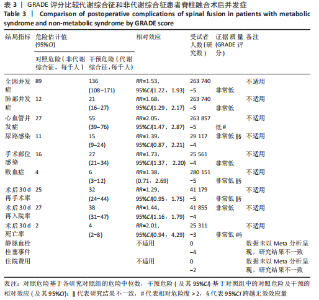
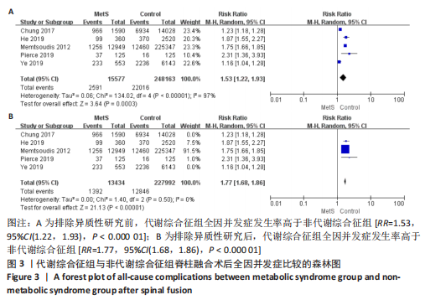
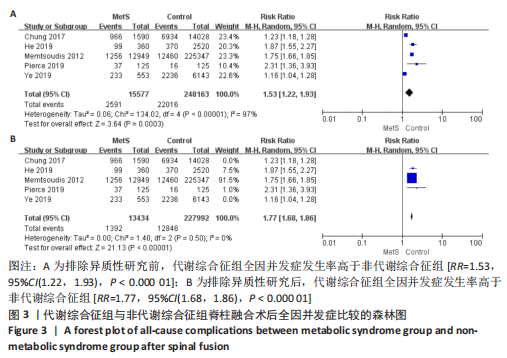
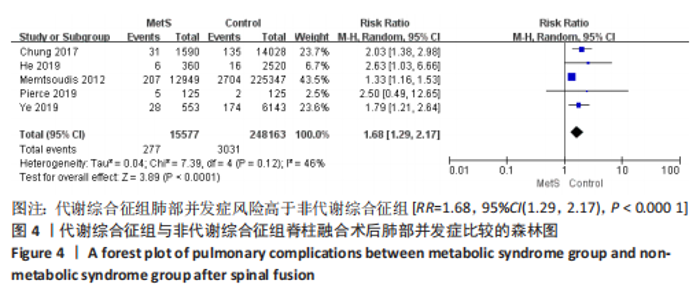
Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (22): 3602-3608.doi: 10.12307/2023.373
Complications after spinal fusion in patients with metabolic syndrome: a systematic review and meta-analysis
Ma Maoxiao1, 2, Cui Guofeng3, Zhang Xue2, Zhang Hong2, Liu Youwen2, Yue Chen2
- 1Hunan University of Chinese Medicine, Changsha 410000, Hunan Province, China; 2Luoyang Orthopedic Hospital of Henan Province (Orthopedic Hospital of Henan Province), Luoyang 471000, Henan Province, China; 3Luoyang Central Hospital Affiliated to Zhengzhou University, Luoyang 471000, Henan Province, China
-
Received:2022-04-26Accepted:2022-06-25Online:2023-08-08Published:2022-11-03 -
Contact:Liu Youwen, Professor, Chief physician, Doctoral supervisor, Luoyang Orthopedic Hospital of Henan Province (Orthopedic Hospital of Henan Province), Luoyang 471000, Henan Province, China Yue Chen, MD, Associate chief physician, Luoyang Orthopedic Hospital of Henan Province (Orthopedic Hospital of Henan Province), Luoyang 471000, Henan Province, China -
About author:Ma Maoxiao, Master candidate, Hunan University of Chinese Medicine, Changsha 410000, Hunan Province, China; Luoyang Orthopedic Hospital of Henan Province (Orthopedic Hospital of Henan Province), Luoyang 471000, Henan Province, China -
Supported by:the National Natural Science Foundation of China, No. 82074472 (to LYW); Science and Technology Project of Henan Province, No. 222102310368 (to CGF); Medical and Health Key Project of Luoyang Municipal Science and Technology Bureau, No. 2101027A (to CGF)
CLC Number:
Cite this article
Ma Maoxiao, Cui Guofeng, Zhang Xue, Zhang Hong, Liu Youwen, Yue Chen. Complications after spinal fusion in patients with metabolic syndrome: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(22): 3602-3608.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
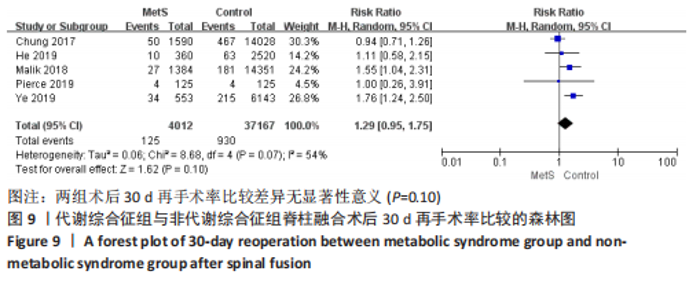
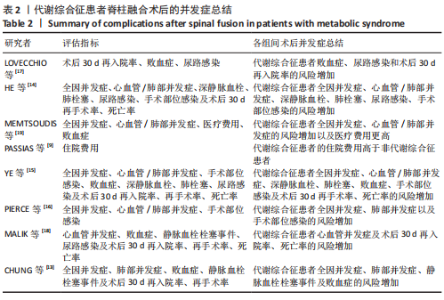
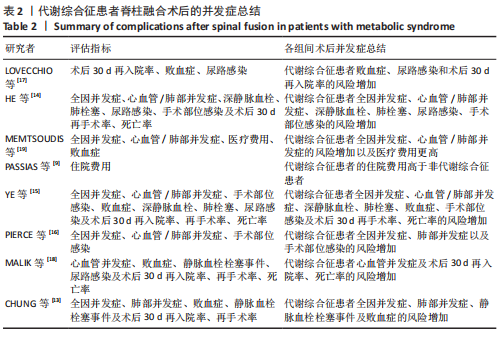
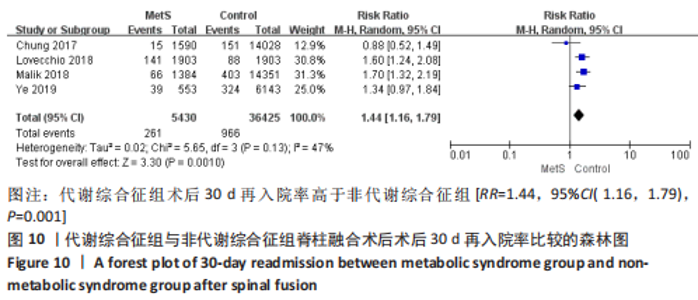
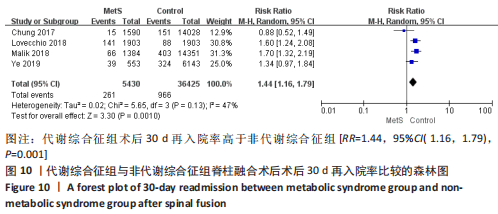
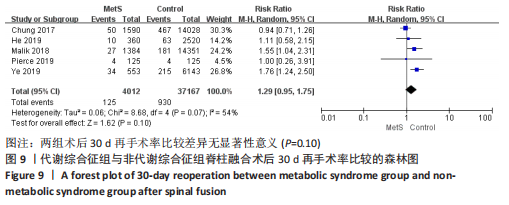
2.3.7 静脉血栓栓塞事件 数据来自4项文献研究[13-15,18],涉及40 929例患者。由于血栓类型、评估方法和时间点的显著异质性,不能进行Meta分析。CHUNG等[13]研究显示,与非代谢综合征患者相比,代谢综合征患者术后静脉血栓栓塞事件发病风险轻微增加。MALIK等[18]研究显示,代谢综合征患者和非代谢综合征患者的静脉血栓栓塞事件发病风险无明显差异。HE等[14]研究表明,与非代谢综合征组相比,代谢综合征组患者发生深静脉血栓形成比发生肺栓塞的风险更高。与之相反,YE等[15]研究发现,代谢综合征患者发生肺栓塞的风险比发生深静脉血栓的风险更高。 2.3.8 术后30 d再手术率 数据来自5项研究[13,15,17-18],涉及41 179例患者,结果显示,两组术后30 d再手术率比较差异无显著性意义[RR=1.29,95%CI(0.95,1.75),P=0.10],异质性中(I2=54%),见图9。证据质量(GRADE评分)非常低。"
