Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (22): 3469-3475.doi: 10.12307/2023.367
Previous Articles Next Articles
Biomechanical response of ankle traction arthroplasty for ankle osteoarthritis through finite element modeling
Xia Yubo, Tang Xiaoxia, Luo Wen, Xu Yongsheng, Yuan Changfei, Wang Zhe, Zhou Xiaohan, Tian Miao, Wang Tao, Guo Ying
- Kunming Municipal Hospital of Traditional Chinese Medicine, Kunming 650500, Yunnan Province, China
-
Received:2022-01-06Accepted:2022-06-13Online:2023-08-08Published:2022-11-02 -
Contact:Wang Tao, Master, Attending physician, Kunming Municipal Hospital of Traditional Chinese Medicine, Kunming 650500, Yunnan Province, China Guo Ying, Chief physician, Kunming Municipal Hospital of Traditional Chinese Medicine, Kunming 650500, Yunnan Province, China -
About author:Xia Yubo, Master, Physician, Kunming Municipal Hospital of Traditional Chinese Medicine, Kunming 650500, Yunnan Province, China -
Supported by:the Science and Technology Planning Project of Yunnan Provincial Department of Science and Technology, No. 202001AZ070001-070 (to XYB)
CLC Number:
Cite this article
Xia Yubo, Tang Xiaoxia, Luo Wen, Xu Yongsheng, Yuan Changfei, Wang Zhe, Zhou Xiaohan, Tian Miao, Wang Tao, Guo Ying. Biomechanical response of ankle traction arthroplasty for ankle osteoarthritis through finite element modeling[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(22): 3469-3475.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
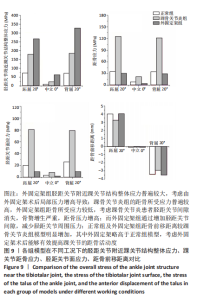
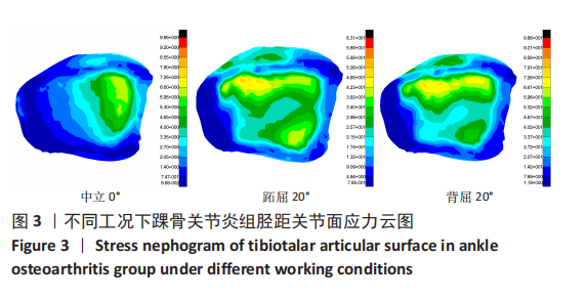
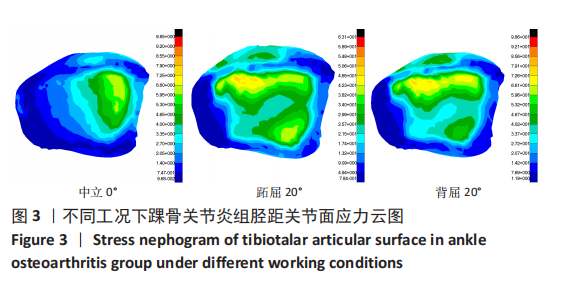
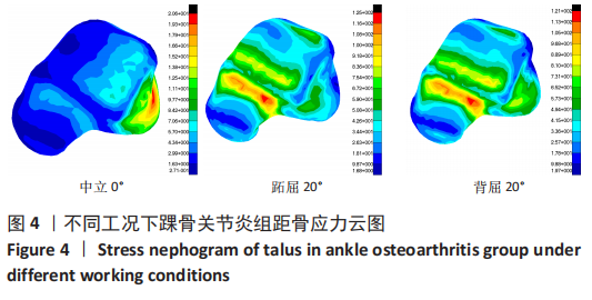
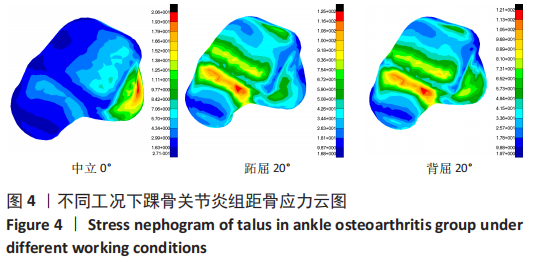
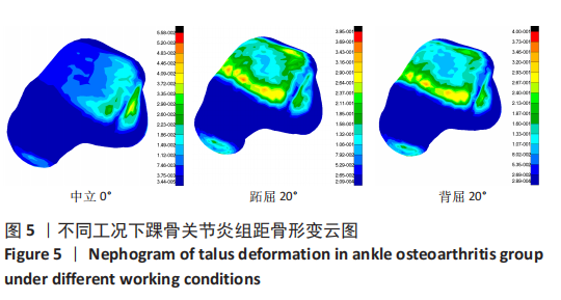
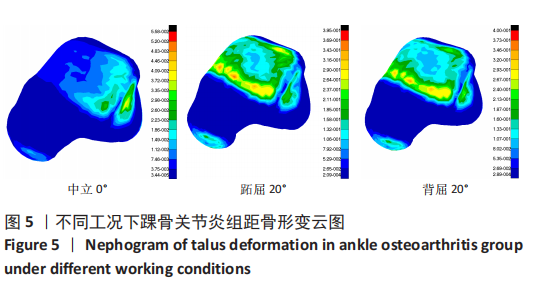
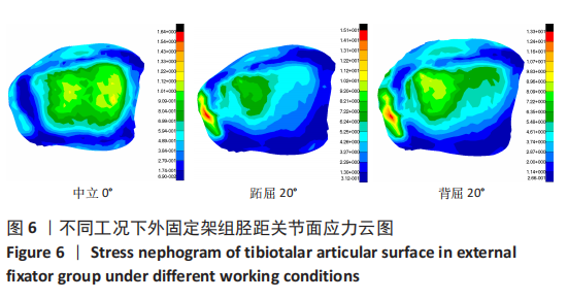
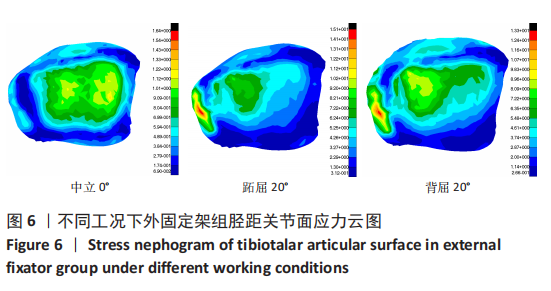
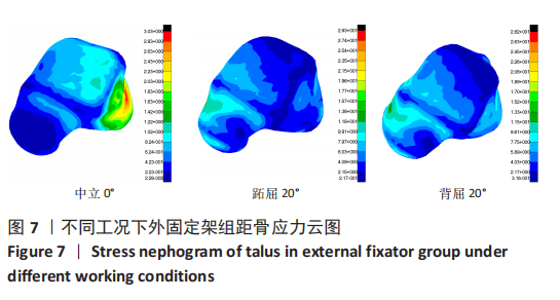
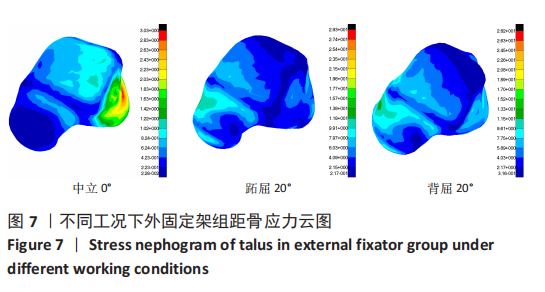
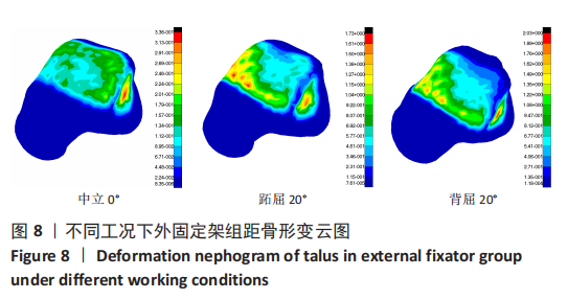
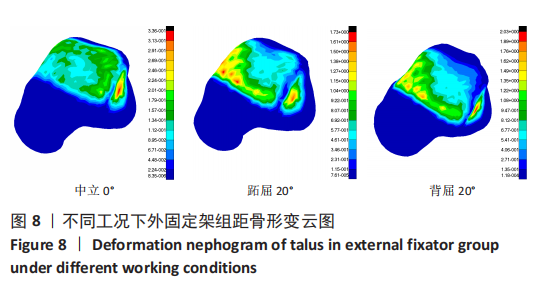
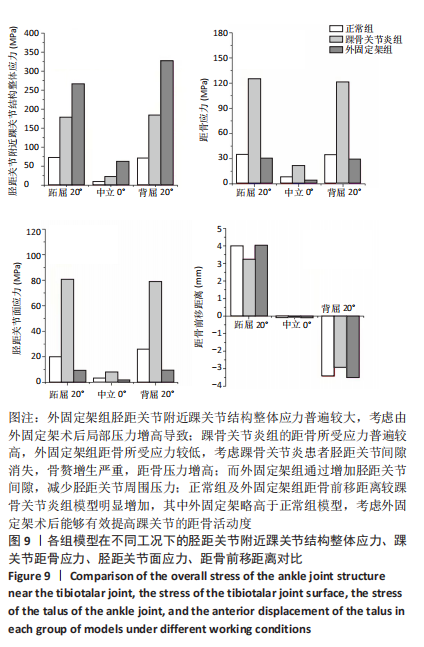
