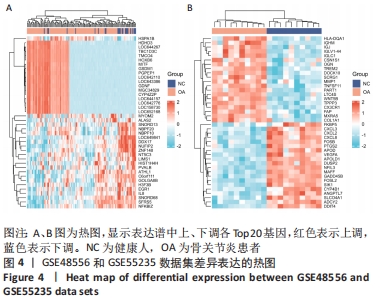
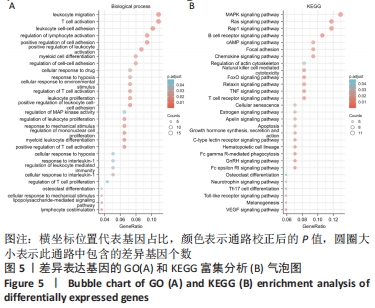
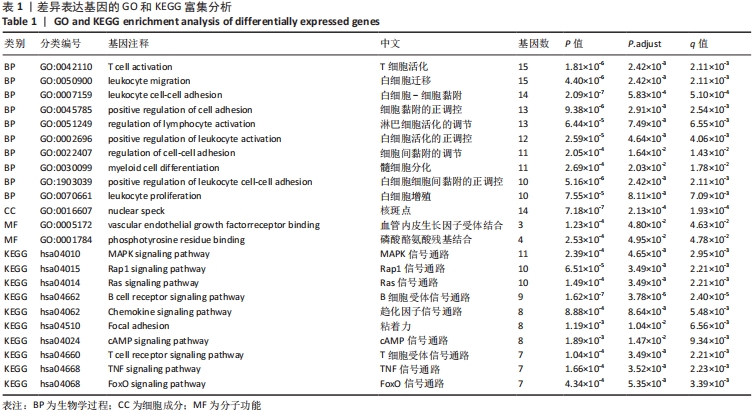
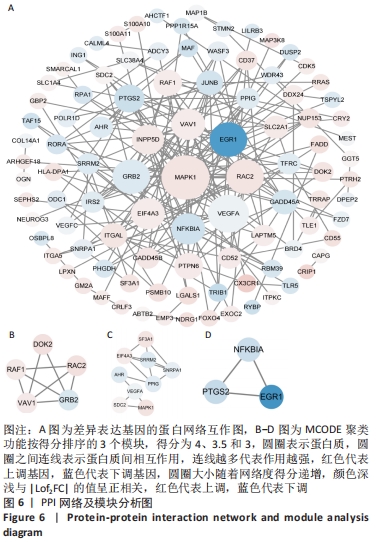
[1] Macfarlane E, Seibel MJ, Zhou H. et al. Arthritis and the role of endogenous glucocorticoids. Bone Res. 2020;8:33.
[2] HUNTER DJ, BIERMA-ZEINSTRA S. Osteoarthritis. Lancet. 2019;393 (10182):1745-1759.
[3] Miller RE, Scanzello CR, Malfait AM. An emerging role for toll-like receptors at the neuroimmune interface in osteoarthritis. Semin Immunopathol. 2019;41(5):583-594.
[4] Aubourg G, Rice SJ, Bruce-Wootton P, et al. Genetics of osteoarthritis. Osteoarthritis Cartilage. 2021;S1063-4584(21)00632-4. doi: 10.1016/j.joca.2021.03.002.
[5] Ratneswaran A, Kapoor M. Osteoarthritis year in review: genetics, genomics, epigenetics. Osteoarthritis Cartilage. 2021;29(2):151-160.
[6] Coryell PR, Diekman BO, Loeser RF. Mechanisms and therapeutic implications of cellular senescence in osteoarthritis. Nat Rev Rheumatol. 2021;17(1):47-57.
[7] Veret D, Jorgensen C, Brondello JM. Osteoarthritis in time for senotherapeutics. Joint Bone Spine. 2021;88(2):105084.
[8] Kulkarni P, Martson A, Vidya R, et al. Pathophysiological landscape of osteoarthritis. Adv Clin Chem. 2021;100:37-90.
[9] Perry TA, Parkes MJ, Hodgson RJ, et al. Association between Bone marrow lesions & synovitis and symptoms in symptomatic knee osteoarthritis. Osteoarthritis Cartilage. 2020;28(3):316-323.
[10] KATZ JN, ARANT KR, LOESER RF. Diagnosis and Treatment of Hip and Knee Osteoarthritis: A Review. JAMA. 2021;325(6):568-578.
[11] Hunter DJ, March L, Chew M. Osteoarthritis in 2020 and beyond: a Lancet Commission. Lancet. 2020;396(10264):1711-1712.
[12] Szilagyi IA, Waarsing JH, Schiphof D, et al. Towards sex-specific osteoarthritis risk models: evaluation of risk factors for knee osteoarthritis in males and females. Rheumatology (Oxford). 2021;keab378. doi: 10.1093/rheumatology/keab378.
