Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (48): 8331-8336.doi: 10.3969/j.issn.2095-4344.2013.48.006
Previous Articles Next Articles
Crowe IV developmental dysplasia treated by total hip arthroplasty with subtrochanteric osteotomy
Gu Jian-ming, Du Hui, Shao Hong-yi, Zhou Yi-xin
- Department of Adult Joint Reconstruction, Beijing Jishuitan Hospital, Beijing 100035, China
-
Online:2013-11-26Published:2013-11-26 -
Contact:Zhou Yi-xin, Ph.D, Chief physician, Department of Adult Joint Reconstruction, Beijing Jishuitan Hospital, Beijing 100035, China orthoyixin@yahoo.com -
About author:Gu Jian-ming☆, Ph.D., Attending physician, Department of Adult Joint Reconstruction, Beijing Jishuitan Hospital, Beijing 100035, China pumc_gu@163.com
CLC Number:
Cite this article
Gu Jian-ming, Du Hui, Shao Hong-yi, Zhou Yi-xin . Crowe IV developmental dysplasia treated by total hip arthroplasty with subtrochanteric osteotomy[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(48): 8331-8336.
share this article
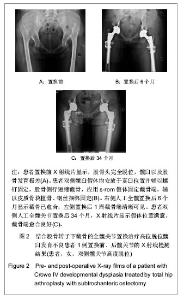
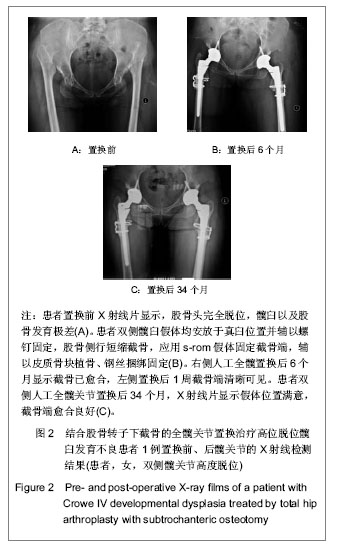
2.1 受试者数量分析 纳入患者17例(21髋)均进入结果分析,无脱落。 2.2 受试者临床资料分析 在17例患者中,1例(1髋)既往行股骨近端外翻截骨术。患者10例(12髋)形成假臼,7例(9髋)无假臼形成。患者有双侧髋臼发育不良者共计7例,其中4例(8髋)行双侧人工全髋关节置换合并转子下短缩截骨,另外3例患者仅单侧行人工全髋关节置换合并转子下短缩截骨(1例患者对侧为crowe3型高位脱位的髋臼发育不良行单纯人工全髋关节置换治疗,另外2例未行髋关节置换治疗)。1例患者对侧髋关节患有髋内翻短颈畸形,其他9例对侧髋关节均为正常。 患者1例(2髋)采用骨水泥髋臼假体ZCA(美国捷迈公司),其中1髋使用自体股骨头行结构性植骨。另外16例(19髋)皆采用非水泥假体,1髋为trilogy(美国捷迈公司)假体,13髋采用TM(美国捷迈公司)假体,2髋采用duraloc(美国强生公司)假体,2髋为duraloc option(美国强生公司)假体。 髋臼假体平均外径为(41.7±3.0) mm(38.0- 46.0 mm)。髋臼假体平均外展角为(46.1±9.1)° (31.4°- 61.4°),前倾角平均为(14.8±6.7)°(5.5°-28.6°)。股骨假体平均大小为(10.7±2.0)号(8-15号),16髋为22 mm股骨头,5髋使用28 mm股骨头,股骨头假体皆为+0 mm。 2.3 典型病例 见图2。"
| [1] Charnley J, Feagin JA. Low-friction arthroplasty in congenital subluxation of the hip. Clin Orthop. 1973;(91):98-113. [2] Sochart DH, Porter ML. The long-term results of Charnley low-friction arthroplasty in young patients who have congenital dislocation, degenerative osteoarthrosis, or rheumatoid arthritis. J Bone Joint Surg Am. 1997;79(11): 1599-1617. [3] Harris WH, Crothers O, Oh I. Total hip replacement and femoralhead bone-grafting for severe acetabular deformity in adults. J Bone Joint Surg Am. 1977;59(6):752-759. [4] Pagnano MW, Hanssen AD, Lewallen DG, et al. The effect of superior placement of the acetabular component on the rate of loosening after total hip arthroplasty. J Bone Joint Surg Am. 1996;78(7):1004-1014. [5] Becker DA, Gustilo RB. Double-chevron subtrochanteric shortening derotational osteotomy combined with total hip arthroplasty for treatment of complete congenital dislocation of the hip in the adult. J Arthroplasty. 1995;10(3): 313-318. [6] Reikeraas O, Lereim P, Gabor I, et al. Femoral shortening in total arthroplasty for completely dislocated hips: 3–7 years results in 25 cases. Acta Orthop Scand. 1996; 67(1): 33-36. [7] Eskelinen A, Helenius I, Remes V, et al. Cementless total hip arthroplasty in patients with high congenital hip dislocation. J Bone Joint Surg Am. 2006;88(1):80-91. [8] Makita H, Inaba Y, Hirakawa K, et al. Results on total hip arthroplasties with femoral shortening for Crowe's group IV dislocated hips. J Arthroplasty. 2007;22(1):32-38. [9] Linde F, Jensen J. Socket loosening in arthroplasty for congenital dislocation of the hip. Acta Orthop Scand. 1988; 59(3):254-257. [10] Hartofilakidis G, Stamos K, Ioannidis TT. Low-friction arthroplasty for old untreated congenital dislocation of the hip. J Bone Joint Surg Br. 1988;70(2):182-186. [11] Hartofilakidis G, Karachalios T. Total hip arthroplasty for congenital hip disease. J Bone Joint Surg Am. 2004;86-A(2): 242-250. [12] Pagnano MW, Hanssen AD, Lewallen DG, et al. The effect of superior placement of the acetabular component on the rate of loosening after total hip arthroplasty. J Bone Jt Surg Am. 1996;78(7):1004-1014. [13] Yoder SA, Brand RA, Pedersen DR, et al. Total hip acetabular component position affects component loosening rates. Clin Orthop Relat Res. 1988;(228):79-87. [14] Symeonides PP, Pournaras J, Petsatodes G, et al. Total hip arthroplasty in neglected congenital dislocation of the hip. Clin Orthop Relat Res.1997;(341):55-61. [15] Reikeeraas O, Lereim P, Gabor I, et al. Femoral short ening in total arthroplasty for completely dislocated hips: 3-7 year result s in 25 cases. Acta Orthop Scand. 