J. 2012;21(11): 2181-2187.
[33] SU K, LUAN J, WANG Q, et al. Radiographic Analysis of minimally invasive transforaminal lumbar interbody fusion versus conventional open surgery on sagittal lumbar-pelvic alignment for degenerative spondylolisthesis. World Neurosurg. 2019; 124: e733-e739.
[34] KAWAKAMI M, TAMAKI T, ANDO M, et al. Lumbar sagittal balance influences the clinical outcome after decompression and posterolateral spinal fusion for degenerative lumbar spondylolisthesis. Spine (Phila Pa 1976). 2002; 27(1): 59-64.
[35] BOUAICHA S, CUNIER M, SCHEYERER MJ, et al. Does sagittal spinopelvic configuration influence vertebral fracture type or localization in trauma patients?: a retrospective radiologic analysis. Clin Spine Surg. 2017; 30(3): E265-E269.
[36] MACTHIONG JM, ROUSSOULY P, BERTHONNAUD E, et al. Sagittal parameters of global spinal balance: normative values from a prospective cohort of seven hundred nine Caucasian asymptomatic adults. Spine (Phila Pa 1976). 2010;35(22):E1193-1198.
[37] LABELLE H, MAC-THIONG JM, ROUSSOULY P. Spino-pelvic sagittal balance of spondylolisthesis: a review and classification. Eur Spine J. 2011; 20 Suppl 5: 641-646.
[38] 王鹏飞,谢威,王民洁. PLIF与TLIF治疗老年退变性腰椎滑脱合并腰椎管狭窄症的疗效比较[J]. 重庆医学, 2014,43(10):1259-1261. [39] 张明凯,汤健,尤涛. 下位节段椎间融合器融合、上位节段自体骨植骨融合治疗双节段退变性腰椎不稳临床观察[J]. 山东医药, 2017, 57(16): 47-49. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [8] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [9] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [10] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [11] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [12] | Yao Rubin, Wang Shiyong, Yang Kaishun. Minimally invasive transforaminal lumbar interbody fusion for treatment of single-segment lumbar spinal stenosis improves lumbar-pelvic balance [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1387-1392. |
| [13] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [14] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [15] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||