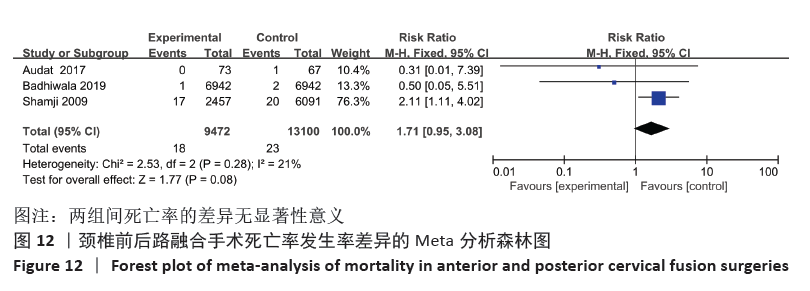
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (30): 4907-4914.doi: 10.12307/2021.281
Previous Articles Next Articles
Meta-analysis of adverse events between anterior and posterior fusion surgery for multiple-level cervical spondylosis
Wang Shuguang1, Cai Tongchuan1, Feng Xinmin2, Nan Liping2, Wang Feng2, Zhu Lei2, Chen Dong2, Zhang Liang2
- 1Graduate School of Dalian Medical University, Dalian 116000, Liaoning Province, China; 2Department of Orthopedic (Spine Center), Clinical Medical College of Yangzhou University, Yangzhou 225001, Jiangsu Province, China
-
Received:2020-08-11Revised:2020-08-12Accepted:2021-02-07Online:2021-10-28Published:2021-07-29 -
Contact:Zhang Liang, MD, Associate chief physician, Department of Orthopedic (Spine Center), Clinical Medical College of Yangzhou University, Yangzhou 225001, Jiangsu Province, China -
About author:Wang Shuguang, Master candidate, Graduate School of Dalian Medical University, Dalian 116000, Liaoning Province, China -
Supported by:the National Natural Science Foundation of China, No. 81972136 (to ZL); Guangxi Natural Science Foundation General Project, No. 2018JJA14775 (to ZL); Young Medical Scholars Major Program of Jiangsu Province, No. QNRC2016342 (to ZL); Key Funding Project of Maternal and Child Health Research of Jiangsu Province, No. F201801 (to ZL); High-Level Health Professionals "Six Projects" Top-notch Talent Research Program of Jiangsu Province, No. LGY2019035 (to ZL)
CLC Number:
Cite this article
Wang Shuguang, Cai Tongchuan, Feng Xinmin, Nan Liping, Wang Feng, Zhu Lei, Chen Dong, Zhang Liang. Meta-analysis of adverse events between anterior and posterior fusion surgery for multiple-level cervical spondylosis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4907-4914.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
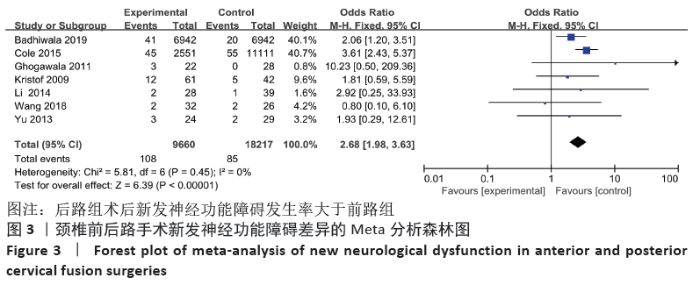
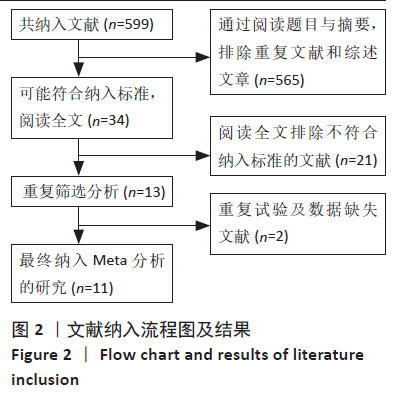
2.3 Meta分析结果 2.3.1 各组总体不良事件发生率差异 共11篇研究报道前后路手术的相关不良事件[12-22]。前路组共24 564例患者,后路组共12 298例患者;前路组发生不良事件2 623例(10.68%),后路组1 529例(12.43%)。各研究间存在统计学异质性(P=0.84,I2=99%),故采用随机效应模型进行分析。随后通过敏感性及亚组分析无法分析其异质性来源,故4位研究者商讨决定只对结果进行一般性描述,不合并效应量。 2.3.2 各组新发神经功能障碍发生率差异 新发神经功能障碍主要记录的数据包括术后C5神经麻痹、其他新发肢体及躯干感觉障碍等。共有7篇文献记录术后新发神经功能障碍[12-13,15-16,18,20-21]。各研究组间具有统计学同质性(P=0.45,I2=0%),采用固定效应模型进行分析。后路组术后新发神经功能障碍发生率大于前路组(OR=2.68,95%CI:1.98-3.63,P < 0.000 01),见图3。"
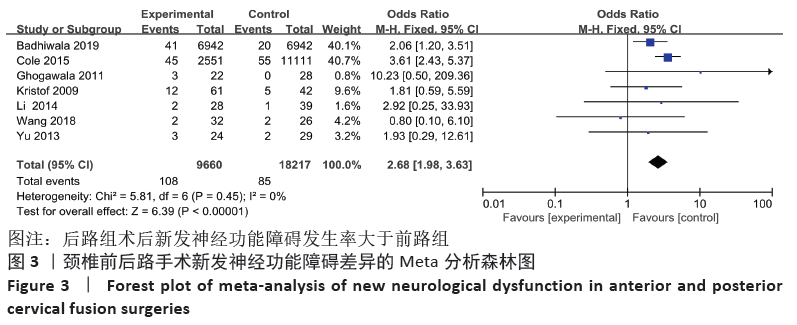

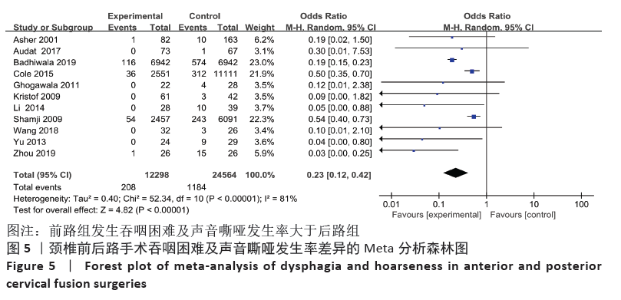
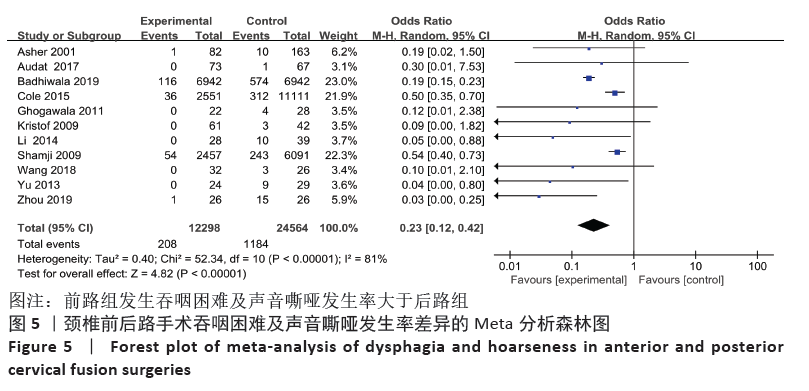
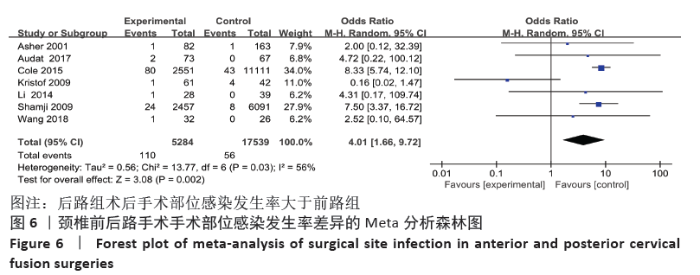
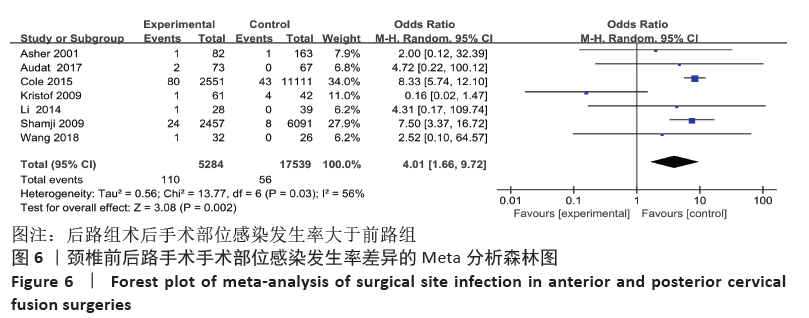
