Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (14): 2278-2283.doi: 10.3969/j.issn.2095-4344.0763
Previous Articles Next Articles
Types and properties of injection-molded thermoplastic denture base resins
Long Yan-ming, Li Xiao-jie
- Department of Prosthodontics, Affiliated Hospital of Stomatology, Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China
-
Received:2017-12-24Online:2018-05-18Published:2018-05-18 -
Contact:Li Xiao-jie, Associate professor, Master’s supervisor, Department of Prosthodontics, Affiliated Hospital of Stomatology, Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China -
About author:Long Yan-ming, Master candidate, Department of Prosthodontics, Affiliated Hospital of Stomatology, Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China -
Supported by:the Natural Science Foundation of Guangxi Zhuang Autonomous Region, No. 2013GXNSFBA019162; the Basic Ability Improving Project of Young Teachers in Guangxi Universities, No. 2017KY0092
CLC Number:
Cite this article
Long Yan-ming, Li Xiao-jie . Types and properties of injection-molded thermoplastic denture base resins[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(14): 2278-2283.
share this article
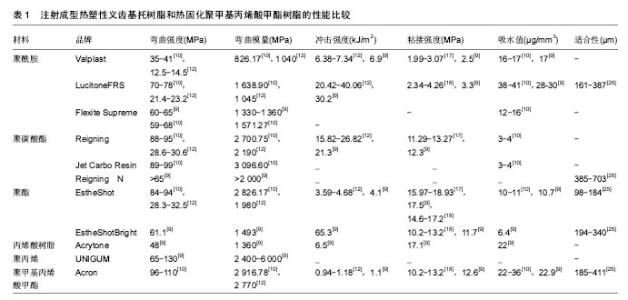
2.1 注射成型热塑性义齿基托树脂的种类与性能 注射成型热塑性树脂材料众多,目前被报道可作为义齿材料的有以下5种:聚酰胺、聚碳酸酯、聚酯、丙烯酸树脂、聚丙烯;临床应用最多的是聚酰胺,而丙烯酸树脂和聚丙烯近年才开始有研究报道,目前应用较少;聚酰胺通用名为尼龙,在20世纪50年代由美国Valplast公司生产,这些聚酰胺通过二胺和二元酸之间的缩合反应制备,为半结晶聚合物,其弹性最高,抗冲击能力好,但硬度低易刮花、水吸收值较高、颜色不稳定、椅旁重衬困难;聚碳酸酯的大分子链上含有苯环、季碳原子、氧键及酯基,它是可非晶或半结晶形式存在的特殊树脂,其适合性较差,但具有较好的刚性,吸水值低,可进行椅旁重衬;聚酯分为聚对苯二甲酸乙二醇酯共聚物与聚对苯二甲酸环己烷酯共聚物2种,为半晶体聚合物,其最大的优点是适合性好,椅旁重衬效果最好,但其冲击强度低,意味着折断风险高;丙烯酸树脂与热固化PMMA树脂有相同的化学组成甲基丙烯酸甲酯,但它们的成型方式不同,丙烯酸树脂为注射成型,其细胞毒性比热固化PMMA树脂小,而水吸收值比聚酰胺低,颜色较稳定,因此,理论上其同时具有热固化PMMA树脂和聚酰胺的优点,为较理想的义齿材料,但缺乏长期临床应用效果观察[8-27]。 为了正确指导临床应用,需详细评价注射成型热塑性义齿基托树脂的性能,目前已被评价的材料性能包括弹性模量和弯曲强度、冲击强度、粘接强度、水吸收和水溶解、适合性、硬度和表面粗糙度、颜色稳定性等。由于材料种类多,临床测试方法和依据标准多样,因此造成不同科学研究中的数值差别较大;文章把已检测的材料的品牌和部分性能列于表1中。"
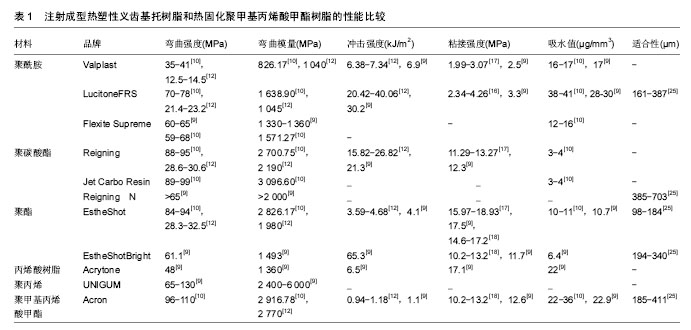
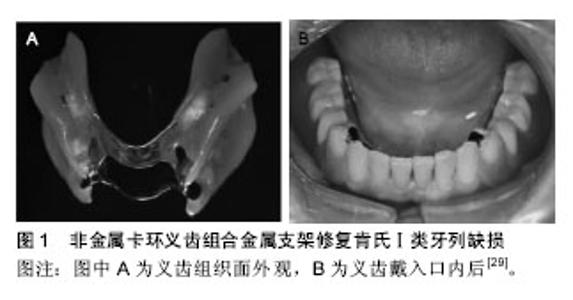
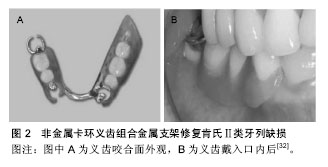