1996;67(1):33-36. [16] Baz AB, Senol V, Akalin S, et al. Treatment of high hip dislocation with a cementless stem combined with a shortening osteotomy. Arch Orthop Trauma Surg. 2012;132 (10):1481-1486. [17] Sonohata M, Tajima T, Kitajima M, et al. Total hip arthroplasty combined with double-chevron subtrochanteric osteotomy. J Orthop Sci. 2012;17(4):382-389. [18] Macheras GS, Kateros K, Koutsostathis SD,et al.The Trabecular Metal Monoblock acetabular component in patients with high congenital hip dislocation. J Bone Joint Surg Br. 2010;92(5):624-628. [19] Stans AA, Pagnano MW, Shaughnessy WJ, et al. Results of total hip arthroplasty for Crowe Type III developmental hip dysplasia. Clin Orthop Relat Res. 1998;(348):149-157. [20] Yoder SA, Brand RA, Pedersen DR, et al. Total hip acetabular component position affects component loosening rates. Clin Orthop Relat Res. 1988;(228):79-87. [21] Lai KA, Shen WJ, Huang LW, et al. Cementless total hip arthroplasty and limb-length equalization in patients with unilateral Crowe type-IV hip dislocation. J Bone Joint Surg Am. 2005;87(2):339-345. [22] Lewallen DG. Neurovascular injury associated with hip arthroplasty. Instr Course Lect. 1988;47:275-283. [23] Edwards BN, Tullos HS, Noble PC. Contributory factors and etiology of sciatic nerve palsy in total hip arthroplasty. Clin Orthop. 1987;(218):136-141. [24] Tanoue M, Yamaga M, Ide J, et al. Acute stretching of peripheral nerve inhibits retrograde axonal transport. J Hand Surg Br. 1996;21(3):358-363. [25] Kiliço?lu O?, Türker M, Akgül T, et al. Cementless total hip arthroplasty with modified oblique femoral shortening osteotomy in Crowe type IV congenital hip dislocation. J Arthroplasty. 2013;28(1):117-125. [26] Akiyama H, Kawanabe K, Yamamoto K, et al. Cemented total hip arthroplasty with subtrochanteric femoral shortening transverse osteotomy for severely dislocated hips: outcome with a 3- to 10-year follow-up period. J Orthop Sci. 2011;16(3): 270-277. [27] Eggli S, Hankemayer S, Müller ME. Nerve palsy after leg lengthening in total replacement arthroplasty for developmental dysplasia of the hip. J Bone Joint Surg Br. 1999;81(5):843-845. [28] Hartofilakidis G, Babis GC, Georgiades G, et al. Trochanteric osteotomy in total hip replacement for congenital hip disease. J Bone Joint Surg Br. 2011;93(5):601-607. [29] Koulouvaris P, Stafylas K, Sculco T, et al. Distal femoral shortening in totalhip arthroplasty for complex primary hip reconstruction: a new surgical technique. J Arthroplasty. 2008; 23(7):992-998. [30] Anwar MM, Sugano N, Masuhara K, et al. Total hip arthroplasty in the neglected congenital dislocation of the hip. A five- to 14-year follow-up study. Clin Orthop Relat Res. 1993; (295):127-134. [31] Kilicarslan K, Yalcin N, Cicek H, et al. What happens at the adjacent knee joint after total hip arthroplasty of Crowe type III and IV dysplastic hips? J Arthroplasty. 2012;27(2):266-270. [32] Whiteside LA, Arima J, White SE, et al. Fixation of the modular total hip femoral component in cementless total hip arthroplasty. Clin Orthop Relat Res. 1994;(298):184-190. [33] Cameron HU. Management of femoral deformities during the total hip replacement. Contemp Orthop. 1996;19(9):745-746. [34] Bernasek TL, Haidukewych GJ, Gustke KA, et al. Total hip arthroplasty requiring subtrochanteric osteotomy for developmental hip dysplasia: 5- to 14-year results. J Arthroplasty. 2007;22(6 Suppl 2):145-150. [35] Onodera S, Majima T, Ito H, et al. Cementless total hip arthroplasty using the modular S-ROM prosthesis combined with corrective proximal femoral osteotomy. J Arthroplasty. 2006;21(5):664-669. [36] Masonis JL, Patel JV, Miu A, et al. Subtrochanteric shortening and derotational osteotomy in primary total hip arthroplasty for patients with severe hip dysplasia: 5-year follow-up. J Arthroplasty. 2003;18(3 Suppl 1):68-73. [37] Takao M, Ohzono K, Nishii T, et al. Cementless modular total hip arthroplasty with subtrochanteric shortening osteotomy for hips with developmental dysplasia. J Bone Joint Surg Am. 2011;93(6):548-555. [38] Dallari D, Pignatti G, Stagni C, et al. Total hip arthroplasty with shortening osteotomy in congenital major hip dislocation sequelae. Orthopedics. 2011;34(8):e328-333. [39] Crowe JF, Mani VJ, Ranawat CS. Total hip replacement in congenital dislocation and dysplasia of the hip. J Bone Joint Surg Am. 1979;61(1):15-23. [40] State Council of the People's Republic of China. Administrative Regulations on Medical Institution. 1994-09-01. |