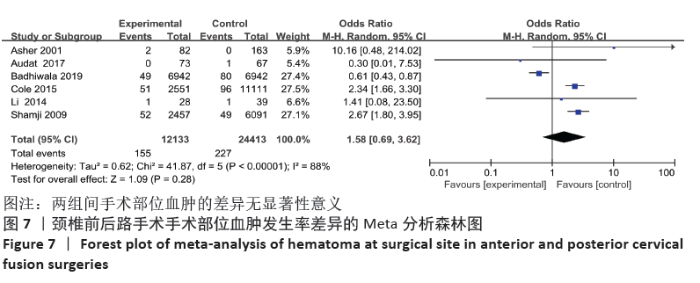
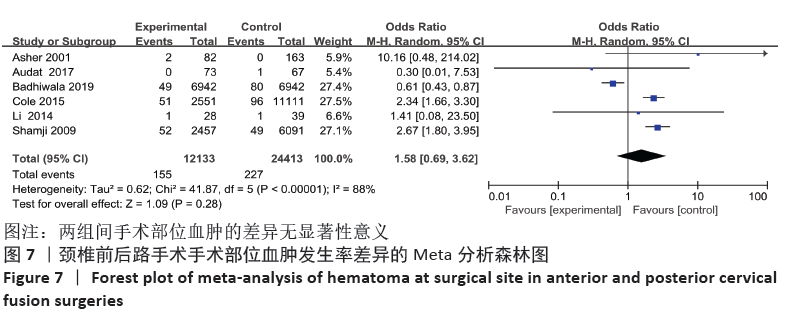
2.4 敏感性分析 采用敏感性分析中的去除单项研究法逐一排除纳入研究,再进行结果的合并。合并吞咽困难及声音嘶哑的数据时,排除BADHIWALA等[16]的研究后异质性明显下降,排除单项研究后,得出前路组术后发生吞咽困难及声音嘶哑发生率仍然大于后路组。合并手术部位感染的结果时,排除KRISTOF等[15]的研究后异质性下降,排除后评价各项指标与之前合并结果无明显差异。合并手术部位血肿的结果时,排除BADHIWALA等[16]的研究后异质性明显下降(P < 0.000 01)。对其他不良事件的研究逐一剔除文献进行对比,合并后效应值未发生明显变化,说明Meta分析结果相对稳定,由单个研究引起的偏倚较小,可靠性较高。 2.5 发表偏倚分析 文章中部分研究的漏斗图检验能力因文献数量不足而下降,从而无法判断不对称性的真实性。吞咽困难及声音嘶哑研究漏斗图提示存在不对称性且密集分布于底部左侧,表明本次系统评价存在发表偏倚,见图13。"

| [1] VERHAGEN AP, VAN MIDDELKOOP M, RUBINSTEIN SM, et al. Effect of various kinds of cervical spinal surgery on clinical outcomes: a systematic review and meta-analysis. Pain. 2013;154(11):2388-2396. [2] SMITH GW, ROBINSON RA. The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg Am. 1958;40-a(3):607-624. [3] VEERAVAGU A, COLE T, JIANG B, et al. Revision rates and complication incidence in single- and multilevel anterior cervical discectomy and fusion procedures: an administrative database study. Spine J. 2014;14(7):1125-1131. [4] CURRIER BL. Neurological complications of cervical spine surgery: C5 palsy and intraoperative monitoring. Spine. 2012; 37(5):E328-E334. [5] WOODS BI, HOHL J, LEE J, et al. Laminoplasty versus laminectomy and fusion for multilevel cervical spondylotic myelopathy. Clin Orthop Related Res. 2011; 469(3):688-695. [6] YOSHII T, EGAWA S, CHIKUDA H, et al. Comparison of anterior decompression with fusion and posterior decompression with fusion for cervical spondylotic myelopathy-A systematic review and meta-analysis. J Orthop Sci. 2020;25(6):938-945. [7] CHEN Z, LIU B, DONG J, et al. A comparison of the anterior approach and the posterior approach in treating multilevel cervical myelopathy: a meta-analysis. Clin Spine Surg. 2017;30(2):65-76. [8] LUO J, CAO K, HUANG S, et al. Comparison of anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy. Eur Spine J. 2015;24(8):1621-1630. [9] XU L, SUN H, LI Z, et al. Anterior cervical discectomy and fusion versus posterior laminoplasty for multilevel cervical myelopathy: a meta-analysis. Int J Surg. 2017;48:247-253. [10] 曾宪涛,包翠萍,曹世义,等.Meta分析系列之三:随机对照试验的质量评价工具[J].中国循证心血管医学杂志,2012, 4(3):183-185. [11] STANG A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010; 25(9):603-605. [12] COLE T, VEERAVAGU A, ZHANG M, et al. Anterior versus posterior approach for multilevel degenerative cervical disease: a retrospective propensity score-matched study of the marketscan database. Spine. 