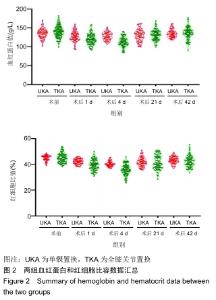
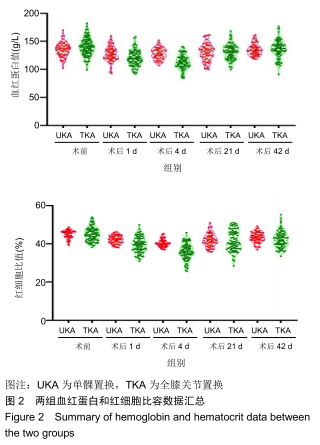
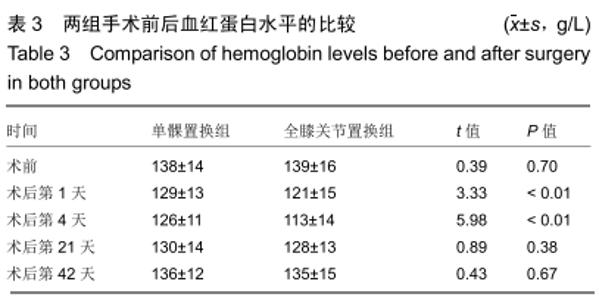
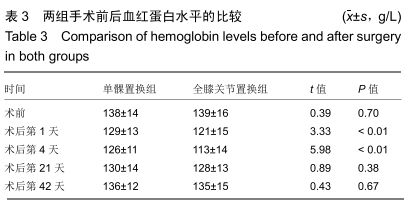
Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (15): 2303-2309.doi: 10.3969/j.issn.2095-4344.2586
Previous Articles Next Articles
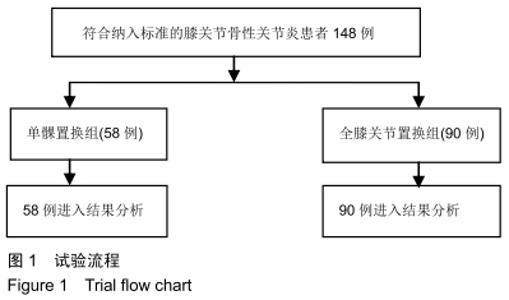
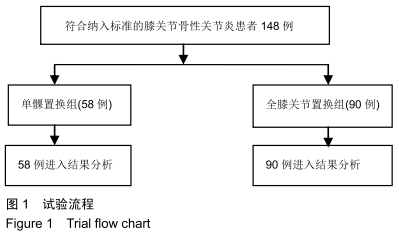
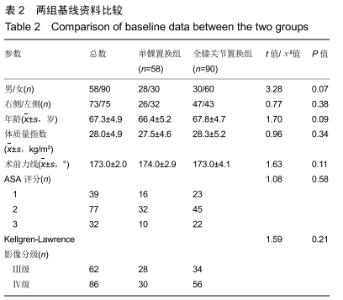
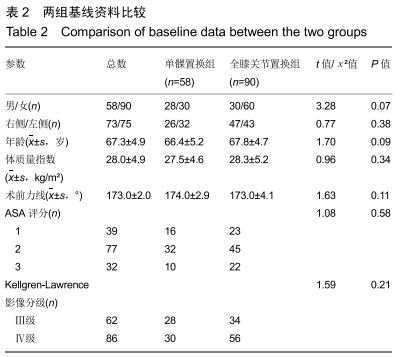
Comparison of occult blood loss after unicompartmental knee arthroplasty and total knee arthroplasty
Peng Chao1, Liu Yunpeng2, Wang Xiaolong1, Wang Xingliang2, Yang Jiaji2, Hua Guojun2
- 1Anhui Medical University, Hefei 230000, Anhui Province, China; 2The 904 Hospital of the Joint Service Support Force of Chinese PLA, Wuxi 214000, Jiangsu Province, China
-
Received:2019-10-08Revised:2019-10-11Accepted:2019-11-14Online:2020-05-28Published:2020-03-19 -
Contact:Liu Yunpeng, Chief physician, The 904 Hospital of the Joint Service Support Force of Chinese PLA, Wuxi 214000, Jiangsu Province, China -
About author:Peng Chao, Master candidate, Anhui Medical University, Hefei 230000, Anhui Province, China -
Supported by:the Science and Technology Development Foundation Project of Wuxi, No. CSE31N1618; the Scientific Research Project of Health and Family Planning Commission of Wuxi, No. Q201772
CLC Number:
Cite this article
Peng Chao, Liu Yunpeng, Wang Xiaolong, Wang Xingliang, Yang Jiaji, Hua Guojun. Comparison of occult blood loss after unicompartmental knee arthroplasty and total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(15): 2303-2309.