2.1.1 弹性模量和弯曲强度 注射成型热塑性义齿基 托树脂的低刚性使其可作为义齿卡环使用,刚性可用弹性模量表征。Takabayashi等[10]研究发现,热固化PMMA树脂的弹性模量和弯曲强度总的来说最高,在研究的几种注射成型热塑性义齿基托树脂中,聚碳酸酯的弹性模量和弯曲强度最高,聚酰胺最低,因此,由聚酰胺制作的义齿的卡环固位力将比其他义齿树脂材料强。 然而,作为义齿基托材料,注射成型热塑性义齿基托树脂的刚性需被加强。根据ISO 1567:2005标准规定,义齿基托树脂的弯曲强度应不低于65 MPa,弹性模量应不低于2 000 MPa[10-11],如果义齿基托树脂刚性较低,将会导致由其制造的义齿基托在咀嚼期间倾向于变形,变形产生垂直应力,义齿基托下面的松质骨在应力作用下将发生再吸收[12]。Sasaki等[13]使用连续单向玻璃纤维增强复合材料和金属丝,以增强聚酰胺、聚酯与聚碳酸酯的刚性,得到令人满意的效果。Nagakura等[14]认为10%或20%玻璃纤维含量对于制备玻璃纤维增强注射成型热塑性义齿基托树脂是有益的。在另一项研究中,Takahashi等[15]发现热循环也可显著提高注射成型热塑性义齿基托树脂的刚性。 2.1.2 冲击强度 当义齿受到冲击负荷时,冲击强度大的义齿材料不易断裂,因此,对注射成型热塑性义齿基托树脂冲击强度大小的评价有利于临床应用。在Hamanaka等[12]的冲击实验中,热固化PMMA树脂与聚酯冲击强度最低,意味着折断风险高;聚酰胺(Lucitone FRS®)和聚碳酸酯具有良好的冲击强度,聚酰胺(Valplast®)则出现中等的冲击强度,可能与其吸水性有关。 2.1.3 粘接强度 注射成型热塑性义齿基托树脂与自凝树脂粘接强度的大小意味着其能否进行椅旁重衬。丙烯酸树脂与热固化PMMA树脂具有相同的化学组成甲基丙烯酸甲酯,因此丙烯酸树脂与自凝树脂的粘接强度类似于热固化PMMA树脂[16]。Hamanaka等[17]测试了聚酰胺、聚酯和聚碳酸酯与自凝树脂的粘接强度,结果显示聚酯的粘接强度最高,其次是聚碳酸酯,聚酯与聚碳酸酯可椅旁重衬,而聚酰胺在没有任何处理的情况下难以与自凝树脂结合。在Hamanaka等[18]的另一项研究中,一种聚酯(EstheShot®)的剪切粘接强度明显高于另一种聚酯(EstheShot Bright®)和热固化PMMA树脂;而聚酯(EstheShot Bright®)与热固化PMMA树脂的剪切粘接强度没有显著不同,因此,在临床使用中两种聚酯理论上都可进行椅旁重衬。 由于聚酰胺与自凝树脂之间不能产生足够的粘接强度,临床重衬困难;因此,为了提高这种粘接强度,研究者分别使用摩擦化学二氧化硅涂层+4- META/MMA-TBB树脂、较小颗粒尺寸的二氧化硅进行摩擦化学涂层处理注射成型热塑性义齿基托树脂表面,有效改善了聚酰胺、聚酯和聚碳酸酯与自凝树脂之间的粘接强度[17,19-20]。Korkmaz等[21]发现使用2 W-20 HZ的Er,Cr:YSGG激光处理聚酰胺表面可增强聚酰胺与热固化软衬树脂(Molloplat-B®)的黏结强度,但进行氧化铝喷砂将影响聚酰胺与热固化软衬树脂的结合。 2.1.4 水吸收和水溶解 义齿材料的高吸水值将引起口腔异味、义齿变色和尺寸不稳定,最终降低义齿的使用寿命[22]。根据ISO 20795-1: 2008标准规定,义齿树脂的吸水值应不大于32 μg/mm3,Takabayashi等[10]比较了6种注射成型热塑性义齿基托树脂和热固化PMMA树脂的水吸收性,结果显示除了一种聚酰胺(Lucitone FRS®),所有测试注射成型热塑性义齿基托树脂的水吸收值比热固化PMMA树脂低,其中聚碳酸酯表现出最低的水吸收值;研究指出聚酰胺的亲水特性可能与酰胺基团浓度有关,酰胺基团浓度越高,水吸收值越大,因此建议通过调节酰胺基团的浓度来减少水吸收值。 义齿材料在吸收水的同时,材料内的增塑剂、单体等组分随之溶解析出,因此,水溶解将影响义齿的物理和机械性能。在Shah等[23]的研究中,聚酰胺比热固化PMMA树脂水溶解度低,原因可能为热固化PMMA树脂较高的残余单体含量导致了其较高的水溶解度。另外,聚酰胺是结晶聚合物,这种结晶效应也解释了聚酰胺在水中较低溶解的原因[8]。 2.1.5 适合性 义齿材料的适合性受多种因素的影响,树脂的聚合收缩、热应力的释放、固化方式、基底几何结构的差异都将影响义齿的适合性[24]。注射成型热塑性义齿基托树脂的适合性需与热固化PMMA树脂相当,否则将影响其临床应用。Wada等[25]通过测量义齿材料与模型的平均间隙尺寸大小(单位μm)来评价注射成型热塑性义齿基托树脂与热固化PMMA树脂的适合性,结果显示聚酯(EstheShot®)的适合性显著高于热固化PMMA树脂,另一种聚酯(EstheShot Bright®)与聚酰胺(Lucitone FRS®)的适合性与热固化PMMA树脂类似,聚碳酸酯最低,因此聚酯与聚酰胺符合临床应用中的适合性要求;虽然聚碳酸酯的适合性低,但研究指出退火处理可显著提高其适合性。 2.1.6 硬度和表面粗糙度 在临床应用中,低硬度的义齿表面容易磨损,长期使用将有表面粗糙问题,而义齿材料表面粗糙度与斑块积累和白色念珠菌黏附直接相关[26]。