2015;40(13):1033-1038. [13] WANG B, Lü G, KUANG L. Anterior cervical discectomy and fusion with stand-alone anchored cages versus posterior laminectomy and fusion for four-level cervical spondylotic myelopathy: a retrospective study with 2-year follow-up. BMC Musculoskelet Disord. 2018;19(1):216. [14] ASHER AL, DEVIN CJ, KEREZOUDIS P, et al. Comparison of outcomes following anterior vs posterior fusion surgery for patients with degenerative cervical myelopathy: an analysis from quality outcomes database. Neurosurgery. 2019;84(4):919-926. [15] KRISTOF RA, KIEFER T, THUDIUM M, et al. Comparison of ventral corpectomy and plate-screw-instrumented fusion with dorsal laminectomy and rod-screw-instrumented fusion for treatment of at least two vertebral-level spondylotic cervical myelopathy. Eur Spine J. 2009;18(12): 1951-1956. [16] BADHIWALA JH, ELLENBOGEN Y, KHAN O, et al. Comparison of the inpatient complications and health care costs of anterior versus posterior cervical decompression and fusion in patients with multilevel degenerative cervical myelopathy: a retrospective propensity score-matched analysis. World Neurosurg. 2020;134:e112-e119. [17] SHAMJI MF, COOK C, PIETROBON R, et al. Impact of surgical approach on complications and resource utilization of cervical spine fusion: a nationwide perspective to the surgical treatment of diffuse cervical spondylosis. Spine J. 2009; 9(1):31-38. [18] GHOGAWALA Z, BROOK M, BENZEL E C, et al. Comparative effectiveness of ventral versus dorsal surgery for cervical spondylotic myelopathy. Eur Spine J. 2010; 19(6):1054. [19] ZHOU C, LIU C, PANCHAL RR, et al. Modified expansive laminoplasty and fusion compared with anterior cervical surgeries in treating four-level cervical spondylotic myelopathy. J Int Med Res. 2019;47(6):2413-2423. [20] SHUNZHI Y, ZHONGHAI L, FENGNING L, et al. Surgical management of 4-level cervical spondylotic myelopathy. Orthopedics. 2013; 36(5):e613-e620. [21] LI Z, GUO Z, HOU S, et al. Segmental anterior cervical corpectomy and fusion with preservation of middle vertebrae in the surgical management of 4-level cervical spondylotic myelopathy. Eur Spine J. 2014; 23(7):1472-1479. [22] AUDAT ZA, FAWAREH MD, RADYDEH AM, et al. Anterior versus posterior approach to treat cervical spondylotic myelopathy, clinical and radiological results with long period of follow-up. SAGE Open Med. 2018;6:2050312118766199. [23] WITWER BP, TROST GR. Cervical spondylosis: ventral or dorsal surgery. Neurosurgery. 2007;60(1 Supp1 1):S130-S136. [24] AL EISSA S, KONBAZ F, ALDEGHAITHER S, et al. Anterior cervical discectomy and fusion complications and thirty-day mortality and morbidity. Cureus. 