2.3 数据分析 综合上述计算结果,将踝关节对应的关节炎组、外固定架组在跖屈20°、中立0°、背屈20° 3种不同工况下进行三维有限元仿真计算数据汇总于图9中,并通过相对正常组的数据换算Von Mises应力增量、Von Mises应变增量、Displacement变形增量等,可见: (1)中立位0°时,踝骨关节炎组胫距关节附近的踝关节结构应力峰值为20.6 MPa,距骨应力峰值20.6 MPa,胫距关节面应力峰值7.25 MPa,距骨前移距离-0.05 mm;外固定架组胫距关节附近的踝关节结构应力峰值为61.3 MPa,距骨应力峰值3.03 MPa,胫距关节面应力峰值1.22 MPa,距骨前移距离-0.06 mm。 (2)跖屈20°时,踝骨关节炎组胫距关节附近的踝关节结构应力为177 MPa,距骨应力峰值125 MPa,胫距关节面应力峰值80.7 MPa,距骨前移距离3.25 mm;外固定架组胫距关节附近的踝关节结构应力峰值为265 MPa,距骨应力峰值29.3 MPa,胫距关节面应力峰值9.2 MPa,距骨前移距离4.03 mm。 (3)背屈20°时,踝骨关节炎组胫距关节附近的踝关节结构应力为183 MPa,距骨应力峰值121 MPa,胫距关节面应力峰值79.1 MPa,距骨前移距离-2.93 mm;外固定架组胫距关节附近的踝关节结构应力峰值为326 MPa,距骨应力峰值28.2 MPa,胫距关节面应力峰值8.96 MPa,距骨前移距离-3.51 mm。"
| [1] GLAZEBROOK M, DANIELS T, YOUNGER A, et al. Comparison of healthrelated quality of life between patients with end stage ankle and hip arthrosis. J Bone Joint Surg Am. 2008;90(3):499-505. [2] DELCO ML, KENNEDY JG, BONASSAR LJ, et al. Post-Traumatic Osteoarthritis of the Ankle: A Distinct Clinical Entity Requiring New Research Approaches. J Orthop Res. 2017;35(3):440-453. [3] GOLDRING MB, GOLDRING SR. Osteoarthritis. J Cell Physiol. 2007; 213(3):626-634. [4] ROOS EM. Joint injury causes knee osteoarthritis in young adults. Curr Opin Rheumatol. 2005;17(2):195-200. [5] VAN VALBURG AA, VAN ROERMUND PM, LAMMENS J, et al. Can Ilizarov joint distraction delay the need for an arthrodesis of the ankle? A preliminary report. J Bone Joint Surg Br. 1995;77(5):720-725. [6] JUDET R, JUDET T. The use of a hinge distraction apparatus after arthrolysis and arthroplasty (author’s transl). Rev Chir Orthop. 1978; 64(5):353-365. [7] VAN VALBURG AA, VAN ROERMUND PM, MARIJNISSEN AC, et al. Joint distraction in treatment of osteoarthritis: a two year followup of the ankle. Osteoarthritis Cartilage. 1998;7(5):474-479. [8] SMITH NC, BEAMAN D, ROZBRUCH SR, et al. Evidence-based indications for distraction ankle arthroplasty. Foot Ankle Int. 2012;33(8):632-636. [9] LABOVITZ JM. The role of arthrodiastasis in salvaging arthritic ankles. Foot Ankle Spec. 2010;3(4):201-204. [10] JACOB S, PATIL MK. Three-dimensional foot modeling and analysis of stresses in normal and early stage Hansen’s disease with muscle paralysis. J Rehabil Res Dev. 1999;36(3):252-263. [11] 卢昌怀. 