| [1] | Cui Keze, Guo Xiang, Han Guibin, Chen Yuanliang, Liu Yiheng, Zhong Haibo. Learning curve and early clinical results of total hip arthroplasty with MAKO robot assisted posterolateral approach [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1313-1317. |
| [2] | Deng Biyong, Deng Bixiang. Differences in relative parameters of acetabulum in hip arthroplasty between CT horizontal plane and CT true pelvic plane [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1405-1409. |
| [3] | Ai Di. Absorbable suture anchors for treating femoroacetabular impingement syndrome combined with acetabular labral tears [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(4): 499-504. |
| [4] | Wang Hui, Zhang Yazhou, Shi Lifang. Three-dimensional model analysis of trabecular acetabular cup and solid acetabular cup [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 390-394. |
| [5] | Yan Yan, Zhao Yan, Fu Fanyu, He Haijun. Systematic evaluation and meta-analysis of total hip arthroplasty with three-dimensional printing model in preoperative planning [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(21): 3423-3429. |
| [6] | Chen Haopeng, Xie Hui, Fu Weimin, Wang Benjie, Zhao Dewei. Effect of body mass index on the early-term hip functional recovery after total hip arthroplasty by three-dimensional gait analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(18): 2842-2847. |
| [7] | Chen Yong, Zhang Bin. Three-dimensional printing technique-assisted total hip arthroplasty for developmental dysplasia of the hip in adults [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(36): 5772-5776. |
| [8] | Cai Zhencun, Piao Chengzhe, Zhou Hongyu, Sun Ming, Gao Zhenhuai. Stress characteristics after fixation in herringbone position in children with developmental dislocation of the hip by finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(36): 5841-5845. |
| [9] | Liu Dahai, Li Haibo, Gou Yongsheng, Li Liang. Effects of different body positions and traction weights on hip bursa pressure after femoral neck fracture [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(36): 5846-5849. |
| [10] | Huang Youyi, Yuan Wei. Application of 3D printing technology in hip diseases [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(34): 5538-5543. |
| [11] | Lian Chao, Zhang Maorong, Wang Junyuan, Cheng Bo, Liu Feng. Relationship between femoral head diameter and edge load under dynamic micro-separation of ceramic hip joints [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(32): 5085-5091. |
| [12] | Yang Jian, Liang Can, Zhang Huizhong. Efficacy of structural bone graft for reconstruction of acetabulum in total hip arthroplasty in patients with developmental dysplasia of hips and severe acetabular defect [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(32): 5092-5096. |
| [13] |
Tan Zhe, Li Kainan, Lan Hai.
Comparison of the efficacy of intramedullary nail fixation assisted by orthopedic robot navigation and traditional surgery for intertrochanteric fractures
[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(24): 3792-3797.
|
| [14] | Su Lianbin, Feng Eryou, Zhang Yiyuan, Zhuo Youguang, Xiao Lili, Wang Wulian, Lin Feitai. Whether direct anterior approach for total hip arthroplasty is a risk factor of eccentric reaming to the anterior column of the acetabulum? [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(20): 3117-3123. |
| [15] | Chen Qunqun, Zhou Chi, He Wei. Relationship between bone marrow edema and “survival with collapse” of osteonecrosis of the femoral head assessed by X-ray [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(20): 3170-3175. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||