2020;12(4):e7643. [25] CHEN Q, QIN M, CHEN F, et al. Comparison of outcomes between anterior cervical decompression and fusion and posterior laminoplasty in the treatment of 4-level cervical spondylotic myelopathy. World Neurosurg. 2019;125:e341-e347. [26] DEBONO B, CORNIOLA MV, PIETTON R, et al. Benefits of enhanced recovery after surgery for fusion in degenerative spine surgery: impact on outcome, length of stay, and patient satisfaction. Neurosurgical Focus. 2019;46(4):E6. [27] REN J, LI R, ZHU K, et al. Biomechanical comparison of percutaneous posterior endoscopic cervical discectomy and anterior cervical decompression and fusion on the treatment of cervical spondylotic radiculopathy. J Orthop Surg Res. 2019; 14(1):71. [28] SALZMANN SN, DERMAN PB, LAMPE LP, et al. Cervical spinal fusion: 16-year trends in epidemiology, indications, and in-hospital outcomes by surgical approach. World Neurosurg. 2018;113:e280-e295. [29] FEHLINGS MG, BARRY S, KOPJAR B, et al. Anterior versus posterior surgical approaches to treat cervical spondylotic myelopathy: outcomes of the prospective multicenter AOSpine North America CSM study in 264 patients. Spine. 2013; 38(26):2247-2252. [30] LIN D, ZHAI W, LIAN K, et al. Anterior versus posterior approach for four-level cervical spondylotic myelopathy. Orthopedics. 2013; 36(11):e1431-1436. [31] YOUSSEF JA, HEINER AD, MONTGOMERY JR, et al. Outcomes of posterior cervical fusion and decompression: a systematic review and meta-analysis. Spine J. 2019;19(10): 1714-1729. [32] PAN FM, WANG SJ, MA B, et al. C5 nerve root palsy after posterior cervical spine surgery. Journal of orthopaedic surgery (Hong Kong). 2017;25(1):2309499016684502. [33] ZHU N, XIE D, DENG QY, et al. Comment on Zhu et al. entitled ‘‘Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review and meta-analysis’’. Eur Spine J. 2014;23(2):486. [34] KOMOTAR RJ, MOCCO J, KAISER MG. Surgical management of cervical myelopathy: indications and techniques for laminectomy and fusion. Spine J. 2006;6(6 Suppl): 252s-267s. [35] NAKASHIMA H, YUKAWA Y, IMAGAMA S, et al. Complications of cervical pedicle screw fixation for nontraumatic lesions: a multicenter study of 84 patients. J Neurosurg Spine. 2012;16(3):238-247. [36] GU Y, CAO P, GAO R, et al. Incidence and risk factors of C5 palsy following posterior cervical decompression: a systematic review. PLoS One. 2014;9(8):e101933. [37] KATSUMI K, YAMAZAKI A, WATANABE K, et al. Can prophylactic bilateral C4/C5 foraminotomy prevent postoperative C5 palsy after open-door laminoplasty?: a prospective study. Spine. 