距骨数值仿真模型的建立及有限元分析[D]. 广州: 南方医科大学,2011. [12] GEFEN A, MEGIDO-RAVID M, ITZCHAK Y, et al. Biomechanical analysis of the three - dimensional foot structure during gait: A basic tool for clinical applications. J Biomech Eng. 2000;122(6):630-639. [13] CHEUNG JT, ZHANG M, LEUNG AK, et al. Three-dimensional finite element analysis of the foot during standing-a material sensitivity study. J Biomech. 2005;38(5):1045-1054. [14] 金乾坤. 人体足踝部三维有限元仿真模型的构建及验证[D]. 大连:大连医科大学,2015. [15] 刘清华, 余斌, 金丹. 解剖结构完整的踝关节有限元模型构建及意义[J].山东医药,2010,50(14):1-3. [16] PFAEFFLE HJ, TOMAINO MM, GREWAL R, et al. Tensile Properties of the interosseous membrane of the human forearm. J Orthop Res. 1996; 14:842-845. [17] BEUMER A, VAN HEMERT WL, SWIERSTRA BA, et al. A biomechanical evaluation of the tibiofibular and tibiotalar ligaments of the ankle. Foot Ankle Int. 2003;24:426-429. [18] HOEFNAGELS EM, WAITES MD, WINGS MD, et al. Biomechanical comparison of the interosseous tibiofibular ligament and the anterior tibiofibular ligament. Foot Ankle Int. 2007;28:602-604. [19] SIEGLER S, BLOCK J, SCHNECK CD. The mechanical characteristics of the collateral ligaments of the human ankle joint. Foot Ankle. 1988;8: 234-242. [20] 张明彦. 踝关节三维有限元模型的建立及三角韧带损伤和重建的踝关节生物力学有限元分析[D]. 长沙:中南大学,2012. [21] LO CC, TSAI KJ, ZHONG ZC, et al. Biomechanical differences of Coflex-F and pedicle screw fixation combined with TLIF or ALIF-a finite element study. Comput Methods Biomech Biomed Engin. 2011;14(11):947-956. [22] RODRIGUEZ-MERCHAN EC. Joint distraction in advanced osteoarthritis of the ankle. Arch Bone Jt Surg. 2017;5(4):208-212. [23] 周源,徐海林.关节牵引术治疗创伤后踝关节炎[J].中国骨与关节外科,2013,6(4):112-114. [24] ZHAO H, QU W, LI Y, et al. Functional analysis of distraction arthroplasty in the trea-tment of ankle osteoarthritis. J Orthop Surg Res. 2017; 12(1):18. [25] MARIJNISSEN AC, HOEKSTRA MC, PRÉ BC, et al. Patient charac. teristics as predictors of clinical outcome of distraction in treatment of severe ankle osteoarthritis. J Orthop Res. 