| [1] ROJAS M, CHÁVEZ-CASTILLO M, PIRELA D, et al. Metabolic Syndrome: Is It Time to Add the Central Nervous System? Nutrients. 2021;13(7):2254. [2] ECKEL RH, GRUNDY SM, ZIMMET PZ. The metabolic syndrome. Lancet. 2005;365 (9468):1415-1428. [3] WILSON PW, D’AGOSTINO RB, PARISE H, et al. Metabolic syndrome as a precursor of cardiovascular disease and type 2 diabetes mellitus. Circulation. 2005;112(20):3066-3072. [4] WEN Q, ZHAO Z, WEN J, et al. Impact of obesity on operative complications and outcome after sacrocolpopexy: A systematic review and meta-analysis. Eur J Obstet Gynecol Reprod Biol. 2021;258:309-316. [5] LJUNGQVIST O. Insulin resistance and outcomes in surgery. J Clin Endocrinol Metab. 2010;95(9):4217-4219. [6] CROWTHER M, VAN DER SPUY K, ROODT F, et al. The relationship between pre-operative hypertension and intra-operative haemodynamic changes known to be associated with postoperative morbidity. Anaesthesia. 2018;73(7):812-818. [7] FEINKOHL I, WINTERER G, PISCHON T. Associations of dyslipidaemia and lipid-lowering treatment with risk of postoperative cognitive dysfunction: a systematic review and meta-analysis. J Epidemiol Community Health. 2018;72(6): 499-506. [8] BHAYANI NH, HYDER O, FREDERICK W, et al. Effect of metabolic syndrome on perioperative outcomes after liver surgery: A National Surgical Quality Improvement Program (NSQIP) analysis. Surgery. 2012; 152(2):218-226. [9] PASSIAS PG, BROWN AE, LEBOVIC J, et al. Metabolic Syndrome has a Negative Impact on Cost Utility Following Spine Surgery. World Neurosurg. 2020;135:e500-e504. [10] GUOFENG C, CHEN Y, RONG W, et al. Patients with metabolic syndrome have a greater rate of complications after arthroplasty: A systematic review and meta-analysis. Bone Joint Res. 2020;9(3):120-129. [11] GLANCE LG, WISSLER R, MUKAMEL DB, et al. Perioperative outcomes among patients with the modified metabolic syndrome who are undergoing noncardiac surgery. Anesthesiology. 2010;113(4):859-872. [12] JOHNSTON SS, FORTIN SP, PRACYK JB, et al. Economic and clinical outcomes of spinal fusion surgeries with skin closure through skin staples plus waterproof wound dressings versus 2-octyl cyanoacrylate plus polymer mesh tape. Spine J. 2021;21(1): 45-54. [13] CHUNG AS, CAMPBELL D, WALDROP R, et al. Metabolic Syndrome and 30-Day Outcomes in Elective Lumbar Spinal Fusion. Spine (Phila Pa 1976). 