share this article
| [1] ALSHRYDA S, SARDA P, SUKEIK M, et al. Tranexamic acid in total knee replacement: a systematic review and meta-analysis. J Bone Joint Surg Br.2011;93:1577-1585. [2] BONG MR, PATEL V, CHANG E, et al. Risks associated with blood transfusion after total knee arthroplasty.J Arthroplast. 2004;19:281-287. [3] ZHANG ZF, MIN JK, WANG D, et al. Analysis on the occult blood loss after unicompartment knee arthroplasty.Zhongguo Gu Shang.2017;30(11):1013-1017. [4] SEHAT KR, EVANS RL, NEWMAN JH. Hidden blood loss fol-lowing hip and knee arthroplasty. Correct management of blood loss should take hidden blood loss into amlount.J Bone Joint Surg Br.2004;86(4):561-565. [5] SPAHN DR.Anemia and patient blood management in hip and knee surgery: a systematic review of the literature. Anesthesiology. 2010;113(2):482-495. [6] TAI TW, LIN CJ, JOU IM, et al.Tourniquet use in total knee arthroplasty: a meta-analysis. Tourniquet use in total knee arthroplasty: a meta-analysis.Knee Surg Sports Traumatol Arthrosc.2011;19(7):1121-1130. [7] MOCHIZUKI T, YANO K, IKARI K, et al.Platelet-rich plasma for the reduction of blood loss after total knee arthroplasty: a clinical trial.Eur J Orthop Surg Traumatol.2016;26(8): 901-905. [8] KELLEY TC, TUCKER KK, ADAMS MJ, et al.Use of tranexamic acid results in decreased blood loss and decreased transfusions in patients undergoing staged bilateral total knee arthroplasty.Transfusion.2014;54:26-30. [9] SU EP, SU S.Strategies for reducing peri-operative blood loss in total knee arthroplasty.Bone Joint J.2016;98-B(1 Suppl A): 98-100. [10] KO PS, TIO MK, TANG YK, et al.Sealing the intramedullary femoral canal with autologous bone plug in total knee arthroplasty. J Arthroplasty.2003;18:6-9. [11] KUMAR N, SALEH J, GARDINER E, et al.Plugging the intramedullary canal of the femur in total knee arthroplasty: reduction in postoperative blood loss. J Arthroplasty. 2000; 15:947-949. [12] YUENYONGVIWAT V, TUNTARATTANAPONG P, IAMTHANAPORN K, et al.Intramedullary sealing with a bone plug in total knee arthroplasty to reduce blood loss: a meta-analysis of randomized controlled trials.J Orthop Surg Res.2019;14:96. [13] GUAY J.The effect of neuraxial blocks on surgical blood loss and blood transfusion requirements: a meta-analysis.J Clin Anesth.2006;18(2):124-128. [14] HU S, ZHANG ZY, HUA YQ, et al.A comparison of regional and general anaesthesia for total replacement of the hip or knee: a meta-analysis.J Bone Joint Surg Br.2009;91:935-942. [15] ZHANG Z, LIANG J, ZUO X, et al.Effect of pneumatic tourniquet on perioperative blood loss in total knee arthroplasty. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2019;33(6):681-684. [16] LI Z, LIU D, LONG G, et al.Association of tourniquet utilization with blood loss, rehabilitation, and complications in Chinese obese patients undergoing total knee arthroplasty: A retrospective study.Medicine(Baltimore).2017;96:e9030. [17] KHANNA A, GOUGOULIAS N, LONGO UG, et al.Minimally invasive total knee arthroplasty: a systematic review.Orthop Clin North Am.2009;40:479-489. [18] ZHANG B, PANG QJ, ZHANG HJ, et al. Progress on recessive blood loss after total knee arthroplasty.Zhongguo Gu Shang. 2012;25:788-792. [19] LOMBARDI AV JR, BEREND KR, WALTER CA, et al.Is recovery faster for mobile-bearing unicompartmental than total knee arthroplasty?Clin Orthop Relat Res. 2009;467: 1450-1457. [20] YANG KY, WANG MC, YEO SJ, et al. Minimally invasive unicondylar versus total condylar knee arthroplasty--early results of a matched-pair comparison.Singapore Med J. 2003;44:559-562. [21] SCHWAB PE, LAVAND'HOMME P, YOMBI JC, et al.Lower blood loss after unicompartmental than total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2015;23:3494-3500. [22] CANKAYA D, DELLA VALLE CJ. Blood Loss and Transfusion Rates in the Revision of Unicompartmental Knee Arthroplasty to Total Knee Arthroplasty Are Similar to Those of Primary Total Knee Arthroplasty But Are Lower Compared With the Revision Total Knee Arthroplasty.J Arthroplasty. 