2013;32(1):96-101. [26] NGUYEN MP, PEDERSEN DR, GAO Y, et al. Intermediate—term follow·up after ankle distraction for treatment of end.stage osteoarthritis. J Bone Joint Surg Am. 2015;97(7):590-596. [27] LEE HS, WAPNER KL, PARK SS, et al. Ligament reconstruction and calcaneal osteotomy for osteoarthritis of the ankle. Foot Ankle Int. 2009;30(6):475-480. [28] YOUN H, KIM YS, LEE J, et al. .Percutaneous lateral ligament reconstruction with allograft for chronic lateral ankle instability. Foot Ankle Int. 2012;33(2):99-104. [29] RAMLEE MH, KADIR MRA, HARUN H. Three-Dimensional Modelling and Finite Element Analysis of an Ankle External Fixator. Adv Mater Res. 2014;845:183-188. [30] ANDERSON DD, GOLDSWORTHY JK, LI W, et al. Physieal validation of a Patient-specific contact finite element model of the ankle. J Biomeeh Eng. 2007;1662-1669. [31] 魏俊杰. 踝关节及周围韧带三维有限元模型的建立与分析[D]. 大连:大连医科大学,2011. [32] BARG A, SALTZMAN CL, BEALS TC, et al. Arthroscopic Talar Dome Access Using a Standard Versus Wire-Based Traction Method for Ankle Joint Distraction. Arthroscopy. 2016;(32):1367-1374. [33] IAMMARINO K, MARRIE J, SELHORST M, et al. Efficacy of the stretch band ankle traction technique in the treatment of pediatric patients with acute ankle sprains: a randomized control trial. Int J Sports Phys Ther. 2018;(13):1-11. [34] LEE RKL, GRIFFITH JF, LAW EKC, et al. Ankle Traction During MRI of Talar Dome Osteochondral Lesions. AJR Am J Roentgenol. 2017;(209):874-882. [35] NAKASA T, IKUTA Y, SAWA M, et al. Evaluation of Articular Cartilage Injury Using Computed Tomography With Axial Traction in the Ankle Joint. Foot Ankle Int. 2018;(39):1120-1127. [36] POWDEN CJ, HOGAN KK, WIKSTROM EA, et al. The Effect of 2 Forms of Talocrural Joint Traction on Dorsiflexion Range of Motion and Postural Control in Those With Chronic Ankle Instability. J Sport Rehabil. 2017; (26):239-244. [37] VEGA J, DALMAU-PASTOR M. Ankle Arthroscopy: No-Distraction and Dorsiflexion Technique Is the Key for Ankle Arthroscopy Evolution, Arthroscopy. 2018;(34):1380-1382. [38] 骆健.不同材料赋值方法下踝关节三维有限元模型的应力及位移变化[D].