2018;43(9):661-666. [14] HE X, FEI Q, SUN T. Metabolic syndrome increases risk for perioperative outcomes following posterior lumbar interbody fusion. Medicine (Baltimore). 2020;99(38): e21786. [15] YE IB, TANG R, SCHWARTZ JT, et al. Postoperative Complications Associated With Metabolic Syndrome Following Adult Spinal Deformity Surgery. Clin Spine Surg. 2020;33(2):E87-E91. [16] PIERCE KE, KAPADIA BH, BORTZ C, et al. Operative fusion of patients with metabolic syndrome increases risk for perioperative complications. J Clin Neurosci. 2020;72: 142-145. [17] LOVECCHIO F, FU MC, IYER S, et al. Does Obesity Explain the Effect of the Metabolic Syndrome on Complications Following Elective Lumbar Fusion? A Propensity Score Matched Analysis. Global Spine J. 2018; 8(7):683-689. [18] MALIK AT, JAIN N, KIM J, et al. The Impact of Metabolic Syndrome on 30-Day Outcomes Following Elective Anterior Cervical Discectomy and Fusions. Spine (Phila Pa 1976).2019;44(5):E282-E287. [19] MEMTSOUDIS SG, KIRKSEY M, MA Y, et al. Metabolic syndrome and lumbar spine fusion surgery: epidemiology and perioperative outcomes. Spine (Phila Pa 1976). 2012;37(11):989-995. [20] SELPH JP, WHITED WM, SMITH AB, et al. Metabolic syndrome as a predictor for postoperative complications after urologic surgery. Urology. 2014;83(5):1051-1059. [21] GONZALEZ DELLA VALLE A, CHIU Y L, MA Y, et al. The metabolic syndrome in patients undergoing knee and hip arthroplasty: trends and in-hospital outcomes in the United States. J Arthroplasty. 2012;27(10): 1743-1749.e1. [22] TILG H, MOSCHEN AR. Adipocytokines: mediators linking adipose tissue, inflammation and immunity. Nat Rev Immunol. 2006;6(10):772-783. [23] FALAGAS ME, KOMPOTI M. Obesity and infection. Lancet Infect Dis. 2006;6(7): 438-446. [24] MCCRACKEN E, MONAGHAN M, SREENIVASAN S. Pathophysiology of the metabolic syndrome. Clin Dermatol. 2018; 36(1):14-20. [25] STORTZ JA, COX MC, HAWKINS RB, et al. Phenotypic heterogeneity by site of infection in surgical sepsis: a prospective longitudinal study. Crit Care. 2020;24(1): 203. [26] DEVARAJ S, VALLEGGI S, SIEGEL D, et al. Role of C-reactive protein in contributing to increased cardiovascular risk in metabolic syndrome. Curr Atheroscler Rep. 2010; 12(2):110-118. [27] EDELSTEIN AI, SULEIMAN LI, ALVAREZ AP, et al. The Interaction of Obesity and Metabolic Syndrome in Determining Risk of Complication Following Total Joint Arthroplasty. J Arthroplasty. 2016;31(9 Suppl): 192-196. [28] ZMISTOWSKI B, DIZDAREVIC I, JACOVIDES CL, et al. Patients with uncontrolled components of metabolic syndrome have increased risk of complications following total joint arthroplasty . J Arthroplasty. 