[13] SUN X, ZHEN X, HU X, et al. Osteoarthritis in the Middle-Aged and Elderly in China: Prevalence and Influencing Factors. Int J Environ Res Public Health. 2019;16(23):4701.
[14] Ma L, Chhetri JK, Zhang L, et al. Cross-sectional study examining the status of intrinsic capacity decline in community-dwelling older adults in China: prevalence, associated factors and implications for clinical care. BMJ Open. 2021;11(1):e043062.
[15] 孙青,梁锴,李岩.血液样本质量的评估技术进展[J].生物化学与生物物理进展,2021,48(8):938-946.
[16] 周巧,刘健,宋倩,等.膝骨关节炎患者外周血单个核细胞CD36表达与氧化应激的相关性研究[J].风湿病与关节炎,2021,10(3):6-11.
[17] WENDLING D, ABBAS W, GODFRIN-VALNET M, et al. Resveratrol, a sirtuin 1 activator, increases IL-6 production by peripheral blood mononuclear cells of patients with knee osteoarthritis. Clin Epigenetics. 2013;5(1):10.
[18] Soyocak A, Kurt H, Ozgen M, et al. miRNA-146a, miRNA-155 and JNK expression levels in peripheral blood mononuclear cells according to grade of knee osteoarthritis. Gene. 2017;627:207-211.
[19] Okuhara A, Nakasa T, Shibuya H, et al. Changes in microRNA expression in peripheral mononuclear cells according to the progression of osteoarthritis. Mod Rheumatol. 2012;22(3):446-457.
[20] Ramos YF, Bos SD, Lakenberg N, et al. Genes expressed in blood link osteoarthritis with apoptotic pathways. Ann Rheum Dis. 2014;73(10): 1844-1853.
[21] Feng Z, Lian KJ. Identification of genes and pathways associated with osteoarthritis by bioinformatics analyses. Eur Rev Med Pharmacol Sci. 2015;19(5):736-744.
[22] Li J, Lan CN, Kong Y, et al. Identification and Analysis of Blood Gene Expression Signature for Osteoarthritis With Advanced Feature Selection Methods. Front Genet. 2018;9:246.
[23] ZHANG W, QIU Q, SUN B, et al. A four-genes based diagnostic signature for osteoarthritis. Rheumatol Int. 2021;41(10):1815-1823.
[24] Riyazi N, Meulenbelt I, Kroon HM, et al. Evidence for familial aggregation of hand, hip, and spine but not knee osteoarthritis in siblings with multiple joint involvement: the GARP study. Ann Rheum Dis. 2005;64(3):438-443.
[25] Shi T, Shen X, Gao G. Gene Expression Profiles of Peripheral Blood Monocytes in Osteoarthritis and Analysis of Differentially Expressed Genes. Biomed Res Int. 2019;2019:4291689.
[26] Cai P, Jiang T, Li B, et al. Comparison of rheumatoid arthritis (RA) and osteoarthritis (oa) based on microarray profiles of human joint fibroblast-like synoviocytes. Cell Biochem Funct. 2019;37(1):31-41.
[27] SUBRAMANIAN A, NARAYAN R, CORSELLO SM, et al. A Next Generation Connectivity Map: L1000 Platform and the First 1,000,000 Profiles. Cell. 2017;171(6):1437-1452.
[28] Enache OM, Lahr DL, Natoli TE, et al The GCTx format and cmap{Py, R, M, J} packages: resources for optimized storage and integrated traversal of annotated dense matrices. Bioinformatics. 2019; 35(8):1427-1429.
[29] 袁普卫.李氏四辨思想在膝骨关节炎防治中的作用[J].中国中西医结合杂志,2021,41(7):782-783.
[30] 李金明,王辉,张志毅.骨关节炎诊断生物标记物研究进展[J].中华风湿病学杂志,2020,24(9):631-634.
[31] 解英,陈斌,汪虹,等.外周血单个核细胞来源的多潜能细胞的研究进展[J].中华烧伤杂志,2016,32(12):762-764.
[32] 李伯阳,赵艳玲,田玉玲,等.轮状病毒感染患者外周血单个核细胞的转录组学分析[J/OL].病毒学报,2021, https://doi.org/10.13242/j.cnki.bingduxuebao.003963.
[33] 郭朋朋,刘亚妮,师少军,等.器官移植受者外周血单个核细胞中免疫抑制剂药物浓度的影响因素研究进展[J].中国医院药学杂志, 2021,41(8):855-859.
[34] 魏叶,刘亚妮,师少军,等.外周血单个核细胞内免疫抑制剂的浓度与实体器官移植术后不良反应相关性的研究进展[J].中国医院药学杂志,2020,40(8):946-951.