昆明:昆明理工大学,2018. [39] WHITEHOUSE M, THOMPSON S, HALLIWELL P, et al. The use of a femoral distractor to aid distal tibial resection during total ankle arthroplasty. J Foot Ankle Surg. 2010;49(2):205-207. [40] 王远瑞,孙强,陈永锋,等. 踝关节牵开成形联合富血小板血浆注射治疗创伤性踝关节炎的临床效果[J].临床医学研究与实践,2020, 5(29): 55-57. [41] 康忠仁. 玻璃酸钠与臭氧注射辅助踝关节牵开成形术对踝关节创伤性关节炎疗效及骨代谢的影响[J]. 包头医学院学报,2021,37(5): 57-61. [42] 顾文奇,徐宏威,王晓康,等. 踝关节牵开成形联合富血小板血浆注射治疗创伤性踝关节炎[J]. 中华创伤骨科杂志,2019,21(4):321-327. [43] 梁景棋,梁晓军,张言,等.牵开成形术治疗踝关节骨性关节炎[J]. 中国矫形外科杂志,2018,26(19):1746-1751. [44] 张成,徐林. 终末期踝关节炎治疗研究进展[J]. 足踝外科电子杂志, 2018,5(4):56-59. |
| [1] | Zhong Yizheng, Huang Peizhen, Cai Qunbin, Zheng Liqin, He Xingpeng, Dong Hang. Microstructural indexes that determine the trabecular bone maximum stress of micro-finite element models [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1313-1318. |
| [2] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [3] | Wu Taoguang, Nie Shaobo, Chen Hua, Zhu Zhengguo, Qi Lin, Tang Peifu. Biomechanical characteristics of a new multi-dimensional cross locking plate in the treatment of subtrochanteric nonunion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1330-1334. |
| [4] | Peng Zhixin, Yan Wengang, Wang Kun, Zhang Zhenjiang. Finite element analysis and structural optimization design of 3D printed forearm braces [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1340-1345. |
| [5] | Wu Tianliang, Tao Xiuxia, Xu Hongguang. Influence of different bone mineral densities on cage subsidence after stand-alone oblique lateral interbody fusion: three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1352-1358. |
| [6] | Liu Jinyu, Zhang Hanshuo, Cui Hongpeng, Pan Lingzhi, Zhao Boran, Li Fei, Ding Yu. Finite element biomechanical analysis of minimally invasive treatment of cervical spondylotic myelopathy and accurate exercise rehabilitation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1359-1364. |
| [7] | He Yujie, Kang Zhijie, Xue Mingming, Jin Feng, Li Zhijun, Wang Xing, Xu Yangyang, Gao Mingjie, Li Jiawei, Li Xiaohe, Wang Haiyan. Finite element analysis of transarticular screw fixation of adolescent thoracic vertebra [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1365-1370. |