在Shah等[23]研究中,与热固化PMMA树脂相比,聚酰胺显示更低的硬度值,该结果可部分归因于热固化PMMA树脂的分子结构和高的分子量;此外,交联剂也可影响表面硬度,注射成型热塑性义齿基托树脂较低的硬度值跟较低量的交联剂有关。 2.1.7 颜色稳定性 义齿表面的染色与其表面对颜料的吸附以及材料本身的吸水性、表面粗糙度和孔隙度等有关,染色将影响义齿的美观[22,27]。Takabayashi等[10]研究发现在咖喱溶液中浸泡60 h后,聚碳酸酯的颜色稳定性与热固化PMMA树脂相似,聚酰胺与聚酯显示出比热固化PMMA树脂更大的颜色变化,表明这些材料的颜 色稳定性需被改善,研究指出这些材料较大的颜色变化可能与其吸水性有关。此外,义齿材料表面粗糙度的差异也将影响义齿的颜色稳定性,注射成型热塑性义齿基托树脂较低的硬度值导致其表面容易磨损变粗糙,因此表面易染色[26]。 2.2 注射成型热塑性义齿基托树脂的临床应用 在口腔修复治疗中,患者的美观需求日趋提高。热固化PMMA树脂义齿暴露金属卡环,在美观方面已不能满足患者的需求。而由注射成型热塑性义齿基托树脂制作的义齿,不含金属卡环,因此可弥补热固化PMMA树脂义齿美观上的不足,其良好的柔韧性使卡环易于进入基牙倒凹,对基牙作用力小[28]。注射成型热塑性义齿基托树脂最早被用来制作不含金属和其他材料的义齿,命名为“弹性义齿”或“尼龙义齿”[2-3]。1995年,注射成型热塑性义齿基托树脂作为一种新型的义齿修复材料被引入国内,由于该种材料制作的义齿色泽接近牙龈,达到仿生隐形的效果,因此也被形象地称为“隐形义齿”[5]。但是,为了同时满足义齿的美观性和足够的刚性,注射成型热塑性义齿基托树脂结合金属支架或热固化PMMA树脂基托制作可摘局部义齿已有报道,该类义齿显然不能称为“弹性义齿”。因此,Fueki等[29]最近对注射成型热塑性义齿基托树脂义齿重新命名,称之为“非金属卡环义齿”。 由于非金属卡环义齿舒适美观,不易断裂,价格低廉,并且设计和制作过程比金属卡环热固化PMMA义齿简单[30],目前在国内已成为一种常规的修复方式。非金属卡环义齿主要用于少量前牙缺失的患者,但材料易老化而失去弹性,使用寿命仅3-5年,需要定期更换;由于其刚性不足,不可用于无功能负荷的游离端牙列缺损修复[29]。但有研究指出,非金属卡环义齿联合金属支架或热固化PMMA树脂基托可克服刚性不足的缺点,可用于修复各类牙列缺损,包括肯氏Ⅰ类(图1)、Ⅱ类(图2)、Ⅲ类(图3)、Ⅳ类牙列缺损,不仅保证了舒适美学,也确保了义齿的刚性,明显减少剩余牙槽嵴的吸收,并且可获得良好的固位和应力分布[29,31-32]。根据最近临床研究,配戴金属支架式非金属卡环义齿后,在面部外观、面部疼痛、心理影响等方面的口腔健康相关生活质量评估比金属卡环热固化PMMA义齿好[33]。周逸宁[34]根据义齿的固位稳固情况、基牙牙体牙周情况、咀嚼功能恢复及美观满意度,对肯氏Ⅰ类、Ⅱ类、Ⅲ类、Ⅵ类金属支架式非金属卡环义齿共156件进行一两年的随访观察,发现151件义齿取得满意疗效,因此,金属支架式非金属卡环义齿是一种具有广泛应用前景的牙列缺损修复方法。 非金属卡环义齿的应用禁忌取决于部分无牙颌和咬合关系的类型、影响义齿的设计和制造的解剖因素和可能影响义齿的维护和管理的口腔卫生状态:①对于没有垂直咬合止点和缺牙多的患者,即使使用金属卡环固位的可摘局部义齿修复也不能取得良好的预期效果,这种情况应慎重考虑使用非金属卡环义齿修复;②需要注意临床牙冠短、牙槽骨倒凹过大的患者,因为这些情况下很难设计合适形态和宽度的树脂卡环;在大多数非金属卡环义齿中,注射成型热塑性义齿基托树脂与人工牙通过机械固位结合,因此对于缺牙区颌间距离小的患者,人工牙容易脱落、破裂或折断,这种情况需注意;③树脂卡环覆盖基牙颈缘、游离龈,因此需要强调足够的菌斑控制,对于口腔卫生差,不能定期复诊的患者不宜非金属卡环义齿修复[29]。 非金属卡环义齿的多种材料性能各异,了解材料的特性和正确的使用方法对非金属卡环义齿的维护至关重要。非金属卡环义齿的维护与热固化PMMA树脂义齿不同,由于注射成型热塑性义齿基托树脂硬度低,容易刮花和变形,因此由该种材料制作的非金属卡环义齿不应用硬质义齿刷清洁,应该用软毛刷[9]。有研究表明超声波组合清洁剂清洗可明显减少义齿表面总细菌数,是替代机械清洗的合适方法[35]。但使用义齿清洁剂增加了注射成型热塑性义齿基托树脂的表面粗糙度,降低了硬度,导致义齿颜色改变,因此影响整个义齿的戴用耐久性和满意度,应建议患者定期复查[36-37]。碱性清洁剂不可用于聚酯,选义齿清洁剂时应注意[9]。研究指出聚酰胺不能直接进行椅旁重衬,但采用摩擦化学二氧化硅涂层+4-META/MMA-TBB树脂或激光等处理能明显增强其与自凝树脂或热固化软衬树脂的结合[17,21]。 "