2013;28(6):904-907. [29] ANDERSEN CJ, MURPHY KE, FERNANDEZ ML. Impact of Obesity and Metabolic Syndrome on Immunity. Adv Nutr. 2016; 7(1):66-75. [30] SCULLY IL, MCNEIL LK, PATHIRANA S, et al. Neutrophil killing of Staphylococcus aureus in diabetes, obesity and metabolic syndrome: a prospective cellular surveillance study. Diabetol Metab Syndr. 2017;9:76. [31] HEDSTROM M, LJUNGQVIST O, CEDERHOLM T. Metabolism and catabolism in hip fracture patients: nutritional and anabolic intervention--a review. Acta Orthop. 2006;77(5):741-747. [32] GONZALEZ-CHÁVEZ A, CHÁVEZ-FERNÁNDEZ JA, ELIZONDO-ARGUETA S, et al. Metabolic Syndrome and Cardiovascular Disease: A Health Challenge. Arch Med Res. 2018; 49(8):516-521. [33] KHAING P, PANDIT P, AWSARE B, et al. Pulmonary Circulation in Obesity, Diabetes, and Metabolic Syndrome. Compr Physiol. 2019;10(1):297-316. [34] CHAPLIN A, CARPÉNÉ C, MERCADER J. Resveratrol, Metabolic Syndrome, and Gut Microbiota. Nutrients. 2018;10(11):1651. [35] DI NISIO M, VAN ES N, BÜLLER HR. Deep vein thrombosis and pulmonary embolism. Lancet. 2016;388(10063):3060-3073. [36] SONG K, RONG Z, YAO Y, et al. Metabolic Syndrome and Deep Vein Thrombosis After Total Knee and Hip Arthroplasty. J Arthroplasty. 2016;31(6):1322-1325. [37] AY C, TENGLER T, VORMITTAG R, et al. Venous thromboembolism--a manifestation of the metabolic syndrome. Haematologica. 2007;92(3):374-380. [38] DY CJ, WILKINSON JD, TAMARIZ L, et al. Influence of preoperative cardiovascular risk factor clusters on complications of total joint arthroplasty. Am J Orthop (Belle Mead NJ). 2011;40(11):560-565. |
| [1] | Jiang Xiaocheng, Shi Lu, Wang Yinbin, Li Qiujiang, Xi Chuangzhen, Ma Zefeng, Cai Lijun. Systematical evaluation of bone fusion rate after interbody fusion in patients with osteoporosis and lumbar degenerative disease treated with teriparatide [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1427-1433. |
| [2] | You Zhengqiu, Zhang Zhongzu, Wang Qunbo. Early symptomatic intervertebral disc pseudocysts after discectomy detected on MRI [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1403-1409. |
| [3] | Wang Yanjin, Zhou Yingjie, Chai Xubin, Zhuo Hanjie. Meta-analysis of the efficacy and safety of 3D printed porous titanium alloy fusion cage in anterior cervical discectomy and fusion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1434-1440. |
| [4] | Li Wenjie, You Aijia, Zhou Junli, Fang Sujuan, Li Chun. Effects of different dressings in the treatment of burn wounds: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1141-1148. |