| [8] | Wen Xinghua, Ding Huanwen, Cheng Kai, Yan Xiaonan, Peng Yuanhao, Wang Yuning, Liu Kang, Zhang Huiwu. Three-dimensional finite element model analysis of intramedullary nailing fixation design for large femoral defects in Beagle dogs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1371-1376. |
| [9] | Du Xueting, Zhang Xiaodong, Chen Yanjun, Wang Mei, Chen Wubiao, Huang Wenhua. Application of compressed sensing technology in two-dimensional magnetic resonance imaging of the ankle joint [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1396-1402. |
| [10] | Huang Linke, Wei Linhua, Jiang Jie, Liu Qian, Chen Weiwei. Effects of estrogen combined with treadmill exercise on bone mass and articular cartilage in ovariectomized mice [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1166-1171. |
| [11] | Liu Jiaxin, Jia Peng, Men Yutao, Liu Lu, Wang Yeming, Ye Jinduo. Design and optimization of bone trabecular structure with triply periodic minimal surfaces [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 992-997. |
| [12] | Guo Tingting, Xie Hong, Xu Guanghua. Finite element analysis of elastic ankle brace performance [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1031-1037. |
| [13] | Zhu Lin, Gu Weiping, Wang Can, Chen Gang. Biomechanical analysis of All-on-Four and pterygomaxillary implants under different maxillary bone conditions [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 985-991. |
| [14] | Sun Jiangwei, Wang Junxiang, Baibujiafu·Yellisi, Dai Huijuan, Nijati·Turson. Three-dimensional finite element analysis of stress distribution in different smooth collar implants [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1004-1011. |
| [15] | Jiang Yifang, Cai Qimin, Chu Zhengyi, Qin Min, Shen Yurong, Gu Yuanping. Simulation analysis of stress distribution of NRT FILES in curved root canals [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1038-1042. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||