| [1] 杨福生,赵延斌,吴靖.国外热塑性树脂基复合材料现状及发展趋势[J].吉林化工学院学报,2001,18(3):74-78.[2] Matthews E,Smith DC.Nylon as a denture base material.Br Dent J.1955;98(7):231-237.[3] Watt DM.Clinical assessment of nylon as a partial denture base material.Br Dent J.1955;98:238-244.[4] Pfeiffer P,Rosenbauer EU.Residual methyl methacrylate monomer, water sorption, and water solubility of hypoallergenic denture base materials.J Prosthet Dent. 2004;92(1):72.[5] 何国强,李建文,张雪华.弹性义齿(隐形义齿)[J].临床口腔医学杂志,1996,12(2):126-127.[6] Macgregor AR,Graham J,Stafford GD,et al. Recent experiences with denture polymers.J Dent. 1984;12(2): 146-157.[7] Stafford GD,Huggett R,Macgregor AR,et al.The use of nylon as a denture-base material.J Dent.1986;14(14):18-22.[8] 曾汉民.高分子复合材料的进展:纤维增强树脂基复合材料(续) [J].材料工程,1989,34(6):8-20.[9] Fueki K,Ohkubo C,Yatabe M,et al.Clinical application of removable partial dentures using thermoplastic resin. Part II: Material properties and clinical features of non-metal clasp dentures. J Prosthodont Res.2014;58(2):71.[10] Takabayashi Y.Characteristics of denture thermoplastic resins for non-metal clasp dentures. Dent MaterJ. 2010;29(4): 353-361.[11] Iwata Y.Assessment of clasp design and flexural properties of acrylic denture base materials for use in non-metal clasp dentures.J Prosthodont Res.2016;60(2):114-122.[12] Hamanaka I,Takahashi Y,Shimizu H.Mechanical properties of injection-molded thermoplastic denture base resins.Acta Odontologica Scandinavica.2011;69(2):75-79.[13] Sasaki H,Hamanaka I,Takahashi Y,et al.Effect of Reinforcement on the Flexural Properties of Injection-Molded Thermoplastic Denture Base Resins.J Prosthodont. 2015; 46(3):203-210.[14] Nagakura M,Tanimoto Y,Nishiyama N.Fabrication and physical properties of glass-fiber-reinforced thermoplastics for non-metal-clasp dentures.J Biomed Mater Res B Appl Biomater.2016.doi: 10.1002/jbm.b.33761. [Epub ahead of print].[15] Takahashi Y,Hamanaka I,Shimizu H.Effect of thermal shock on mechanical properties of injection-molded thermoplastic denture base resins.Acta Odontologica Scandinavica. 2012; 69(4):75.[16] Kim JH,Choe HC,Son MK.Evaluation of adhesion of reline resins to the thermoplastic denture base resin for non-metal clasp denture.Dent Mater J.2014;33(1):32-38.