2012;37(9): 748-754. [38] WADA E, SUZUKI S, KANAZAWA A, et al. Subtotal corpectomy versus laminoplasty for multilevel cervical spondylotic myelopathy: a long-term follow-up study over 10 years. Spine. 2001;26(13):1443-1447;discussion 8. [39] WANG SJ, JIANG SD, JIANG LS, et al. Axial pain after posterior cervical spine surgery: a systematic review. Eur Spine J. 2011;20(2):185-194. [40] NAKAMA S, NITANAI K, OOHASHI Y, et al. Cervical muscle strength after laminoplasty. J Orthop Sci. 2003;8(1):36-40. [41] SILVERMAN JL, RODRIQUEZ AA, AGRE JC. Quantitative cervical flexor strength in healthy subjects and in subjects with mechanical neck pain. Arch Phys Med Rehabil. 1991;72(9):679-681. [42] CAMPBELL PG, YADLA S, MALONE J, et al. Early complications related to approach in cervical spine surgery: single-center prospective study. World Neurosurgery. 2010;74(2-3):363-368. [43] 石云志,刘泉.长节段颈椎后纵韧带骨化症修复:后路椎板切除植骨内固定与前路椎体次全切除减压的比较[J].中国组织工程研究,2014,18(53):8601-8606. [44] ROSENTHAL BD, NAIR R, HSU WK, et al. Dysphagia and dysphonia assessment tools after anterior cervical spine surgery. Clin Spine Surg. 2016;29(9):363-367. [45] 严妹,胡学昱,王倩.前路与后路减压融合术治疗颈椎后纵韧带骨化症的效果比较及术后1年预后的影响因素分析[J].中国医药,2019,14(6):909-913. [46] CHE W, LI RY, DONG J. Progress in diagnosis and treatment of cervical postoperative infection. Orthop Surg. 2011;3(3):152-157. [47] BARNES M, LIEW S. The incidence of infection after posterior cervical spine surgery: a 10 year review. Global Spine J. 2012;2(1):3-6. [48] NASSER R, KOSTY JA, SHAH S, et al. Risk Factors and Prevention of Surgical Site Infections Following Spinal Procedures. Global Spine J. 2018;8(4 Suppl):44s-48s. |
| [1] | Zhong Jun, Wang Wen. Network meta-analysis of different anatomical repair strategies to improve chronic lateral ankle instability [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1470-1476. |
| [2] | Ma Shuwei, He Sheng, Han Bing, Zhang Liaoyun. Exosomes derived from mesenchymal stem cells in treatment of animals with acute liver failure: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1137-1142. |
| [3] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [4] | Hu Zhixing, Li Qun, Yang Chao, Wang Xiaoxiao, Fang Luochangting, Hou Wuqiong, Lin Na, Chen Weiheng, Liu Chunfang, Lin Ya. Network meta-analysis of the modeling effects of different factors on rabbit models of steroid-induced osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 976-984. |
| [5] | Yu Zhaoyu, Tan Lixin, Sun Kai, Lu Yao, Li Yong. Meta-analysis of cement-augmented pedicle screw for thoracolumbar degenerative diseases with osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 813-820. |