| [5] | Chen Guanting, Zhang Linqi, Li Qingru. Meta-analysis of the value of exosomal miRNA for the diagnosis of chronic kidney disease [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 970-976. |
| [6] | Yan Le, Zhang Huiping, Dai Lintong. Mesenchymal stem cells for allergic rhinitis: a meta-analysis based on animal experiments [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 977-984. |
| [7] | Shen Lianwei, Zhu Hongliu, Wang Wei. Risk factor analysis of metabolic syndrome and construction of a nomogram prediction model in middle-aged and elderly people [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 657-662. |
| [8] | Feng Liang, Gong Shuhui, Huo Hongfeng. Effect of short-foot training on foot and ankle function in patients with flat feet: Meta-analysis and systematic review [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 799-804. |
| [9] | Pan Weimin, Wang Bing, Han Yabing, Li Ting, Song Jiaqi, Qin Huasheng, Liu Yang. Effects of blood flow restriction training on muscle strength, muscle mass and physical performance in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 805-812. |
| [10] | Yu Jiaan, Liu Xinwei, Lian Hongyu, Liu Kexin, Li Zitao. Medial open-wedge tibial osteotomy versus lateral closed-wedge tibial osteotomy for unicompartmental knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 632-639. |
| [11] | Xu Yangyang, He Peiliang, Meng Qingqi, Li Siming. A meta-analysis of the effects of continuous adductor canal block and continuous femoral nerve block on early activity after knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 640-645. |
| [12] | Chai Hao, Yang Deyong, Zhang Lei, Shu Li. 3D printing personalized osteotomy guide technology versus conventional total knee arthroplasty on the accuracy of lower limb force alignment: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 646-654. |
| [13] | You Aijia, Li Wenjie, Zhou Junli, Li Chun. Systematic evaluation of six dressings on wound safety following total hip and knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 486-492. |
| [14] | Weng Youlin, Cai Yu, Li Zutao, Guo Bin, Xu Jiangbo. Construction and validation of a model for predicting postoperative severe complications of intertrochanteric fracture in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2915-2920. |
| [15] | Wu Yihan, Wei Qiaoye, Pang Yu, Liu Zhongqiang. Proprioception characteristics of functional ankle instability: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2943-2952. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||