[17] Hamanaka I,Shimizu H,Takahashi Y.Shear bond strength of an autopolymerizing repair resin to injection-molded thermoplastic denture base resins.Acta Odontol Scand. 2013; 71(5):1250-1254.[18] Hamanaka I,Takahashi Y,Shimizu H.Properties of injection-molded thermoplastic polyester denture base resins.Acta Odontologica Scandinavica.2014;72(2):139.[19] Hamanaka I,Shimizu H,Takahashi Y.Bond strength of a chairside autopolymerizing reline resin to injection-molded thermoplastic denture base resins.J Prosthodont Res. 2017; 61(1):67-72. [20] Katsumata Y,Hojo S,Hamano N,et al.Bonding strength of autopolymerizing resin to nylon denture base polymer.Dent Mater J.2009;28(4):409-418.[21] Korkmaz FM,Bagis B,Ozcan M,et al.Peel strength of denture liner to PMMA and polyamide: laser versus air-abrasion.J Adv Prosthodont.2013;5(3):287-295.[22] Jang DE,Lee JY,Jang HS,et al.Color stability, water sorption and cytotoxicity of thermoplastic acrylic resin for non metal clasp denture.J Adv Prosthodont.2015;7(4):278-287.[23] Shah J,Bulbule N,Kulkarni S,et al.Comparative evaluation of sorption, solubility and microhardness of heat cure polymethylmethacrylate denture base resin & flexible denture base resin. J Clin Diagn Res.2014;8(8):ZF01-4.[24] Moussa ARA,Zaki DYI,Gabry HSE,et al.Comparative adaptation accuracy of heat cured and injection molded resin denture base materials.J Appl Sci Res.2012;36(1):1-23.[25] Wada J,Fueki K,Yatabe M,et al.A comparison of the fitting accuracy of thermoplastic denture base resins used in non-metal clasp dentures to a conventional heat-cured acrylic resin.Acta Odontologica Scandinavica.2015;73(1):33-37.[26] Kawara M,Iwata Y,Iwasaki M,et al.Scratch test of thermoplastic denture base resins for non-metal clasp dentures.J Prosthodont Res.2013;58(1):35-40.[27] Sagsoz NP,Yan?koglu N,Ulu H,et al.Color Changes of Polyamid and Polymetyhl Methacrylate Denture Base Materials.Open J Stomatol.2014;4(10):489.[28] Thakral GK,Aeran H,Yadav B,et al.Flexible Partial Dentures - A hope for the Challenged Mouth. Peoples J Sci Res. 2012; 5(2):55.