| [6] | Abuduwupuer·Haibier, Alimujiang·Yusufu, Maihemuti·Yakufu, Maimaitimin·Abulimiti, Tuerhongjiang·Abudurexiti. Meta-analysis of efficacy and safety of terlipatide and bisphosphate in the treatment of postmenopausal osteoporosis fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 639-645. |
| [7] | Bai Xiaotian, Chen Zhaoying, Song Yiling, Wang Ye, Liu Jingmin. Effect of minimalist shoes on foot muscle morphology: systematic evaluation and Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 646-650. |
| [8] | Wang Juan, Wang Ling, Zuo Huiwu, Zheng Cheng, Wang Guanglan, Chen Peng. Rehabilitative efficacy of kinesio taping following anterior cruciate ligament reconstruction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 651-656. |
| [9] | Dong Kuan, Xu Chengli, Tian Jing, Xu Changchun. Effects of endurance training with blood flow restriction on aerobic capacity, lower limb muscle strength, and sports performance: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3766-3772. |
| [10] | Chang Wanpeng, Zhang Zhongwen, Yang Yulin, Zi Yang, Yang Mengqi, Du Bingyu, Wang Nan, Yu Shaohong. Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 321-328. |
| [11] | Jiang Yu, Luo Yan, Lin Xisheng, Wang Yilin, Gao Zefu, Lyu Houchen, Zhang Licheng, Tang Peifu, Liu Yujie. Effect of dementia on postoperative complications in older patients with hip fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2895-2900. |
| [12] | Zhang Guoxu, Zeng Jianbo, Li Jing, Xie Qijun, Zhou Guanbin, Guan Jianhao, Chen Wenchuang, Chen Haiyun. Meta-analysis of efficacy of orthopedic robot-assisted versus freehand percutaneous sacroiliac screw fixation for posterior pelvic ring fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2932-2938. |
| [13] | Wang Ke, Zhang Zeyi, Zhang Liwen, Zhang Meizhen. Biomechanics characteristics during sitting up in knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2939-2946. |
| [14] | Liu Renfan, Lyu Liting, Wu Yi, Wang Lu. Effects of high-intensity interval training and moderate-intensity continuous training on body composition and glucose metabolism in overweight or obese patients with type 2 diabetes: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2274-2281. |
| [15] | Liu Xinxin, Geng Zhizhong, Chen Jian. Effects of high-intensity interval training with different intervention durations on cognitive function in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2282-2289. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||