[35] Ponchel F, Burska AN, Hensor EM, et al. Changes in peripheral blood immune cell composition in osteoarthritis. Osteoarthritis Cartilage. 2015;23(11):1870-1878.
[36] Moradi B, Rosshirt N, Tripel E, et al. Unicompartmental and bicompartmental knee osteoarthritis show different patterns of mononuclear cell infiltration and cytokine release in the affected joints. Clin Exp Immunol. 2015;180(1):143-154.
[37] 王猛,陈敬东,王佳蔚. 膝关节骨关节炎外周血标志物变化的临床研究[J].重庆医科大学学报,2021,46(3):306-310.
[38] Wu CL, Harasymowicz NS, Klimak MA, et al. The role of macrophages in osteoarthritis and cartilage repair. Osteoarthritis Cartilage. 2020;28(5):544-554.
[39] Thomson A, Hilkens CMU. Synovial Macrophages in Osteoarthritis: The Key to Understanding Pathogenesis? Front Immunol. 2021;12: 678757.
[40] Zhang H, Cai D, Bai X. Macrophages regulate the progression of osteoarthritis. Osteoarthritis Cartilage. 2020;28(5):555-561.
[41] Kooistra MR, Dubé N, Bos JL. Rap1: a key regulator in cell-cell junction formation. J Cell Sci. 2007;120(1):17-22.
[42] Boettner B, Van Aelst L. Control of cell adhesion dynamics by Rap1 signaling. Curr Opin Cell Biol. 2009;21(5):684-693.
[43] Xia Z, Storm DR. The role of calmodulin as a signal integrator for synaptic plasticity. Nat Rev Neurosci. 2005;6(4):267-276.
[44] Doebele RC, Schulze-Hoepfner FT, Hong J, et al. A novel interplay between Epac/Rap1 and mitogen-activated protein kinase kinase 5/extracellular signal-regulated kinase 5 (MEK5/ERK5) regulates thrombospondin to control angiogenesis. Blood. 2009;114(20): 4592-4600.
[45] Minato N, Kometani K, Hattori M. Regulation of Immune Responses and Hematopoiesis by the Rap1 Signal. 2007:229-264.
[46] Breckler M, Berthouze M, Laurent AC, et al. Rap-linked cAMP signaling Epac proteins: Compartmentation, functioning and disease implications. Cellular Signalling. 2011;23(8):1257-1266.
[47] 于雅丽,孔奕翼,叶静,等.基于综合生物信息学筛选骨关节炎潜在生物标记物的研究[J].中华创伤骨科杂志,2021,23(1):75-80.
[48] STRZELECKA-KILISZEK A, MEBAREK S, ROSZKOWSKA M, et al. Functions of Rho family of small GTPases and Rho-associated coiled-coil kinases in bone cells during differentiation and mineralization. Biochim Biophys Acta Gen Subj. 2017;1861(5 Pt A):1009-1023.
[49] HOU SM, HOU CH, LIU JF. CX3CL1 promotes MMP-3 production via the CX3CR1, c-Raf, MEK, ERK, and NF-κB signaling pathway in osteoarthritis synovial fibroblasts. Arthritis Res Ther. 2017;19(1):282.
[50] Stiffel VM, Thomas A, Rundle CH, et al. The EphA4 Signaling is Anti‑catabolic in Synoviocytes but Pro‑anabolic in Articular Chondrocytes. Calcif Tissue Int. 2020;107(6):576-592.
[51] HAMILTON JL, NAGAO M, LEVINE BR, et al. Targeting VEGF and its Receptors for the Treatment of Osteoarthritis and Associated Pain. J Bone Miner Res. 2016;31(5):911-924.
[52] GUAN M, ZHU Y, LIAO B, et al. Low-intensity pulsed ultrasound inhibits VEGFA expression in chondrocytes and protects against cartilage degeneration in experimental osteoarthritis. FEBS Open Bio. 2020;10(3):434-443.
[53] Xu K, Gao Y, Yang L, et al. Magnolin exhibits anti-inflammatory effects on chondrocytes via the NF-kappaB pathway for attenuating anterior cruciate ligament transection-induced osteoarthritis. Connect Tissue Res. 2021;62(4):475-484.
[54] LI Z, WANG H, WEI J, et al. Indirubin exerts anticancer effects on human glioma cells by inducing apoptosis and autophagy. AMB Express. 2020; 10(1):171.
[55] LAI J, LIU Y, LIU C, et al. Indirubin Inhibits LPS-Induced Inflammation via TLR4 Abrogation Mediated by the NF-kB and MAPK Signaling Pathways. Inflammation. 2017;40(1):1-12.
|