2016;31: 339-341. [23] AHN JH, KANG DM, CHOI KJ.Bilateral simultaneous unicompartmental knee arthroplasty versus unilateral total knee arthroplasty: A comparison of the amount of blood loss and transfusion, perioperative complications, hospital stay, and functional recovery.Orthop Traumatol Surg Res. 2017; 103:1041-1045. [24] HU KZ, SUN HY, SUI C. Effects of five treatment regimens on blood loss and blood transfusion in total knee arthroplasty: a preliminary study in China.Int J Clin Pharmacol Ther.2017;55: 433-441. [25] FU X, TIAN P, LI Z, et al.Postoperative leg position following total knee arthroplasty influences blood loss and range of motion: a meta-analysis of randomized controlled trials.Curr Med Res Opin.2016;32:771-778. [26] FALDINI C, TRAINA F, DE FINE M, et al.Post-operative limb position can influence blood loss and range of motion after total knee arthroplasty: a systematic review.Knee Surg Sports Traumatol Arthrosc.2015;23(3):852-859. [27] WU Y, YANG T, ZENG Y, et al. Effect of different postoperative limb positions on blood loss and range of motion in total knee arthroplasty: An updated meta-analysis of randomized controlled trials.Int J Surg.2017;37:15-23. [28] LIN C, QI Y, JIE L, et al. Is combined topical with intravenous tranexamic acid superior than topical, intravenous tranexamic acid alone and control groups for blood loss controlling after total knee arthroplasty: A meta-analysis.Medicine (Baltimore). 2016;95(51):e5344. [29] AGGARWAL AK, SINGH N, SUDESH P. Topical vs Intravenous Tranexamic Acid in Reducing Blood Loss After Bilateral Total Knee Arthroplasty: A Prospective Study.J Arthroplasty. 2016;31: 1442-1448. [30] WU J, FENG S, CHEN X, et al.Intra-Articular Injection of Tranexamic Acid on Perioperative Blood Loss During Unicompartmental Knee Arthropla.sty.Med Sci Monit.2019;25: 5068-5074. [31] ISHII Y, NOGUCHI H, SATO J, et al. Effect of a single injection of tranexamic acid on blood loss after primary hybrid TKA.Knee.2015;22:197-200. [32] ZHANG YM, YANG B, SUN XD, et al.Combined intravenous and intra-articular tranexamic acid administration in total knee arthroplasty for preventing blood loss and hyperfibrinolysis: A randomized controlled trial.Medicine(Baltimore). 2019;98: e14458. [33] ISEKI T, TSUKADA S, WAKUI M, et al. Intravenous tranexamic acid only versus combined intravenous and intra-articular tranexamic acid for perioperative blood loss in patients undergoing total knee arthroplasty.Eur J Orthop Surg Traumatol.2018;28:1397-1402. [34] PONGCHAROEN B, RUETIWARANGKOON C.Does tranexamic acid reduce blood loss and transfusion rates in unicompartmental knee arthroplasty?J Orthop Sci.2016;21(2):211-215. [35] BROWN NM, SHETH NP, DAVIS K, et al. Total knee arthroplasty has higher postoperative morbidity than unicompartmental knee arthro-plasty: a multicenter analysis.J Arthroplast. 2012;27(8 Suppl):86-90. [36] SALIDO JA, MARÍN LA, GÓMEZ LA, et al. Preoperative hemoglobin levels and the need for transfusion after prosthetic hip and knee surgery: analysis of predictive factors.J Bone Joint Surg Am.2002;84:216-220. [37] FUJIMOTO H, OZAKI T, ASAUMI K, et al.Blood loss in patients for total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc.2003;11:149-154. [38] JANS Ø, JØRGENSEN C, KEHLET H, et al. Role of preoperative anemia for risk of transfusion and postoperative morbidity in fast-track hip and knee arthroplasty. Transfusion. 2014; 54(3):717-726. [39] MINODA Y, SAKAWA A, FUKUOKA S, et al. Blood management for patients with hemoglobin level lower than 1300g/L in total knee arthroplasty.Arch Orthop Trauma Surg. 2004;124(5):317-319. [40] LI Y, LI B G, ZHAO R, et al.Effect of autologous blood transfusion device on preventing blood loss in primary total knee arthroplasty using comprehensive hemostatic methods. Beijing Da Xue Xue Bao.2018;50:651-656. [41] ZHANG H, CHEN J, CHEN F, et al.The effect of tranexamic acid on blood loss and use of blood products in total knee arthro-plasty: a meta-analysis.Knee Surg Sports Traumatol Arthrosc.2012;20(9):1742-1752 |