[29] Fueki K,Ohkubo C,Yatabe M,et al.Clinical application of removable partial dentures using thermoplastic resin—Part I: Definition and indication of non-metal clasp dentures.J Prosthodont Res.2014;58(1):3.[30] Hundal M,Madan R.Comparative clinical evaluation of removable partial dentures made of two different materials in Kennedy Applegate class II partially edentulous situation.Med J Armed Forces India.2015;71(Suppl 2):S306-312.[31] 覃峰,王焱.弹性树脂固位体与PMMA基托联合应用改善传统活动义齿的美观[J].口腔颌面修复学杂志, 2001,2(2):21-22.[32] Ito M,Wee AG,Miyamoto T,et al.The combination of a nylon and traditional partial removable dental prosthesis for improved esthetics: a clinical report.J Prosthet Dent. 2013; 109(1):5-8.[33] Fueki K,Yoshida-Kohno E,Wakabayashi N.Oral-health related quality of life in patients with non‐metal clasp dentures: a randomized crossover trial.J Oral Rehabil. 2017;44(5): 405-413. [34] 周逸宁.铸造支架式隐形可摘局部义齿的临床应用体会[J].赣南医学院学报,2010,30(3):452-453.[35] Duyck J,Vandamme K,Krausch-Hofmann S,et al.Impact of Denture Cleaning Method and Overnight Storage Condition on Denture Biofilm Mass and Composition: A Cross-Over Randomized Clinical Trial. PloS One.2016;11(1):e0145837.[36] Ramadan MA,Mohamed DW,Nabil EA,et al.A Comparative Clinical Study of the Effect of Denture Cleansing on the Surface Roughness and Hardness of Two Denture Base Materials.Open Access Maced J Med Sci.2016;4(3):476-481.[37] Shah VR,Shah DN,Chauhan CJ,et al.Evaluation of flexural strength and color stability of different denture base materials including flexible material after using different denture cleansers.J Indian Prosthodont Soc.2015;15(4):367.[38] Nagakura M,Tanimoto Y,Nishiyama N.Effect of fiber content on flexural properties of glass fiber-reinforced polyamide-6 prepared by injection molding.Dent Mater J. 2017;36(4): 415-421.[39] Tanimoto Y.Dental materials used for metal-free restorations: Recent advances and future challenges.J Prosthodont Res. 2015;59(4):213.[40] Fueki K.Non-metal clasp dentures: More evidence is needed for optimal clinical application. J Prosthodont Res. 2016;60(4): 227. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||