| [1] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [2] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [3] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [4] | Cao Xuhan, Bai Zixing, Sun Chengyi, Yang Yanjun, Sun Weidong. Mechanism of “Ruxiang-Moyao” herbal pair in the treatment of knee osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 746-753. |
| [5] | Li Yonghua, Feng Qiang, Tan Renting, Huang Shifu, Qiu Jinlong, Yin Heng. Molecular mechanism of Eucommia ulmoides active ingredients treating synovitis of knee osteoarthritis: an analysis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 765-771. |
| [6] | Yang Wei, Chen Zehua, Yi Zhiyong, Huang Xudong, Han Qingmin, Zhang Ronghua. Effectiveness of intra-articular injection of hyaluronic acid versus placebo in the treatment of early and mid-stage knee osteoarthritis: a Meta-analysis based on randomized, double-blind, controlled, clinical trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3760-3766. |
| [7] | Deng Zhibo, Li Zhi, Wu Yahong, Mu Yuan, Mu Yuexi, Yin Liangjun. Local infiltration anesthesia versus femoral nerve block for pain control and safety after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3401-3408. |
| [8] | Mieralimu•Muertizha, Ainiwaerjiang•Damaola, Lin Haishan, Wang Li . Relationship between tibio-femoral mechanical axis deviation on coronal plane and early joint function recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3300-3304. |
| [9] | Zuo Xiuqin, Yin Sasa, Xie Huimin, Jia Zishan, Zhang Lining. Applicability and specifications of platelet-rich plasma in musculoskeletal repair [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3239-3245. |
| [10] | Huang Chenyu, Tang Cheng, Wei Bo, Li Jiayi, Li Xuxiang, Zhang Huikang, Xu Yan, Yao Qingqiang, Wang Liming. Application of three-dimensional printing guide plate in total knee arthroplasty for patients with varus and valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2789-2793. |
| [11] | Li Shangzhi, Zheng Dezhi, Liu Jun. Early analgesia of cocktail therapy after total knee arthroplasty with enhanced recovery after surgery program [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2794-2798. |
| [12] | Liu Jinlei, Yin Li, Zhang Yi, Wang Haitao, Li Zhuangyan, Xia Peige, Qiao Renqiu. Effects of intravenous tranexamic acid combined with periarticular multipoint injection of tranexamic acid cocktail on blood loss and pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2833-2839. |
| [13] | Xu Hui, Kang Bingxin, Gao Chenxin, Zhao Chi, Xu Xirui, Sun Songtao, Xie Jun, Xiao Lianbo, Shi Qi. Effectiveness of Tuina in the treatment of pain after total knee arthroplasty in patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2840-2845. |
| [14] | Deng Bo, Hong Hainan, Fan Yongyong, Cai Guoping, Feng Xingbing, Hong Zhenghua. Efficacy and safety of tourniquet application in total knee arthroplasty and only at the time of cementing: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2908-2914. |
| [15] | Zhong Yuanming, Fu Xiaopeng, Xu Wei, Zhao Qingrui, Huang Yong, Ye Weiquan. Nicardipine controlled hypotension applied to perioperative blood loss in orthopedics: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2930-2937. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||